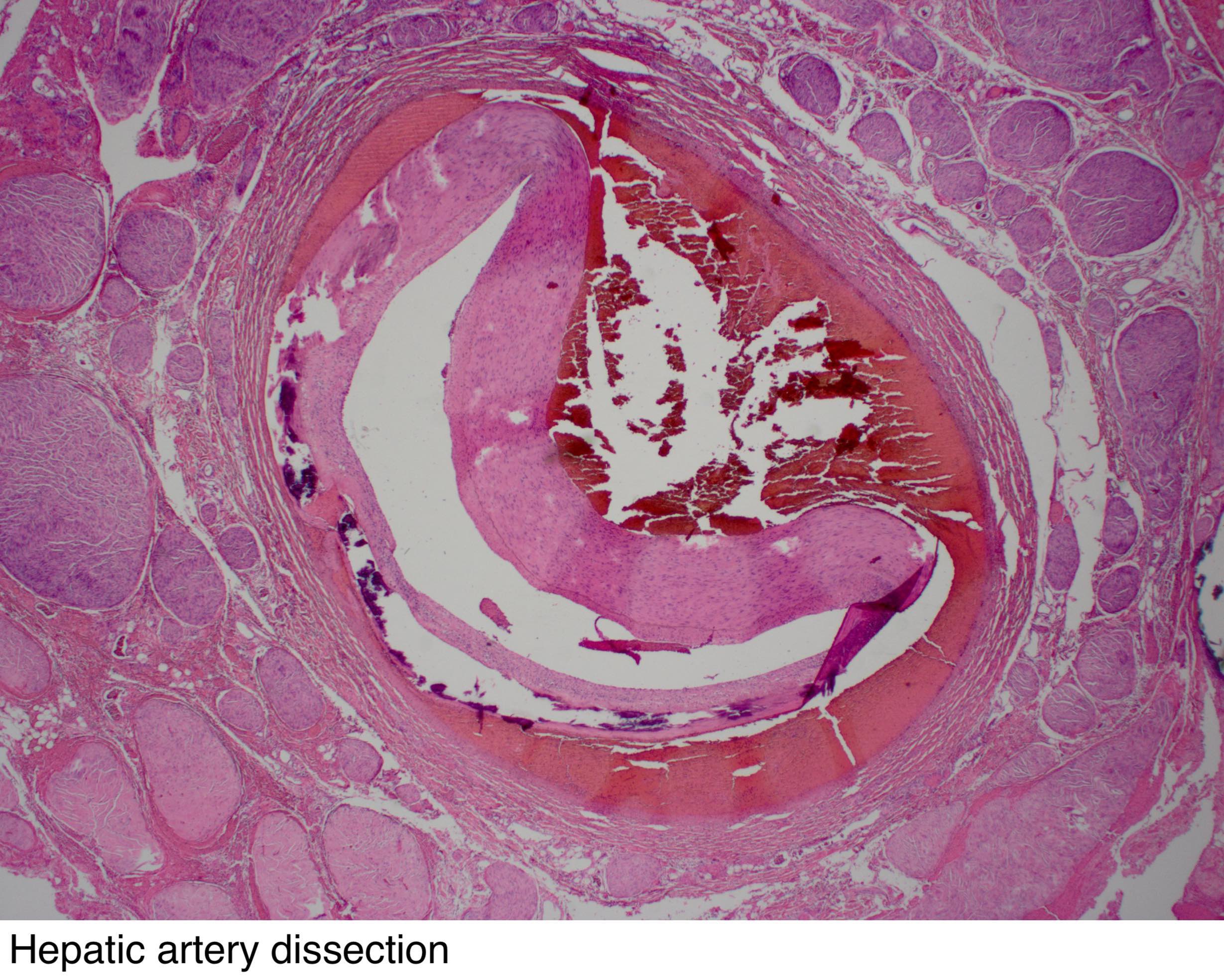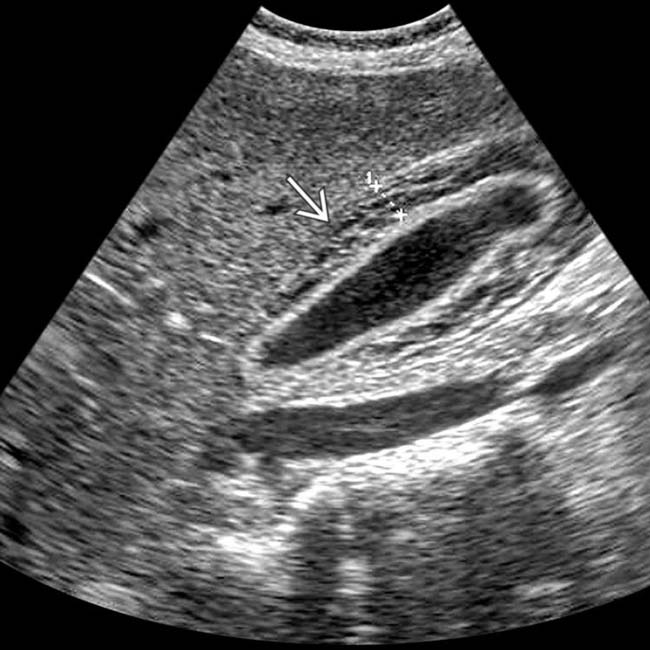
What causes necrosis of the liver?
Abusing heavy amounts of alcohol over time can kill liver cells and trigger necrosis in your liver. 14 Having an open wound, such as an abscess or surgical incision heightens your risk of infection and therefore necrosis. Traumatic injuries and insect bites are necrosis risk factors as well. 15
What is acute hepatic necrosis caused by iron poisoning?
Acute hepatic necrosis is the second most common cause of death due to iron poisoning. It is characterized by hypertransaminasemia, with enzyme concentrations in the range of several thousands of international units per liter ( Tenenbein, 2001; Robertson and Tenenbein, 2005 ).
What is the clinical course of acute hepatic necrosis?
The clinical course of acute hepatic necrosis resembles an acute, toxic injury to the liver with sudden and precipitous onset, marked elevations in serum aminotransferase levels, and early signs of hepatic (or other organ) dysfunction or failure despite minimal or no jaundice. Rapid recovery after withdrawal of the agent is also typical.
What causes necrotic tissue to form?
Blood clots and blood vessel damage are just two of the many causes that can trigger necrosis. Injuries, infections, chronic diseases, and toxins that block blood flow to an area can cause necrotic tissue to form in that area. Traumatic injuries can damage blood vessels and cut off blood flow to the surrounding bones and tissue areas.

What causes necrosis in liver?
Causes of massive or submassive necrosis usually include drug toxicity (e.g., acetaminophen), acute viral or autoimmune hepatitis, acute allograft failure, and fulminant Wilson's disease.
What is hepatic necrosis?
Hepatic necrosis is defined as death of hepatocytes, which maybe single cell, multiple cells in piecemeal, focal, multifocal, submassive or massive. Submassive hepatic necrosis is defined as necrosis involving 26%-75% of the parenchymal volume, while massive necrosis involves more than 75%.
What causes hepatic damage?
The viruses that cause liver damage can be spread through blood or semen, contaminated food or water, or close contact with a person who is infected. The most common types of liver infection are hepatitis viruses, including: Hepatitis A. Hepatitis B.
Can the liver heal with necrosis?
Introduction. Massive hepatic necrosis (MHN) with consequent fulminant liver failure is a rare but very severe complication of liver disease with various etiology. 1 Although this condition often results in the death of the patients, 10–20% of them can recover spontaneously, without liver transplantation.
What are 4 warning signs of a damaged liver?
Tip-offs to Liver DamageJaundice or yellowing of the eyes or skin.Pain and distention of the abdomen due to the release of fluid from the liver.Swelling of lower legs due to fluid retention.Confusion or forgetfulness. ... Dark-colored urine.Pale-colored stool.Chronic fatigue.Nausea or vomiting.
What are the last days of liver failure like?
The person may be unable to tell night from day. He or she may also display irritability and personality changes, or have memory problems. As brain function continues to decline, he or she will become sleepy and increasingly confused. This state can progress to unresponsiveness and coma.
What medications can cause liver damage?
Many over-the-counter (OTC) and prescription medications can cause toxic liver disease....Prescription drugs:Statins.Antibiotics like amoxicillin-clavulanate or erythromycin.Arthritis drugs like methotrexate or azathioprine.Antifungal drugs.Niacin.Steroids.Allopurinol for gout.Antiviral drugs for HIV infection.
What causes liver damage other than alcohol?
Obesity, Diabetes or High Cholesterol These conditions can cause nonalcoholic fatty liver disease, which may also lead to cirrhosis and liver cancer. “Fatty liver disease is the world's fastest growing reason for needing a liver transplant,” says Dr.
How quickly can liver damage occur?
Acute liver failure can happen in as little as 48 hours. It's important to seek medical treatment at the first signs of trouble. These signs may include fatigue, nausea, diarrhea, and discomfort in your right side, just below your ribs.
Is necrosis reversible?
Necrosis is the death of body tissue. It occurs when too little blood flows to the tissue. This can be from injury, radiation, or chemicals. Necrosis cannot be reversed.
How long does it take for liver to regenerate?
The liver, however, is able to replace damaged tissue with new cells. If up to 50 to 60 percent of the liver cells may be killed within three to four days in an extreme case like a Tylenol overdose, the liver will repair completely after 30 days if no complications arise.
Can the liver fully regenerate?
The liver has a unique capacity among organs to regenerate itself after damage. A liver can regrow to a normal size even after up to 90% of it has been removed. But the liver isn't invincible. Many diseases and exposures can harm it beyond the point of repair.
What is massive hepatic necrosis?
Massive hepatic necrosis is a key event underlying acute liver failure, a serious clinical syndrome with high mortality. Massive hepatic necrosis in acute liver failure has unique pathophysiological characteristics including extremely rapid parenchymal cell death and removal.
What type of necrosis is fatty liver?
Fatty liver disease involves the accumulation of triglycerides in hepatocytes, necrosis of hepatocytes, inflammation, and often fibrosis with progression to cirrhosis. The two-hit model summarizes the important early metabolic events leading to hepatocellular necrosis in nonalcoholic steatohepatitis (NASH).
How can you tell if your liver is failing?
What are the symptoms of liver failure?Fatigue.Nausea.Loss of appetite.Diarrhea.Vomiting blood.Blood in the stool.
What is the effect of liver enzymes on hepatocellular necrosis?
Thus increased blood activity of these enzymes may be indicative of active hepatocellular disease.
What cells are preserved in hepatocyte necrosis?
In areas of severe hepatocyte necrosis and collapse, the reticulin framework and endothelial cells are often preserved and are mixed with variable numbers of inflammatory cells and hypertrophied Kupffer cells or macrophages that contain a brown ceroid pigment.
What is the most common lesion in hepatitis?
Severe hepatic necrosis with loss of lobular architecture and collapse of the reticulin framework is the commonest lesion seen in either viral infection 59 or an idiosyncratic drug reaction. In viral hepatitis, necrosis tends to be panacinar in distribution, whereas in toxic injury it is zonal. Most acute liver failure is associated with massive confluent necrosis 60,61 and it is difficult to identify any viable hepatocytes. In non-A-E hepatitis or indeterminate hepatitis, there may be lymphoid aggregates around bile ducts with congestion of centrilobular sinusoids. In hepatitis B there is a minimal inflammatory infiltrate, whereas in Epstein-Barr viral hepatitis, centrilobular necrosis with bridging and collapse may be obvious with cholestasis and lymphoid “blast cells.” In most cases, some evidence of regeneration can be found, 61 with proliferation of ductules. The degree and pattern of necrosis do not correlate with the development of encephalopathy or cerebral edema. 60-62
What causes bile stasis?
Hepatic necrosis or hepatocyte swelling may lead to impaired bile flow, resulting in biliary stasis.
What is the second most common cause of death due to iron poisoning?
Acute hepatic necrosis is the second most common cause of death due to iron poisoning. It is characterized by hypertransaminasemia, with enzyme concentrations in the range of several thousands of international units per liter ( Tenenbein, 2001; Robertson and Tenenbein, 2005 ). When this occurs, the prognosis is poor because the site of damage is Zone 1 of the hepatic acinus. Therefore, hepatocytes that possess the capacity for hepatic regeneration are affected; this differs from acetaminophen poisoning, despite similar transaminase concentrations. The prognosis for the latter is less severe because the site of damage is Zone 3 of the hepatic acinus, the daughter cells.
What is necrosis accompanied by destruction of the endothelial cells?
Hepatocellular necrosis accompanied by destruction of the endothelial cells results in central lobular hemorrhage into the zone of necrotic hepatocytes.
Where does submassive necrosis occur?
Liver necrosis (whether it appears as ballooning degeneration, apoptotic bodies, or coagulative necrosis) occurs mainly in the centrilobular zones, which leads to dropout and loss of hepatocytes.
What causes coagulation necrosis?
Classical coagulation necrosis is typically caused by ischemia or infarction, and tissue architecture is somewhat maintained because lysosomal enzymes responsible for proteolysis are denatured. Another form of necrosis, liquefaction necrosis, may result in cellular dissolution and loss of cytologic architecture.
Is necrosis a subclassification?
Necrosis should not be subclassified based on type, with the exception of single-cell necrosis. For a given xenobiotic, dose and animal variability in response can influence whether hepatocellular necrosis is panlobular or centrilobular and whether it is focal or occurs in extensive irregular patches. If the fundamental process is the same, the lesion (s) should be recorded simply as necrosis and assigned a severity grade. The pattern and other features of the hepatocellular necrosis should be described in the pathology narrative. Splitting out diagnoses too finely will result in complicated incidence tables and may compromise appropriate interpretation of any induced toxicity. When accompanying changes such as fatty change or inflammation are sufficiently extensive, separate diagnoses may be warranted with severity grading and discussion in the pathology narrative. Since degeneration is considered part of the continuum of changes involved in the necrotic process, it should not be diagnosed separately when present with necrosis. However, degeneration without necrosis may occur at exposure levels below doses that cause necrosis and thus may warrant a separate diagnosis. In some cases, hepatocellular necrosis can result in cavernous, blood-filled spaces within the hepatic parenchyma. These blood-filled spaces should not be diagnosed as hemorrhage because they are secondary to necrosis.
What causes necrosis without hepatitis?
Hepatocellular necrosis without the diffuse inflammatory lesion of hepatitis is usually a consequence of the intrinsic type of hepatotoxicity. A common example is suicidal or accidental overdose with the analgesic paracetamol. 76 Jaundice develops after an interval of days, during which available glutathione, which reacts with a toxic metabolite, is used up. The necrosis—like that of shock or heatstroke ( see Fig. 12.2 )—is most severe in perivenular regions (acinar zones 3) and is accompanied by little or no inflammation ( Fig. 8.4 ). Kupffer cells contain brown ceroid pigment. Portal tracts usually remain normal. A few neutrophils and lymphocytes are sometimes also seen in necrotic regions, due to activation of innate immunity by damage-associated molecular pattern (DAMP) molecules such as high-mobility group box-1 (HMGB1) and keratin 18 released from necrotic hepatocytes. 77–79 Complete recovery is possible. While most paracetamol-induced necrosis follows suicidal overdose, it is occasionally found in habitual drinkers taking large doses in the high therapeutic range. 80
What is hepatocellular necrosis?
Hepatocellular necrosis without the diffuse inflammatory lesion of hepatitis is usually a consequence of the intrinsic type of hepatotoxicity. A common example is suicidal or accidental overdose with the analgesic paracetamol (acetaminophen). 58 Jaundice develops after an interval of days, during which available glutathione, which reacts with a toxic metabolite, is used up. The necrosis – like that of shock or heatstroke ( see Fig. 12.2) – is most severe in perivenular regions (acinar zones 3) and is accompanied by little or no inflammation ( Fig. 8.4 ). Kupffer cells contain brown ceroid pigment. Portal tracts usually remain normal. Complete recovery is possible. While most paracetamol-induced necrosis follows suicidal overdose, it is occasionally found in habitual drinkers taking large doses in the high therapeutic range. 59
What is the most common lesion in hepatitis?
Severe hepatic necrosis with loss of lobular architecture and collapse of the reticulin framework is the commonest lesion seen in either viral infection 59 or an idiosyncratic drug reaction. In viral hepatitis, necrosis tends to be panacinar in distribution, whereas in toxic injury it is zonal. Most acute liver failure is associated with massive confluent necrosis 60,61 and it is difficult to identify any viable hepatocytes. In non-A-E hepatitis or indeterminate hepatitis, there may be lymphoid aggregates around bile ducts with congestion of centrilobular sinusoids. In hepatitis B there is a minimal inflammatory infiltrate, whereas in Epstein-Barr viral hepatitis, centrilobular necrosis with bridging and collapse may be obvious with cholestasis and lymphoid “blast cells.” In most cases, some evidence of regeneration can be found, 61 with proliferation of ductules. The degree and pattern of necrosis do not correlate with the development of encephalopathy or cerebral edema. 60-62
What is the most common lesion seen in viral hepatitis 134?
Severe hepatocellular necrosis with collapse of the reticulin framework and thus loss of the lobular architecture is the most common lesion seen in viral hepatitis 134 and from idiosyncratic drug-induced liver injuries. Necrosis tends to have a panacinar distribution in viral infections, whereas in toxic injury it is zonal, with a predilection for the perivenular region (zone 3). Most ALF will have submassive confluent necrosis, 135,136 with minimal viable hepatocytes remaining. In seronegative hepatitis, there may be lymphoid aggregates around bile ducts with congestion of centrilobular sinusoids. In hepatitis B, there is very little inflammatory infiltrate, whereas in Epstein-Barr viral hepatitis, centrilobular necrosis and collapse may be evident with cholestasis. Among the hepatic necrosis, there may be some evidence of attempts at regeneration, with ductular proliferation. 135
What is necrosis accompanied by destruction of the endothelial cells?
Hepatocellular necrosis accompanied by destruction of the endothelial cells results in central lobular hemorrhage into the zone of necrotic hepatocytes.
What is the second most common cause of death due to iron poisoning?
Acute hepatic necrosis is the second most common cause of death due to iron poisoning. It is characterized by hypertransaminasemia, with enzyme concentrations in the range of several thousands of international units per liter ( Tenenbein, 2001; Robertson and Tenenbein, 2005 ). When this occurs, the prognosis is poor because the site of damage is Zone 1 of the hepatic acinus. Therefore, hepatocytes that possess the capacity for hepatic regeneration are affected; this differs from acetaminophen poisoning, despite similar transaminase concentrations. The prognosis for the latter is less severe because the site of damage is Zone 3 of the hepatic acinus, the daughter cells.
Where does liver necrosis occur?
Liver necrosis (whether it appears as ballooning degeneration, apoptotic bodies, or coagulative necrosis) occurs mainly in the centrilobular zones , which leads to dropout and loss of hepatocytes. Extension of hepatocyte injury to the midzonal areas of the lobule leads to the formation of well-demarcated, more or less confluent necrotic areas that contrast abruptly with surviving hepatocyte parenchymal regions. This pattern of necrosis may lead to “maplike” or “geographic” hepatitis (Fig. 40-2 ). In areas of severe hepatocyte necrosis and collapse, the reticulin framework and endothelial cells are often preserved and are mixed with variable numbers of inflammatory cells and hypertrophied Kupffer cells or macrophages that contain a brown ceroid pigment. Several types of drugs may lead to this type of necroinflammatory injury, which can exhibit a zonal coagulative pattern. In rare cases, one may see predominantly midzonal necrosis (furosemide) or periportal necrosis. Drugs such as cocaine ( Fig. 40-3 ), especially in combination with other toxins (e.g., halogenated hydrocarbons), can cause this pattern of periportal injury, as well as allylformate and albitocin. But this is rarer than the centrilobular type of hepatocellular injury (e.g., acetaminophen, halothane).
What is a hepatitis?
Hepatitis is an inflammation of the liver characterized by diffuse or patchy necrosis.
What percentage of hepatitis is jaundice?
Clinical hepatitis with jaundice in 5–10%; subclinical liver involvement in 90–95%. Acute hepatitis sometimes severe in young adults. Herpes simplex virus. Anicteric hepatitis, usually in immunocompromised patients (but can also occur in immunocompetent patients) Fever in the majority; rash in 50%.
Is liver metastasis asymptomatic?
Metastatic Liver Cancer. Liver metastases are common in many types of cancer, especially those of the GI tract, breast, lung, and pancreas. Symptoms of early liver metastases may be asymptomatic, and nonspecific symptoms often develop first.
Is schistosomiasis a hepatitis?
Parasitic infections (eg, schistosomiasis , malaria , amebiasis ), pyogenic infections, and abscesses that affect the liver are not considered hepatitis. Liver involvement with tuberculosis (TB) and other granulomatous infiltrations is sometimes called granulomatous hepatitis, but the clinical, biochemical, and histologic features differ ...
What causes necrosis in the body?
Necrosis is caused by a lack of blood and oxygen to the tissue. It may be triggered by chemicals, cold, trauma, radiation or chronic conditions that impair blood flow. 1 There are many types of necrosis, as it can affect many areas of the body, including bone, skin, organs and other tissues. It isn't always a clot or cold ...
What is the type of necrosis that occurs when a clot forms in a blood vessel?
Another type of necrosis happens when a clot, such as a deep vein thrombosis (DVT) forms in a blood vessel and blocks blood flow to an area of the body.
Can a car accident cause necrosis?
Any time blood flow is blocked to an area, or an area is so damaged that blood can not flow to and from it , necrosis may be possible.
What causes the liver to fail?
Cancer. Cancer that either begins in or spreads to your liver can cause your liver to fail.
What causes a blockage in the veins of the liver?
Diseases of the veins in the liver. Vascular diseases, such as Budd-Chiari syndrome, can cause blockages in the veins of the liver and lead to acute liver failure.
What are the complications of liver failure?
Acute liver failure often causes complications, including: 1 Excessive fluid in the brain (cerebral edema). Too much fluid causes pressure to build up in your brain, which can lead to disorientation, severe mental confusion and seizures. 2 Bleeding and bleeding disorders. A failing liver cannot make enough clotting factors, which help blood to clot. Bleeding in the gastrointestinal tract is common with this condition. It may be difficult to control. 3 Infections. People with acute liver failure are more likely to develop infections, particularly in the blood and in the respiratory and urinary tracts. 4 Kidney failure. Kidney failure often occurs after liver failure, especially if you had an acetaminophen overdose, which damages both your liver and your kidneys.
What is liver failure?
Overview. Acute liver failure is loss of liver function that occurs rapidly — in days or weeks — usually in a person who has no preexisting liver disease. It's most commonly caused by a hepatitis virus or drugs, such as acetaminophen.
How do you know if you have liver failure?
Signs and symptoms of acute liver failure may include: Yellowing of your skin and eyeballs (jaundice) Pain in your upper right abdomen. Abdominal swelling (ascites) Nausea. Vomiting. A general sense of feeling unwell (malaise) Disorientation or confusion. Sleepiness.
How to avoid hepatitis?
Avoid contact with other people's blood and body fluids. Accidental needle sticks or improper cleanup of blood or body fluids can spread hepatitis viruses. Sharing razor blades or toothbrushes also can spread infection.
Which supplements cause liver failure?
Herbal supplements. Herbal drugs and supplements, including kava, ephedra, skullcap and pennyroyal, have been linked to acute liver failure.
What are the pathophysiology, microscopic findings and associated hepatic diseases?
This broad topic highlights the pathophysiology, microscopic findings and associated hepatic diseases with commonly encountered structural changes, patterns of cell damage and necrosis, intracellular hepatic changes and common patterns of biliary reaction to injury in hepatology
What is a dead hepatocyte?
Usually a nonspecific finding to describe a dead hepatocyte, most commonly seen in major inflammatory hepatic diseases: viral hepatitis, autoimmune hepatitis, alcoholic and nonalcoholic steatohepatitis, drug induced liver injury and low grade / transient ischemia.
How many droplets are in a hepatocyte?
Microscopically, usually large fat droplets are seen in hepatocytes (exceeding 20 micrometers), typically 1 per cell, pushing the nucleus to the periphery and giving an appearance of a signet ring / adipocyte; macrovesicular steatosis can be of the small droplet or large droplet type
Why does bile salt dissolution occur?
Pathophysiologically, in adults it is thought to be due to the detergent action of retained bile salts, leading to dissolution of plasma membranes and coalescence of adjacent hepatocytes
Which zone of the hepatic lobule is most prone to ischemia?
Refers to a distribution of necrosis within the centrilobular tissue of the hepatic lobule around the central vein (acinar zone 3), most prone to ischemia and metabolic toxin injury. Centrilobular zone (acinar zone 3) is especially vulnerable to ischemic injury due to anatomic location at the distal end of afferent blood flow.
Why are cytoskeletal filaments misfolded?
Misfolded, aggregated and clumped intracellular cytoskeletal filaments due to alterations in the hepatocellular cytokeratin assembly, usually seen in ballooned hepatocytes and an indication of cellular injury
Which membrane is responsible for apoptosis?
Pathophysiologically and biochemically, cells undergoing apoptosis exhibit externalization of phosphatidylserine on the outer leaflet of plasma membrane, increased mitochondrial membrane permeability and release of proteins from the intermembrane space with activation of caspases and endonucleases, resulting in cleavage of structural proteins and DNA