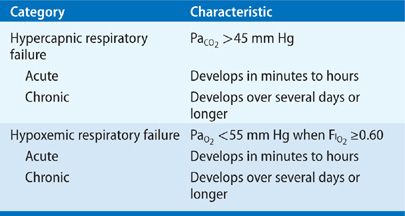
How does COPD affect respiratory failure?
What can COPD cause?
- Respiratory infections. People with COPD are more likely to catch colds, the flu and pneumonia. …
- Heart problems. …
- Lung cancer. …
- High blood pressure in lung arteries. …
- Depression.
Are You at risk of developing COPD?
While we can’t say that COPD is entirely caused by genetics, your risk factor for developing COPD can absolutely be genetic. The most easily recognized genetic risk factor for COPD is alpha-1 antitrypsin (AAT) deficiency. AAT deficiency is passed on to a child at birth by one, or both, parents.
Will you have choking with COPD?
You might find that you have dysphagia if you have COPD. Drooling or choking on food indicates that you have an increased risk for aspiration pneumonia. Yet, aspiration differs from choking. When the airway is blocked by food, drink, or foreign objects, choking happens.
What are the risk factors for respiratory failure?
Risk factors for respiratory failure. – Alterations in the mechanics of the chest wall: severe kyphoscoliosis, obesity, flail injury with multiple rib fractures, paralysis of the thoracic muscle and diaphragm, immobility of the chest wall, as in progressive systemic sclerosis. – Pleural disorders: large pleural fluid, pneumothorax and ...

What type of respiratory failure is COPD?
Type II respiratory failure involves low oxygen, with high carbon dioxide (pump failure). It occurs when alveolar ventilation is insufficient to excrete the carbon dioxide being produced. The most common cause is chronic obstructive pulmonary disease (COPD).
What qualifies as respiratory failure?
Respiratory failure develops when the lungs can't get enough oxygen into the blood. We breathe oxygen from the air into our lungs, and we breathe out carbon dioxide, which is a waste gas made in the body's cells.
What are the three types of respiratory failure?
Acute Respiratory Failure:Type 1 (Hypoxemic ) - PO2 < 50 mmHg on room air. Usually seen in patients with acute pulmonary edema or acute lung injury. ... Type 2 (Hypercapnic/ Ventilatory ) - PCO2 > 50 mmHg (if not a chronic CO2 retainer). ... Type 3 (Peri-operative). ... Type 4 (Shock) - secondary to cardiovascular instability.
What are the two types of respiratory failure?
Type 1 respiratory failure occurs when the respiratory system cannot adequately provide oxygen to the body, leading to hypoxemia. Type 2 respiratory failure occurs when the respiratory system is unable to sufficiently remove carbon dioxide from the body, leading to hypercapnia.
Can you recover from respiratory failure?
Most people who survive ARDS go on to recover their normal or close to normal lung function within six months to a year. Others may not do as well, particularly if their illness was caused by severe lung damage or their treatment entailed long-term use of a ventilator.
Can respiratory failure go away?
There often isn't any cure for chronic respiratory failure, but symptoms can be managed with treatment. If you have a long-term lung disease, such as COPD or emphysema, you may need continuous help with your breathing.
How long can you live with chronic respiratory failure?
The time-to-death is around five years in patients with CWD and slowly progressive NMD, around two to three years in those with OHS and Overlap Syndrome, around one to two years in COPD patients and those with other diseases that lead to chronic hypercapnic respiratory failure.
How is respiratory failure treated?
Treatments for respiratory failure may include oxygen therapy, medicines, and procedures to help your lungs rest and heal. Chronic respiratory failure can often be treated at home. If you have serious chronic respiratory failure, you may need treatment in a long-term care center.
What are the complications of respiratory failure?
Complications of acute respiratory failure may be pulmonary, cardiovascular, gastrointestinal (GI), infectious, renal, or nutritional. Common pulmonary complications of acute respiratory failure include pulmonary embolism, barotrauma, pulmonary fibrosis, and complications secondary to the use of mechanical devices.
What is the most common type of respiratory failure?
Hypoxaemic (type I) respiratory failure Ventilation/perfusion mismatching is the most common mechanism and develops when there is decreased ventilation to normally perfused regions or when there are lung regions with a greater reduction in ventilation than in perfusion.
What is the treatment for type 2 respiratory failure?
You may be treated with therapy called non- invasive ventilation (NIV), sometimes referred to as bi-level positive airways pressure (BiPAP), to help the body get rid of the carbon dioxide.
What does chronic respiratory failure mean?
1 Introduction. Chronic respiratory failure is a condition that results in the inability to effectively exchange carbon dioxide and oxygen, and induces chronically low oxygen levels or chronically high carbon dioxide levels.
What lab values indicate respiratory failure?
One needs to have two of the following three criteria to make a formal diagnosis of acute respiratory failure: pO2 less than 60 mm Hg (hypoxemia). pCO2 greater than 50 mm Hg (hypercapnia) with pH less than 7.35. Signs and symptoms of acute respiratory distress.
What is the difference between respiratory distress and respiratory failure?
As respiratory failure worsens, a person may exhibit no effort to breathe, or stop breathing altogether. People in respiratory distress, by contrast, continue exerting immense effort to breathe.
What is the most common cause of respiratory failure?
Pneumonia, acute respiratory distress syndrome (ARDS), drowning, and other lung diseases can cause this fluid buildup. It can also be caused by heart failure, which is when your heart can't pump enough blood to the rest of your body. Severe head injury or trauma can also cause sudden fluid buildup in the lungs.
What are clinical indicators for acute respiratory failure?
Acute respiratory failure results from acute or chronic impairment of gas exchange between the lungs and the blood causing hypoxia with or without hypercapnia. Patients may present with shortness of breath, anxiety, confusion, tachypnea, cardiac dysfunction, and cardiac arrest.
What are the factors that contribute to NPPV failure?
Another key indicator of failure seems to be the lack of improvement in clinical and gas exchange measures within the first hour after initiation of NPPV (Garpestad et al 2007). There are further predictors for NPPV failure that have been revealed during the last years and might be helpful for the decision on initiation and continuation of NPPV in patients with COPD and ARF (Table 1). Moreover, a number of contraindications such as persistent unconsciousness, hemodynamic instability, gastrointestinal or orofacial bleeding, a high risk for aspiration , or the inability to protect the airways have to be kept in mind when using this technique (Ambrosino et al 2007b) (Table 2).
What is the best way to treat COPD?
Among the non-invasive ventilation techniques, non-invasive positive pressure ventilation (NPPV) via nasal or facial mask or a helmet (Antonelli et al 2004) is meanwhile the therapy of choice for the treatment of acute hypercapnic respiratory failure in acute exacerbations of COPD. However, also negative pressure ventilation (via an iron lung) seems to be effective in avoiding endotracheal intubation and reducing the risk of death (Corrado et al 2002). Even more, also continuous positive airway pressure (CPAP) support – though not being a ventilation in the proper sense of the word – has been proven as useful during ARF in patients with COPD (Dial et al 2006).
What are the prophylactic strategies for COPD?
Naturally, the prophylactic strategies against respiratory failure in COPD comprise the avoidance or reduction of disease progression and the prevention or amelioration of exacerbations by vaccination (Alfageme et al 2006; Wongsurakiat et al 2004), anti-inflammatory therapy (Burge et al 2000), long-acting bronchodilators (Mahler et al 1999; Niewoehner et al 2005), or their combination (Calverley et al 2007). In the presence of an exacerbation the treatment of airway obstruction with bronchodilators (Bach et al 2001), and the administration of systemic steroids (Niewoehner et al 1999) and antibiotics are basic in the management of acute respiratory failure. The practical aspects and therapeutic efficacies of these interventions for treating acute exacerbations have recently been reviewed in detail (MacIntyre et al 2008) and are summarized in the current COPD-update provided by GOLD (Rabe et al 2007).
What is ARF in COPD?
The onset of acute respiratory failure (ARF) in COPD generally marks a serious change in clinical state and is a frequent cause of admissions to emergency and/or intensive care units (ICU). Even more, ARF is also associated with excess mortality both during the hospital stay and in the months following discharge from the hospital (Connors Jr et al 1996; Seneff et al 1995). The long-term prognosis of patients with COPD and ARF particularly worsens if their clinical state calls for a ventilatory support, irrespective of whether this is applied invasively (Connors et al 1996) or non-invasively (Chu et al 2004). Despite these commonalities, the introduction of non-invasive ventilation must be considered as one of the major advances in respiratory medicine, with significant consequences in terms of improved short- and long-term outcome (Plant et al 2003).
Is NPPV effective in COPD?
Despite the reported effectiveness of NPPV in patients with COPD and ARF , it should be noted that the benefit from NPPV critically depends on the degree of hypercapnia and respiratory acidosis. Arterial pH seems to constitute the best marker reflecting both the severity of ARF and the effect of NPPV in the acute setting (Plant et al 2003). In mild exacerbations of COPD (pH > 7.35), NPPV seems to be of limited value and not being well tolerated by the patients, as indicated by a randomized controlled trial (Keenan et al 2005). In accordance with these findings, in patients with very severe ARF (pH < 7.25) the rate of NPPV failure was inversely related to the severity of respiratory acidosis (Ambrosino et al 2008). This indicates that severe acidosis resulting from acute exacerbation is a relevant predictor for treatment failure of NPPV (Plant et al 2001), in addition to being a prognostic factor for mortality per se (Jeffrey et al 1992; Plant et al 2000).
Is ventilation good for COPD?
Patients with advanced COPD and acute or chronic respiratory failure are at high risk for death. Beyond pharmacological treatment, supplemental oxygen and mechanical ventilation are major treatment options. This review describes the physiological concepts underlying respiratory failure and its therapy, as well as important treatment outcomes. The rationale for the controlled supply of oxygen in acute hypoxic respiratory failure is undisputed. There is also a clear survival benefit from long-term oxygen therapy in patients with chronic hypoxia, while in mild, nocturnal, or exercise-induced hypoxemia such long-term benefits appear questionable. Furthermore, much evidence supports the use of non-invasive positive pressure ventilation in acute hypercapnic respiratory failure. It application reduces intubation and mortality rates, and the duration of intensive care unit or hospital stays, particularly in the presence of mild to moderate respiratory acidosis. COPD with chronic hypercapnic respiratory failure became a major indication for domiciliary mechanical ventilation, based on pathophysiological reasoning and on data regarding symptoms and quality of life. Still, however, its relevance for long-term survival has to be substantiated in prospective controlled studies. Such studies might preferentially recruit patients with repeated hypercapnic decompensation or a high risk for death, while ensuring effective ventilation and the patients’ adherence to therapy.
Is COPD a chronic disease?
In COPD, as in other conditions of respiratory illness, respiratory failure can occur as acute, chronic, or acute-on-chronic failure. In addition to ventilation/perfusion inhomogeneities, lung hyperinflation is a major factor in the pathogenesis of hypercapnic respiratory failure, being associated with a flat diaphragm and thereby diminishing muscle efficiency and increasing energy consumption (Calverley 2003). In the chronic setting, patients with COPD often show a rapid shallow breathing. This presumably represents a key protective mechanism to prevent respiratory muscle fatigue, however at the price of an insufficient alveolar ventilation (Roussos et al 2003). In severe COPD with markedly limited functional reserves, acute-on-chronic respiratory failure may aggravate the pre-existing chronic respiratory failure. This can happen when an acute deterioration of whatsoever origin, most often increased airway obstruction during acute exacerbation, poses an additional load on the respiratory system. The pre-existing mechanical disadvantage is further boosted by incomplete emptying of the lungs, leading to air trapping. This promotes a significant intrinsic positive end-expiratory airway pressure (PEEPi) which further aggravates respiratory muscle dysfunction and enhances ventilation-perfusion mismatch (Smith et al 1988).
How many people died from COPD in 2010?
The global incidence of COPD in 2010 was 384 million, affecting 11.7% of the population. 1 Approximately 3 million deaths from COPD occur annually worldwide. 2 The Burden of Obstructive Lung Diseases program, run in 29 countries, found a COPD prevalence of 10.1%, with 11.8% in men and 8.5% in adults over age 40. 3,4.
What are the different types of emphysema?
7 The types are centriacinar (also known as centrilobular), panacinar (also known as panlobular), and localized emphysema (also known as paraseptal). Centriacinar emphysema is associated with cigarette smoking and occurs in the upper lobes and superior segments of the lower lobes. 7 Panacinar emphysema is uniformly distributed within the pulmonary acinus and occurs in basal lung areas. Localized emphysema occurs in isolated areas and is usually found in the apex of the upper lobe. 7,8
What are the factors that contribute to COPD?
Genetic factors, gender, and occupational and environmental exposures to pollutants are risk factors for COPD. Smoking is the leading environmental risk factor for COPD, but less than 40% of smokers develop the disease. 6 Cigarette smoking is a factor in the decline of volume of air exhaled within the first second of forced expiratory volume (FEV 1) related to a dose-response (pack-years). 7 However, the variability of FEV 1 decline is only partially explained by pack-years of smoking. 7,8 Occupational exposure is a risk factor for 19.2% of patients with COPD and 31.1% of never-smokers. 9 Primary occupational dust exposure comes from mining and textile manufacturing. 7
How to assess dyspnea?
Assessing dyspnea requires determining the quality of the discomfort. Scales such as a Modified Borg Dyspnea Scale or visual analogue can measure dyspnea at rest or immediately after an activity. 15 More extensive dyspnea scales are available to determine intensity during many different activities and can determine the extent of disability. 15
What are the risk factors for COPD?
Genetic risk factors include an alpha-1 antitrypsin deficiency, which occurs in 1% to 2% of all patients with COPD. 7 Other genetic factors play a role in the development of COPD; genome studies have identified COPD loci that probably contain susceptibility determinants, but have yet to identify specific genes. 7.
Why does hyperinflation occur in COPD?
Hyperinflation. Occurring in COPD to preserve expiratory airflow because it decreases airway resistance, hyperinflation pushes the diaphragm into a flattened position. 7 This can affect the application of abdominal pressure to the chest wall during inspiration. The shortened diaphragm muscle fibers are less able to generate inspiratory pressures, and the flattened diaphragm has to generate greater tension for the transpulmonary pressure to produce tidal breathing. 7
What is the inflammatory response in COPD?
Inflammation is a key component in the pathophysiology of COPD. 5,7 This inflammation is a modification of the normal respiratory tract inflammatory response. Lung inflammation occurs because of oxidative stress, protease-antiprotease imbalance, inflammatory cells, inflammatory mediators, and/or peribronchiolar and interstitial fibrosis. 5,7 The small airway changes and parenchymal destruction often result in airflow limitation and gas trapping with hyperinflation, gas exchange abnormalities (which include outcomes of hypoxemia and hypercapnia), mucus hypersecretion, and in later stages, pulmonary hypertension from hypoxic vasoconstriction of pulmonary arteries. 7
What is respiratory failure?
Respiratory failure happens when the respiratory system fails to maintain gas exchange and is classified into type 1 and type 2 according to blood gases abnormalities. In type 1 (hypoxemic) respiratory failure, the partial pressure of arterial oxygen (PaO2) is less than 60 millimeters of mercury ...
What happens when blood is shunted?
In cases of a shunt, the deoxygenated blood (mixed venous blood) bypasses the alveoli without being oxygenated and mixes with oxygenated blood that has flowed through the ventilated alveoli, and this leads to hypoxemia as in cases of pulmonary edema (cardiogenic or noncardiogenic), pneumonia and atelectasis.
What is the role of a pharmacist in respiratory care?
Because the patient with respiratory failure is usually on multiple medications, the pharmacist is responsible for ensuring the most appropriate drug is administered without causing drug interactions or severe adverse reactions.
What are some examples of warm extremities?
Warm extremities. Symptoms and signs of the underlying disease. Examples: Fever, cough, sputum production, chest pain in cases of pneumonia. History of sepsis, polytrauma, burn, or blood transfusions before the onset of acute respiratory failure may point to acute respiratory distress syndrome[2].
What is an example of hypoventilation?
Hypoventilation: Depression of CNS from drugs is an example of this condition.
What are the disorders of the peripheralnervoussystem?
Disorders of the peripheralnervoussystem: Respiratory muscle and chest wall weakness as in cases of Guillian-Barre syndrome and myasthenia gravis.
How is oxygen delivered?
Oxygen can be delivered by several routes depending on the clinical situations in which we may use a nasal cannula, simple face mask nonrebreathing mask, or high flow nasal cannula.
What is the difference between Type I and Type II respiratory failure?
Type I respiratory failure - the blood oxygen is low and the carbon dioxide is normal or low. Type II respiratory failure - the blood oxygen is low and the carbon dioxide is high. Respiratory failure can also be described according to the time it takes to develop: Acute - happens within minutes or hours; usually, ...
How is the diagnosis of respiratory failure made?
The diagnosis of respiratory failure requires an arterial blood gas which provides information on the levels of the blood oxygen and carbon dioxide levels. An arterial blood gas simply involves a needle connected to a syringe, which is then inserted at the wrist directly into the point where the pulse can be felt. Sometimes the pulse at the wrist is weakened and so a different site has to be used: this is usually the groin and, less commonly, the elbow.
What are the causes of respiratory failure?
This crosses over into the blood and is then transported to the various organs. At the same time carbon dioxide, which is the waste gas produced by organs, crosses from the blood and into the lungs - we then breathe this out.
What are the systems involved in respiratory failure?
This whole process requires an interplay of various systems such as the lungs, the heart, the chest muscles and the brain. When any of these are impaired we are at risk of respiratory failure. Respiratory failure is defined by low blood oxygen levels and there may also be raised blood carbon dioxide levels.
How long does it take for a lung to become acute?
Acute - happens within minutes or hours; usually, the patient has no underlying lung disease. Chronic - occurs over days and usually there is an underlying lung disease. Acute on chronic - this is usually a sudden or quick worsening of the respiratory function in someone who already has chronic respiratory failure.
Can a patient with respiratory failure be treated at home?
They need to be resuscitated and may need admission to an intensive care unit or the high dependency unit (based on how unwell the patient is) with artificial ventilation and life support. On the other hand many patients with chronic respiratory failure can be treated at home. This will depend on how severe the respiratory failure is, the underlying cause, whether other illnesses are present and the patient's social circumstances. Some patients may need ventilators at home and oxygen support.
Can shortness of breath be caused by exertion?
Shortness of breath - at first, this may happen only on exertion; however, later on it may also occur at rest and when trying to sleep.
Why should Pdx be COPD?
caused the acute respiratory failure.
Is PDX valid for COPD?
The thought that COPD is ‘always’ the PDX is not valid. As stated above, one would have to review the circumstances of each admission and make a determination for each case. There is information available with details that can be cited in AHA Coding Clinic - there are scenarios that address sequencing for ARF with certain conditions.
Can COPD be treated at home?
I would have to review each case individually; some COPD exacerbations are treated at home without any need for additional support - the fact that the patient is seeking support and treatment is provided for the respiratory failure makes me lean toward the failure as the Principal diagnosis. any other thoughts?