Why is malignant melanoma cancer so dangerous?
Melanoma is much less common than some other types of skin cancers. But melanoma is more dangerous because it’s much more likely to spread to other parts of the body if not caught and treated early. Where do skin cancers start? Most skin cancers start in the top layer of skin, called the epidermis. There are 3 main types of cells in this layer:
What is the prognosis of malignant melanoma?
almost all people (almost 100%) will survive their melanoma for 1 year or more after they are diagnosed; around 90 out of every 100 people (around 90%) will survive their melanoma for 5 years or more after diagnosis; more than 85 out of every 100 people (more than 85%) will survive their melanoma for 10 years or more after they are diagnosed
Is malignant melanoma totally curable?
Most early malignant melanomas are macular and grow in diameter for some time before they become elevated. Macular lesions are almost always curable, whereas lesions that develop plaques, papules, or nodules have a greater risk for metastases.
What does malignant melanoma look like, visual signs?
Possible signs and symptoms of melanoma. The most important warning sign of melanoma is a new spot on the skin or a spot that is changing in size, shape, or color. Another important sign is a spot that looks different from all of the other spots on your skin (known as the ugly duckling sign).

How serious is lentigo maligna melanoma?
Lentigo maligna melanoma has a mortality rate similar to that of other melanoma types if depth of the tumor is taken into account. The overall prognosis is good for patients with localized melanoma and no nodal or distant metastases.
Can lentigo maligna melanoma be removed?
Because it grows slowly it can take years to develop. Similar to melanoma in situ, lentigo maligna has not spread and is only in the top layer of skin. Both melanoma in situ and lentigo maligna are cured with surgery. However if not treated with appropriate surgery, they can develop into an invasive cancer.
Is lentigo maligna curable?
With sufficiently early diagnosis and treatment, lentigo maligna and lentigo maligna melanoma are both curable forms of skin cancer. The key to treatment is catching the cancer as early as possible and preventing it from spreading to other areas of the body.
Is lentigo melanoma cancerous?
Lentigo maligna (LM) and lentigo maligna melanoma (LMM) are types of skin cancer. They begin when the melanocytes in the skin grow out of control and form tumors. Melanocytes are the cells responsible for making melanin, the pigment that determines the color of the skin.
How long does it take for lentigo melanoma to spread?
In fact, a 2020 study in Melanoma Research found that it takes about 28.3 years on average for a precancerous lesion (called lentigo maligna) to turn into a cancerous lentigo maligna melanoma.
How fast does lentigo melanoma grow?
It grows slowly in diameter over 5 to 20 years or longer. Lentigo maligna melanoma is diagnosed when the melanoma cells have invaded into the dermis and deeper layers of skin. Lentigo maligna has a lower rate of transformation to invasive melanoma than the other forms of melanoma in situ (under 5% overall).
How long do you live after being diagnosed with melanoma?
5-year relative survival rates for melanoma skin cancerSEER stage5-year relative survival rateLocalized99%Regional68%Distant30%All SEER stages combined93%Mar 1, 2022
Should I worry about melanoma in situ?
In situ melanomas don't spread to other parts of the body or cause death, but if the tumor has an opportunity to grow even one millimeter deep into the skin, it can lead to more involved treatment and greater danger. If left untreated, it can metastasize and even become life-threatening.
What is the difference between lentigo and lentigo maligna?
Lentigo maligna (LM), first described by Hutchinson in 1890, is the noninvasive counterpart to lentigo maligna melanoma (LMM). The latter (LMM) refers to invasive melanoma associated with a LM. LM and LMM occur on chronically sun-damaged skin, most commonly on the head and neck.
How do you biopsy lentigo maligna?
Excisional biopsy is ideal for diagnosis of lentigo maligna [40]. In theory, excisional biopsy removes the whole clinical lesion down to subcutaneous fat with a 1–3 mm margin. This potentially allows for complete evaluation of depth and peripheral involvement.
Is lentigo maligna slow growing?
Lentigo maligna (LM) is a slow-growing subtype of melanoma that often occurs on chronically sun-damaged skin, particularly the head and neck, in the elderly.
Does melanoma in situ come back?
Melanoma in situ is usually cured with simple surgery. The prognosis is normally excellent. It is very rare for them to come back because they were 'in situ', therefore they will not usually have had an opportunity to spread elsewhere in the body.
Is lentigo maligna the same as melanoma in situ?
Lentigo maligna is a type of melanoma in situ. It is a slow growing lesion that appears in areas of skin that get a lot of sun exposure, such as the face or upper body. Because it grows slowly it can take years to develop.
How do you biopsy lentigo maligna?
Excisional biopsy is ideal for diagnosis of lentigo maligna [40]. In theory, excisional biopsy removes the whole clinical lesion down to subcutaneous fat with a 1–3 mm margin. This potentially allows for complete evaluation of depth and peripheral involvement.
Is lentigo maligna fast growing?
Lentigo maligna (LM) is a slow-growing subtype of melanoma that often occurs on chronically sun-damaged skin, particularly the head and neck, in the elderly.
What is the difference between lentigo and lentigo maligna?
Lentigo maligna (LM), first described by Hutchinson in 1890, is the noninvasive counterpart to lentigo maligna melanoma (LMM). The latter (LMM) refers to invasive melanoma associated with a LM. LM and LMM occur on chronically sun-damaged skin, most commonly on the head and neck.
What is the difference between lentigo maligna and melanoma?
Compared to other types of skin cancer, lentigo maligna and lentigo maligna melanoma are on the larger side. They tend to be at least 6 millimeters (mm) wide and can grow to several centimeters.
How to prevent lentigo malignant melanoma?
The best way to prevent lentigo malignant melanoma is to limit your exposure to UV rays from the sun and tanning beds. When you do spend time in the sun , use a high-SPF sunscreen and wear a large hat that protects your face and neck.
What are the risk factors for lentigo maligna?
Other risk factors for developing lentigo maligna melanoma include: fair or light skin. family history of skin cancer. being male. being over 60 years old. having a history of noncancerous or precancerous skin spots.
How to tell if lentigo maligna is cancerous?
It can be hard to tell lentigo maligna melanoma from a freckle or age spot by looking at it. To help, you can use a trick known as the “ABCDEs” of skin cancer. If the spot is cancerous, it likely has the following symptoms: A symmetry: The two halves of the spot don’t match.
What is lentigo maligna?
Lentigo maligna melanoma is a type of invasive skin cancer. It develops from lentigo maligna, which is sometimes called Hutchinson’s melanotic freckle. Lentigo maligna stays on the outer surface of the skin. When it starts growing beneath the skin’s surface, it becomes lentigo maligna melanoma. It’s the least common type of melanoma.
Can you remove lentigo maligna?
Surgery to remove lentigo maligna melanoma may have cosmetic complications because it usually occurs on highly visible areas such as the face. Tell your doctor if you’re worried about this. Depending on where the cancer is, they may be able to minimize the scar using a variety of surgical techniques.
Is lentigo maligna melanoma more likely to return after surgery?
Lentigo maligna melanoma is more likely to return after nonsurgical treatment than it is after surgical treatment, so it’s important to regularly follow up with your doctor and monitor the affected area for any changes.
What is lentigo maligna?
Lentigo maligna is a precursor to lentigo maligna melanoma, a potentially serious form of skin cancer. Lentigo maligna is also known as Hutchinson melanotic freckle.
What are the characteristics of lentigo maligna?
The characteristics of lentigo maligna include: Large size: >6 mm and often several centimetres in diameter at diagnosis. Irregular shape.
What tests should be done if I have lentigo maligna?
It is essential to diagnose lentigo maligna and lentigo maligna melanoma accurately. Clinical diagnosis is aided by dermoscopy and in some centres, by confocal microscopy. New techniques are being evaluated to help identify the margin of lentigo maligna prior to excision biopsy.
What is the outlook for patients with melanoma?
Lentigo maligna is not dangerous; it only becomes potentially life threatening if an invasive melanoma develops within it.
How much margin is needed for melanoma in situ?
The ideal margin for all forms of melanoma in situ is 5-10mm, depending on how well defined are the edges of the lesion.
How much margin is needed for a biopsy of lentigo maligna?
If a skin lesion is clinically suspicious of lentigo maligna, it is best cut out ( excision biopsy) with a 2–3 mm margin. Partial biopsy is less accurate than complete excision biopsy, as a single small biopsy could miss a malignant focus.
How many invasive melanomas were diagnosed in 2008?
According to New Zealand Cancer Registry data, 2256 invasive melanomas were diagnosed in 2008 and about 10% were pathologically lentigo maligna melanoma. Rates of the precursor, lentigo maligna, are not reported by national cancer registries but it is thought to be the most common variant of melanoma in situ in New Zealand and Australia.
What is LMM in skin?
LMM refers to the disease after it has grown deeper into the skin and is considered invasive. Together, LM and LMM account for about 4 to 15 percent of the melanomas diagnosed worldwide. LM and LMM usually form on the face, ears, or neck of elderly people with sun-damaged skin. They often cause a blotchy appearance.
What is a LMM?
Lentigo Maligna Melanoma. Kishwer Nehal is one of the country’s foremost experts in lentigo maligna and lentigo maligna melanoma. Lentigo maligna (LM) and lentigo maligna melanoma (LMM) are types of skin cancer. They begin when the melanocytes in the skin grow out of control and form tumors.
Is LM a curable disease?
LM and LMM are highly curable when diagnosed early. The goals of treatment are to: cure the cancer. preserve the appearance of your skin. prevent the cancer from coming back. The extent and depth of the melanoma guides your care plan.
What is the risk of LM/LMM?
The major risk factor for developing LM/LMM is ultraviolet radiation (UVR), particularly cumulative lifetime UVR exposure. [6][7][8][9] Several studies have demonstrated that LM/LMM is strongly associated with chronic UVR exposure, as opposed to nodular melanoma (NM) and superficial spreading melanoma (SSM), which are associated with intense intermittent UVR exposure. [7][8][9][10][11][12][13][14] An Australian study showed an increased risk of LM with the number of years lived in Australia, hours of sunlight, amount of actinic damage, and prior history of nonmelanoma skin cancer.[9] LM/LMM is also most likely to occur on the face, a site of chronic sun damage, whereas SSM and NM are more likely to occur on the trunk in men and legs in women, sites which are more often protected.[6] Finally, LM tends to occur in older patients compared to SSM and NM, presumably due to the increased lifetime sun exposure in older individuals. [15][16]
How to prevent LM/LMM?
Due to the causative nature of chronic UVR damage in inducing LM/LMM, diligent sun protection is key to prevention. The American Academy of Dermatology (AAD) periodically publishes guidelines on the prevention and treatment of skin cancer. [59][74] Patients should wear broad-spectrum sunscreen (SPF ≥ 30) whenever outdoors, reapply every 2 hours and immediately after swimming, and use a sufficient amount (approximately 1 ounce or 1 shot-glass equivalent to cover the entire body). Wearing UPF clothing, avoiding the sun between peak hours of 10 am to 3 pm, and seeking shade will provide additional sun protection. Finally, patients should be aware of the ABCDE criteria for melanoma, perform monthly skin self-examinations, and seek professional care by a dermatologist or primary care provider for any concerning lesions.
How long does LM/LMM last?
In a study of 270 patients with LM/LMM that were completely excised, there were zero disease-related deaths for LM and only one for LMM.[71] The 5-year and 10-year disease-specific survival was 100% and 97.1%, respectively. Thus, LM, in itself, does not reduce lifespan. Once the tumor becomes invasive, however, the prognosis is the same as for all other melanomas after controlling for Breslow depth and can be potentially quite poor if the disease becomes metastatic (5-year survival 9-27%). [14][72] While mortality is low, morbidity for patients can be significant, given the potentially large surface area on the head/neck that may be involved and the need for extensive surgical excision and reconstruction. [73]
Is melanoma a slow growing disease?
Lentigo maligna (LM) is a slow-growing subtype of melanoma that often occurs on chronically sun-damaged skin, particularly the head and neck, in the elderly. Due to its clinical and histopathologic mimicry of benign lesions, it is often misdiagnosed for years or even decades, which can lead to increased morbidity and mortality. This activity summarizes the key findings of LM and discusses the unique diagnostic and treatment challenges of this disease.
Is LM a smooth lesion?
Due to its in situ nature, LM is typically smooth and non-palpable. If the lesion becomes invasive (LMM), then a papular or dermal component may be felt. LM exhibits slow radial growth and might be misdiagnosed for years or even decades as solar lentigo or other benign lesions (see Differential Diagnosis section).[5] The overall lifetime risk of progression from LM to LMM has been estimated to be 5% based on a retrospective epidemiologic study.[40] However, the true lifetime risk may be greater, as between 10 to 20% of cases that are initially diagnosed as LM on biopsy are later upstaged to LMM after excision. [41][42][43][44] The timeframe of progression to LMM varies widely, from less than 10 years to more than 50 years. [45][46]
Is LM a genetic condition?
LM is also more likely to occur in genetic conditions that predispose to sun sensitivity, including oculocutaneous albinism, xeroderma pigmentosum, Werner syndrome, and porphyria cutanea tarda.[2] There have been no associations demonstrated with smoking or alcohol. [17]
Can lentigo maligna be metastasized?
Left untreated, lentigo maligna melanoma can eventually metastasize, so early diagnosis and intervention are crucial. Surgery to remove LMM may carry cosmetic complications because it often occurs on exposed areas such as the face; modern surgical techniques can help minimize scarring.
What is Lentigo Maligna?
This is a skin condition, also known as Hutchinson’s melanotic freckle or melanoma in situ. Basically, in parts of the skin that were damaged by the sun, these malignant cells appear without any invasive growth. The progression of the skin condition is very slow and it may remain in the non-invasive form for years.
How to diagnose lentigo melanoma?
Often time, a specialist doctor will prefer to see the affected tissue under a microscope. The whole area will be removed surgically and then it will be sent to a specialized laboratory for further examination. In cases of areas that have grown too extensively, then only a sample will be taken, which is known as a biopsy. This is extremely important, as it can determine whether the malignant cells have breached the border and what course of treatment should be taken.
Can sun exposure cause lentigo melanoma?
As sun exposure is considered to be the main triggering factor, it seems that having periodic severe sunburn episodes is also a favoring factor. If those episodes took place during childhood and they were severe enough for blisters to form on the skin, then that skin was already hurt and predisposed to lentigo melanoma in older years. Last, but not the least, it seems that people with numerous moles on their bodies and especially hairy birthmarks present an increased risk for this skin condition, as there are those who suffer from immune-deficiency.
When to go to the doctor for moles?
Go to the doctor the moment a mole has changed its form, color, growth or if it has started to bleed or ooze.
Is lentigo maligna dangerous?
First of all, you should understand that lentigo maligna is not dangerous, as it evolves slowly over the years but the malignant cells stay within a certain border. However, if they make a turn for melanoma, then the prognosis changes. The prognosis depends on whether the lesions can be removed surgically or not, the efficiency of other treatments and also on the appearance of new, modified lesions. The moment the diagnosis of lentigo maligna melanoma has been made, the prognosis depends on the thickness of the tumor.
What is the most aggressive melanoma?
Nodular melanoma. What you should know: This is the most aggressive type of melanoma. It accounts for 10 to 15 percent of all cases. How and where it grows: The tumor grows deeper into the skin more rapidly than other types and is most frequently found on the torso, legs and arms, as well as the scalp in older men.
What is the survival rate for melanoma?
The estimated five-year survival rate for U.S. patients whose melanoma is detected early is about 99 percent.
What does melanoma look like?
Melanomas present in many different shapes, sizes and colors. That’s why it’s tricky to provide a comprehensive set of warning signs. Since detecting melanoma early is so vital, we’ve provided common signs, symptoms, images and early detection strategies on our Melanoma Warning Signs page.
What is a melanocyte?
Melanocytes are skin cells found in the upper layer of skin. They produce a pigment known as melanin, which gives skin its color. There are two types of melanin: eumelanin and pheomelanin. When skin is exposed to ultraviolet (UV) radiation from the sun or tanning beds, it causes skin damage that triggers the melanocytes to produce more melanin, but only the eumelanin pigment attempts to protect the skin by causing the skin to darken or tan. Melanoma occurs when DNA damage from burning or tanning due to UV radiation triggers changes (mutations) in the melanocytes, resulting in uncontrolled cellular growth.
What is the name of the cancer that spreads beyond the original site?
When this cancer becomes invasive or spreads beyond the original site, the disease is known as lentigo maligna melanoma.
Where does a mole grow?
When it begins in a mole that is already on the skin, it tends to grow on the surface of the skin for some time before penetrating more deeply. While it can be found nearly anywhere on the body, it is most likely to appear on the torso in men, the legs in women and the upper back in both.
Is melanoma a cancer?
A Dangerous Skin Cancer. Melanoma is a serious form of skin cancer that begins in cells known as melanocytes. While it is less common than basal cell carcinoma (BCC) and squamous cell carcinoma (SCC), melanoma is more dangerous because of its ability to spread to other organs more rapidly if it is not treated at an early stage. ...
Where does acral lentiginous melanoma occur?
Acral Lentiginous Melanoma: occurs on palms or soles, or under nails. Lentigo Maligna Melanoma: flat and dark, less invasive. Mucosal Melanoma occurs on mucosal membranes – the moist skin in the mouth, nose, throat, vagina, or anus. Ocular Melanoma is a rare form of melanoma that occurs in the eye.
How to test for melanoma?
1. Biopsy. The doctor will take a small sample (a biopsy) and send it off to a lab for testing. In the lab they will look at the cells in the melanoma and the skin cells around it to determine the type and stage. 2.
How many types of melanoma are there?
There are three main types of melanoma to know about: Cutaneous Melanoma is the one we watch out for at Skin Analytics. It appears in the skin, and is the most common type. There are four types of cutaneous melanoma: Superficial Spreading Melanoma: flat, dark, grows sideways. Nodular Melanoma: raised, bumpy, grows downwards.
What is the name of the cancer that produces pigments?
Melanoma is a cancer of the melanocytes, which are cells that produce a pigment called melanin. Melanin gives colour to the skin, hair and eyes. Melanocytes can also form moles, where melanomas can develop. Although most moles do not become cancerous, it’s important to spot the rare ones that do.
What to do if you are worried about a mole?
If you are worried about a particular mole, it is always good to get it checked by a doctor.
Can melanomas be detected early?
But don’t worry, melanomas most commonly occur on the skin, so if you’re checking regularly, they can be easily detected early.
Can melanoma spread to lymph nodes?
Any spread to lymph nodes; Any spread to other organs. Once melanoma has spread to other parts of the body (known as stage 4), it is called metastatic melanoma, and is very difficult to treat. But, if you regularly keep an eye on your moles melanoma can be easily caught at an early stage.

Classification
Prognosis
- Lentigo maligna grows slowly and is usually harmless, but lentigo maligna melanoma can spread aggressively. Its important to recognize the symptoms of lentigo maligna melanoma so you can seek treatment early on. Untreated lentigo maligna melanoma can eventually spread throughout the body, so identifying it as early is possible is important. The mor...
Symptoms
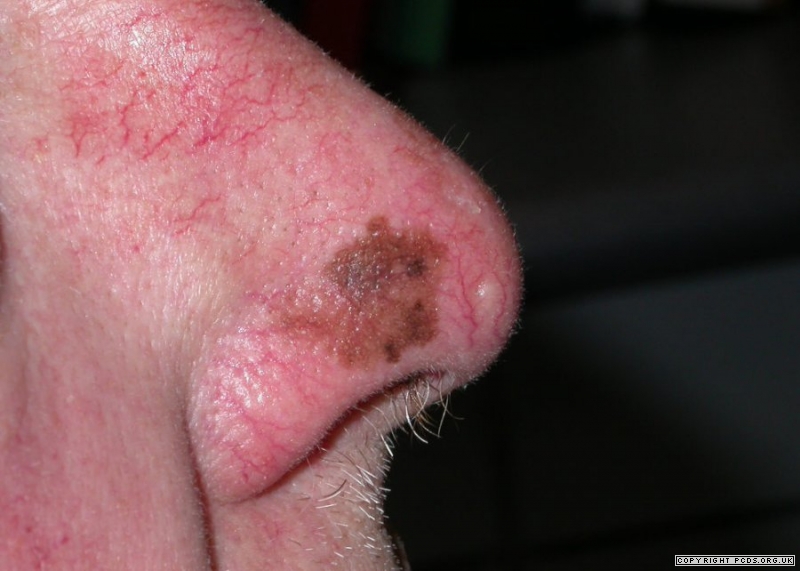
- The visual symptoms of lentigo maligna melanoma are very similar to those of lentigo maligna. Both look like a flat or slightly raised brown patch, similar to a freckle or age spot. They have a smooth surface and an irregular shape. While theyre usually a shade of brown, they can also be pink, red, or white. It can be hard to tell lentigo maligna melanoma from a freckle or age spot by l…
Signs and symptoms
- Compared to other types of skin cancer, lentigo maligna and lentigo maligna melanoma are on the larger side. They tend to be at least 6 millimeters (mm) wide and can grow to several centimeters. Most people with either condition have it on their neck or face, especially their nose and cheeks.
Diagnosis
- Its also hard to visually tell the difference between lentigo maligna and lentigo maligna melanoma. Keep an eye out for these signs that may indicate lentigo maligna melanoma: After reviewing your medical history and doing a physical exam, your doctor may refer you to a dermatologist or other specialist. They may use a dermatoscope, which combines a magnifying …
Causes
- The exact cause of lentigo maligna melanoma is unknown, but sun exposure is the biggest risk factor for developing it. That puts people with sun-damaged skin and those who spend a lot of time outside at a higher risk. Other risk factors for developing lentigo maligna melanoma include:
Treatment
- The most common treatment for lentigo maligna melanoma is to remove the spot with surgery. Lentigo maligna melanoma is more likely to return than some other types of skin cancer, so your doctor may also remove some of the skin surrounding the spot to prevent this. If its spread to your lymph nodes, your doctor may choose to remove those as well. If you have other condition…
Prevention
- The best way to prevent lentigo malignant melanoma is to limit your exposure to UV rays from the sun and tanning beds. When you do spend time in the sun, use a high-SPF sunscreen and wear a large hat that protects your face and neck.