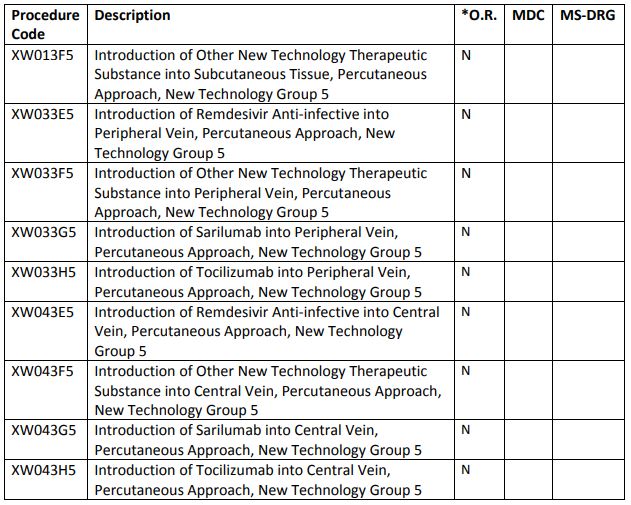
What is the difference between ICD and DRG coding?
- The addition or removal of a heavy admitting physician - especially specialty surgeons
- Opening or closing a specialty unit
- Changes in a facility's trauma level designation
- Movement of cases from the inpatient setting to outpatient, and
- Anything else that impacts the type of services the hospital provides
What does DRG stand for in medical coding?
Diagnosis-related group (DRG) is a system to classify hospital cases into one of approximately 500 groups, also referred to as DRGs, expected to have similar hospital resource use. They have been used in the United States since 1983. There is more than one DRG system being used in the United States,
Are DRG codes used for outpatient?
Since 2015, the diagnoses that are used to determine the DRG are based on ICD-10 codes. And additional codes were added to that system in 2021, to account for the COVID-19 pandemic. DRGs have historically been used for inpatient care, but the 21st Century Cures Act, enacted in late 2016, required the Centers for Medicare and Medicaid Services to develop some DRGs that apply to outpatient surgeries .
What does DRG stand for?
What Does DRG Mean? DRG stands for diagnosis-related group. Medicare's DRG system is called the Medicare severity diagnosis-related group, or MS-DRG, which is used to determine hospital payments under the inpatient prospective payment system (IPPS).

What is a DRG code in healthcare?
A diagnosis-related group (DRG) is a case-mix complexity system implemented to categorize patients with similar clinical diagnoses in order to better control hospital costs and determine payor reimbursement rates.
What is an example of a DRG?
The top 10 DRGs overall are: normal newborn, vaginal delivery, heart failure, psychoses, cesarean section, neonate with significant problems, angina pectoris, specific cerebrovascular disorders, pneumonia, and hip/knee replacement. They comprise nearly 30 percent of all hospital discharges.
How do I find my DRG code?
You have a couple of options when it comes to identifying the code. You could look it up in the ICD-10-CM/PCS code book, you could contact the coding department and ask for help, or look it up using a search engine or app on your smart device.
What is the difference between a CPT code and a DRG code?
DRG codes are used to classify inpatient hospital services and are commonly used by many insurance companies and Medicare. The DRG code, the length of the inpatient stay and the CPT code are combined to determine claim payment and reimbursement.
How do I assign a DRG code?
15:5623:32MS-DRG assignment for facility coding from principal diagnosis to DRGYouTubeStart of suggested clipEnd of suggested clipRoom in order to factor into the drg. If the case we are coding. For has any of these proceduresMoreRoom in order to factor into the drg. If the case we are coding. For has any of these procedures coded it will count as a surgical mdc.
Why are DRGs important?
Policymakers are searching for ways to control health care costs and improve quality. Diagnosis-related groups (DRGs) are by far the most important cost control and quality improvement tool that governments and private payers have implemented.
What is the difference between ICD-10 and DRG?
ICD-10 combination codes that incorporate a CC or MCC into a single diagnosis code pose an issue for DRG grouping. A combination code is a single code which represents multiple clinical issues. Clinical concepts that required two or more codes in ICD-9 only require a single combination code to be assigned in ICD-10.
Are DRGs only for inpatient?
Ambulatory payment classifications (APCs) are a classification system for outpatient services. APCs are similar to DRGs. Both APCs and DRGs cover only the hospital fees, and not the professional fees, associated with a hospital outpatient visit or inpatient stay.
Is DRG same as Revenue code?
DRG is a reimbursement methodology that uses information on the claim form (including revenue codes, diagnosis and procedure codes, patient's age, discharge status and complications) to classify the hospital stay into a group.
What are the 3 DRG options?
There are currently three major versions of the DRG in use: basic DRGs, All Patient DRGs, and All Patient Refined DRGs. The basic DRGs are used by the Centers for Medicare and Medicaid Services (CMS) for hospital payment for Medicare beneficiaries.
Is DRG a bundled payment?
Medicare's diagnosis-related groups (DRGs), which were introduced in 1983, are essentially bundled payments for hospital services, categorized by diagnosis and severity.
How many digits are in a DRG code?
4 Digit DRG? Medical Billing and Coding Forum - AAPC.
What is a DRG code?
DRG Codes (Diagnosis Related Group) Diagnosis-related group (DRG) is a system which classifies hospital cases according to certain groups,also referred to as DRGs, which are expected to have similar hospital resource use (cost). They have been used in the United States since 1983.
Is there more than one DRG system?
There is more than one DRG system being used in the United States , but only the MS-DRG (CMS-DRG) system is used by Medicare. A variety of other payers have adapted elements of the MS-DRG system including some Medicaid programs, workers compensation, and even some private payers.
What is a DRG in Medicare?
A DRG, or diagnostic related group, is how Medicare and some health insurance companies categorize hospitalization costs and determine how much to pay for your hospital stay. Rather than pay the hospital for each specific service it provides, Medicare or private insurers pay a predetermined amount based on your Diagnostic Related Group.
What is DRG system?
The DRG system is intended to standardize hospital reimbursement, taking into consideration where a hospital is located, what type of patients are being treated, and other regional factors. 4 . The implementation of the DRG system was not without its challenges.
Why is DRG payment important?
The DRG payment system encourages hospitals to be more efficient and takes away their incentive to over-treat you. However, it's a double-edged sword. Hospitals are now eager to discharge you as soon as possible and are sometimes accused of discharging people before they’re healthy enough to go home safely. 6 .
What was the DRG in the 1980s?
What resulted was the DRG. Starting in the 1980s, DRGs changed how Medicare pays hospitals. 3 .
What was included in the DRG bill?
Before the DRG system was introduced in the 1980s, the hospital would send a bill to Medicare or your insurance company that included charges for every Band-Aid, X-ray, alcohol swab, bedpan, and aspirin, plus a room charge for each day you were hospitalized.
What happens if a hospital spends less than the DRG payment?
Your age and gender can also be taken into consideration for the DRG. 2 . If the hospital spends less than the DRG payment on your treatment, it makes a profit. If it spends more than the DRG payment treating you, it loses money. 4 .
What does DRG mean in Medicare?
A DRG dictates how much Medicare pays the hospital if you’re admitted as an inpatient. However, keep in mind that your DRG does not affect what you owe for an inpatient admission when you have Medicare Part A coverage, assuming you receive medically necessary care and that your hospital accepts Medicare.
What is Medicare DRG?
What exactly is a Medicare DRG? A Medicare DRG (often referred to as a Medicare Severity DRG) is a payment classification system that groups clinically-similar conditions that require similar amounts of inpatient resources. It’s a way for Medicare to easily pay your hospital after an inpatient stay.
Why was the DRG system created?
The DRG system was created to standardize hospital reimbursement for Medicare patients while also taking regional factors into account. Another goal was to incentivize hospitals to become more efficient. If your hospital spends less money taking care of you than the DRG payment it receives, it makes a profit.
How is a DRG determined?
How is a Medicare DRG determined? A Medicare DRG is determined by the diagnosis that caused you to become hospitalized as well as up to 24 secondary diagnoses (otherwise known as complications and comorbidities) you may have. Medical coders assign ICD-10 diagnosis codes to represent each of these conditions.
What is a DRG in 2021?
April 27, 2021. A Medicare diagnosis related group (DRG) affects the pre-determined amount that Medicare pays your hospital after an inpatient admission. Understanding what it means can help you gain insight into the cost of your care. As you probably know, healthcare is filled with acronyms. Although you may be familiar with many ...
How to contact Medicare DRG?
Speak with a licensed insurance agent. 1-800-557-6059 | TTY 711, 24/7. Your Medicare DRG is based on your severity of illness, risk of mortality, prognosis, treatment difficulty and need for intervention as well as the resource intensity necessary to care for you. Here’s how it works:
Is DRG 470 a relative weight?
In 2021, DRG 195 has a relative weight of 0.6650 in while DRG 470 has a relative weight of 1.8999.
MS-DRG Definitions Manual and Software
We are providing a test version of the ICD-10 MS-DRG GROUPER Software, Version 39, so that the public can better analyze and understand the impact of the proposals included in the FY 2022 IPPS/LTCH PPS proposed rule. This test software reflects the proposed GROUPER logic for FY 2022.
HCPCS-MS-DRG Definitions Manual and Software
The 21 st Century Cures Act requires that by January 1, 2018, the Secretary develop an informational “HCPCS version” of at least 10 surgical MS-DRGs.
