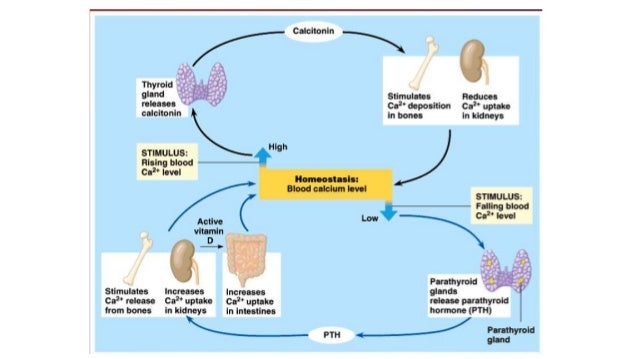
Certain medical conditions can cause hypophosphatemia by:
- decreasing the amount of phosphate your intestines absorb
- increasing the amount of phosphate your kidneys remove into your urine
- moving phosphate from inside the cells to the area outside the cells
- Inadequate phosphate intake.
- Increased phosphate excretion.
- Shift from extracellular phosphate into the intracellular space.
What are the possible complications of hypophosphatemia?
You’re more likely to get hypophosphatemia if you:
- have a parent or other close family member with the condition
- have the blood infection, sepsis
- have hyperparathyroidism
- are severely malnourished because of starvation or anorexia
- are an alcoholic
- take medications such as steroids, diuretics, or antacids in excess or for long periods of time
What are the signs and symptoms of hypophosphatemia?
Symptoms and Signs of Hypophosphatemia Although hypophosphatemia usually is asymptomatic, anorexia, muscle weakness, and osteomalacia can occur in severe chronic depletion. Serious neuromuscular disturbances may occur, including progressive encephalopathy, seizures, coma, and death.
Why does hypoparathyroidism cause hyperphosphatemia?
There are a number of causes of hyperphosphatemia. For example, hereditary or acquired hypoparathyroidism, in which circulating levels of PTH are low or absent, results in the development of hyperphosphatemia, most likely due to increased renal reabsorption of phosphate.
What are the causes of hypoproteinemia?
Other causes of hypoproteinemia include:
- Cirrhosis of liver
- Acute and chronic inflammation
- Drug side effect- Cefpodoxime, Cidofovir, Ibuprofen, Olanzapine, Thalidomide
- Endotoxemia: protein loss is secondary to leakage of protein from the vascular space into interstitial spaces because of increased capillary permeability.
- Extensive burns
- Congestive heart failure
What is the most common cause of hypophosphatemia?
Hypophosphatemia is most often caused by long-term, relatively low phosphate intake in the setting of a sudden increase in intracellular phosphate requirements such as occurs with refeeding. Intestinal malabsorption can contribute to inadequate phosphate intake, especially if coupled with a poor diet.
Which condition can cause hypophosphatemia?
Causes of hypophosphatemia include:severe malnutrition, such as from anorexia or starvation.alcoholism.severe burns.a diabetes complication called diabetic ketoacidosis.the kidney disorder, Fanconi syndrome.an excess of parathyroid hormone (hyperparathyroidism)chronic diarrhea.vitamin D deficiency (in children)More items...
What are symptoms of hypophosphatemia?
Although hypophosphatemia usually is asymptomatic, anorexia, muscle weakness, and osteomalacia can occur in severe chronic depletion. Serious neuromuscular disturbances may occur, including progressive encephalopathy, seizures, coma, and death.
What are the causes of hyperphosphatemia?
Hyperphosphatemia is a serum phosphate concentration > 4.5 mg/dL (> 1.46 mmol/L). Causes include chronic kidney disease, hypoparathyroidism, and metabolic or respiratory acidosis. Clinical features may be due to accompanying hypocalcemia and include tetany.
What is the treatment of hypophosphatemia?
In chronic hypophosphatemia, standard treatment includes oral phosphate supplementation and active vitamin D. Future treatment for specific disorders associated with chronic hypophosphatemia may include cinacalcet, calcitonin, or dypyrimadole.
What is a dangerously low phosphate level?
You may not know that your blood phosphate levels are lower than normal, if they are not life-threateningly low. If your phosphorous levels are below 1.0 mg/dL, your tissues may have more trouble connecting hemoglobin with oxygen - which is critical for breathing.
Does vitamin D increase phosphate?
Vitamin D is known to increase the absorption of calcium and phosphate in the human gut, in order to maintain the calcium homeostasis.
Can hypocalcemia cause hyperphosphatemia?
Short-term complications of hyperphosphatemia include tetany due to hypocalcemia. There can also be deposition of calcium/phosphate in soft tissues, subcutaneous tissues, and joints.
Can low vitamin D cause high phosphorus?
The most striking abnormality in the present case was severe vitamin D deficiency. With vitamin D deficiency, serum phosphorus values usually decrease because of the associated hyperparathyroidism, but hyperphosphatemia has been reported to occur when vitamin D deficiency is severe [1, 6].
What causes hypophosphatemia?
Acute hypophosphatemia is usually the more severe and common type of hypophosphatemia seen in clinical settings. Its causes include: 1 Recovery from diabetic ketoacidosis. Diabetic ketoacidosis happens when someone mismanages their diabetes or might not realize they have it. It is a state that the body goes into when it is unable to produce enough insulin. Insulin is what helps your body break fat down and burn it as fuel. When you go into diabetic ketoacidosis, you have a buildup of acids in your bloodstream, leading to loss of consciousness or even death. 2 Chronic Alcoholism. It is believed that over time, alcoholism hampers your kidney’s ability to absorb phosphorus fully. This is one of the most common causes of hypophosphatemia. Fifty percent of people who are hospitalized due to alcoholism develop hypophosphatemia within the first three days of their hospitalization. 3 Burns. Phosphate is a source of intracellular energy, and when someone experiences a severe burn, their phosphate levels dip dangerously low. Therefore, patients must receive supplemental phosphate to stay healthy. 4 Respiratory alkalosis. This is a decreased amount of carbon dioxide pressure without increased bicarbonate. It usually happens when you hyperventilate or simply breathe in and out too quickly. Respiratory alkalosis causes acute hypophosphatemia because your cells naturally begin to shift around the phosphate stores in your bones. This cause of acute hypophosphatemia is different than the other causes because it will immediately return to normal once the hyperventilation stops.#N#
Why does respiratory alkalosis cause hypophosphatemia?
Respiratory alkalosis causes acute hypophosphatemia because your cells naturally begin to shift around the phosphate stores in your bones. This cause of acute hypophosphatemia is different than the other causes because it will immediately return to normal once the hyperventilation stops. . Chronic Hypophosphatemia.
What causes phosphorus to deplete?
Long-term starvation, malnutrition, and anorexia can deplete the body’s stores of phosphorous over time. Acute hypophosphatemia is especially common in hospital patients undergoing refeeding. Additional causes include chronic infections, Crohn’s disease, or malignant tumors. Hyperparathyroidism.
What is the normal phosphorus level?
Phosphorous is a mineral found in your bones that helps to keep your bones and body healthy. Normal blood phosphorous levels are between 2.5 to 4.5 mg/dL. Hypophosphatemia is a condition in which your blood has a low level of phosphorous. Low levels can cause a host of health challenges, including muscle weakness, respiratory or heart failure, ...
What happens when you go into ketoacidosis?
When you go into diabetic ketoacidosis, you have a buildup of acids in your bloodstream, leading to loss of consciousness or even death. Chronic Alcoholism. It is believed that over time, alcoholism hampers your kidney’s ability to absorb phosphorus fully. This is one of the most common causes of hypophosphatemia.
Why do people need phosphate?
Phosphate is a source of intracellular energy, and when someone experiences a severe burn, their phosphate levels dip dangerously low. Therefore, patients must receive supplemental phosphate to stay healthy. Respiratory alkalosis. This is a decreased amount of carbon dioxide pressure without increased bicarbonate.
Can antacids cause hypophosphatemia?
Long-term use of diuretics and antacids can significantly impact the kidney’s ability to absorb phosphorous. Symptoms. As stated previously, hypophosphatemia is always caused by an underlying condition. However, often it is asymptomatic.
What causes hypophosphatemia?
Hypophosphatemia is caused by the following three mechanisms: Inadequate intake (often unmasked in refeeding after long-term low phosphate intake) Increased excretion ( e.g. in hyperparathyroidism, hypophosphatemic rickets) Shift of phosphorus from the extracellular to the intracellular space.
How does hypophosphatemia occur?
Hypophosphatemia is caused by the following three mechanisms: 1 Inadequate intake (often unmasked in refeeding after long-term low phosphate intake) 2 Increased excretion (e.g. in hyperparathyroidism, hypophosphatemic rickets) 3 Shift of phosphorus from the extracellular to the intracellular space. This can be seen in treatment of diabetic ketoacidosis, refeeding, short-term increases in cellular demand (e.g. hungry bone syndrome) and acute respiratory alkalosis.
How is phosphate given?
Phosphate may be given by mouth or by injection into a vein. Hypophosphatemia occurs in about 2% of people within hospital and 70% of people in the intensive care unit (ICU).
Why does alkalemia occur?
This includes most common respiratory alkalemia (a higher than normal blood pH from low carbon dioxide levels in the blood), which in turn is caused by any hyperventilation (such as may result from sepsis, fever, pain, anxiety, drug withdrawal, and many other causes).
Why do cells need phosphate?
Causes. Refeeding syndrome – This causes a demand for phosphate in cells due to the action of hexokinase, an enzyme that attaches phosphate to glucose to begin metabolism of glucose. Also, production of ATP when cells are fed and recharge their energy supplies requires phosphate.
What causes a person to lose appetite?
Symptoms may include weakness, trouble breathing, and loss of appetite. Complications may include seizures, coma, rhabdomyolysis, or softening of the bones. Causes include alcohol use disorder, refeeding in those with malnutrition, diabetic ketoacidosis, burns, hyperventilation, and certain medications.
What causes rhabdomyolysis in white blood cells?
White blood cell dysfunction, causing worsening of infections. Instability of cell membranes due to low adenosine triphosphate (ATP) levels – This may cause rhabdomyolysis with increased serum levels of creatine phosphokinase, and also hemolytic anemia. Increased affinity for oxygen in the blood caused by decreased production ...
Hypophosphatemia Symptoms
Hypophosphatemia may not show any symptoms in the early stages. 3 In severe cases, you may notice the following: 4
Causes
Hypophosphatemia can be caused by health conditions, medical treatments, or malnutrition. They include. 6
Diagnosis
Hypophosphatemia is diagnosed by a blood test to check phosphate levels. You have the condition if levels are 2.5 mg/dL or less. 2 If the cause is unclear, your doctor may test vitamin D levels, liver function, and kidney function. 4
Treatment
If blood tests show that you have hypophosphatemia, you’ll be treated for the disorder causing it and given phosphate-replacement treatment.
Prognosis
Outcomes depend on what caused the hypophosphatemia. 4 If the cause is chemotherapy drugs, keeping phosphate at or above normal levels will help. Treating the condition that caused hypophosphatemia, such as diabetic ketoacidosis, will also help get levels back to normal.
Summary
Hypophosphatemia is a condition in which phosphate levels decrease below 2.5 mg/dL. When phosphate levels get too low, your heart, lungs, and brain can be damaged. Medical conditions, medications, injury, and lifestyle can cause hypophosphatemia. These include severe burns, diabetic ketoacidosis, alcohol use disorder, and chemotherapy drugs.
A Word From Verywell
Early stages of hypophosphatemia may not show any symptoms. You may find out you have it during routine blood work. Or perhaps you have diabetes and develop hypophosphatemia during treatment for diabetic ketoacidosis. In either case, phosphate-replacement treatment can return phosphate levels to normal.
What causes hypophosphatemia?
Chronic hypophosphatemia usually is the result of decreased renal phosphate reabsorption. Causes include the following: Increased parathyroid hormone levels, as in primary and secondary hyperparathyroidism. Other hormonal disturbances, such as Cushing syndrome and hypothyroidism. Vitamin D deficiency.
Why is sodium phosphate not tolerated?
Oral sodium phosphate or potassium phosphate may be poorly tolerated because of diarrhea. Ingestion of 1 L of low-fat or skim milk provides 1 g of phosphate and may be more acceptable. Removal of the cause of hypophosphatemia may include stopping phosphate-binding antacids or diuretics or correcting hypomagnesemia.
Why do people take phosphate binders?
Patients with advanced chronic kidney disease (especially those on dialysis) often take phosphate binders with meals to reduce absorption of dietary phosphate. The prolonged use of these binders can cause hypophosphatemia, particularly when combined with greatly decreased dietary intake of phosphate.
Is potassium phosphate safe to take IV?
It should be administered in any of the following circumstances: IV administration of potassium phosphate (as buffered mix of K2HPO4 and KH2PO4) is relatively safe when renal function is well preserved. Parenteral potassium phosphate contains 93 mg (3 mmol) phosphorus and 170 mg (4.4 mEq) potassium per mL.
Can hypophosphatemia cause muscle weakness?
Hypophosphatemia is usually asymptomatic, but severe depletion can cause anorexia, muscle weakness, and osteomalacia. Treat the underlying disorder, but some patients require oral, or rarely, IV phosphate replacement.
Why do people have hypophosphatemia?
Because the body uses large amounts of phosphate during recovery from certain disorders , acute hypophosphatemia may occur in people recovering from the following conditions: Severe undernutrition (including starvation) Diabetic ketoacidosis. Severe alcoholism.
How is hypophosphatemia diagnosed?
Hypophosphatemia is diagnosed when blood tests show that the level of phosphate in the blood is low. Doctors do other tests to identify the cause if it is not readily apparent.
What is the role of phosphate in the body?
(See also Overview of Electrolytes and Overview of Phosphate's Role in the Body .) Phosphate is one of the body's electrolytes, which are minerals that carry an electric charge when dissolved in body fluids such as blood, but the majority of phosphate in the body is uncharged.
Can you take phosphate by mouth?
If hypophosphatemia is mild and causes no symptoms, drinking low-fat or skim milk, which provides a large amount of phosphate, may help. Or people can take phosphate by mouth, but doing so usually causes diarrhea.
What Are Symptoms of Hypophosphatemia?
Low phosphate levels in the blood (hypophosphatemia) often do not cause any symptoms.
What Causes Hypophosphatemia?
Low phosphate levels in the blood (hypophosphatemia) have numerous causes, such as:
How Is Hypophosphatemia Diagnosed?
Low phosphate levels in the blood (hypophosphatemia) are diagnosed with a blood test to check for blood phosphate concentration.
What Are Complications of Hypophosphatemia?
Complications of low phosphate levels in the blood (hypophosphatemia) depend on how severe and/or chronic the depletion is and may include:
What causes hypophosphatemia in the endocrine system?
endocrine physiology. The most common endocrine causes of hypophosphatemia are as follows: (1a) Hyperparathyroidism – as shown above, this may cause hypophosphatemia and hypercalcemia. (1b) Hungry Bone Syndrome. Occurs immediately following resection of a parathyroid adenoma which was causing hyperparathyroidism.
How to determine hypophosphatemia?
Generally, the cause of hypophosphatemia can be determined by a history and review of labs and medications. In rare situations where hypophosphatemia persists and the cause is unclear, a fractional excretion of phosphate might be helpful (Fe-Phos).
Is hypophosphatemia a contributory factor?
If there is clinical concern of symptoms due to hypophosphatemia. In patients with difficulty weaning from ventilation (some evidence shows that hypophosphatemia may be a contributory factor by causing diaphragmatic weak ness).
Does phosphate increase calcium?
Increasing phosphate may risk precipitation of calcium-phosphate in tissues (calciphylaxis). Try to keep the calcium-phosphate product <70 (calcium multiplied by phosphate, both in mg/dL). (3) Hypocalcemia. Rapid infusion of IV phosphate may reduce calcium level.
Is phosphate present in cells?
phosphate basics. 99% of phosphate is present within cells. Symptoms from phosphate deficiency result from intracellular phosphate deficiency. Unfortunately, we can measure only extracellular phosphate levels. This creates some variability among patients with hypophosphatemia:
Can phosphate be repleted?
Significant hypophosphatemia (e.g. phosphate <2 mg/dL or <0.65 mM) should generally be repleted, with the following potential exceptions: (1) Renal insufficiency. Phosphate should be given only if truly necessary, since these patients tend to develop hyper phosphatemia over time. (2) Hypercalcemia.
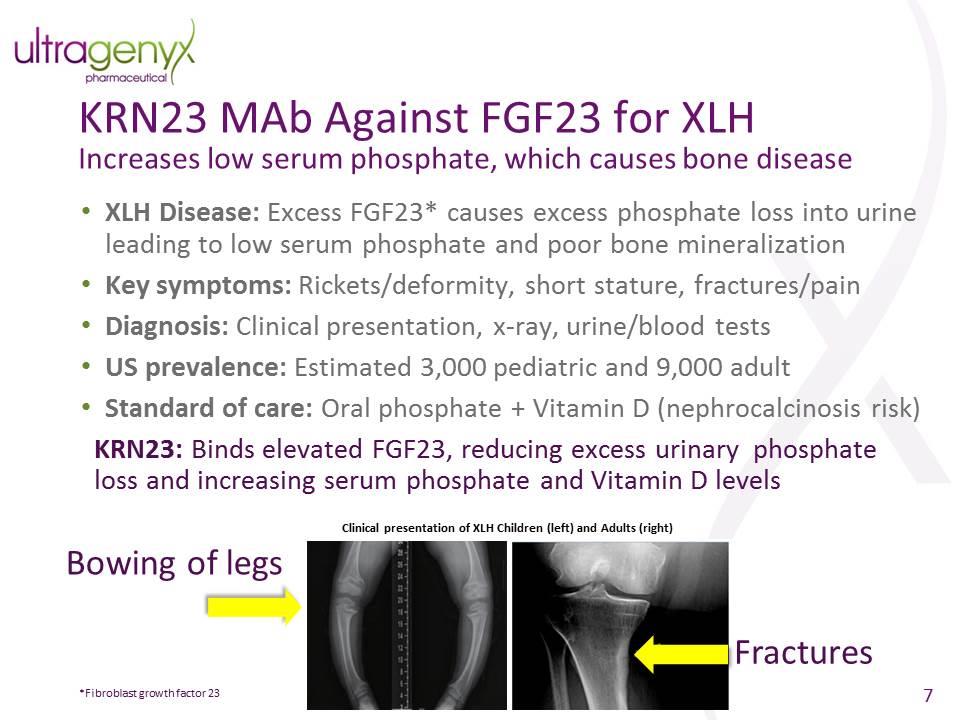
Overview
Hypophosphatemia is an electrolyte disorder in which there is a low level of phosphate in the blood. Symptoms may include weakness, trouble breathing, and loss of appetite. Complications may include seizures, coma, rhabdomyolysis, or softening of the bones.
Causes include alcohol use disorder, refeeding in those with malnutrition, diabeti…
Signs and symptoms
• Muscle dysfunction and weakness – This occurs in major muscles, but also may manifest as: diplopia, low cardiac output, dysphagia, and respiratory depression due to respiratory muscle weakness.
• Mental status changes – This may range from irritability to gross confusion, delirium, and coma.
Causes
• Refeeding syndrome – This causes a demand for phosphate in cells due to the action of hexokinase, an enzyme that attaches phosphate to glucose to begin metabolism of glucose. Also, production of ATP when cells are fed and recharge their energy supplies requires phosphate. A similar mechanism is seen in the treatment of diabetic ketoacidosis, which can be complicated by respiratory failure in these cases due to respiratory muscle weakness.
Pathophysiology
Hypophosphatemia is caused by the following three mechanisms:
• Inadequate intake (often unmasked in refeeding after long-term low phosphate intake)
• Increased excretion (e.g. in hyperparathyroidism, hypophosphatemic rickets)
• Shift of phosphorus from the extracellular to the intracellular space. This can be seen in treatment of diabetic ketoacidosis, refeeding, short-term increases in cellular demand (e.g. hungry bone syndrome) and acute respir…
Diagnosis
Hypophosphatemia is diagnosed by measuring the concentration of phosphate in the blood. Concentrations of phosphate less than 0.81 mmol/L (2.5 mg/dL) are considered diagnostic of hypophosphatemia, though additional tests may be needed to identify the underlying cause of the disorder.
Treatment
Standard intravenous preparations of potassium phosphate are available and are routinely used in malnourished people and people who consume excessive amounts of alcohol. Supplementation by mouth is also useful where no intravenous treatment are available. Historically one of the first demonstrations of this was in people in concentration camp who died soon after being re-fed: it was observed that those given milk (high in phosphate) had a higher survival rate than those wh…
See also
• X-linked hypophosphatemia