Explore
- Wash your hands thoroughly with soap and water.
- Stand or sit in a comfortable position in front of a mirror (in the bathroom over the sink is a good place to care for your trach tube).
- Put on the gloves.
- Suction the trach tube. ...
- If your tube has an inner cannula, remove it. ...
How to maintain and care for a tracheostomy?
- Adjust the wall suction to the appropriate level.
- Explain the procedure to the client.
- Open sterile packages and set up sterile field.
- Auscultate the client's lung sounds for evaluation of the intervention
- Don sterile gloves.
- Adjust the bed and position the client.
What care is needed for a tracheostomy?
- Need for prolonged respiratory support, such as Bronchopulmonary Dysplasia (BPD)
- Chronic pulmonary disease to reduce anatomic dead space
- Chest wall injury
- Diaphragm dysfunction
Why would someone need a tracheotomy?
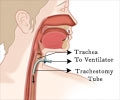
A tracheostomy is often needed when health problems require long-term use of a machine (ventilator) to help you breathe. In rare cases, an emergency tracheotomy is performed when the airway is suddenly blocked, such as after a traumatic injury to the face or neck.
Does a traceotomy always require a ventilator to breath?

Can you go back to normal after tracheostomy?
After having a tracheostomy you should be able to continue doing everyday activities, but should avoid vigorous activities for about 6 weeks after the procedure. It's very important to keep the opening of your tracheostomy clean and dry when you're outside. It will usually be covered with a dressing.
How long does it take for a tracheostomy hole to close?
The healing process We expect the stoma to close within 7-14 days, however for some patients this may take longer. The stoma will naturally heal from the inside of the body (windpipe) to the outside. This means the part you can see on your neck will heal last.
What to expect after a tracheostomy is removed?
Healing Time After Tracheostomy Removal The bandage will remain in place while the opening is fully healed — which could take up to two weeks. The doctor will provide instructions on how to clean the wound and how often to do so. Once the opening is healed, there will be a small scar.
What are the long term effects of a tracheostomy?
Air trapped in the deeper layers of the chest(pneumomediastinum) Air trapped underneath the skin around the tracheostomy (subcutaneous emphysema) Damage to the swallowing tube (esophagus) Injury to the nerve that moves the vocal cords (recurrent laryngeal nerve)
What is the most serious complication of a tracheostomy?
One of the most striking direct complications of a tracheostomy is a displaced tube. This is likely to occur if the tracheostomy is too low or not in the midline.
Can you ever get off a trach?
After having a tracheostomy, you'll need to stay in hospital for at least a few days or weeks. It may sometimes be possible to remove the tube and close the opening before you leave hospital. However, the tube may need to stay in permanently if you have a long-term condition that affects your breathing.
What is the difference between a tracheotomy and a tracheostomy?
The term “tracheotomy” refers to the incision into the trachea (windpipe) that forms a temporary or permanent opening, which is called a “tracheostomy,” however; the terms are sometimes used interchangeably.
Can patient eat orally with a tracheostomy?
If the patient eats by mouth, it is recommended that the tracheostomy tube be suctioned prior to eating. This often prevents the need for suctioning during or after meals, which may stimulate excessive coughing and could result in vomiting. Encouraging fluid intake is helpful for a patient with a tracheostomy.
Does a tracheostomy leave a scar?
Tracheotomy wounds, healing as they do by secondary intention, leave, at best, unsightly scars which are often complicated by large depressions due to the ingrowth of skin, which communicates directly with the mucosa of the trachea (Fig. 1).
How could he overcome his difficulties after the tracheotomy operation?
1 Answer. Since Hawking could not speak, Walt Woltosz, a computer expert in California, sent him a programme he had developed. It was called the Equalizer. It would allow Hawking to select words from the screen and this way he could continue to do his work, although very slowly.
Can you speak after a tracheostomy is removed?
That changes in the voice are common during the first few weeks following tracheostomy tube removal. If this change is likely to be permanent, patients should be advised of this before they go home. If the voice changes (e.g. hoarseness, weakness, or whispering quality), patients should contact the hospital.
Can you fly if you have a trach?
There is no reason why patients with a tracheostomy cannot travel domestically or abroad. Adequate insurance provisions will need to be made to ensure that the patient can be flown home quickly if necessary.
Can the hole be closed after a tracheostomy?
When it's possible for a person to breathe, protect their airway and clear fluids unaided, then the tracheostomy tube may be able to be removed. The opening will usually close on its own within a couple of weeks, leaving a small scar. If it doesn't close on its own, it can be closed using stitches.
How do they close up a tracheostomy?
The patient is instructed to occlude the gauze with their finger tip every time they cough or speak so that air does not leak. They should change the gauze and the tape at least once a day (more often as needed) until the hole in the neck heals itself closed over the next few days to weeks.
How do tracheostomy scars heal?
To correct hypertrophic tracheostomy scars, the most common procedure is excision of the scar with tensionless closure. Skin closure is performed by simple reapproximation or with local flaps, most commonly a z-plasty. Autologous fat transplantation is a newer, less invasive alternative.
Does a tracheostomy leave a scar?
Tracheotomy wounds, healing as they do by secondary intention, leave, at best, unsightly scars which are often complicated by large depressions due to the ingrowth of skin, which communicates directly with the mucosa of the trachea (Fig. 1).
How long do you stay in the hospital after a tracheostomy?
After the tracheostomy procedure, you'll likely stay in the hospital for several days as your body heals. If possible, plan ahead for your hospital stay by bringing: A communication method, such as a pencil and a pad of paper, a smartphone, or a computer, as you'll be unable to talk at first.
When is a tracheostomy performed?
In rare cases, an emergency tracheotomy is performed when the airway is suddenly blocked, such as after a traumatic injury to the face or neck. When a tracheostomy is no longer needed, it's allowed to heal shut or is surgically closed. For some people, a tracheostomy is permanent. Mayo Clinic's approach.
How to get rid of tracheostomy secretions?
Putting small amounts of saline directly into the tracheostomy tube, as directed, may help loosen secretions. Or a saline nebulizer treatment may help. A device called a heat and moisture exchanger captures moisture from the air you exhale and humidifies the air you inhale.
How is a tracheostomy tube inserted?
A tracheostomy tube is inserted through the hole and secured in place with a strap around your neck. Tracheostomy (tray-key-OS-tuh-me) is a hole that surgeons make through the front of the neck and into the windpipe (trachea). A tracheostomy tube is placed into the hole to keep it open for breathing. The term for the surgical procedure ...
What is a tracheostomy tube?
Overview. A tracheostomy is a surgically created hole (stoma) in your windpipe (trachea) that provides an alternative airway for breathing. A tracheostomy tube is inserted through the hole and secured in place with a strap around your neck. Tracheostomy (tray-key-OS-tuh-me) is a hole that surgeons make through the front ...
Why do we need a tracheostomy?
A tracheostomy is often needed when health problems require long-term use of a machine (ventilator) to help you breathe. In rare cases, an emergency tracheotomy is performed when the airway is suddenly blocked, ...
Why do nurses clean tracheostomy tubes?
A nurse will teach you how to clean and change your tracheostomy tube to help prevent infection and reduce the risk of complications. You'll continue to do this as long as you have a tracheostomy.
What are the long-term effects of a tracheostomy?
Long-term complications include tracheal stenosis, swallowing disorders, voice complaints or scarring. Swallowing disorders were described as difficulty swallowing, pain or aspiration. Voice complaints were mainly complaints of hoarseness.
Why would a trach be permanent?
A permanent tracheostomy is non-weanable and cannot be removed. It is inserted for a number of underlying long-term, progressive or permanent conditions, including cancer of the larynx or nasopharynx, motor neurone disease, locked-in syndrome, severe head injury, spinal-cord injury and paralysis of vocal cords.
What happens when a trach is removed?
After the tube is removed, the skin edges are taped shut, the patient is encouraged to occlude the defect while speaking or coughing. The wound should heal within 5-7 days. In preparation for decannulation, the tracheostomy tube may be plugged. The patient must be able to remove the plug should dyspnea develop.
How serious is a tracheostomy?
Tracheostomies are generally safe, but they do have risks. Some complications are particularly likely during or shortly after surgery. The risk of such problems greatly increases when the tracheotomy is performed as an emergency procedure.
Can a person with a trach live at home?
Can I go home with a tracheostomy? Some patients with a tracheostomy are able to go home. One major factor in moving back home is whether you still need a breathing machine (ventilator) to help you breathe.
Can you live a long life with a tracheostomy?
It’s possible to enjoy a good quality of life with a permanent tracheostomy tube. However, some people may find it takes time to adapt to swallowing and communicating. Your care team will talk to you about possible problems, the help that’s available, and how to look after your tracheostomy.
Does your voice change after a tracheostomy?
That changes in the voice are common during the first few weeks following tracheostomy tube removal. If this change is likely to be permanent, patients should be advised of this before they go home. If the voice changes (e.g. hoarseness, weakness, or whispering quality), patients should contact the hospital.
Is tracheostomy part of intensive care?
I have also worked in the community with dozens of long-term Intensive Care Patients (adults & children) on ventilators with tracheostomies as part of INTENSIVE CARE AT HOME.
Does a tracheostomy help with end of life?
In some instances it can also improve quality of end of life too. What a tracheostomy is also doing is it buys critically ill Patients time to come off a ventilator and recover.
Is a tracheostomy better for a coma?
Generally speaking, quality of life after a tracheostomy is improved in Intensive Care, because the need for sedation and induced coma is often minimized and/or excluded.
Should a tracheostomy be rushed?
Therefore, a tracheostomy on the one hand should not be rushed, but on the other hand it should always be offered. If a critically ill Patient can be weaned off the ventilator but can’t have the tracheostomy removed they should definitely be in a position to leave Intensive Care.
How long can you leave a decannulation cap on after neck surgery?
Tolerates speaking valve 12 hours or more (usually during daytime) or decannulation cap for up to four hours (If air flow is present on finger occlusion). In patients following head and neck surgery, the decannulation cap may be left for longer periods at the discretion of the surgeon
Why do patients die in LTAC?
Many Patients in LTAC die because the facilities simply lack the skills, expertise and know-how when it comes to ventilation and tracheostomy.
Is tracheostomy removal viable?
Whenever weaning off ventilation and removal of tracheostomy in Intensive Care fails or is prolonged, INTENSIVE CARE AT HOME of course is a viable and genuine option, creating a win-win situation for all parties involved by
Can you wean off a ventilator after a tracheostomy?
Once a tracheostomy has been done, your loved one can hopefully take the first steps to wean off ventilation and tracheostomy! Once the ventilator has been weaned , then the next step is to remove the tracheostomy !
Is a tracheostomy permanent?
In most cases, a tracheostomy is temporary, providing an alternative breathing route until other medical issues are resolved. If your loved one needs to remain connected to a ventilator indefinitely, the tracheostomy is often the best permanent solution.
Is it safe to ventilate a child with a tracheostomy?
Therefore, the only safe environment for ventilated adults and children with tracheostomies are either ICU or a home care environment with ICU nurses like you can get here at INTENSIVE CARE AT HOME.
What are the symptoms of a tracheostomy?
Furthermore, patients who have not fully recovered from the illness of the operation will require a breathing tube. Some of the aspects that patients should be fully aware of following removal of tracheostomy include: 1 Noisy Breathing Sound: When the patient develops a noisy squeaking sound during breathing, they should immediately call for assistance before things getting worse. 2 Feeling Breathless And Uncomfortable: Similarly, when the patient suffers shortness of breath or panicky, they should require immediate hospitalization for further treatment. 3 Soreness: Post-surgery, there can be soreness on the skin edges, and you may have trouble swallowing in the initial few days. It may take a couple of days or more to get used to breathing and expect to feel better each day. 3
How long does it take for a wound to heal?
However, the wound will take 1-2 weeks to heal completely but during this period if the injury becomes wet or starts to develop an infection, check with the nurse or GP immediately. Advertisement. Require frequent dressings than usual and also when the dressing changes color to green or red.
What Else The Patients Should Be Aware Of After Removal?
There are a few things the patients need to follow for the speedy recovery and when to reach for immediate medical assistance.
How long does it take to get used to breathing after a syringe?
Soreness: Post-surgery, there can be soreness on the skin edges, and you may have trouble swallowing in the initial few days. It may take a couple of days or more to get used to breathing and expect to feel better each day. 3.
Why is it so hard to speak after a breathing tube is removed?
3. Speaking is very difficult because speech is generated from the vocal cord at the back of the throat. 4.
Can a tracheostomy tube be removed?
In general, people with a tracheostomy often have problems with their routine lifestyle such as speaking, coughing, eating, drinking, and swallowing. In many instances, these difficulties persist despite the removal of the tracheostomy tube however it gets better over time.
Do you need a breathing tube after a tracheostomy?
Furthermore, patients who have not fully recovered from the illness of the operation will require a breathing tube. Some of the aspects that patients should be fully aware of following removal of tracheostomy include:
Who is this leaflet for?
This leaflet contains information about what happens with the stoma (hole) where your tracheostomy tube was removed (decannulation). It will help you and your family to understand the normal healing process and to be aware of things that could delay healing.
What is a tracheostomy stoma?
When a person requires a tracheostomy tube to be inserted, a stoma is made in their neck through to the trachea (windpipe). Once the tracheostomy tube has been removed the stoma remains. During the healing process of the stoma, you may experience secretions and air escaping when you cough or talk. This is normal.
The healing process
We expect the stoma to close within 7-14 days, however for some patients this may take longer.
Who will look after the stoma?
Whilst you are in hospital, the nursing team will monitor your stoma and carry out all dressing changes. Sometimes the tracheostomy nursing service will review you if necessary. If you go home whilst the stoma is still healing, the community nurses can continue to monitor, until the stoma is fully healed and closed.
How will I know that my stoma is fully healed?
Your nurses and doctors will be able to guide you as to when the stoma is fully healed. A good indication is when you can no longer see a visible hole or secretions and you cannot feel air escaping.
Are there any possible complications?
Sometimes there can be complications with the stoma healing; these can include the following:
What is over granulation tissue?
Overgranulation tissue is when the body tries to heal itself too much. This can cause varying sizes of extra tissue to be grown around the stoma. This can look like small bobble like growths. This does happen sometimes and is nothing to be alarmed by.
How long do you stay in the hospital after a tracheostomy?from mayoclinic.org
After the tracheostomy procedure, you'll likely stay in the hospital for several days as your body heals. If possible, plan ahead for your hospital stay by bringing: A communication method, such as a pencil and a pad of paper, a smartphone, or a computer, as you'll be unable to talk at first.
When is a tracheostomy performed?from mayoclinic.org
In rare cases, an emergency tracheotomy is performed when the airway is suddenly blocked, such as after a traumatic injury to the face or neck. When a tracheostomy is no longer needed, it's allowed to heal shut or is surgically closed. For some people, a tracheostomy is permanent. Mayo Clinic's approach.
How to get rid of tracheostomy secretions?from mayoclinic.org
Putting small amounts of saline directly into the tracheostomy tube, as directed, may help loosen secretions. Or a saline nebulizer treatment may help. A device called a heat and moisture exchanger captures moisture from the air you exhale and humidifies the air you inhale.
How is a tracheostomy tube inserted?from mayoclinic.org
A tracheostomy tube is inserted through the hole and secured in place with a strap around your neck. Tracheostomy (tray-key-OS-tuh-me) is a hole that surgeons make through the front of the neck and into the windpipe (trachea). A tracheostomy tube is placed into the hole to keep it open for breathing. The term for the surgical procedure ...
What is a tracheostomy tube?from mayoclinic.org
Overview. A tracheostomy is a surgically created hole (stoma) in your windpipe (trachea) that provides an alternative airway for breathing. A tracheostomy tube is inserted through the hole and secured in place with a strap around your neck. Tracheostomy (tray-key-OS-tuh-me) is a hole that surgeons make through the front ...
Why do we need a tracheostomy?from mayoclinic.org
A tracheostomy is often needed when health problems require long-term use of a machine (ventilator) to help you breathe. In rare cases, an emergency tracheotomy is performed when the airway is suddenly blocked, ...
Why do nurses clean tracheostomy tubes?from mayoclinic.org
A nurse will teach you how to clean and change your tracheostomy tube to help prevent infection and reduce the risk of complications. You'll continue to do this as long as you have a tracheostomy.

Overview
Why It's Done
- Situations that may call for a tracheostomy include: 1. Medical conditions that make it necessary to use a breathing machine (ventilator) for an extended period, usually more than one or two weeks 2. Medical conditions that block or narrow your airway, such as vocal cord paralysis or throat cancer 3. Paralysis, neurological problems or other condit...
Risks
- Tracheostomies are generally safe, but they do have risks. Some complications are particularly likely during or shortly after surgery. The risk of such problems greatly increases when the tracheotomy is performed as an emergency procedure. Immediate complications include: 1. Bleeding 2. Damage to the trachea, thyroid gland or nerves in the neck 3. Misplacement or displ…
How You Prepare
- How you prepare for a tracheostomy depends on the type of procedure you'll undergo. If you'll be receiving general anesthesia, your doctor may ask that you avoid eating and drinking for several hours before your procedure. You may also be asked to stop certain medications.
What You Can Expect
- During the procedure
A tracheotomy is most commonly performed in an operating room with general anesthesia, which makes you unaware of the surgical procedure. A local anesthetic to numb the neck and throat is used if the surgeon is worried about the airway being compromised from general anesthesia or i… - After the procedure
You'll likely spend several days in the hospital as your body heals. During that time, you'll learn skills necessary for maintaining and coping with your tracheostomy: 1. Caring for your tracheostomy tube.A nurse will teach you how to clean and change your tracheostomy tube to h…
Results
- In most cases, a tracheostomy is temporary, providing an alternative breathing route until other medical issues are resolved. If you need to remain connected to a ventilator indefinitely, the tracheostomy is often the best permanent solution. Your health care team will help you determine when it's appropriate to remove the tracheostomy tube. The hole may close and heal on its own…