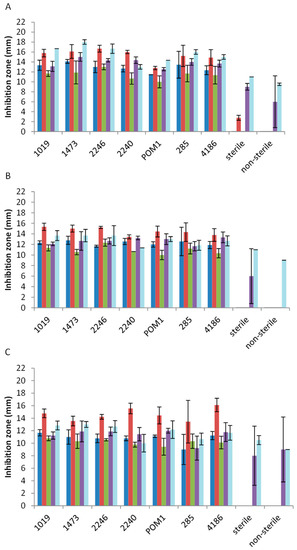
Which would be most effective against Pseudomonas?
- Wash your hands often. This is the best way to avoid getting pseudomonas.
- Rinse fruits and vegetables before eating.
- Clean your water bottles.
- Avoid unclean pools and hot tubs.
- Ask questions about your medical care.
- Take care of your health.
What is the biochemical test for Pseudomonas?
Pseudomonas gives negative Voges Proskauer, indole and methyl red tests, but a positive catalase test. While some species show a negative reaction in the oxidase test, most species, including P. fluorescens, give a positive result (Figure 2). Another feature associated with Pseudomonas is the secretion of pyoverdin (fluorescein, a siderophore ...
What does it take to be a Pseudomonas aeruginosa?
Pseudomonas aeruginosa is a common, free-living, Gram-negative bacterium that can cause significant disease as an opportunistic pathogen. Rapid growth, facile genetics, and a large suite of virulence-related phenotypes make P. aeruginosa a common model organism to study Gram-negative opportunistic pathogens and basic microbiology.
Is it dangerous to have Pseudomonas aeruginosa?
Pseudomonas can be dangerous to people with weakened immune systems. While Pseudomonas aeruginosa bacteria are of little concern to those who are healthy and strong, they can be deadly for those whose health is not as robust. Indeed, this is one of the reasons why it can cause serious infections among people who are ill and being treated in ...
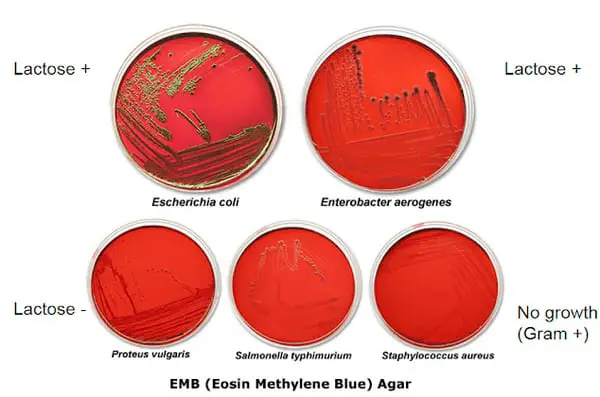
Is Pseudomonas a lactose fermentation?
Panel C shows Pseudomonas aeruginosa, a lactose non-fermenter. Almost 120 years later, MacConkey agar remains ubiquitous in clinical laboratories, where it is used routinely to select for non-fastidious Gram-negative organisms in wound, urine, stool, and blood cultures.
Is Pseudomonas aeruginosa lactose positive?
P. aeruginosa is a gram-negative, lactose nonfermenting, straight or slightly curved rod with a length ranging from 1.5 to 7 µm and a width of 0.5 to 1.0 µm. It is catalase positive, oxidase positive, and motile with one or more polar flagella. Most species oxidize glucose and reduce nitrate to nitrite or nitrogen gas.
Does P. aeruginosa ferment lactose or sucrose?
However, multiple other tests showed that lactose is not fermented by P. aeruginosa....Biochemical characteristics and Enzymes Made.Gram StainNegativePhenol Red SucroseRed: no Sucrose fermentationPhenol Red LactoseRed: no Lactose fermentation.28 more rows•Dec 8, 2017
Is Pseudomonas aeruginosa fermented?
Only one Pseudomonas species is capable of anaerobic fermentation: Pseudomonas aeruginosa [17,18,19,20]. P. aeruginosa is capable of arginine fermentation and pyruvate fermentation, although the latter only leads to prolonged survival under anoxic conditions, not to growth [18,19,20].
What does Pseudomonas aeruginosa look like on MacConkey agar?
In MacConkey agar, Pseudomonas aeruginosa forms flat and smooth colonies that are between 2 and 3mm in diameter. Generally, these colonies have regular margins and have an alligator skin-like appearance when viewed from above. See more on Cell Culture.
What is non lactose fermenting bacteria?
Organisms unable to ferment lactose will form normal-colored (i.e., un-dyed) colonies. The medium will remain yellow. Examples of non-lactose fermenting bacteria are Salmonella, Proteus species, Yersinia, Pseudomonas aeruginosa and Shigella.
Is Pseudomonas a glucose fermenter?
If an organism is capable of fermenting the sugar glucose, then acidic byproducts are formed and the pH indicator turns yellow. Escherichia coli is capable of fermenting glucose as are Proteus mirabilis (far right) and Shigella dysenteriae (far left). Pseudomonas aeruginosa (center) is a nonfermenter.
How do you identify Pseudomonas aeruginosa?
Conventional Pseudomonas aeruginosa detection methods are based on the biological characteristics of the bacterium under certain culture conditions, such as Gram-negative or Gram-positive status, or the activities of bacterial molecules such as oxidase, acetamidase, arginine dihydrolase, and pyocyanin.
What is the confirmatory test for Pseudomonas aeruginosa?
Confirmation of P. Production of pigments such as pyocyanin and pyoverdin by the purified isolates were tested by “fluorescent technique” after growing the isolates on cetrimide and Pseudomonas agar followed by ultraviolet (UV) illumination [12] for confirmation.
Is Pseudomonas aeruginosa a facultative anaerobe?
Though P. aeruginosa is a facultative anaerobe that preferably uses aerobic respiration, its ability to undergo anaerobiosis is due to the presence of nitrate (NO3−), which acts as an end terminal electron acceptor38,39. Nitrate has been detected in both airway surface liquid (ASL) and in CF airway sputum31,32,40.
Is Pseudomonas an Anaerobe?
Pseudomonas aeruginosa had been considered as an obligately aerobic bacterium previously, but it is now recognized to be highly adapted to anaerobic conditions.
Is Pseudomonas aeruginosa positive for starch hydrolysis?
It was casein hydrolysis and lipase positive but starch hydrolysis negative. Acid production from carbohydrates tested (glucose and lactose) was negative. It can grow at 42°C but not at 4°C and tolerates <5% NaCl concentration.
Is Pseudomonas aeruginosa urease positive?
aeruginosa [96%]) or have a tuft of three to eight flagella (P. cepacia [99%]). They are catalase-positive and can also be positive for urease (P. aeruginosa [72%]), P.
What is the confirmatory test for Pseudomonas aeruginosa?
Confirmation of P. Production of pigments such as pyocyanin and pyoverdin by the purified isolates were tested by “fluorescent technique” after growing the isolates on cetrimide and Pseudomonas agar followed by ultraviolet (UV) illumination [12] for confirmation.
Is Pseudomonas aeruginosa positive for starch hydrolysis?
It was casein hydrolysis and lipase positive but starch hydrolysis negative. Acid production from carbohydrates tested (glucose and lactose) was negative. It can grow at 42°C but not at 4°C and tolerates <5% NaCl concentration.
What are the characteristics of Pseudomonas aeruginosa?
Pseudomonas aeruginosa is a Gram-negative, rod-shaped, asporogenous, and monoflagellated bacterium. It has a pearlescent appearance and grape-like or tortilla-like odour. P. aeruginosa grows well at 25°C to 37°C, and its ability to grow at 42°C helps distinguish it from many other Pseudomonas species.
What is the cause of P. aeruginosa?
P. aeruginosa causes infection in the urinary tract, respiratory system, dermis, soft tissue, bacteraemia, bone and joint, gastrointestine and blood, particularly in patients with severe burns, tuberculosis, cancer and AIDS. Importantly, P. aeruginosa causes a significant problem in patients hospitalized with cancer, cystic fibrosis and burns, ...
Why is P. aeruginosa so versatile?
Because of the large genome, P. aeruginosa encodes a large number of enzymes for various metabolic pathways, conferring high nutritional versatility. In addition, about 8% of the genome encodes regulatory genes, which enables the bacterium to adapt to complex growth environments. View chapter Purchase book.
What pigments does P. aeruginosa produce?
Most strains of P. aeruginosa produce one or more pigments, including pyocyanin (blue-green), pyoverdine (yellow-green and fluorescent), and pyorubin (red-brown). Previous investigations have suggested that pyocyanin not only contributes to the persistence of P. aeruginosa in the lungs of CF patients, but also interferes with many mammalian cell functions, including cell respiration, ciliary beating, epidermal cell growth, calcium homeostasis and prostacyclin release from lung endothelial cells [1]. However, the precise molecular mechanism mediated by pyocyanin pathology is unknown.
What are the different types of P. aeruginosa?
P. aeruginosa isolates demonstrate three types of colonies. Natural isolates from soil or water typically are a small, rough colony, while clinical isolates are likely smooth colony types, occasionally with a fried-egg appearance that is large, smooth, with flat edges and an elevated appearance. Respiratory and urinary tract secretions may show a mucoid-type (alginate slime). P. aeruginosa has two different soluble pigments, the fluorescent pigment pyoverdin and blue pyocyanin. Pyocyanin refers to blue pus, a typical feature of suppurative infections caused by P. aeruginosa. Pyochelin (a derivative of pyocyanin) is a siderophore and can acquire iron from the host or in low-iron environments to maintain the pathogen growth. Pyocyanin can disrupt the normal function of human nasal cilia and the respiratory epithelium, thereby igniting pro-inflammatory responses [147]. No virulence evidence is described for the fluorescent pigments.
What is the role of P. aeruginosa in the human body?
P. aeruginosa exploits weaknesses in host defence to mount an infection. Indeed, P. aeruginosa is the epitome of an opportunistic pathogen of humans. The bacterium hardly infects uncompromised tissues, but it can invade any tissue beleaguered by immunodeficiency. P. aeruginosa causes infection in the urinary tract, respiratory system, dermis, soft tissue, bacteraemia, bone and joint, gastrointestine and blood, particularly in patients with severe burns, tuberculosis, cancer and AIDS. Importantly, P. aeruginosa causes a significant problem in patients hospitalized with cancer, cystic fibrosis and burns, with 50% fatality [143]. According to the Centers for Disease Control and Prevention (CDC), the overall incidence of P. aeruginosa infections in US hospitals averages about 0.4% (4 per 1000 discharges), and the bacterium is the fourth most common isolated nosocomial pathogen, accounting for 10% of all hospital-acquired infections. P. aeruginosa shows a rod shape of 0.5–0.8 µm by 1.5–3.0 µm. The bacterial strains are motile with a single polar flagellum. The metabolism is oxygen-based respiratory, but this ubiquitous bacterium will grow in the absence of O 2 but in the presence of NO 3 [144].
What temperature does P. aeruginosa grow?
The optimum temperature for growth is 37°C, but P. aeruginosa also grows at temperatures as high as 42°C [146]. P. aeruginosa is resistant to high concentrations of salts and dyes, weak antiseptics, and many commonly used antibiotics.
How common is P. aeruginosa?
aeruginosa infections in US hospitals averages about 0.4% (4 per 1000 discharges ), and the bacterium is the fourth most common isolated nosocomial pathogen, accounting for 10% of all hospital-acquired infections.
Where do pseudomonas live?
Pseudomonasspecies normally inhabit soil, water, and vegetation and can be isolated from the skin, throat, and stool of healthy persons. They often colonize hospital food, sinks, taps, mops, and respiratory equipment. Spread is from patient to patient via contact with fomites or by ingestion of contaminated food and water.
Which species of pseudomonads produce glanders?
Only two species, P mallei and P pseudomallei, produce specific human diseases: glanders and melioidosis. Pseudomonas aeruginosa and P maltophilia account for approximately 80 percent of pseudomonads recovered from clinical specimens. Because of the frequency with which it is involved in human disease, P aeruginosa has received the most attention.
How many species of pseudomonads are there?
The genus Pseudomonas contains more than 140 species, most of which are saprophytic. More than 25 species are associated with humans. Most pseudomonads known to cause disease in humans are associated with opportunistic infections.
How does P aeruginosa grow?
Pseudomonas aeruginosais a nonfermentative aerobe that derives its energy from oxidation rather than fermentation of carbohydrates. Although able to use more than 75 different organic compounds, it can grow on media supplying only acetate for carbon and ammonium sulfate for nitrogen. Furthermore, although an aerobe, it can grow anaerobically, using nitrate as an electron acceptor. This organism grows well at 25° C to 37° C, but can grow slowly or at least survive at higher and lower temperatures. Indeed, the ability to grow at 42° C distinguishes it from many other Pseudomonasspecies. In addition to its nutritional versatility, P aeruginosaresists high concentrations of salt, dyes, weak antiseptics, and many commonly used antibiotics. These properties help explain its ubiquitous nature and contribute to its preeminence as a cause of nosocomial infections.
Why is the mortality rate high in Pseudomonas?
The high mortality associated with these infections is due to a combination of weakened host defenses, bacterial resistance to antibiotics, and the production of extracellular bacterial enzymes and toxins. The genus Pseudomonas contains more than 140 species, most of which are saprophytic. More than 25 species are associated with humans.
What is the opportunistic pathogen that may infect virtually any tissue?
Diverse sites of infection by P aeruginosa. This opportunistic pathogen may infect virtually any tissue. Infection is facilitated by the presence of underlying disease (e.g., cancer, cystic fibrosis) or by a breakdown in nonspecific host defenses (as (more...)
What media can pseudomonascan be cultured on?
Pseudomonascan be cultured on most general-purpose media and identified with biochemical media.
INTRODUCTION
The pseudomonads are a heterogeneous group of gram-negative bacteria that have in common an inability to ferment lactose.
PSEUDOMONAS AERUGINOSA
P. aeruginosa is found in most moist environments. Soil, plants, vegetables, tap water, and countertops are all potential reservoirs for this microbe, as it has simple nutritional needs. Given the ubiquity of P. aeruginosa, simple contact with the organism is not sufficient for colonization or infection.
Introduction of LF and NLF Gram-Negative Bacteria on MacConkey Medium
MacConkey agar/ medium is recommended for use as a selective, differential, and indicator growth medium for the isolation of gram-negative bacilli including coliform organisms and enteric pathogens, on the basis of lactose fermentation.
List of LF Bacteria and NLF Bacteria
The list of lactose fermenter Gram-negative bacteria on the basis of MacConkey medium are as follows-
Keynotes
Pasteurella species (including Pasteurella multocida) will not grow on MacConkey Agar.
Spinal cord injury, heavily sedated, or ventilated patients
Surveillance criteria may not be equally sensitive for all patient populations. Patient populations in which the UTI criteria may not be as sensitive include spinal cord injury patients, those with brain injuries, and heavily sedated patients.
Mixed flora
No, this urine culture is not eligible for use in an NHSN UTI determination. Because “mixed flora”* implies that at least 2 organisms are present in addition to the identified organism, the urine culture does not meet the criteria for a positive urine culture with 2 organisms or less.
Multiple colony counts for the same organism
Yes.
Number of organisms in cultures
Do not add multiple cultures together. More than 2 organisms in a single urine culture suggests the possibility of contamination of the specimen. The same is not true for separate urine cultures with less than 3 organisms in each.
Identifying single vs multiple UTIs
Yes. This time period is called the Repeat Infection Timeframe (RIT). Please see the information on RIT found in Chapter 2 “ Identifying Healthcare-associated Infections pdf icon [PDF – 1 MB] ” in the NHSN manual.
Patient reported fever
If the patient reports a fever > 38.0°C (or over 100.4 0 F), during the POA timeframe and within the IWP of a positive urine culture, this can be used to determine if the definition of a POA infection is met. A general report of “fever” by the patient, without an accompanying temperature measurement, may not be used.
UTI Symptom: dysuria
Urinary retention is not the same as dysuria and cannot be used to meet the UTI definition.

Overview
Diagnosis
Depending on the nature of infection, an appropriate specimen is collected and sent to a bacteriology laboratory for identification. As with most bacteriological specimens, a Gram stain is performed, which may show Gram-negative rods and/or white blood cells. P. aeruginosa produces colonies with a characteristic "grape-like" or "fresh-tortilla" odor on bacteriological media. In mixed cultures, i…
Nomenclature
The word Pseudomonas means "false unit", from the Greek pseudēs (Greek: ψευδής, false) and (Latin: monas, from Greek: μονάς, a single unit). The stem word mon was used early in the history of microbiology to refer to germs, e.g., kingdom Monera.
The species name aeruginosa is a Latin word meaning verdigris ("copper rust"), …
Biology
The genome of Pseudomonas aeruginosa consists of a relatively large circular chromosome (5.5–6.8 Mb) that carries between 5,500 and 6,000 open reading frames, and sometimes plasmids of various sizes depending on the strain. Comparison of 389 genomes from different P. aeruginosa strains showed that just 17.5% is shared. This part of the genome is the P. aeruginosa core genome.
Pathogenesis
An opportunistic, nosocomial pathogen of immunocompromised individuals, P. aeruginosa typically infects the airway, urinary tract, burns, and wounds, and also causes other blood infections.
It is the most common cause of infections of burn injuries and of the outer ear (otitis externa), and is the most frequent colonizer of medical devices (e.g., cath…
Treatment
Many P. aeruginosa isolates are resistant to a large range of antibiotics and may demonstrate additional resistance after unsuccessful treatment. It should usually be possible to guide treatment according to laboratory sensitivities, rather than choosing an antibiotic empirically. If antibiotics are started empirically, then every effort should be made to obtain cultures (before admini…
Research
In 2013, João Xavier described an experiment in which P. aeruginosa, when subjected to repeated rounds of conditions in which it needed to swarm to acquire food, developed the ability to "hyperswarm" at speeds 25% faster than baseline organisms, by developing multiple flagella, whereas the baseline organism has a single flagellum. This result was notable in the field of experimental evolution in that it was highly repeatable.
Distribution
As of 2019 the East African Community considers P. aeruginosa to be a quarantine concern. The presence of Phaseolus vulgaris-pathogenic strains of P. aeruginosa in Kenya for the rest of the area. A pest risk analysis by the EAC was based on this bacterium's CABI's Crop Protection Compendium listing, following Kaaya & Darji 1989's initial detection in Kenya.