Biopsychosocial approach meaning George Engel
George Engel
George Engel was a labor union activist executed after the Haymarket riot, along with Albert Parsons, August Spies, and Adolph Fischer.
Full Answer
What does the biopsychosocial model suggest?
What does the biopsychosocial model suggest? A biopsychosocial model suggests that gender differences are caused by a combination of social forces acting on biological processes and, in turn, biological processes operating on psychological and social processes.
What is the biopsychosocial model of care?
understanding health, illness, and health care delivery. The biopsychosocial model is both a philosophy of clinical care & a practical clinical guide. Philosophically, it is a way of understanding how suffering, disease, and illness are affected by multiple levels of organization, from the societal to the molecular.
What are the limitations of the biopsychosocial model?
The biopsychosocial model has been criticized that it does notconstitute a scientific or philosophical model, it does not provide an answer to the crucial question of how the biological, psychologicaland social variables interact in the disease's expression, that it does not provide guidance on the exact time of itsapplication and, finally, that it allows for a wide range of interventions without providing specific guidelines of a concrete therapeutic scheme.
What is the biopsychosocial model of psychology?
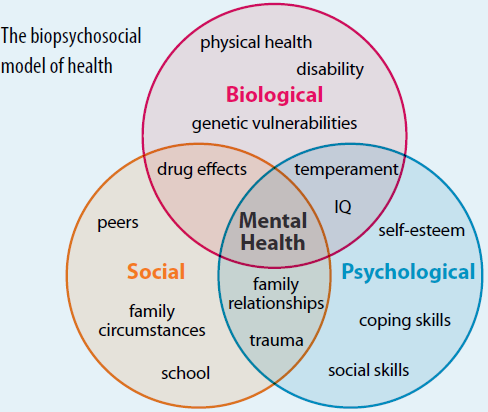
The Three Aspects of the Biopsychosocial Model
- Biological. ''Bio'' refers to the biological components that impact health. This includes genetics, neurochemistry, physical health, or effects of medication.
- Psychological. ''Psycho'' refers to psychological components that address thoughts, emotions, and behaviors. ...
- Social. ''Social'' refers to one's social environment. ...

How to explain the biopsychosocial model?
The biopsychosocial model is a comprehensive model used to understand why and how illness occurs. It incorporates three components, biology, psycho...
What is an example of a biopsychosocial approach?
A doctor has a patient who needs a treatment plan for recovery from a recent knee surgery that is not healing as quickly as hoped. With the BPS app...
Why is the biopsychosocial approach important?
The biopsychosocial approach is important because it provides an alternative to reductionist models that only consider biological factors in diagno...
Who proposed biopsychosocial model?
The biopsychosocial model was proposed by Dr. George Engel in 1977. He began using it with students at the University of Rochester.
What are biopsychosocial characteristics?
The biopsychosocial characteristics are biological, psychological, and social. Biological factors include factors relating to the body, such as gen...
How does the biopsychosocial approach explain who a person becomes?
The biopsychosocial approach believes that health and wellness are impacted by a dynamic interplay of factors. A person's mental health is a produc...
What is the first part of the pain definition?
What about the first part of the pain definition? We would all agree that pain is an unpleasant sensation – its purpose is to get our attention and alert us to something wrong. But have you ever thought of pain as an unpleasant emotion? There is always some kind of unpleasant emotion associated with pain – for example, sadness (crying) when it hurts, anger if it stops us doing what we want, or fear that it won’t go away. When we realise that pain encompasses both a sensory and emotional experience, we can already see there are both biological and psychological aspects to pain. Let’s look further at the biopsychosocial model.
What is biopsychosocial approach?
The biopsychosocial approach considers not only the biological aspects of a health condition (what is going on physically) but also the psychological and sociological aspects. Before I lose you on this, let’s take a step back and think about the example of pain. Let’s start with the definition of pain, which was recently updated by the International Association for the Study of Pain (IASP).
Why do I feel pain when I cut my finger?
If we cut our finger, the danger message is sent to our brain, and pain is produced to get our attention, so we tend to the cut and stop it bleeding. But what about potential tissue damage? To understand this, it helps to know that pain is produced by our brain as a warning signal. Sometimes the brain produces this warning not only when we cause actual damage, but when we might cause damage. If we bend a finger back, pain warns us not to go any further before we actually cause damage - the finger is fine if we listen to that warning and stop. I heard another great example of this recently. A carpenter accidentally punched a nail into his foot using a nail gun. He presented to emergency in agonising pain. However, when they X-rayed his foot, it turned out the nail had missed his foot entirely and was only in his boot! His brain had good reason to assume he had caused damage, and until proven otherwise, the pain was warning him to seek help.
What is the sociological side of biopsychosocial?
The sociological side of the biopsychosocial model includes things like cultural beliefs, and social support from friends or family. The role this plays in health has been recognised in some ways. For example, it has long been known that people from a lower socio-economic background have poorer health outcomes. This is not just due to access to good healthcare, but also because more people from these backgrounds tend to engage in “riskier” health behaviours, such as smoking or having a poor diet. However, there are also less obvious ways that social context can influence health symptoms. An interesting study published this year showed women given the same painful stimulus reported less pain when their partner was holding their hand, compared with when their partner was present but not holding their hand, or wasn’t there at all. Some other examples might help.
Do biological aspects matter in healthcare?
If we only ever look at the biological aspects, we may miss key elements of the whole picture. This is not to say the biological aspects don’t matter – they still do! But they are not the only thing that influences health conditions.
What Is the Biopsychosocial Model?
There is so much to consider that psychologists have adopted what's called the biopsychosocial (BPS) model, which examines biological, psychological, and social factors affecting an individual, to examine how and why disorders occur.
What is the difference between psychosocial and biopsychosocial?
Biopsychosocial (BPS) Model. Bio - Bio references the biology and physical health of the patient. Psycho - Psycho refers to a person's behavior, thoughts and emotions. Social - The social interactions, cultural background and economics are covered by the social component of the model.
What is schizophrenia found in?
Schizophrenia - Schizophrenia may be found in people with delusions, unusual behavior and difficulty focusing on daily tasks. Learning Outcomes. After this lesson is done, students should be able to: Define the interactions of the three parts of the biopsychosocial model.
How to write a biochosocial essay?
In one to two paragraphs, write an essay that provides the definition of the biopsychosocial (BPS) model. Be sure to individually address each component and its meaning (bio, psycho, and social).
What is the power of the BPS model?
Thus, the power of the BPS model is that it looks at health and disease in a variety of contexts and examines how the interaction of different factors leads to specific issues for an individual. To successfully treat Joan, her doctors might incorporate physical therapy to help her arm recover, psychological therapy to work out distress, and maybe integration into social programs so Joan can return to or create a regular social routine.
Why is the BPS model used in psychology?
The BPS model isn't just used by psychologists; it has many applications in different fields because of how inclusive it is of different factors that influence human behavior. A doctor might wonder: 'How could different social situations lead to this disease?' Or, a social worker might want to see if a child's developmental disorder might have to do with being in a foster family.
What does it mean to enroll in a course?
Enrolling in a course lets you earn progress by passing quizzes and exams.
What are the environmental stressors?
There are in fact a host of environmental stressors such as loss of control over adversity, early separation, attachment loss, social support, defeat and social harassment (bullying) that produce profound physiological disturbances and negative states of mind (Gilbert, 2001; Wilkinson, 1996). So the biopsychosocial approach argues ...
What is the biopsychosocial approach?
Bio-Psycho-Social Approach. The idea that mental states are influenced by many interacting processes, such as bodily processes, personality dispositions and life events, is a very old one. It was well articulated by the early Greek physicians over 2000 years ago and has existed in many cultures old and new Oackson, 1986).
Why do people become sick?
Many people can become very ill because of toxic environments, and such illnesses are not merely social constructions (although one could argue the whole concept of what constitutes an “illness” is a construction of sorts). There are in fact a host of environmental stressors such as loss of control over adversity, early separation, attachment loss, ...
Is clinical psychology a biopsychosocial approach?
For clinical psychology to become a genuinely integrative profession, capable of utilizing scientific findings from a multitude of areas, it is vital we do not confuse the biopsychosocial approach with psychiatry’s use of the biomedical model (Kiesler, 1999; Meehl, 1995). The biopsychosocial approach is ideally suited to cope with the increasing complexities of the clinical sciences, because its focus is on interactions in various domains. The competitive dynamics between professions and between different schools of therapy are understandable as basic human dispositions to assert their views over those of others, but from a scientific and therapeutic point of view this is often unhelpful. We need to break the shackles of brainlessness verses mindlessness, as well as our often decontextualized and desocialized clinical sciences (Eisenberg, 1986; 2000). At the risk of sounding competitive myself, I do believe that clinical psychologists could and should be at the forefront of developing biopsychosocial models of disorders and of interventions. Understanding the interaction between evolved brains, social contexts and experienced selves is the challenge.
Is genetic variation irrelevant to suffering?
Clinical psychologists sometimes give the impression that physiological and genetic variation are irrelevant to suffering. The biopsychosocial approach, however, pays due regard to the physiology of mental states, for we are embodied, feeling beings – not just collections of internal schema or behavioural strategies.
Who used biopsychosocial approach to heart disease?
The biopsychosocial approach, however, is most closely identified with the cardiologist Engel (1977), who in the 1960s used it to understand heart disease. Engel pointed out that heart disease was often the end point of a large variety of cultural, social and psychological factors impinging on the cardiovascular system.
Is depression a physical disorder?
If we focus on depression, it is clear that the physical picture of depression is real enough with abundant evidence of disturbances of physiolog y (for example, in stress systems and sleep; McGuade and Young, 2000). Depression is a horrible, affect-laden experience that people often feel trapped in. Even for those with (so called) sub-syndromal depressions such as dysthymia, there is good evidence that, as in major depression, there are significant physiological disturbances of functioning (for example, of stress, immune and neurotransmitters systems; Griffiths et al., 2000). New work is exploring the interaction between mood and immune systems (Anisman and Merali, 1999) and the way depression compromises immune functioning, increasing vulnerability to a range of physical disorders (Maes, 1995; Martin, 1997). Even more worrying are the findings that those who are chronically stressed may be vulnerable to subtle forms of brain damage due to the effects of cortisol on neuronal pathways (Sapolsky, 1996; 2000).
What did the student's doctor discover about the biopsychosocial approach?
The student's doctor used the biopsychosocial approach, and discovered that the student had some social problems, including a fear of presenting in front of people and relationship difficulties .
How long is the TCI program?
TCI offers a one-year program that adapts the 12-step method and biopsychosocial approach.
Is the Bulletin de Psihiatrie Integrativa humanistic?
This spirit has been preserved over the years, including in the pages of the current "Buletin de Psihiatrie Integrativa" [Integrative Psychology Bulletin], open to humanistic valences and very much to research and adjacent medical fields, overlapping the biopsychosocial approach to mental illness, a concept consolidated by the School of Socola.
How do developmental psychologists explain maturation?
Developmental psychologists who are social scientists that examine the different forces that impact how we grow and develop throughout life, use the biopsychosocial approach to explain maturation in terms of multiple factors. It's based on the idea that biological, psychological and social factors are all affecting the way we develop.
How does human development occur?
Human development occurs constantly throughout the lifespan as we grow and change. Developmental psychologists examine the different forces that impact how we grow and develop throughout life. The biopsychosocial approach to development is based on the idea that biological, psychological and social factors are all affecting the way we develop.
What are the psychological factors that contribute to who you are?
Your answers to these questions help to describe the psychological factors, or the thought processes behind a person's behavior, that contribute to who you are. Psychological factors include things such as temperament and coping skills.
Why is biopsychosocial development important?
The biopsychosocial approach to development views social factors, along with biological and psychological factors, as important in terms of understanding how an individual grows and matures throughout the lifespan.
How do biological factors affect development?
Biological factors, or ingrained aspects of a person, influence development because of genetic material that is inherited from the parents. Psychological factors, or the thought processes behind a person's behavior, such as temperament, also affect development.
What does it mean to enroll in a course?
Enrolling in a course lets you earn progress by passing quizzes and exams.
What are social factors?
Social factors include the relationships that someone has, one's environment and even the cultural influences of that person, and all are important in development. As with biological and psychological factors, positive social factors can enhance development while negative influences can deter development.
How does acute pain affect recovery?
Knowing that not all individuals who experience an injury develop a chronic pain condition, it is important to recognize how an acute situation transitions to a chronic pain state. Acute pain is generally viewed as an indicator of tissue damage and is interpreted through noxious sensations. 7 In general, as the level of nociception decreases, the acute pain state diminishes. While the individual experiencing acute pain may report an increased level of anxiety, it is typically temporary. Anxiety, fear, and worry in acute pain situations are often viewed as being adaptive in that the negative emotions influence proactive recovery behaviors, such as seeking medical care and attending to the injury.
What is the biopsychosocial model?
The biopsychosocial model has led to the development of the most therapeutic and cost-effective interdisciplinary pain management programs and makes it far more likely for the chronic pain patient to regain function and experience vast improvements in quality of life.
How does primary care help with injury?
Most patients who incur an injury recover well following the primary care treatment. When psychological factors and social issues merge with the physiological impairment, though, a more integrated rehabilitation process is necessary to help the patient avoid entering into a full chronic pain condition. Commonly, a subset of the injured population finds recuperation to be difficult at the level of primary care, and will therefore require an expanded treatment program for their injury, which is termed secondary care. At this level, an interdisciplinary team works together to help the patient avoid physical deconditioning and reduce psychological barriers that interfere with recovery. Most patients for whom primary care is not sufficient experience positive outcomes following secondary care. 27
How long does pain last after injury?
An intermittent stage occurs following the acute phase, such that the pain condition is seen to last for two to four months post injury. During this stage, the patient is described as experiencing more psychological and behavioral distress, such as anger, somatization, and learned helplessness. 15 Chronic pain typically lasts for at least six months past the injury, which surpasses the time for which general musculoskeletal disorders heal sufficiently. 16 Syndromes producing long-term pain conditions are often associated with depression and resentment. 17 Chronic pain patients frequently develop a “physical deconditioning syndrome” for which atrophy—reflected by a decrease in strength, flexibility and stamina—is the product of neglect of the injured area.18 Along with the physical deconditioning component, chronic pain patients can also be characterized with a “mental deconditioning” dilemma. As their emotional well-being is compromised, these chronic pain patients often become avoidant and lose touch with their daily responsibilities so that others in their social group need to not only “pick up the slack” but also, by doing so, reinforce the avoidant behaviors. 19 In this type of situation, chronic pain patients are seen to lose motivation, specifically with their family, in their physical activities and within their careers. When the lack of motivation interferes with their occupation, the chronic pain patient may also experience a significant financial burden, which can exacerbate the affective state as well.
What is the theory of pain?
The earliest theories of pain had focused primarily on the understanding of the biological or pathophysiological component of pain . Cartesian Dualism, or separation of the mind and the body, dates back to the 17th century when Rene Descartes conceptualized pain as an exclusive process within the sensory nervous system. 5 At that time, diseases and illnesses were described purely as mechanistic biological processes. Even without empirical evidence, it was conceived that the experience of pain was conveyed directly to the brain from the skin, without any psychosocial interplay. Termed biomedical reductionism, this point of view remained constant through the late 19th century. During the late 1800s, two additional theories arose, providing a clearer conceptualization of the biological view of pain. The specificity theory of pain, put forth by Maximilian von Frey in 1894, proposed that there were subcutaneous receptors unique to the different types of sensory input. 6 The distinctions between these receptors varied with respect to their functionality, such that they were designed explicitly to allow for the interpretation of sensations such as touch, temperature, pressure, or pain.
Why do people not respond to primary care?
Some patients do not respond well to either primary or secondary care for reasons relating to poor physical and psychological recovery, or other factors such as legal and work-related issues that may contribute to more pronounced emotional distress. Functional restoration, which is a form of tertiary care, has been developed for this chronic pain population. The focus of functional restoration is to avert permanent disability by utilizing a biopsychosocial approach. Within the scope of this treatment, the patient receives assistance from an interdisciplinary team of health care professionals, often including, but not limited to, a primary care physician, a psychiatrist or psychologist, a physical therapist, an occupational therapist, and a disability case manager. Together, this team develops a comprehensive plan to help the patient not only regain mobility and function, but also to teach the patient stress management techniques and coping skills necessary for dealing with any lifestyle or work issues that develop as a result of the pain and impairment. 28 Oftentimes, chronic pain patients admitted to a tertiary care program are found to be reliant on their pain medications. Although relief from pain symptoms is an appropriate course of action in the primary and secondary care programs, substance use, specifically opioid dependency, is far too common. 29 In most functional restoration programs, detoxification is found to be an essential part of treatment which is found to produce positive lifetime outcomes.
Which perspective is the most heuristic approach to understanding the concept of pain?
As the gate control and neuromatrix theories provided the opportunity to explore how the mind-body relationship relates to the pain experience, the biopsychosocial perspective has become the most heuristic approach to truly understanding the concept of pain. This approach views a physical disorder as the result of an intricate and dynamic interaction among biological, psychological, and social factors that can often antagonize the pain condition. Individuals tend to express variability in their pain experiences due to the range and interaction of these factors that modulate the interpretation of symptoms. 5,12
How did Engel change medical thinking?
Engel revolutionized medical thinking by reintroducing the idea of mind/body dualism (René Descartes) that was forgotten during the biomedical approach. After Engel's publication, the biopsychosocial model was adopted by the World Health Organization in 2002 as a basis for the International Classification of Function (ICF).
What is the biopsychosocial model?
The biopsychosocial model reflects the development of illness through the complex interaction of biological factors, psychological factors, and social factors.
Who developed the biopsychosocial model?
The biopsychosocial model was first proposed by Engel GE and Romano R in 1977. As opposed to the biomedical approach, Engel strived for a more complete approach by recognizing that each patient has their own thoughts, feelings, and history; he framed this model for both illnesses and psychological problems.
Is biopsychosocial a psychological model?
The biopsychosocial model is still widely used as a psychological model. The biological, psychological, and social categories have expanded into bigger categories: specifically, the social aspect has greatly expanded through ideas such as spirituality and culture.