Full Answer
What is peak pressure on a ventilator?
Peak Pressure (Ppeak): This is the summation of pressure generated by the ventilator to overcome airway (ETT and bronchus) resistance and alveolar resistance to attain peak inspiratory flow and to deliver desired tidal volume.
What is peak inspiratory pressure (P peak)?
The total amount of airway pressure delivered by the ventilator to overcome resistive and elastic work is defined as the peak inspiratory pressure ( P peak). The total airway pressure can be separated into component parts by measuring an inspiratory pause.
What does peak pressure mean on an ECG?
Peak Pressure. Peak pressure applies when there is airflow in the circuit, i.e. during inspiration. What determines the peak pressure is the airway resistance in the lungs. So it follows that if there is a problem with the airways the peak pressure will rise.
What causes peak inspiratory pressure to increase?
As a simplified equation, it can be thought of as: Elevations in airway pressure can thus be thought of being caused by increases in airway resistance and/or decreases in lung compliance. The total amount of airway pressure delivered by the ventilator to overcome resistive and elastic work is defined as the peak inspiratory pressure ( P peak).

What is normal peak pressure on ventilator?
Peak pressure is graphed as a summation of both initial airway resistance and lung compliance. In general, an acceptable maximum Ppeak is 40 cmH2O.
What does peak flow mean on a ventilator?
Mechanical Ventilation Flow rate, or peak inspiratory flow rate, is the maximum flow at which a set tidal volume breath is delivered by the ventilator. Most modern ventilators can deliver flow rates between 60 and 120 L/min. Flow rates should be titrated to meet the patient's inspiratory demands. 31.
What do peak pressures mean?
Definitions. Peak pressure: This is the pressure that is generated by the ventilator to overcome BOTH airway resistance AND alveolar resistance. The goal of the pressure is to obtain the set inspiratory flow and the tidal volume goal that is set by the provider.
What causes high peak pressures on ventilator?
Peak inspiratory and plateau pressures Elevations in airway pressure can thus be thought of being caused by increases in airway resistance and/or decreases in lung compliance.
What's a normal peak flow score?
Peak expiratory flow (PEF) is measured in litres per minute. Normal adult peak flow scores range between around 400 and 700 litres per minute, although scores in older women can be lower and still be normal.
Does peak flow measure lung capacity?
A peak flow meter is a portable, inexpensive, hand-held device that measures your ability to push air out of your lungs. Air flow is measured by the amount of air that you can blow out in one "fast blast." Peak flow meters come in two ranges to measure the air pushed out of your lungs.
What causes low peak pressure on ventilator?
Some causes for low pressure alarms are: The patient becomes disconnected from the ventilator circuit. Inadequate inflation of the tracheostomy tube cuff. Poorly fitting noninvasive masks or nasal pillows/prongs. Loose circuit and tubing connections.
What do static and peak pressures represent on the ventilator?
What do static pressures represent on the ventilator? The static or “plateau” pressure is representative of the compliance of the respiratory system (lung, chest wall and abdomen). In essence, it is telling you how much pressure is necessary to inflate the alveoli with each breath.
What affects peak airway pressure?
Peak inspiratory pressure increases with any airway resistance. Things that may increase PIP could be increased secretions, bronchospasm, biting down on ventilation tubing, and decreased lung compliance.
How do you reduce peak pressure?
High peak inspiratory pressure (PIP) during mechanical ventilation is associated with increased risk of barotrauma. High frequency jet ventilation (HFJV) and pressure control ventilation (PCV) have been advocated for the reduction of PIP.
What is high peak inspiratory pressure?
The peak inspiratory pressure (PIP) is the highest pressure measured during the respiratory cycle and is a function of both the resistance of the airways and the compliance of the respiratory system.
Can plateau pressure be higher than peak?
Can the plateau pressure be higher than the peak pressure? Yes. In pressure-regulated modes of ventilation, plateau pressures can be higher than peak pressures if inspiratory efforts of the patient generate larger tidal volumes and significantly negative pleural pressures.
What does a low peak flow reading mean?
If your airways are tight and inflamed, your peak flow score will be lower than normal. This could be a sign your asthma is getting worse. See your GP if: you're having symptoms, or need to use your reliever inhaler three or more times a week, even if your peak flow scores are normal.
What does a peak flow measure?
Peak flow is a simple measurement of how quickly you can blow air out of your lungs. It's often used to help diagnose and monitor asthma. Credit: A peak flow test involves blowing as hard as you can into a small handheld device called a peak flow meter.
What peak flow indicates COPD?
A peak expiratory flow rate of less than 80% will detect more than 90% of people with chronic obstructive pulmonary disease in the community, including all of those with moderate or severe disease—that is, patients most likely to benefit from treatment with bronchodilators.
What is the normal breathing flow rate?
At complete rest, the typical adult male exchanges approximately 0.5 l (500; 400 ml for female) of air per breath (tidal volume) at a rate of 12 times per minute, resulting in a minute ventilation rate of about 6 l of air per minute.
What is the constellation of high airway pressures and hypotension?
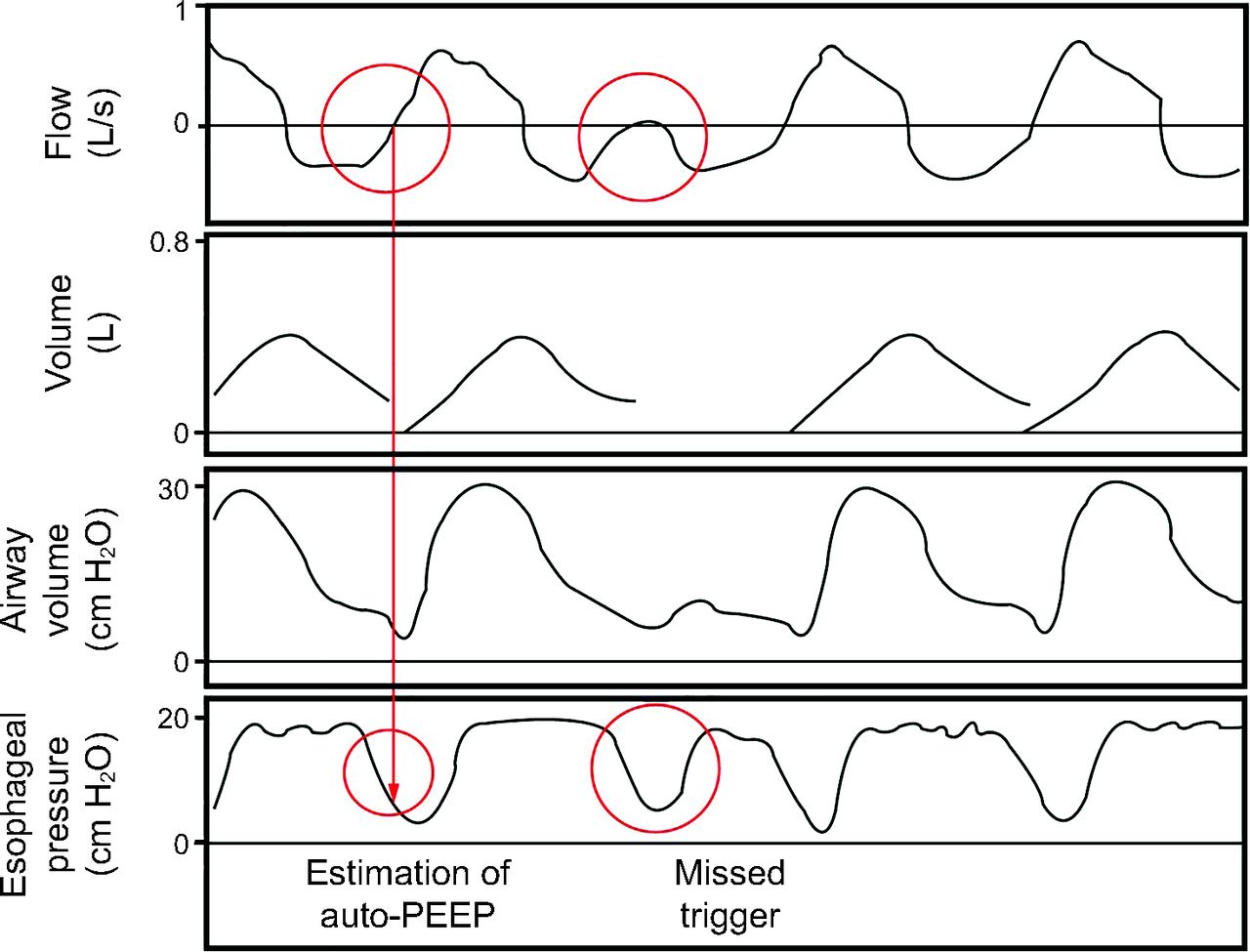
Elevations in intrathoracic pressure limit cardiac output. The constellation of high airway pressures and hypotension suggest critical auto-PEEP or tension pneumothorax. If hypotension improves when the ventilator is removed, auto-PEEP may be the likely cause. If it does not improve, tension pneumothorax and needle decompression should be ...
What is the work of breathing?
Work of Breathing. When a patient is on a ventilator, the amount of work needed to deliver a breath can be thought of in terms of pressure. The total amount of work (or pressure) can be divided into two components: Work to overcome resistance in the airways (resistive work) Work to distend the lungs and chest wall (elastic work).
What is high peak inspiratory pressure?
High peak inspiratory pressures are associated with pneumothorax, whereas elevated mean airway pressures are associated with pneumothorax and reduction in cardiac output.73 It is not clear whether high peak inspiratory pressures are a primary or secondary phenomenon associated with the generation of pneumothorax.
What are the parameters of a ventilator?
Various parameters can be preset on most ventilators, including the respiratory rate, PIP, PEEP, inspiratory time, and gas flow rate . When adjusting these parameters it is necessary to consider the pathologic condition present in the lung. Infants with primary pulmonary hypertension have very compliant lungs that are easily overdistended. In these patients adequate minute ventilation may be achieved with low PIP and PEEP, a short inspiratory time, and a moderate respiratory rate. Conversely a child with ARDS has noncompliant lungs and may require a relatively high PIP and PEEP, a short inspiratory time, and a high respiratory rate to achieve adequate alveolar ventilation. Obstructive disorders such as meconium aspiration syndrome and asthma have a longer time constant and require ventilation at a slower rate. After determining the initial settings, however, the patient's response must be evaluated and adjustments must be made to stay abreast of dynamic changes in pulmonary compliance and resistance that occur over time.
What is a continuous flow ventilator?
For use in infants, ventilators were modified to provide continuous flow throughout the respiratory cycle. 14 A continuous flow device refers to a ventilator in which the flow of respiratory gas occurs throughout the respiratory cycle. Most infant ventilators are continuous flow devices (e.g., Infant Star, Baby Bird). In most continuous flow infant ventilators, inspiratory valves are lacking, and the cycling is controlled by the exhalation valve. Closure of the exhalation valve begins inspiration, and the flow of gas going through the circuit is diverted to the patient. If the inspiratory flow rate is low (1 to 3 L/kg) and if the PIP is not limited, the tidal volume delivered by the patient can be calculated from the inspiratory flow rate and the inspiratory time. This would result in a time-cycled, volume-regulated breath. For pressure-control ventilation, the flow rates used are usually higher (4 to 10 L/kg). Once the preset PIP is reached, the excess flow is vented through a pressure relief valve, and the lungs are maintained in inflation throughout the rest of inspiration. During exhalation, there is continuous flow of gas, allowing the patient to breathe from the circuit rather than open a demand valve. A demand flow ventilator refers to a ventilator that allows inspiratory flow of gas to the patient between ventilator breaths through a demand valve that is opened by the patient’s inspiratory efforts. Work of breathing is higher with a demand flow ventilator compared with a continuous flow device because of the effort required to open the demand valve.
What is PEEP in lung?
1. PEEP in part determines lung volume during the expiratory phase, improves ventilation-perfusion mismatch, and prevents alveolar collapse. 2. PEEP contributes to the pressure gradient between the onset and end of inspiration, and thus affects the tidal volume and minute ventilation.
What is the goal of assisted respiratory support?
The goal of assisted respiratory support, whether invasive (ETT) or less invasive (nasal CPAP, high-flow nasal cannula, NIPPV, BIPAP, or HFNV), is to keep the lung ventilation in the midportion of the PV curve. Expiratory flow is dependent on the elastic and resistive properties of the lung. On assisted ventilation, the slope of the expiratory waveform plays a role also. A too rapid (steep slope) decline of the expiratory wave may lead to air-trapping and movement away from the midportion of the PV curve. This can be especially true of the patient with established BPD or evolving BPD. Latzin et al. used time of peak tidal expiratory flow (tPTEF) divided by expiratory time (tE) to measure compliance ( Fig. 12-8 ). Patients with BPD had decreased tPTEF/tE suggestive of poorer lung compliance.
How does PIP affect ventilation?
Physiologic effects. 1. PIP in part determines the pressure gradient between the onset and end of inspiration and thus affects the tidal volume and minute ventilation. 2. During volume ventilation, an increase in tidal volume corresponds to an increase in PIP during pressure ventilation.
What is the most common complication of mechanical ventilation?
Barotrauma is the most commonly associated complication of mechanical ventilation, with the literature suggesting an incidence of between 7% and 25%. 75 Much of the difference depends on the case mix in a particular study as well as the definition of barotrauma used.
What is a ventilator?
What does a ventilator do? First of all, it’s important to understand that a ventilator is used to help people breathe when they can’t breathe on their own. It is a type of life support. A tube from the ventilator machine is inserted through the mouth, down into the windpipe.
How long should I be on a ventilator?
Four things determine how long a patient may be on a ventilator: 1 The patient’s health and age before they got sick. For people over 65 who require emergency ventilator use, about 2 out of 3 survive to leave the hospital. Older people with chronic conditions tend to have more disabilities after ventilator use and lower survival rates. 2 The reason for needing the ventilator. How serious is being put on a ventilator? In some cases, such as surgery, ventilators are used for a few hours to a few days. Sometimes the ventilator is used for days to weeks—for example, for serious pneumonia or lung injury. 3 How long the ventilator is needed. The longer the ventilator is needed, the higher the chance of long-term complications such as weakness, loss of independence, depression/anxiety, and long-term dependence on the ventilator. For those over the age of 70 or those with health problems, the chance of long-term complications is higher. 4 Your personal values and beliefs. It is important to think about what matters most to you. What gives meaning to your life? Is there any condition that would not be acceptable to you? What would you be willing to try? It’s best to talk to your family and providers about your priorities and medical wishes in advance of a situation where you will need to make these kinds of decisions.
What is the purpose of a ventilator?
The ventilator provides air pressure to keep the lungs open, and the tube makes it easier to remove mucus that builds up in the lungs. What is it like to be on a ventilator? The tube from the ventilator can feel uncomfortable, but it is not usually painful. Most people need sedating medicine to tolerate the discomfort.
Can you talk on a ventilator?
Artificial nutrition can be given through a small tube in your nose (tube-feeding). While on a ventilator, you cannot talk. If you’re not sedated, you can write notes to communicate.
Can everyone go on a ventilator?
While ventilators can offer hope for many patients, not everyone chooses to go on a ventilator when given the choice. There are benefits and potential complications of going on a ventilator. Read on to learn more:
