What is a normal ABG for a COPD patient?
What is a normal ABG for a COPD patient? Ideally, a patient that has well-controlled COPD should in fact have a normal ABG finding. However, there are many factors involved with this. Age is a very large contributing factor. It is said that a PaO2 of 10.6-11.3 kPa (80-85 mmHg) is most likely normal for a patient with COPD.
What causes chronic obstructive pulmonary disease?
What Causes COPD?
- Smoking. About 85 to 90 percent of all COPD cases are caused by cigarette smoking. ...
- Your Environment. What you breathe every day at work, home and outside can play a role in developing COPD. ...
- Alpha-1 Deficiency. A small number of people have a rare form of COPD called alpha-1 deficiency-related emphysema. ...
What is differential diagnosis of COPD?
The differential diagnosis of COPD includes asthma, congestive heart failure, bronchiectasis, lung cancer, interstitial lung disease and pulmonary fibrosis, sarcoidosis, tuberculosis, and bronchopulmonary dysplasia. Asthma is the clinical disease that most often mimics COPD.
What is the full form of COPD?
What is the full form of COPD COPD: Chronic Obstructive Pulmonary Disease COPD stands for Chronic Obstructive Pulmonary Disease. It refers to a group of progressive lung diseases that get worse over time. The most common types of COPD are Emphysema and Chronic Bronchitis.

What is normal PaO2 for COPD?
PaO2 ≤ 55 mm Hg or SaO2 ≤ 88% taken during exercise for a patient with a PaO2 > 56 mm Hg or SaO2 > 89% during the day while at rest.
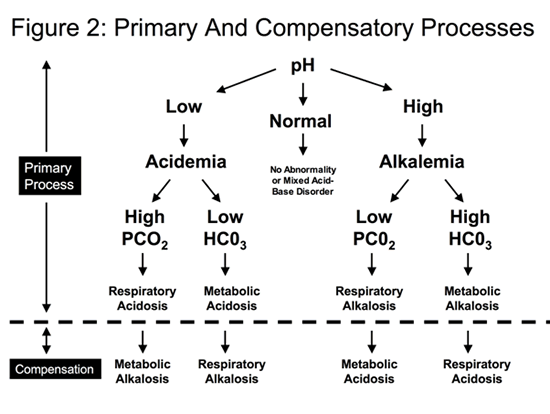
Does COPD result in acidosis or alkalosis?
COPD is one of the main causes of respiratory acidosis. The best way to prevent the condition is to protect lung health.
Why is ABG normal in COPD?
ABG's are near normal due to compensatory hyperventilation. The only subtle changes typically are a PaO2 slightly depressed (often in the mid 70's, resulting in mild pulmonary vasoconstriction), and a low-normal PaCO2.
Do COPD patients have higher CO2 levels?
Patients with chronic obstructive pulmonary disease who have worse lung function and prior history of acidotic hypercapnic respiratory failure (AHRF) are more likely to develop hypercapnia, defined as excessive carbon dioxide (CO2) in the bloodstream, a new study has found.
What acid-base imbalance is COPD?
A major complicance in COPD patients is the development of stable hypercapnia [6, 7]. Thus, the consequence of hypercapnia due to alteration of gas exchange in COPD patients mainly consists in increase of H+ concentration and development of respiratory acidosis, also called hypercapnic acidosis [8].
What labs would be abnormal with COPD?
The following laboratory findings may be seen in patients suspected to have COPD.Pulse Oximetry.Arterial Blood Gas (ABG)Hematocrit.Blood Test.Serum Electrolytes.Sputum Culture.Human B-type Natriuretic Peptide.Alpha 1 Antitrypsin Levels.
What ABG values indicate respiratory failure?
The gold standard for the diagnosis of acute hypoxemic respiratory failure is an arterial pO2 on room air less than 60 mmHg measured by arterial blood gases (ABG).
Is PaCO2 high or low in COPD?
In all patients with COPD there is the decrease of pH, PaO2 and increase of PaCO2 during follow-up period but in patients receiving complete therapy during exacerbations of COPD the changes are statistically significantly smaller than in patients not using complete therapy.
What is the normal range for ABG?
pH: 7.35-7.45. Partial pressure of oxygen (PaO2): 75 to 100 millimeters of mercury (mmHg). Partial pressure of carbon dioxide (PaCO2): 35 to 45 mmHg.
Why do you not give oxygen to COPD patients?
Too much oxygen can be dangerous for patients with chronic obstructive pulmonary disease (COPD) with (or at risk of) hypercapnia (partial pressure of carbon dioxide in arterial blood greater than 45 mm Hg). Despite existing guidelines and known risk, patients with hypercapnia are often overoxygenated.
What is a high reading for CO2?
A carbon dioxide (CO2) blood test helps healthcare providers determine if the body is balancing electrolytes properly. Results outside the normal range of 20 to 29 millimoles per liter (mmol/L) may point to a more serious issue with the kidneys or lungs.
What is CO2 retention in COPD?
Another indicator that holds promise for assessing the severity of COPD is carbon dioxide retention. Carbon dioxide retention indicates the exhaustion of lung reserve, loss of ventilatory function, worsening of clinical symptoms, respiratory failure, and secondary damage.
What happens to blood PH in COPD?
In COPD, the blood is more acidic, as the pH levels are low and the PaCO2 levels are above normal.
Is respiratory acidosis associated with COPD?
Causes of respiratory acidosis include: Diseases of the airways, such as asthma and COPD. Diseases of the lung tissue, such as pulmonary fibrosis, which causes scarring and thickening of the lungs.
What happens to PH in COPD?
In most cases, PH associated with COPD develops slowly over time and the pressure increases approximately 0.4 mmHg yearly (Kessler et al 2001). Moderately severe COPD is associated with PH in 10%–35% of patients (Scharf et al 2002; Eddahibi et al 2003). PH leads to pressure overload of the right ventricle (RV).
Why COPD can lead to respiratory acidosis?
On the contrary, chronic respiratory acidosis may be caused by COPD where there is a decreased responsiveness of the reflexes to states of hypoxia and hypercapnia. Other individuals who develop chronic respiratory acidosis may have fatigue of the diaphragm resulting from a muscular disorder.
Who performs an ABG?
An ABG can be performed by a doctor, nurse practitioner, physician assistant, registered nurse, and/or respiratory therapist. It will depend on the...
What happens before an ABG test?
Before an ABG, the patient will be informed about the test and why it is being drawn. All supplies are gathered and the blood is drawn.
What happens after an ABG test?
After the ABG is sent to the lab for analysis, the results are analyzed by the healthcare team. Changes to respiratory support or fluids are determ...
When do patients get the results?
Depending on the healthcare facility and the urgency of the results, they can be delivered in as little as 30 minutes. However, if it is a routine...
What does an ABG reveal?
An ABG will reveal several things including, pH, partial pressure of oxygen (PaO2), partial pressure of carbon dioxide (PaCO2), bicarbonate (HCO3),...
What are normal ABG levels?
pH: 7.35-7.45. Partial pressure of oxygen (PaO2): 75 to 100 mmHg. Partial pressure of carbon dioxide (PaCO2): 35-45 mmHg. Bicarbonate (HCO3): 22-26...
What is a normal ABG for a COPD patient?
Ideally, a patient that has well-controlled COPD should in fact have a normal ABG finding. However, there are many factors involved with this. Age...
What is an Arterial Blood Gas (ABG)?
An ABG is a blood test commonly performed in the ICU and ER setting; however, ABGs can be drawn on any patient on any floor depending on their diagnosis.
Why do nurses draw arterial samples?
The main issue is if the patient does not have a functioning arterial line , a frontline clinician has to draw the arterial sample. Some hospitals allow specially trained nurses or phlebotomists to perform this skill but only after an intense training program. If a provider is not available to perform the arterial stick, treatment could be delayed.
What is an ABG test?
What is an Arterial Blood Gas (ABG)? An ABG is a blood test that measures the acidity, or pH, and the levels of oxygen (O2) and carbon dioxide (CO2) from an artery.² The test is used to check the function of the patient’s lungs and how well they are able to move oxygen into the blood and remove carbon dioxide. ...
What is the blood test for oxygen?
An arterial blood gases (A BG) test is a blood test that measures the acidity, or pH, and the levels of oxygen (O2) and carbon dioxide (CO2) from an artery. The test is used to check the function of the patient’s lungs and how well they are able to move oxygen into the blood and remove carbon dioxide.
Why is the acronym "rome" used?
The acronym ROME is used to help nurses remember the relationship between pH and CO2.
What is the normal pH of blood gas?
According to the National Institute of Health, typical normal values are: pH: 7.35-7.45. Partial pressure of oxygen (PaO2): 75 to 100 mmHg. Partial pressure of carbon dioxide (PaCO2): 35-45 mmHg.
Where to draw blood for arterial gas?
Blood can be drawn via an arterial stick from the wrist, groin, or above the elbow. The radial artery on the wrist is most commonly used to obtain the sample. However, the femoral artery and brachial artery can be used if necessary.
What is type 2 respiratory failure?
Type II of respiratory failure: PaCO2> 45 mmHg (6kPa), PaO2< 60 mmHg (8kPa). Both PaO2 and PaCO2 indicate that lungs are not well ventilated; we talk about a global or hypoventilation respiratory insufficiency.
What is the treatment for anty obstructive pulmonary disease?
Smoking habits imply the duration of smoking in years, the number of cigarettes smoked per a day. The complete anty obstructive therapy involves antibiotics, combined spray therapy (inhaled corticosteroids and long acting β-agonists), eventually anticholinergic, corticosteroids and methylxanthines (either orally or intravenously). Data were collected from patients’ hospital charts in phases of exacerbations and data during remissions were taken from the competent pulmonologist of Houses of Health or Counseling Department of Clinic “Podhrastovi”.
What is the characteristic of COPD?
The basic characteristic of COPD is airflow limitation. The course of COPD is progressive and can lead to respiratory failure, but the course of disease may be made slower with appropriate continuous therapy using in phases of remissions and appropriate treatment of exacerbations of illness.
Why is respiratory failure defined as a PaO2 60 mmHg (8kPa)?
Thus, metabolic tissue consumption of oxygen must be equal to the oxygen taken up in the blood from alveolar gas. Or, metabolic tissue production of carbon dioxide must be equal to the amount of carbon dioxide blown off at the alveoli . Respiratory failure is defined as a PaO2< 60 mmHg (8kPa) and is divided into type I and type II depending on PaCO2.
What is COPD characterized by?
COPD (Chronic Obstructive Pulmonary Disease) is characterized by airflow limitation that is not fully reversible and that can lead to respiratory failure. Objective: to show the changes of arterial blood gases in COPD during the 4 -year evolution of illness. Material and Methods:
How old are patients in the 1st group?
The average age of patients in 1stgroup is 57.36 years, in 2ndgroup 61.57 and in 3rdgroup 61.58 years. Patients with 1 or less exacerbations per year are statistically significantly younger than patients with 2-3 (p=0.05) and patients with more than 3 exacerbations per year (p=0.05). There is no statistic significant difference between two last groups.
What are the co-morbidities of COPD?
Systemic manifestations and co-morbidities in COPD are body weight loss, skeletal muscle wasting, cachexia, osteoporosis, right heart failure, cardiac ischemia, cardiac arrhythmias, anemia, hypoalbuminaemia, diabetes, cognitive deficits, depression (5, 6) . Co-morbidities are common for people with COPD because organ systems work differently when they do not receive enough oxygen.
Why does pH change?
Broadly speaking the causes can be either metabolic or respiratory. The changes in pH are caused by an imbalance in the CO 2 (respiratory) or HCO 3 – (metabolic). These work as buffers to keep the pH within a set range and when there is an abnormality in either of these the pH will be outside of the normal range.
How does the respiratory system compensate for pH imbalance?
This works the other way around as well; if the cause of a pH imbalance is metabolic, the respiratory system can try and compensate by either retaining or blowing off CO 2 to counterbalance the metabolic problem (via increasing or decreasing alveolar ventilation).
What should be the first question when looking at the ABG?
Your first question when looking at the ABG should be “Is this patient hypoxic?” as hypoxia is the most immediate threat to life.
Why is it important to look at the patient's clinical status before interpreting an ABG?
Before getting stuck into the details of the analysis , it’s important to look at the patient’s current clinical status, as this provides essential context to the ABG result. Below are a few examples to demonstrate how important context is when interpreting an ABG:
What is the recommended oxygen concentration for a Venturi mask?
Venturi masks are available in the following concentrations: 24%, 28%, 35%, 40% and 60%.
How much oxygen does a simple face mask deliver?
Simple face masks can deliver a maximum FiO 2 of approximately 40%-60% at a flow rate of 15L/min. These masks should not be used with flow rates less than 5L/min.³
What is the oxygen concentration of a reservoir mask?
Reservoir masks deliver oxygen at concentrations between 60% and 90% when used at a flow rate of 10–15 l/min.³ The concentration is not accurate and will depend on the flow of oxygen as well as the patient’s breathing pattern. These masks are most suitable for trauma and emergency use where carbon dioxide retention is unlikely.
What protein is used to protect the lungs from irritants?
A family history of premature COPD may signal that you have the condition. Your doctor may check your levels of alpha-1 antitrypsin (AAT). This protein helps protect your lungs from inflammation caused by irritants such as pollution or smoking. It’s produced by your liver and then released into your bloodstream.
How to find out if you have an AAT deficiency?
People with low levels have a condition called alpha-1 antitrypsin deficiency and often develop COPD at a young age. Through genetic testing, you can find out if you have an AAT deficiency. Genetic testing for AAT deficiency is done with a blood test.
What is a reversibility test?
Bronchodilator reversibility test. This test combines spirometry with the use of a bronchodilator, which is medicine to help open up your airways. For this test, you’ll undergo a standard spirometry test to get a baseline measurement of how well your lungs are working.
Why is spirometry important?
Spirometry results help determine which type of lung disease you have and its severity. The results can be interpreted immediately. This test is the most effective because it can determine COPD before significant symptoms appear. It can also help your doctor track the progression of COPD and monitor the effectiveness of treatment.
What is COPD based on?
A diagnosis of chronic obstructive pulmonary disease (COPD) is based on your signs and symptoms, history of exposure to lung irritants (such as smoking ), and family history. Your doctor will need to do a complete physical examination before determining a diagnosis.
How long does it take to get COPD results?
Results can often be obtained within a couple of days or, at most, a couple of weeks.
What is the best test for COPD?
Spirometry. The most effective and common method for diagnosing COPD is spirometry. It’s also known as a pulmonary function test or PFT. This easy, painless test measures lung function and capacity. To perform this test, you’ll exhale as forcefully as possible into a tube connected to the spirometer, a small machine.
What does an elevated A-A gradient mean?
An elevated A-a gradient indicates that the partial pressure of O₂ is higher in the alveoli than in arterial blood, indicating a V/Q mismatch.
How is the alveolar value calculated?
The alveolar value is calculated, based on the patient's inspired FiO₂ and the PCO₂ from their blood gas result, while the arterial value is the PaO₂ from the patient's blood gas result.
What is the A-A gradient?
The alveolar-arterial (A-a) gradient is a comparison of the partial pressure of O₂ in the alveoli and in arterial blood.