
Is COPD a painful death?
Ideally, this research will provide wisdom needed to help physicians help their patients live better and longer with COPD. Again, COPD is not generally considered a painful disease, although it may be associated with pain, even chronic pain.
Is COPD a terminal disease?
COPD is not a terminal illness but a chronic disease that gets worse over time . Although there is no cure for COPD, the illness can be successfully managed especially if it’s recognized early. Studies have shown that the rate at which the lung function of COPD patients decreases can be reduced if a diagnosis is made in the early stages of ...
What is the prognosis for COPD?
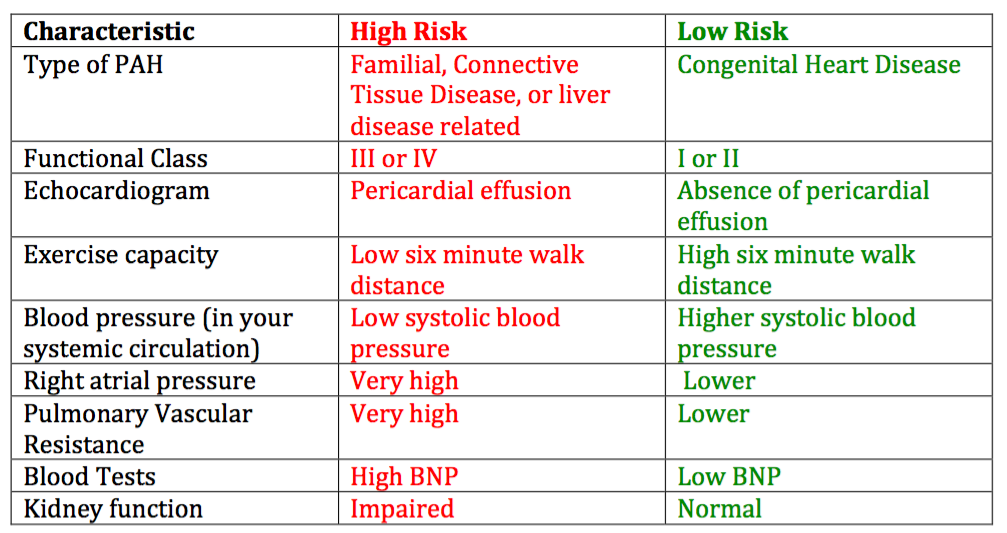
Summary COPD is a heterogeneous disease without a simple prognostic trajectory. For ambulatory patients, age, degree of dyspnea, weight loss (BMI), functional status, and FEV1 are relevant prognostic factors for predicting 1-3 year survival. For hospitalized patients, the same factors are relevant.
How do you die from COPD?
Most patients that die of COPD die of a complication such ad penumonia or pulmonary embolism. It is true that you can die of copd. The leading cause of death however across all stages of the disease is coronary artery disease (ie heart attack). Most patients that die of COPD die of a complication such ad penumonia or pulmonary embolism.

When did COPD become a diagnosis?
William Briscoe is believed to be the first person to use the term COPD in discussion at the 9th Aspen Emphysema Conference. This term became established and today we refer to COPD as the designation of this growing health problem (Briscoe and Nash 1965).
What was COPD originally called?
The term “chronic obstructive pulmonary disease” (COPD) came into use gradually in the 1960s and 1970s replacing the previous term “chronic bronchitis and emphysema” (CB&E).
What is the natural history of COPD?
Lung function decline is part of the natural history of COPD and is strongly predictive of COPD-related morbidity and mortality. However, many other factors also influence COPD outcome.
How is COPD identified?
COPD is diagnosed using a simple breathing test called spirometry.
Do non smokers get COPD?
Smoking, asthma, or air pollution account for many COPD cases, but up to 30% of cases occur in people who never smoked, and only a minority of heavy smokers develop the disease, suggesting that there are other risk factors at play.
What 3 diseases make up COPD?
Chronic obstructive pulmonary disease, or COPD, refers to a group of diseases that cause airflow blockage and breathing-related problems. It includes emphysema and chronic bronchitis. COPD makes breathing difficult for the 16 million Americans who have this disease.
What are the 4 major risk factors of COPD?
Risk factors for COPD include:Exposure to tobacco smoke. The most significant risk factor for COPD is long-term cigarette smoking. ... People with asthma. ... Occupational exposure to dusts and chemicals. ... Exposure to fumes from burning fuel. ... Genetics.
What are the main causes of COPD?
Smoking is the main cause of COPD and is thought to be responsible for around 9 in every 10 cases. The harmful chemicals in smoke can damage the lining of the lungs and airways. Stopping smoking can help prevent COPD from getting worse.
Is COPD a progressive disease?
COPD, or chronic obstructive pulmonary disease, is a progressive disease, which means it gets worse over time. With COPD, less air flows in and out of the airways, making it hard to breathe.
Why do you not give oxygen to COPD patients?
Too much oxygen can be dangerous for patients with chronic obstructive pulmonary disease (COPD) with (or at risk of) hypercapnia (partial pressure of carbon dioxide in arterial blood greater than 45 mm Hg). Despite existing guidelines and known risk, patients with hypercapnia are often overoxygenated.
Can lungs heal from COPD?
There's currently no cure for chronic obstructive pulmonary disease (COPD), but treatment can help slow the progression of the condition and control the symptoms.
How long do people live with COPD?
Many people will live into their 70s, 80s, or 90s with COPD.” But that's more likely, he says, if your case is mild and you don't have other health problems like heart disease or diabetes. Some people die earlier as a result of complications like pneumonia or respiratory failure.
What is another name for COPD?
Emphysema is one of the two most common conditions that fall under the umbrella term chronic obstructive pulmonary disease (COPD). The other major COPD condition is chronic bronchitis.
Did COPD used to be called emphysema?
Earliest references to COPD They described cases in which the lungs were “turgid”, particularly from air. Baillie in 1789 published a series of illustrations of the emphysematous lung putting forth the pathology of the disease. Thus emphysema was known to be a part of COPD early one.
How long do people live with COPD?
Many people will live into their 70s, 80s, or 90s with COPD.” But that's more likely, he says, if your case is mild and you don't have other health problems like heart disease or diabetes. Some people die earlier as a result of complications like pneumonia or respiratory failure.
What are the two types of COPD?
Having COPD makes it hard to breathe. There are two main forms of COPD: Chronic bronchitis, which involves a long-term cough with mucus. Emphysema, which involves damage to the lungs over time.
Who discovered emphysema?
The first credible production of emphysema was by Gross in 1964, who instilled pancreatic extracts (papain) into the airways of guinea pigs to cause destruction of alveoli and hyperinflation (Gross et al 1964). This was somewhat of a fortuitous discovery, since he was not trying to produce emphysema, but was hoping to determine the effect of papain on the fibrosis associated with experimental silicosis that he was studying. Gross’s work produced emphysema, due to proteolytic damage of elastin and thus was the forerunner of the protease – antiprotease therapy of the pathogenesis, as described by Laurel and Erickson (1963)in Sweden with alpha-one-antitrypsin deficiency and emphysema. Other investigations also used elastases to produce experimental emphysema (Snider and Sherter 1977). Many genetic, infectious, and immunologic models in small animals followed and continue to be investigated at the present time. A recent model employing methylprednisolone to produce emphysema in rats induces matrix metalloproteinase and can be prevented by a metal proteinase inhibitor (Choe et al 2003). The concept that emphysema is an autoimmune vascular disease has been offered as one pathway in pathogenesis (Voelkel and Taraseviciene-Stewart 2005). Studies in experimental emphysema, though possibly species specific, are useful in suggesting new therapeutic targets.
What is the acronym for COPD?
Other acronyms that predated the COPD designation were chronic obstructive bronchopulmonary disease, chronic airflow obstruction, chronic obstructive lung disease, nonspecific chronic pulmonary disease, and diffuse obstructive pulmonary syndrome. William Briscoe is believed to be the first person to use the term COPD in discussion at the 9th Aspen Emphysema Conference. This term became established and today we refer to COPD as the designation of this growing health problem (Briscoe and Nash 1965).
What was the 9th conference on COPD?
This conference may have been the “tipping point” in the establishment of comprehensive treatment for COPD (Petty 1967). Because of the success of the 8th conference, the 9th, 10th, and 11th conferences were held annually at the same venue. These three conferences dealt with the mushrooming advances in research in COPD during that era. At the 9th conference Ben Burrows and Charles Fletcher presented their concept of “The bronchial and emphysematous types of chronic obstructive lung disease in London and Chicago”, pointing out that the same disease spectrum was found on both sides of the Atlantic. This work was also published elsewhere (Burrows et al 1966). Fletcher gave his initial findings on “Prognosis in chronic bronchitis”.
What is the fourth most common cause of death in the USA?
COPD includes chronic bronchitis, emphysema, and chronic asthmatic bronchitis (defined further below). Today, COPD is the fourth most common cause of death in the USA, and is the only disease state that is rising in morbidity and mortality amongst the top five killers.
Which doctor described a combination of emphysema and chronic bronchitis?
The bronchus of the trachea are often at the same time a good deal filled with mucous fluid (Laënnec 1821, p 89). Thus Laënnec had described a combination of emphysema and chronic bronchitis. John Hutchinson invented the spirometer in 1846 (Hutchinson 1846).
What did Osler believe about emphysema?
Osler’s Principles and practices of medicine(1916)says little about emphysema. Osler believed emphysema was caused by excessive pressure in the alveoli (Osler 1916), and reference to the spirometer cannot be found in this classic text. In 1912, another author did not mention spirometry, but shows a nice picture of the sphygmomanometer, invented by Rico Rossi in 1896, and excellent quality EKG strips are shown (Bovard 1912). This occured 50 years after Hutchinson’s invention. A textbook of Disease in the chestin 1918 makes only brief mention of spirometry with no illustrations (Norris and Landis 1918).
Why were corticosteroids never used?
Corticosteroids were almost never used, even in cases of exacerbations of COPD. One paper in the early 1960s by Noehren, offered new hope that at least some treatments might be beneficial in emphysema.
How long has COPD been around?
Chronic obstructive pulmonary disease (COPD) has been known to mankind for over 200 year . The disease was initially recognized with the use of the stethoscope and spirometer and spirometry still remains the most effective means of identification and assessment of the course of COPD and responses to therapy.
What is COPD in medical terms?
The American Thoracic Society defined chronic bronchitis in clinical terms including chronic cough lasting at least three months for at least two years.
When was emphysema discovered?
It was corroborated around a century later in 1769 by Morgagni. They described cases in which the lungs were “turgid”, particularly from air. Baillie in 1789 published a series of illustrations of the emphysematous lung putting forth the pathology of the disease. Thus emphysema was known to be a part of COPD early one.
What is the name of the drug that took over atropine?
There has also been the advent of antimuscarinic agents like tiotropium and ipratropium that took over initially used atropine. Oxygen therapy and pulmonary rehabilitation also developed over the last half of the 20 th century.
What is the treatment for COPD?
Treatment of COPD. Earlier the only therapies for COPD were antibiotics for pneumonia, a mucus thinner called potassium iodide and bronchodilators like ephedrine, theophylline etc. There were in addition sedatives to deal with the side effects of ephedrine.
Who was the inventor of the stethoscope?
Laënnec described emphysema of the lungs in 1821 in his Treatise of diseases of the chest. He was the inventor of the stethoscope who wrote that emphysema lungs were excessively inflated that did not empty well. Laënnec went on to describe a combination of emphysema and chronic bronchitis.
Who invented the spirometer?
Laënnec went on to describe a combination of emphysema and chronic bronchitis. It was in 1846 that John Hutchinson invented the spirometer. This was the key to diagnosing COPD. The spirometer is still used today for diagnosis and regular assessment regarding response to therapy in COPD.
How to treat COPD?
Treating your COPD can greatly improve your quality of life. Treatment options that your doctor may consider include: 1 Quitting smoking. For people who smoke, the most important aspect of treatment is to stop smoking. 2 Avoiding tobacco smoke and other air pollutants at home and at work. 3 Medication. Symptoms such as coughing or wheezing can be treated with medication. 4 Pulmonary rehabilitation, a personalized treatment program that teaches you how to manage your COPD symptoms to improve quality of life. Plans may include learning to breathe better, how to conserve your energy, and advice on food and exercise. 5 Avoiding lung infections. Lung infections can cause serious problems in people with COPD. Certain vaccines, such as flu and pneumonia vaccines, are especially important for people with COPD. Learn more about vaccination recommendations. Respiratory infections should be treated with antibiotics, if appropriate. 6 Supplemental oxygen from a portable oxygen tank may be needed if blood oxygen levels are low.
How many people have COPD?
Chronic obstructive pulmonary disease (COPD), which includes emphysema and chronic bronchitis, makes breathing difficult for the 16 million Americans who have been diagnosed with COPD. Millions more suffer from COPD, but have not been diagnosed and are not being treated.
What is the purpose of pulmonary rehabilitation?
Pulmonary rehabilitation helps improve COPD symptoms and allows you to be active without shortness of breath.
What is the treatment for COPD?
Medication. Symptoms such as coughing or wheezing can be treated with medication. Pulmonary rehabilitation, a personalized treatment program that teaches you how to manage your COPD symptoms to improve quality of life.
Can COPD cause lung infections?
Lung infections can cause serious problems in people with COPD. Certain vaccines, such as flu and pneumonia vaccines, are especially important for people with COPD. Learn more about vaccination recommendations. Respiratory infections should be treated with antibiotics, if appropriate.
Could you have COPD?
The main cause of COPD is tobacco smoke, so if you smoke or used to smoke, you are at a higher risk of having COPD . Exposure to air pollution in the home or at work, family history, and respiratory infections like pneumonia also increase your risk.
How many genome-wide associations are there for COPD?
International COPD Genetics Consortium and UK Biobank genome-wide association studies for COPD. Manhattan plot demonstrating 82 genome-wide significant associations to COPD. Novel associations (not previously reported for COPD or lung function) are labeled with the nearest gene, and replication in the SpiroMeta cohort for lung function phenotypes is indicated. Adapted with permission from Reference 27.
How to understand COPD heterogeneity?
Studying genetic determinants of COPD-related phenotypes is one approach to understand COPD heterogeneity. An alternative is to define COPD subtypes using machine learning, imaging patterns, or other clinical features, and then to assess genetic associations to those subtypes. Castaldi and colleagues (50) used K-means clustering to define four COPD subtypes based on FEV1 (% predicted), emphysema at −950 HU, emphysema distribution (upper lung field/lower lung field), and segmental airway wall area. A cluster with mild upper lung–predominant emphysema was associated with an SNP near HHIP, while a severe emphysema cluster was most strongly associated with the chromosome 15q25 locus.
What is the long-range interaction between the COPD GWAS region and HHIPpromoter?
Chromosome conformation capture assay demonstrated a 7-kb region of interaction upstream from the HHIPgene with the HHIPpromoter. This upstream interacting genomic region is located within a frequently replicated COPD GWAS locus. Abbreviation: GWAS, genome-wide association study. Adapted with permission from Reference 29.
What are the phenotypes of chest CT?
Chest CT phenotypes are especially promising assessments to understand COPD heterogeneity, as the presence, severity, distribution, and pattern of emphysema can be determined. Manichaikul and colleagues (45) analyzed quantitative CT emphysema in a multiethnic general population sample of 7,914 subjects, the MESA (Multi-Ethnic Study of Atherosclerosis) Lung Study. They found genome-wide significant associations near SNRPFand PPT2. With additional fine mapping, the most strongly associated SNP in the PPT2region was located within an intron of the AGERgene. AGERencodes the sRAGE protein biomarker, which has been strongly associated with emphysema (46). Cho and colleagues (47) performed GWAS of chest CT phenotypes in the COPDGene, ECLIPSE, GenKOLS, and NETT studies. Five genome-wide significant associations with quantitative emphysema (percentage of low attenuation areas below −950 HU) were identified, including two previously identified COPD GWAS loci (HHIPand CHRNA3). The AGERregion, previously associated with lung function, was also associated with quantitative emphysema, and it was subsequently associated with COPD in the ICGC analysis (26). A region near the SERPINA1gene was also associated with emphysema, and it appeared to be driven by the Z allele; thus, with a highly specific phenotype (CT emphysema), even rare variants of large effect can be identified in genetic association studies. In addition, a region near DLC1, which has not been associated with lung function levels, was implicated in emphysema. Finding genetic determinants of CT airway wall phenotypes has been more challenging than emphysema phenotypes, potentially because only relatively large airways can be visualized due to the limits of CT resolution.
What can we expect to learn from large-scale whole genome sequencing studies of COPD?
Importantly, association of rare variants with COPD and COPD-related phenotypes will be enabled. In addition, these whole genome sequencing data will provide insights into genetic determinants of omics data types collected on the same subjects, which will empower systems and network-based analyses.
Is COPD a heritable disease?
Although COP D GWA S have identified multiple genome-wide significant associations, much of the estimated heritability for COPD remains unexplained. This missing heritability could be related to common variants of very small effect and/or rare variants of either small or large effect. One of the most interesting findings in COPD GWAS is the identification of five genomic regions that are also associated with idiopathic pulmonary fibrosis (IPF), but with opposite directions of effect (the risk allele for COPD protects from IPF and vice versa) (27). Although risk for both of these pulmonary diseases is influenced by cigarette smoking, these genetic clues could point to molecular switches that influence the distinct pathological patterns of COPD and IPF.
Is smoking a cigarette a determinant of COPD?
Although chronic obstructive pulmonary disease (COPD) risk is strongly influenced by cigarette smoking, genetic factors are also important determinants of COPD. In addition to Mendelian syndromes such as alpha-1 antitrypsin deficiency, many genomic regions that influence COPD susceptibility have been identified in genome-wide association studies. Similarly, multiple genomic regions associated with COPD-related phenotypes, such as quantitative emphysema measures, have been found. Identifying the functional variants and key genes within these association regions remains a major challenge. However, newly identified COPD susceptibility genes are already providing novel insights into COPD pathogenesis. Network-based approaches that leverage these genetic discoveries have the potential to assist in decoding the complex genetic architecture of COPD.
What causes COPD?
People with COPD are at increased risk of developing heart disease, lung cancer and a variety of other conditions.
What is COPD in a lung?
Overview. Chronic obstructive pulmonary disease (COPD) is a chronic inflammatory lung disease that causes obstructed airflow from the lungs. Symptoms include breathing difficulty, cough, mucus (sputum) production and wheezing. It's typically caused by long-term exposure to irritating gases or particulate matter, most often from cigarette smoke.
Why do my lungs lose air?
Your lungs rely on the natural elasticity of the bronchial tubes and air sacs to force air out of your body. COPD causes them to lose their elasticity and over-expand, which leaves some air trapped in your lungs when you exhale.
How to prevent COPD?
The majority of cases are directly related to cigarette smoking, and the best way to prevent COPD is to never smoke — or to stop smoking now .
Which disease is more likely to cause lung cancer?
Lung cancer. People with COPD have a higher risk of developing lung cancer.
What causes airway obstruction?
Causes of airway obstruction. Causes of airway obstruction include: Emphysema. This lung disease causes destruction of the fragile walls and elastic fibers of the alveoli. Small airways collapse when you exhale, impairing airflow out of your lungs. Chronic bronchitis.
What is the color of cough?
A chronic cough that may produce mucus (sputum) that may be clear, white, yellow or greenish
Join over 52,000 people on COPD360social
COPD360social is the free online social community about everything COPD. Members can share thoughts and ideas, ask questions, give and receive support, discuss what matters to them, and learn how to take action.
Our Education and Support Framework
The COPD Foundation’s Education and Support Framework is positioned at the intersection of the patient, caregiver and health care provider communities.
About COPD360: Our Research Framework
The COPD Foundation Research Framework (COPD360) strategically aligns the goals of all COPD stakeholders: patients, health care professionals, caregivers, academic, government and industry partners.
Earliest References to COPD
Definition of COPD
- The CIBA Guest Symposium in 1959 and the American Thoracic Society Committee on Diagnostic Standards in 1962 were the first to describe the definition of COPD. 1. The American Thoracic Society defined chronic bronchitis in clinical terms including chronic cough lasting at least three months for at least two years. 2. The American Thoracic Society defined emphysem…
Treatment of COPD
- Earlier the only therapies for COPD were antibiotics for pneumonia, a mucus thinner called potassium iodide and bronchodilators like ephedrine, theophylline etc. There were in addition sedatives to deal with the side effects of ephedrine. It was in 1960’s that isoproterenol – a selective beta 2 agonist was used. Corticosteroids were almost never used and oxygen was not …
Further Reading