Full Answer
How do you calculate effluent in CRRT?
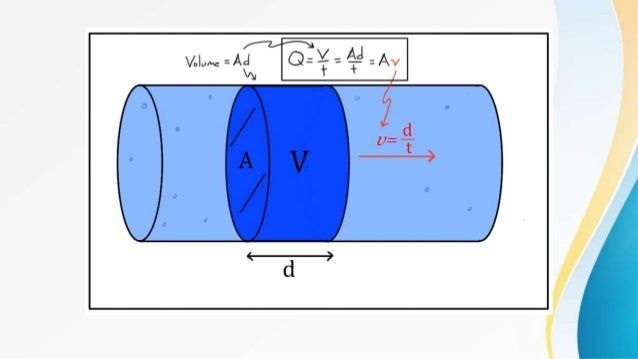
Effluent is calculated and reported by the CRRT machine and expressed as prescribed and delivered. Dialysis rate (ml/hr) + Predilution replacement rate (ml/hr) + Postdilution replacement rate (ml/hr) + Patient fluid removal (ml/hr)
How do you calculate TMP in CRRT?
Relevance to CRRT: Transmembrane pressure (TMP) = (Filter pressure + Return pressure) / 2 – (Effluent pressure) Thus, TMP is the effluent pressure subtracted from the average of the pressures in the blood side of the circuit (which are the filter pressure and the return pressure).
What is the TMP of crrt1 filter?
TMP = Filter Pressure + Return Pressure─ Effluent Pressure 2 Transmembrane Pressure (TMP) is the pressure exerted on the filtermembrane during CRRT1 Reflects the pressure difference between the blood and fluid compartments of the filter
What is transmembrane pressure (TMP) in CRRT?
Relevance to CRRT: The college examiners give this as their definition: Transmembrane pressure (TMP) = (Filter pressure + Return pressure) / 2 – (Effluent pressure) Thus, TMP is the effluent pressure subtracted from the average of the pressures in the blood side of the circuit (which are the filter pressure and the return pressure).
What is the mean creatinine level for CRRT?
How to determine efficacy of a filter?
What filter is used for CVVHDF?
What is Qr fluid?
Does effluent volume overestimate dose of small solutes?
See 2 more
About this website
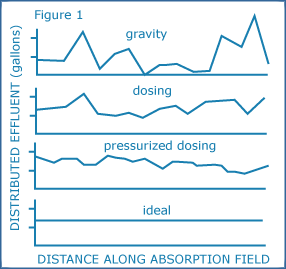
What is CRRT effluent rate?
CRRT dose is essentially quantified by the effluent flow rate and there is no survival benefit from a dose > 20 to 25 mL/kg/h [12]. We prescribe an effluent flow rate of 25 mL/kg/h to achieve a delivered dose of at least 20 mL/kg/h. Patients with severe metabolic derangements may benefit from higher CRRT dosage [13].
What does effluent mean in CRRT?
Effluent rate is the ultrafiltration rate for haemofiltration (CVVH), or the sum of ultrafiltration rate and dialysis rate for CVVHDF.
What is effluent fluid in dialysis?
Dialysate is the fluid which is infused into the filter; by convention everything that comes out of the filter is called effluent, even though it might be essentially unchanged in its composition.
What is the normal access pressure in CRRT?
This occurs relatively early during continuous RRT. For example: Access pressure -70 mmHg (-50 to -150 mmHg); Return pressure 90 mmHg (50 to 150 mmHg); Filter pressure 350 mmHg (100 to 250 mmHg) = indicative of filter clotting.
How do you calculate effluent rate in CRRT?
One way to measure delivered CRRT dose is using the clearance equation of U/P × V, in which U represents the urea nitrogen concentration in the effluent fluid, P represents the BUN concentration entering the circuit (arterial port), and V represents the total effluent fluid rate [28].
What is effluent fluid?
Effluent discharge is liquid waste, other than waste from kitchens or toilets, surface water or domestic sewage. It is produced and discharged by any industrial or commercial premises, such as a food processing factory or manufacturing business.
What are the 3 components of dialysate?
The relative amounts of water, bicarbonate, and acid components define the final dialysate composition. Bicarbonate has replaced acetate as the dialysate buffer in most countries.
What is UF in CRRT?
ULTRAFILTRATION. Ultrafiltration is the movement of water across a semi-permeable membrane because of a pressure gradient (hydrostatic, osmotic or oncotic). The increased blood pressure in the glomerulus creates a favourable driving pressure to force water across the glomerular membrane.
What is PBP in CRRT?
PRE BLOOD PUMP (PBP) The PBP is a "replacement pump" is also a form of hemofiltration. Hemofiltration refers to the removal of large volumes of plasma water across the dialysis filter in order to "drag" even more solutes toward the effluent side than would be lost by diffusion gradients alone.
What is negative pressure in dialysis?
DALP is a negative pressure that has been used to determine catheter dysfunction, which is identified when a dialysis blood flow of 300 mL/min is not being attained in a catheter previously able to deliver greater Qb than 350 mL/min and at a pre pump pressure of -250 mmHg3.
How do you know if CRRT is effective?
Check blood urea nitrogen and creatinine levels at least daily to assess CRRT efficacy. Routinely monitor the patient's complete blood counts to check for unintended blood loss in case the CRRT circuit suddenly clots. Check electrolyte levels. (Electrolytes are filtered out in the ultrafiltrate removed by CRRT.)
What is high TMP in dialysis?
High transmembrane pressure (TMP) Some machines will report the TMP together with, or instead of, the filter pressure. Again, one usually hears this alarm when the filter is dying. Causes of high TMP. TMP tends to rise gradually over the course of the dialysis session, as the filter becomes clogged with filth.
What is the difference between effluent and influent?
Influent flow refers to the untreated or contaminated water flowing into the WWTP ready for processing. Whereas Effluent flow is when the water flows out of the plant into a body of water after it has been processed.
What is effluent synonym?
sewage. pollution from the discharge of treated sewage. pollutant. outpouring. outflow.
What is pre and post dilution in CRRT?
There are two general strategies for CVVH replacement solution entering into the blood circuit: pre-dilution (in which replacement solution is mixed with the blood prior to its entry into the filter), or post-dilution (in which replacement solution is mixed with the blood after it has passed through the filter).
How do you use effluent in a sentence?
Examples of effluent in a Sentence Noun The factory has been accused of discharging effluent into the river.
Effluent volume and dialysis dose in CRRT: time for reappraisal
NATURE REVIEWS | NEPHROLOGY VOLUME 8 | JANUARY 2012 | 57 Introduction Until recently, dialysis dose was thought to have a pivotal role in improving outcomes in critically ill patients who require contin -
Effluent volume in continuous renal replacement therapy overestimates ...
Background and objectives: Studies examining dose of continuous renal replacement therapy (CRRT) and outcomes have yielded conflicting results. Most studies considered the prescribed dose as the effluent rate represented by ml/kg per hour and reported this volume as a surrogate of solute removal.
CRRT question - MICU, SICU - allnurses
The only hard part is putting up with all the f-ing bulls@#%!. Its not rocket science. Your spelling and grammar in your post were fine so you should do well in nursing school. :rotfl: I totally agree!! Thanks for the laugh!!However, you cannot mentally prepare for nursing school and you wont und...
CRRT Dosing Calculator | QxMD
Dosage in continuous renal replacement therapy (CRRT) has been assessed in multiple randomized controlled trials and two meta-analyses. Results from these studies indicate that higher intensity dialysis did not result in improved survival or clinical benefits.
Renal replacement therapy: Dose • LITFL • CCC Renal
References and Links. CCC – RRT Indications CCC – RRT principles in fluid management CCC – RRT Types CCC – RRT terminology and nomenclature CCC – RRT troubleshooting CCC – Renal Literature Summaries Social media and web resources. DerangedPhysiology.com — Determining the dose of renal replacement therapy Journal articles
What is the effluent rate?
Effluent rate is the ultrafiltration rate for haemofiltration (CVVH), or the sum of ultrafiltration rate and dialysis rate for CVVHDF
What does "dose" mean in CRRT?
Definition of "dose" in CRRT is volume of blood "purified."
What is the effluent rate for dialysis?
Most studies prescribe weight-based effluent rates as their dose of dialysis. In practical terms, the "volume of blood purified" dose of dialysis is essentially the effluent flow rate (i.e. the combination of dialysate and ultrafiltrate flow rates).Thus, when one signs the patient up for "two litre exchanges" one is prescribing an effluent rate of 2000ml/hr, and a replacement rate of 2000ml/hr (that is the "exchange volume"). This works out to be a dialysis dose of 2000ml/hr, or 28.6ml/kg/hr for a 70kg lump of human tissue. This prescribed "dose of effluent" is usually about 20% less than the actual dose of dialysis measured by marker solute, largely because the filter efficiency tends to diminish over the course of a CRRT session.
What is the sieving coefficient?
Sieving coefficient is the ratio of a solute in the ultrafiltrate in comparison to its concentration in the plasma which returns to the patient. The correct phrase is "a measure of equilibration between the concentrations of two mass transfer streams". The sieving coefficient describes the efficiency of solute removal by ultrafiltration, and depends upon the properties of the membrane and on the rate of ultrafiltration.
What determines the success of a molecule's removal by CVVHDF?
The sieving coefficient of any given molecule determines the success of its removal by CVVHDF
What is TMP in a circuit?
Thus, TMP is the effluent pressure subtracted from the average of the pressures in the blood side of the circuit (which are the filter pressure and the return pressure).
What does high TMP with normal return pressure mean?
High TMP with normal return pressure suggests there is a filter problem
What is CRRT delivered as?
CRRT is delivered using sterile fluids, therefore, solutions can be delivered as either dialysis fluid or as replacement fluids into the blood path. 2. ACCESS. Historically, early dialysis circuits required the removal of blood from an artery with return of the "cleaned" blood to a vein.
Where is ESRD inserted?
Most are inserted in the upper limb, although, the lower limb can also be used.
What is CRRT in medical terms?
CRRT = continuous renal replacement therapy. The most common complication during CRRT is circuit clotting, and the most common reason for circuit clotting is inadequate catheter function resulting in flow restriction and pressure alarms that interrupt blood flow.
What is the most common complication during CRRT?
Clotting of the extracorporeal circuit is the most common complication during CRRT. Practice patterns regarding the use of anticoagulation vary widely, with estimates of 30% to 60% of patients undergoing CRRT without anticoagulation. 62, 70 Although the use of anticoagulation is often avoided in patients who are coagulopathic, thrombocytopenic, or are having active hemorrhage, anticoagulation-free treatment may also be successful in the absence of coagulopathy and thrombocytopenia. Strategies to minimize the risk of clotting of the extracorporeal circuit include the following: use of higher blood flow rates; minimization of filtration fraction (the ratio of ultrafiltration to plasma flow) by using CVVHD rather than CVVH, or by infusing replacement fluids prefilter during CVVH and CVVHDF; ensuring optimal catheter function and responding promptly to machine alarms to minimize interruptions in blood flow; and increasing the frequency of scheduled replacement of the extracorporeal circuit. 62, 64 In the absence of anticoagulation, increased vigilance is required to ensure there is no compromise of delivered dose. 71
What is CRRT in AKI?
CRRT has become a mainstay in the management of AKI in critically ill patients. In patients who do not have objective indications for the emergent initiation of renal support, the optimal timing of RRT remains controversial. Although the use of continuous therapies may facilitate management in hemodynamically unstable patients, existing data do not show that use of CRRT results in improved survival or recovery of kidney function compared with alternatives such as conventional IHD and PIRRT. Large, well-designed clinical trials have established that for the majority of patients, augmenting solute clearance using effluent flow rates > 20 to 25 mL/kg per hour is not associated with improved outcomes; however, optimal strategies for volume management still must be defined. Similarly, other aspects of the management of CRRT are subject to substantial variations in practice, including strategies for anticoagulation. Finally, the role of CRRT needs to be considered in the setting of overall goals of care and the use of other life-sustaining treatments.
What is the criterion for discontinuing CRRT?
There are no specific criteria for discontinuation of CRRT because of recovery of kidney function or transition to other modalities of RRT. 59, 94, 95 An initial manifestation of recovery of kidney function is increased urine output, although specific criteria are sparse. In the observational Beginning and Ending Supportive Therapy for the Kidney (BEST Kidney) study, a urine output > 400 mL/d without concomitant diuretic therapy was a predictor of successful CRRT discontinuation. 96 In this observational cohort, patients who were successfully discontinued from CRRT without requiring re-initiation were more likely to survive to hospital discharge compared with those requiring re-initiation of CRRT. In another study, urine output > 500 mL/d was proposed as a criterion for discontinuation of RRT in a study of initiation and discontinuation of therapy in patients with AKI. 97 The usefulness of this criterion is uncertain, however, as the treating clinicians continued RRT despite this recommendation approximately two thirds of the time, citing continued volume overload as the most common reason for continuation of RRT. In the ATN study, a 6-h timed urine collection was obtained when the urine output was > 750 mL/d. 62 RRT was continued if the measured creatinine clearance was < 12 mL/min, was discontinued if > 20 mL/min, and was left to clinician judgment if the measured creatinine clearance was between 12 and 20 mL/min. Although these strategies can inform clinical decision-making, precise criteria for discontinuation of RRT are lacking.
How does ultrafiltration work in CVVH?
In CVVH, a high rate of ultrafiltration across the semi-permeable hemofilter membrane is created by a hydrostatic gradient, and solute transport occurs by convection ( Fig 2 A). Solutes are entrained in the bulk flow of water across the membrane, a process often referred to as “solvent drag.” 1, 27 High ultrafiltration rates are needed to achieve sufficient solute clearance, and the ultrafiltrate volume beyond what is required to achieve desired net fluid removal is replaced with balanced IV crystalloid solutions. These replacement solutions may be infused into the extracorporeal circuit either prior to or following the hemofilter. Because the high ultrafiltration rate hemoconcentrates the blood as it passes through the hemofilter fibers, the risk of sludging and fiber occlusion is increased. Prefilter infusion of replacement fluid dilutes the blood entering the hemofilter, mitigating this hemoconcentration. However, prefilter administration of replacement fluid dilutes the solute content of the blood, reducing effective solute clearance at a fixed ultrafiltration rate. Postfilter infusion has no such effects.
What is CRRT therapy?
Continuous renal replacement therapy (CRRT) is commonly used to provide renal support for critically ill patients with acute kidney injury, particularly patients who are hemodynamically unstable. A variety of techniques that differ in their mode of solute clearance may be used, including continuous venovenous hemofiltration with predominantly convective solute clearance, continuous venovenous hemodialysis with predominantly diffusive solute clearance, and continuous venovenous hemodiafiltration, which combines both dialysis and hemofiltration. The present article compares CRRT with other modalities of renal support and reviews indications for initiation of renal replacement therapy, as well as dosing and technical aspects in the management of CRRT.
What are the ethical issues associated with RRT?
Issues related to the clinical and ethical appropriateness of initiation or continuation of RRT often occur in patients with AKI. Discussions of initiation and discontinuation of therapy with patients and/or their family/surrogate decision-makers should be framed in light of the overall prognosis and goals of care, and need to consider other life-sustaining treatments in addition to RRT. It is important to ensure that both the primary managing service and nephrology consultants managing the RRT provide a consistent assessment of prognosis and treatment options, presented in a clear but sympathetic manner, to facilitate the process of shared decision-making. 98 The high mortality of AKI in the setting of critical illness and the complex and emotionally laden aspects of the decisions associated with initiating or discontinuing renal support suggest that early involvement of palliative care services may be of benefit. 99 Time-limited trials of RRT may be a useful strategy in circumstances in which there is uncertainty of prognosis or when the patient or family/surrogate decision-maker are not prepared to make a definite decision regarding initiating or discontinuing RRT and other life-sustaining care. 100
What is the effluent flow rate for CRRT?
So, for now, it seems that effluent flow rates of 20-25mL/kg/hr should be sufficient CRRT dosing in AKI – though careful attention should also be paid to actual delivered as well as clinical parameters that may justify dosing adjustments.
How much effluent volume is required for CRRT?
The KDIGO clinical practice guideline for acute kidney injury (AKI) recommends “delivering an effluent volume of 20 to 25 mL/kg/h for CRRT in (AKI) .” However, the prescribed dose is not always delivered due to CRRT interruptions due to procedures, clotting, replacement of filters, and tubing changes. Therefore, the guidelines also recommend frequent evaluation and “assessment of the actual delivered dose in order to adjust the prescription.”
How is CRRT dose calculated?
Once deciding on the modality of choice, we must choose a dose. The dose of CRRT is often estimated by the effluent flow rate (mL/kg/hr). It is commonly calculated as the ultrafiltration rate in CVVH, delivered dialysate flow rate in CVVHD, and a combination of both for CVVHDF.
What is CVVH fluid?
CVVH utilizes convection. Replacement fluid is administer ed to maintain euvolemia and dilute the plasma concentration of solutes not present in the replacement fluid (i.e. urea nitrogen, creatinine).
What is the process of a solvent passing freely across a semipermeable membrane?
Diffusion is the process by which “molecules that are present in a solvent and can pass freely across a semipermeable membrane tend to move from the region of higher concentration into the region of lower concentration.”
What are the risks of CRRT?
The risks of the therapy itself include electrolyte disturbances, clearance of trace elements or antibiotics, hypothermia, and hypotension. Although hypotension should occur less commonly than in IHD, if the net ultrafiltration rate exceeds the rate of intravascular filling, then hypotension may occur. Monitoring of electrolytes and acid-base status should be done every 6-12 hours when starting CRRT. If remaining stable after the first 24 to 48 hours, the interval may be increased to 12-24 hours. The exception, as discussed above, is when using citrate as regional anticoagulation because this requires frequent monitoring of ionized calcium levels. The removal of medications during CRRT is variable, and so it is advised to check the dose of required medications when on CRRT. This practice is especially important when it comes to the administration of antibiotics, as the trough concentrations of these medications will determine their bacteriocidal or bacteriostatic effectiveness. Many patients who meet indications for CRRT will do so as a result of sepsis, meaning that appropriate antibiotic dosage is vital. [4][5]Finally, the risks associated with the extracorporeal circuit include hypersensitivity to the circuit, air embolization, as well as blood loss with filter or circuit changes. [1]
What is CRRT in nursing?
Nursing is vital during CRRT as they have the most exposure to the vascular access site, the CRRT circuit itself, and the patient. Nursing staff and patient care technicians should be aware of complications so that intervention can be initiated early, and the physician team alerted promptly. In addition, pharmacists and nutritionists are vital to ensure proper medication doses and nutrition while on CRRT.
How long does CRRT last?
It is intended to be applied for 24 hours or longer through continuous, slower dialysis. CRRT acts as renal support through blood purification to allow solute and fluid homeostasis. It requires appropriate vascular access, pumps to allow blood circulation, a permeable membrane, and varying solutions to allow fluid balance. There are different techniques of CRRT that are distinguished by their method of solute removal.
What is CRRT therapy?
Continuous renal replacement therapy (CRRT) is one of the renal replacement methods that include intermittent hemodialysis and peritoneal dialysis. The role of the interprofessional team is reviewed. This activity details the principals, indications, and complications of continuous renal replacement therapy. Additionally, it discusses when to consider initiating CRRT and when to discontinue.
How to monitor renal function after CRRT?
There are no standards for dialysis discontinuation. One way of monitoring renal recovery is through measuring urine output; increased urine output is an indicator of improving renal function. In addition to renal function, otherfactors such as fluid overload, ongoing hemodynamic instability, or continued need for nephrotoxic medication or large volumes may need to be considered before stopping CRRT. [6]
What are the factors that determine if a patient should undergo CRRT?
There are many factors to consider when deciding whether to initiate CRRT. Two main factors are the severity of illness and the necessity of the procedure. The severity of the illness may be judged through the severity of the AKI and the observed trend. Further supporting factors would include the presence ofelectrolyte and acid-base disorders, evidence of fluid overload, and other significant organ dysfunction that requires renal support for promoting recovery. The necessity of the procedure may be judged through the assessment of the likelihood of the reversibility of the acute kidney injury (AKI), the presence of oliguria, and the nature and timing of the renal insult.
Is CRRT delivered safely?
With this team approach and good education for each member, CRRT may be delivered as safely and effectively as possible. [7]
What is the effluent rate for CRRT?
What effluent dose? The effluent fluid rate is a surrogate of solute clearance provided by CRRT and is reported in milliliters per hour and adjusted by the patient’s weight in kilograms (ml/kg per hour). When determining CRRT dose, it is recommended to use the most updated patient weight (at the time of prescribing CRRT), as it theoretically accommodates acute increases in volume of distribution due to fluid overload. The recommended average delivered effluent dose is 20–25 ml/kg per hour for patients with AKI requiring CRRT on the basis of data from the Veterans Affairs / National Institutes of Health Acute Renal Failure Trial Network Study and Randomized Evaluation of Normal versus Augmented Level Replacement Therapy Study ( 7, 15, 16 ). However, one should recognize that the prescribed dose is not always delivered due to multiple patient-related reasons, such as off-room diagnostic procedures, interventions, or CRRT-related downtime as a result of replacing filters, bags, tubing, or catheter-malfunction problems ( 17, 18 ). Therefore, a patient on CRRT requires an iterative evaluation of goals of care (solute and volume control) to adjust CRRT dose and prescription as needed ( 6 ). When prescribing high-dose CRRT (>30 ml/kg per hour), careful monitoring of electrolyte disturbances ( e.g., hypophosphatemia), nutritional deficits, and drug dosing ( e.g., antibiotics) is necessary to prevent complications. For our patient, LC, we will prescribe an effluent dose of approximately 30 ml/kg per hour (4000 ml/h) accommodating for an expected 5%–10% downtime and the predilution factor. Table 2 summarizes similar effluent doses under different CRRT modalities, including the adjustment for predilution if needed.
What is CRRT in dialysis?
CRRT is a method of dialysis support commonly utilized in patients who are critically ill with AKI. However, several aspects of CRRT delivery are still not fully standardized and do not have solid evidence-based foundations. In this study, we discussed the stepwise decision-making process made for the care of a specific patient, according to specific clinical needs and the logistics available at the corresponding institution. We provided a framework for evidence and considerations in relation to initial prescription, CRRT dosing, and adjustments related to severe hyponatremia management, concomitant ECMO support, dialysis catheter placement, use of RCA, and antibiotic dosing. This CRRT simulation highlights the importance of iterative assessment and adjustments of goals of therapy for patients on CRRT, and the need for effective communication among all multidisciplinary stakeholders involved in the care of this debilitated ICU population.
How to decrease sodium in CRRT?
Infusing electrolyte-free water as a D5W solution into the patient or into the return limb (venous return port) of the CRRT blood circuit is another approach to decrease the rate of correction of serum sodium. Safety concerns with this technique include the theoretical risk of worsening hyponatremia with filter clotting and rapid correction of sodium if consecutive D5W bags run out while the CRRT continues. The D5W infusion rate to maintain serum sodium below a desired target level could be estimated using the following formula ( 31 ): (4) For example, in this patient with initial serum sodium of 119 mEq/L, CRRT solution [Na +] of 140 mEq/L, effluent rate or clearance of 4.0 L/h, the D5W infusion should be administered at a rate 0.314 L/h (314 ml/h) to keep the serum sodium concentration at or below 127 mEq/L. The net UF setting should be increased by the rate of the D5W infusion (314 ml/h). For our patient, we will dilute the CRRT solutions (dialysate and replacement fluid) to an initial sodium concentration of 129 mEq/L in the first 24 hours, with anticipated successive adjustment of sodium concentration in CRRT solutions according to the patient’s most current serum sodium in the following 24 hours.
What is continuous RRT?
Continuous RRT (CRRT) is the preferred dialysis modality for solute management, acid-base stability, and volume control in patients who are critically ill with AKI in the intensive care unit (ICU). CRRT offers multiple advantages over conventional hemodialysis in the critically ill population, such as greater hemodynamic stability, better fluid management, greater solute control, lower bleeding risk, and a more continuous (physiologic) approach of kidney support. Despite its frequent use, several aspects of CRRT delivery are still not fully standardized, or do not have solid evidence-based foundations. In this study, we provide a case-based review and recommendations of common scenarios and interventions encountered during the provision of CRRT to patients who are critically ill. Specific focus is on initial prescription, CRRT dosing, and adjustments related to severe hyponatremia management, concomitant extracorporeal membrane oxygenation support, dialysis catheter placement, use of regional citrate anticoagulation, and antibiotic dosing. This case-driven simulation is made as the clinical status of the patient evolves, and is on the basis of step-wise decisions made during the care of this patient, according to the specific patient’s needs and the logistics available at the corresponding institution.
How to avoid rapid correction of chronic hyponatremia?
Strategies to avoid overly rapid correction of chronic hyponatremia include using hyponatremic CRRT solutions, using separate hypotonic infusions, and regulating the overall and hourly clearance delivered by CRRT using kinetic principles ( 31 ). In those with concomitant clinically significant abnormalities of other solutes ( e.g ., hyperkalemia, metabolic acidosis), decreasing the CRRT dose should be avoided. Although these strategies are helpful in predicting the rate of change in serum sodium level, frequent laboratory confirmation is still advised. Clinical factors that affect serum sodium may change over time, and readjustment of the approach may be necessary ( 31 ).
Why is functional vascular access important for CRRT?
It is critical to recognize that a functional vascular access is necessary for CRRT delivery, particularly because adequate blood flow is required to achieve CRRT goals. The latter is more relevant when prescribing convection ( e.g ., CVVH or CVVHDF) due to its effect on filtration fraction with postfilter mode and the relationship between blood flow and clearance when using prefilter mode (6:1 blood flow rate to prefilter replacement fluid ratio to maximize clearance) ( 23, 24 ). Furthermore, infection control maneuvers should be routinely employed to minimize catheter-related infections in patients on CRRT.
What is the filtration fraction of a hemofilter?
The filtration fraction is the ratio of UF rate to plasma water flow rate and represents the fraction of plasma that is removed from the blood during hemofiltration. Maintaining a filtration fraction of <20% to 25% can prolong hemofilter patency. When blood flow, hematocrit, and total effluent flow rates are held constant, purely convective modes of therapy, such as CVVH, always have a higher filtration fraction compared with diffusive therapies ( e.g ., CVVHD). Hemofilter survival can be prolonged by using higher blood flow rates and predilution replacement fluid to reduce the filtration fraction in convective CRRT. Despite these measures to improve filter survival, anticoagulation is often required for CRRT.
What is the mean creatinine level for CRRT?
The mean serum creatinine concentration at CRRT initiation was 1.64 ± 1.2 mg/dl, median daily urine output was 80 ml (24.5 to 278), and mean Sequential Organ Failure Assessment and Acute Physiology, Age, Chronic Health Evaluation 3 scores were 9.9 ± 3.6 and 111.1 ± 24.8, respectively ( Table 1 ). In 93.5% of the patients, the reason for starting dialysis was a combination of volume problems (oliguria <400 cc/24 h or signs of volume overload) and solute problems ( e.g., BUN ≥80 mg/dl and/or serum creatinine ≥6 mg/dl, electrolyte disturbances, and pH). In 6.5% of the patients, the indication for dialysis was exclusively volume related (oliguria <400 cc/24 h and/or signs of volume overload).
How to determine efficacy of a filter?
Filter efficacy was assessed by calculating fluid urea nitrogen (FUN)/BUN ratios for each 12-hour period of filter use . We assessed factors that affect treatment time in each of the CRRT treatments and ascribed them to one of the two following categories (detailed in Table 3 ): ( 1) factors affecting treatment time without affecting filter function and ( 2) factors affecting filter function.
What filter is used for CVVHDF?
Braun Diapact machine (18% of all treatments) with a polysulfone synthetic high-flux filter (Fresenius NR60). The essentials of the CVVHDF therapy setup have been previously described ( 21 ). The operational characteristics and circuit schematic are shown in Figure 1. Further description of dialysis technique and fluid balance technique are shown in Appendix 1 and Appendix 2, respectively.
What is Qr fluid?
Replacement fluid ( Qr) was comprised of 0.9% saline at a fixed rate of 500 ml/h at treatment initiation, but it could be subsequently modified between 250 and 700 ml/h.
Does effluent volume overestimate dose of small solutes?
Conclusions Effluent volume significantly overestimates delivered dose of small solutes in CRRT. To assess adequacy of CRRT, solute clearance should be measured rather than estimated by the effluent volume.

Treatment
Contraindications
Medical uses
Uses
Technology
Example
Course
Structure
Function
Operation
Pathophysiology
Administration
Research
Mechanism
Diagnosis
- Blood pressure within the hollow fibers is positive, while the pressure outside the hollow fibers is lower. Increased negativity can be generated outside the hollow fibers by the effluent pump by either increasing the fluid removal rate, or by increasing the replacement flow rate. The difference between the blood pressure in the hollow fibers and t...
Variations