What does ileitis feel like?
What ileitis feels like? Symptoms include violent and relatively acute epigastric or abdominal pain caused by penetration of larvae through the stomach or lower small intestine mucosa, especially the ileum. Nausea, vomiting, and fever may occur. Symptoms begin within 48 hours of ingestion, and quickly self-resolve or become chronic.
What does terminal ileum and colon mean?
The terminal ileum, located in the cecum,or caecum,connects the small intestine to the large. The terminal ileum is part of the digestive system. The most distant portion of the small intestine, it aids in digestion by absorbing materials not previously digested by the jejunum, the middle portion of the small intestine.
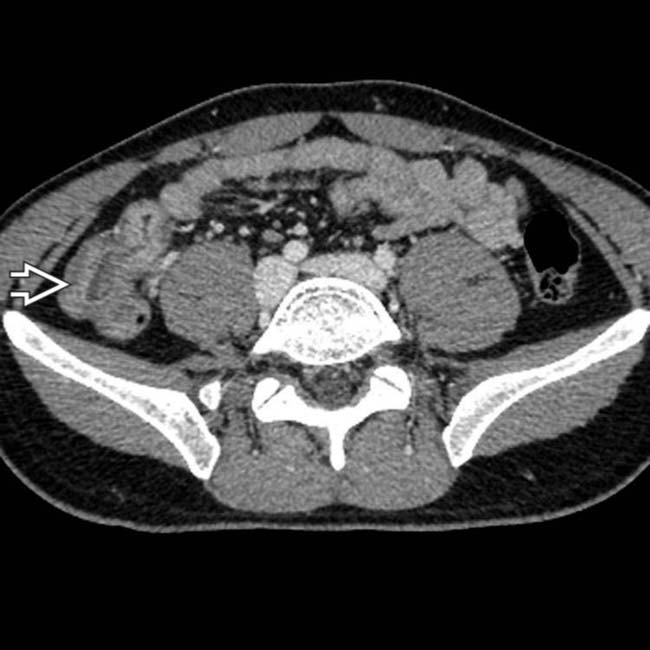
What causes thickening of the terminal ileum?
Introduction
- Normal bowel wall. Acceptable bowel wall thickness values on CT strongly depend on the degree of bowel distension and vary widely in the literature.
- Thickening of the bowel wall. Thickening of the bowel wall may be caused by several pathologic conditions or be a normal variant [ 4 ].
- Approach to the thickened bowel wall. ...
What does terminal ileum mean?
The terminal ileum is the most distal segment of the small intestine and hosts many toxic substances, including bacteria, viruses, parasites, and digested food. Therefore, it is lined by a specialized lymphoid tissue of the immune system.
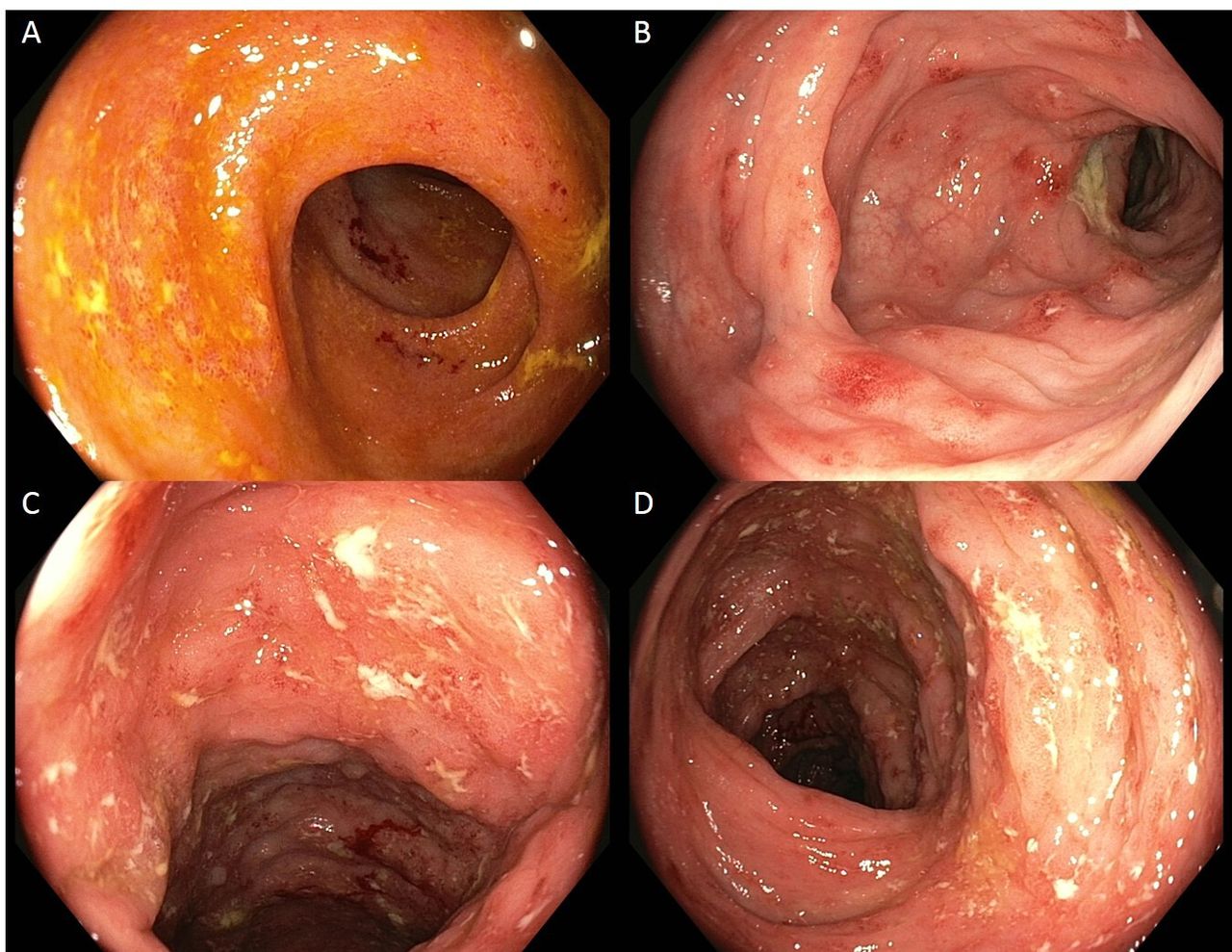
Is terminal ileitis curable?
It is a life-long chronic condition which cannot currently be cured and is part of a group of conditions known as inflammatory bowel disease (IBD).
Is terminal ileitis the same as Crohn's?
Terminal ileal and ileocaecal Crohn's in the ileum (the last part of the small intestine) may be called ileal or sometimes 'terminal ileal' Crohn's – because it is affecting the terminus or end of the ileum. If it also affects the beginning of the large bowel it is known as ileocecal Crohn's.
How is terminal ileitis diagnosed?
Knowing the difficulty in diagnosing terminal ileitis, a complete diagnostic workup is often recommended to try and get to the right diagnosis. Your doctor will likely recommend a colonoscopy with an ileoscopy.
What causes terminal ileitis?
Ileitis, or inflammation of the ileum, is often caused by Crohn's disease. However, ileitis may be caused by a wide variety of other diseases. These include infectious diseases, spondyloarthropathies, vasculitides, ischemia, neoplasms, medication-induced, eosinophilic enteritis, and others.
What does terminal ileitis feel like?
The main symptoms are abdominal pain and diarrhea [4, 78]. EG may reach the stomach and small intestine, and sometimes the colon. Patients with small-bowel EG may have abdominal pain, diarrhea, or malabsorption and ileal strictures and bowel obstruction may be observed with muscle layer involvement.
How is terminal ileitis treatment?
Based on the results of the diagnostic tests, ileitis may be treated with medications including antibiotics, corticosteroids, anti-inflammatories, antidiarrheal and immune-suppressing medications, as well as dietary supplements to reduce inflammation and manage associated symptoms.
Can you live without terminal ileum?
Removal of the valve can cause difficulty in absorbing nutrition and other digestive problems like diarrhea. However, it is possible to survive without the ileum with appropriate postoperative care, nutritional therapy, and digestive aids.
Is ileitis the same as colitis?
Ileitis: Inflames the last section of the small intestine (ileum) Gastroduodenal Crohn's: Inflames the stomach and the start of the small intestine (duodenum) Jejunoileitis: Inflames the middle part of the small intestine (jejunum) Crohn's (granulomatous) colitis: Inflames only the colon.
Can you remove terminal ileum?
Ileocecal Resection This procedure removes diseased tissue at the end of the small intestine, an area called the terminal ileum, which is often severely affected by Crohn's disease. This surgery is often required for patients with a stricture, fistula, or abscess in the terminal ileum.
What is severe ileitis?
ileitis, chronic inflammation of one or more sections of the intestine. In its strict sense, the term refers to an inflammation of the lower, or terminal, portion of the small intestine, known as the ileum.
Where is terminal ileum located?
small bowelThe terminal ileum (plural: ilea (rarely: ileums) is the most distal segment of small bowel. It immediately precedes the small bowel's connection with the colon through the ileocecal valve.
Is Crohn's considered a terminal illness?
Left untreated, Crohn's spreads throughout the intestinal tract, causing more severe symptoms and a bleaker prognosis. The disease itself is not classified as a terminal illness, but the complications that arise from it can sometimes be life-threatening.
What is terminal ileitis?
Terminal ileitis is also referred as Crohn’s disease that affects the terminal ileum or the rear part of the small intestine. It is a disease that is closely related to ulcerative colitis and both are referred to as inflammatory bowel disease.
What is the role of the immune system in terminal ileitis?
It is believed that the immune system is also attacking the digestive tract while it is warding off microorganisms from viral or bacterial infection.
What is the pain in the lower right abdomen?
Abdominal pain is the most common symptom of terminal ileitis which is often perceived in the lower right area of the abdomen. The abdominal pain can be so severe which may have a debilitating effect on the patient.
What are the factors that contribute to terminal ileitis?
The characteristic of the disease to be running in the family raised the suspicion of terminal ileitis linked with the genes in the family. Immune system is another factor believed to play a role in the incidence of terminal ileitis.
What is the best medicine for inflammation?
Immunosuppressant drugs such as methotrexate, cyclosporine, infliximab and azathioprine are considered to reduce the inflammation by suppressing the immune response of the body.
Which part of the small intestine is responsible for absorbing the materials that are not digested by the je?
The terminal ileum is the end and most distal part of the small intestine that leads to the cecum which adjoins the small intestine to the large intestine. The terminal ileum is responsible for absorbing the materials that are not digested by the jejunum or the middle part of the small intestine.
Is terminal ileitis a cure?
Terminal ileitis has no known cure just like the other inflammatory bowel disease. The aim of treatment is to relieve the symptoms that resulted from the inflammation.
What is terminal ileitis?
Ileitis also called terminal ileitis, is an inflammation of the ileum, the last part of the small intestine that joins the large intestine. Ileitis symptoms include weight loss, diarrhea, cramping or pain in the abdomen, or fistulas (abnormal channels that develop between parts of the intestine). Ileitis can be caused by a wide variety of other diseases, Crohn’s disease being the most common 1). Other causes of ileitis include infectious diseases, effects of non-steroidal anti-inflammatory drugs (NSAIDs), spondyloarthropathies, vasculitides, ischemia, neoplasms, medication-induced, eosinophilic enteritis, abnormal growths, sarcoidosis, amyloidosis, and others 2).
Why is ileitis important?
Delayed growth or sexual development, in children. The diagnosis of the cause of ileitis is of paramount importance because misdiagnosis may result in critical delays or errors in management.
What causes ischemic ileitis?
Other conditions aside from vasculitis cause ischemic ileitis. An important cause is nonocclusive mesenteric ischemia (nonocclusive mesenteric ischemia) as a result of splanchnic hypoperfusion and vasospasm observed predominantly in elderly patients with atherosclerotic vascular disease in the setting of low-flow states (eg, shock, heart failure, drugs such as cocaine). The microvasculature is patent in nonocclusive mesenteric ischemia, but blood flow is inadequate to meet intestinal tissue demands. Because the ileocolic branches are the longest branches of the superior mesenteric artery, the ileocecal region is most susceptible to ischemia from poor perfusion 50).
What are the most common causes of ileitis?
Vasculitides that are primary to the intestine or occur secondary to systemic vasculitis represent a rare cause of ileitis. The most common vasculitides with gastrointestinal involvement include the medium-sized vessel vasculitides of systemic lupus erythematosus and polyarteritis nodosa, and the small vessel vasculitides of Henoch-Schönlein purpura and Behçet’s disease. Visceral vasculitis presents with abdominal pain, nausea, vomiting, diarrhea, and gastrointestinal bleeding. Small-vessel or leukocytoclastic vasculitis is characterized by mucosal ischemia, whereas vasculitis involving medium-size or larger vessels may more likely result in transmural involvement, leading to peritoneal findings or perforation. Other serious complications include obstruction, protein-losing enteropathy, and intussusception. Moreover, patients with acquired antiphospholipid antibodies and systemic lupus erythematosus or related disorders are at increased risk for mesenteric artery thrombosis and subsequent bowel infarction 47).
What is backwash ileitis?
Backwash ileitis refers to inflammation in the distal few centimeters of terminal ileum in patients with ulcerative colitis 13). Backwash ileitis is caused by reflux of colonic contents, and when present, may raise the differential diagnosis of Crohn’s disease.
What is the best treatment for ileitis?
Based on the results of the diagnostic tests, ileitis may be treated with medications including antibiotics, corticosteroids, anti-inflammatories, antidiarrheal and immune-suppressing medications, as well as dietary supplements to reduce inflammation and manage associated symptoms.
What is the diagnosis of ileitis?
Diagnosis of the exact cause of ileitis is critical to timely treatment and the treatment plan decided by your doctor. Your doctor will review your medical history and perform a thorough physical examination.
What is the term for inflammation of the ileum?
ileitis. inflammation of the ileum; it may result from infection, obstruction, severe irritation, or faulty absorption of material through the intestinal walls. See also crohn's disease. The advanced stage is marked by hardening, thickening, and ulceration of parts of the bowel lining.
What is the advanced stage of ileitis?
The advanced stage is marked by hardening, thickening, and ulceration of parts of the bowel lining. An obstruction may cause the development of a fistula. A common symptom of ileitis is pain in the lower right quadrant of the abdomen or around the umbilicus.
What are the symptoms of distal ileitis?
Other symptoms include loss of appetite, loss of weight, anemia, and diarrhea, which may alternate with periods of constipation. Treatment may require medication to remove any source of infection, special diet, or surgery if there is obstruction. distal ileitis Crohn's disease.
What is terminal ileitis?
Terminal ileitis (TI) is an inflammatory condition of the terminal portion of the ileum described in medical literature since a long time ago. It may occur acutely with right lower quadrant pain followed or not by diarrhea, or exhibit chronic obstructive symptoms and bleeding [1-4].
What is TI in medical terms?
In 1936, the Epitome of Current Medical Literature [5] described the TI or ileitis terminalis and pointed that this condition recognized by Crohn in 1932 should be described as a new disease. In that Epitome, it is possible to read that “ileitis is a non-specific inflammation of the terminal portion of the ileum which sometimes spreads to the cecum causes ulceration of the intestinal mucosa, thickening and retraction of the intestinal wall... The diagnosis is based on the exclusion of specific infective processes in the ileum such as ileo-cecal tuberculosis and actinomycosis ”
What is TI in UC?
When TI is observed in UC, the name used is BWI that refers to an inflammation process in the distal few centimeters of terminal ileum. This inflammation condition of the ileum occurs due to reduced ileocecal valve function in severe UC (when present, may indicate the differential diagnosis of CD), allowing for retrograde flow of colonic content and inflammation of the ileum. There is stasis that occurs from inflammation-induced colonic hypomotility, or continuous extension of inflammation from the colon. This ileitis is normally mild and is related to neutrophilic inflammation in the lamina propria, focal cryptitis/crypt abscesses and, rarely, superficial mucosal erosions. Occasionally it may only exhibit mucosal injury, as villous blunting and regenerative epithelial changes. It can be differentiated from CD by the large length of involved small bowel separated by skip regions in the cecum or distal ileum, higher inflammatory process and mucosal injury in the ileum, transmural ileal inflammation and neural hyperplasia, and mucous gland metaplasia of the ileal mucosa. Literature also reports that ileal changes in UC may reach 17%. Normally, the severity of ileum inflammation parallels the severity of the colonic activity, commonly with pancolitis and cecal involvement [3, 34-36].
How are enterocolitis microorganisms acquired?
These microorganisms are mainly acquired more commonly by ingestion of contaminated water or food and the most frequent clinical aspect is the presence of enterocolitis with pain, diarrhea, low-grade fever, mucosal ulceration, neutrophil invasion, thickening of the ileal wall (leading to perforation), rectal bleeding, reactive polyarthritis and septicemia. Diagnosis is by stool culture and colonoscopy with biopsy. Endoscopic patterns include aphthoid lesions of the cecum and TI with round or oval elevations with ulcerations that are mostly uniform in size and shape, in contrast to CD. The formation of fistula and fibrotic stenosis appears commonly in CD [4, 60-62].
What is the response of the innate immune system to pathogens?
When the body is exposed to a pathogenic microorganism, the innate immune system is activated and a response of macrophages, dendritic cells and granulocytes, and activation of pattern recognition receptor which may recognize pathogen-associated molecular patterns normally named as PAMPs are observed.
How does the gastrointestinal microbiota interact with the host?
In healthy individuals, the gastrointestinal microbiota interacts with the host in a perfect balance resulting in the maintenance of homeostasis and even in healthy conditions , the gastrointestinal immune system is stimulated by millions of antigens. If this balance in lost for some reason, there is a trigger in the immune system leading ...
Is ileitis a symptom of MD?
Many studies have shown the association among MD and CD, and some authors postulate that ileitis is attributable to acid-secreting gastric heterotopia. Complications of MD are more frequent in male and younger individuals. Bleeding occurs more frequently in adult males and in children, mainly younger than 4 years of age, and it occurs mainly as obstruction [43-45].
What causes ileocolitis?
Infiltrative causes of ileitis include a number of diseases: eosinophilic gastroenteritis (EG), systemic mastocytosis, sarcoidosis and endometriosis. The endoscopic findings of EG vary from normal mucosa to mild erythema, nodularity and ulceration. Diffuse enteritis with complete loss of villi, submucosal edema, and fibrosis may be present. Multiple biopsies are required because of the patchy nature of the disease, and full-thickness surgical biopsies may be necessary if disease is confined to the muscle layer. CD can usually be differentiated by the typical architectural distortion that is not found in EG. Eosinophilic ileocolitis may be more common than originally thought and the counting of high-power microscopic fields for eosinophils may be a useful way of distinguishing eosinophilic ileocolitis from CD ileocolitis. Rarely, CD is associated with peripheral eosinophilia and/or an eosinophil-rich tissue infiltrate [20,21].
What is Yersinia enterocolitica?
Yersinia enterocoliticainfection occurs mainly in the TI and causes mucosal ulceration, neutrophil invasion, and thickening of the ileal wall. Distal ileal and cecal involvement predominates, and patients present with symptoms of small-bowel obstruction and a tender abdominal mass. The diagnosis is made most directly by colonoscopy with biopsy and culture. Endoscopic features of Yersiniainclude aphthoid lesions of the cecum and TI with round or oval elevations with ulcerations. The ulcers are mostly uniform in size and shape, in contrast to CD [8]. Mycobacterium avium-intracellulare complex infection occurs in advanced stages of HIV infection and in other immunocompromized states; it usually manifests as a systemic infection with diarrhea, abdominal pain, weight loss, fever, and malabsorption. Diagnosis is established by culture of mucosal biopsies. Disseminated histoplasmosis can also involve the ileocecal area. TI can be affected in other intestinal infections caused by Salmonella spp., cytomegalovirus. Ileitis was described in infection with Clostridium difficile(BI/NAP1/027 strains [9]), typical pseudomembranes were seen on ileal mucosa.
What is the cause of TI?
Chronic inflammation in the terminal ileum (TI) suggests a cause for the patient’s symptoms, especially when the clinical suspicion is Crohn’s disease (CD). Clinic, laboratory, endoscopic, histopathological evaluation of patients is required for the diagnosis of CD. The most frequent localization of CD is the TI. There are many other diseases affecting the TI. Non-steroidal antiinflammatory drug (NSAID) intake as well as other pathological conditions such as lymphoid hyperplasia, intestinal infections, lymphoma, infections and ulcerative colitis (UC) can mimic CD terminal ileitis.
What is the significance of ileocolonoscopy for sarcoidosis?
In patients with sarcoidosis and suspected ileitis, ileocolonoscopy with biopsy revealing noncaseating granulomas containing multinucleated giant cells is nearly diagnostic. Precise interpretation of ileal biopsies is crucial because CD, mycobacterial infections, histoplasmosis and lymphoma are granulomatous conditions that mimic sarcoidosis.
What causes chronic inflammation in TI?
Ulcerative colitis as a cause of chronic inflammation in TI
Why are malignant tumors of the small intestine easy to misdiagnose?
Primary malignant tumors of the small intestine are easy to be misdiagnosed because of nonspecific symptoms and signs and the limited examination methods. In the ileum, malignant lymphoma constitutes about half of all malignancies (48.3% in this group), followed by adenocarcinoma, leiomyosarcoma and carcinoid tumors.
Is focal lymphoid hyperplasia a terminal ileitis?
Focal lymphoid hyperplasia of the TI is a rare cause of terminal ileitis. In 1996 the case of a 13-year-old boy was described with a stricture of the TI that was diagnosed as CD on barium follow through. This patient had no response to steroid therapy and the boy required resection of TI. Histology findings of TI showed focal lymphoid hyperplasia and not CD [10].
What causes ileitis?
However, ileitis may be caused by a wide variety of other diseases. These include infectious diseases, spondyloarthropathies, vasculitides, ischemia, neoplasms, medication-induced, eosinophilic enteritis, and others. The clin …. Ileitis, or inflammation of the ileum, is often caused by Crohn's disease. However, ileitis may be caused by ...
Is ileitis associated with spondylarthropathy?
Ileitis associated with spondylarthropathy or nonsteroidal anti- inflammatory drugs is typically subclinical and often escapes detection unless further testing is warranted by symptoms. In a minority of patients with long-standing Crohn's ileitis, the recrudescence of symptoms may represent a neoplasm involving the ileum.
Is ileitis caused by a disease?
However, ileitis may be caused by a wide variety of other diseases. These include infectious diseases, spondyloarthropathies, vasculitides, ischemia, neoplasms, medication-induced, eosinophilic enteritis, and others. The clinical presentation of ileitis may vary from an acute and self-limited form of right lower quadrant pain and/or diarrhea, ...
What is a single-contrast enema study in a patient with total colitis?
Inflammatory bowel disease. This single-contrast enema study in a patient with total colitis shows mucosal ulcers with a variety of shapes, including collar-button ulcers, in which undermining of the ulcers occurs, and double-tracking ulcers, in which the ulcers are longitudinally oriented. Inflammatory bowel disease.
What is plasmacytosis in ulcerative colitis?
Inflammatory bowel disease. Basal plasmacytosis in ulcerative colitis. Plasma cells separate the crypt bases from the muscularis mucosae.
What is an example of low grade glandular dysplasia in a patient with longstanding ulcerative colitis?
Inflammatory bowel disease. This is an example of low-grade glandular dysplasia in a patient with longstanding ulcerative colitis. Note the loss of mucin, nuclear hyperchromasia, and nuclear pseudostratification. See the next image.
What is the high power view of a crypt abscess in ulcerative colitis?
Inflammatory bowel disease. High-power view of a crypt abscess in ulcerative colitis shows the crypt to be dilated and filled with neutrophils and debris.
What is an example of a deep fissuring ulcer in a patient with Crohn's disease?
Inflammatory bowel disease. Another example of a deep, fissuring ulcer in a patient with Crohn disease. Note the increase in submucosal inflammation and scattered lymphoid aggregates.
What is the name of the disease that causes inflammation of the descending colon?
Inflammatory bowel disease. This colonoscopic image of a large ulcer and inflammation of the descending colon in a 12-year-old boy with Crohn disease.
Where does barium enter the sigmoid colon?
Note that barium is just starting to enter the cecum in the right lower quadrant (viewer's left), but the barium has also started to enter the sigmoid colon toward the bottom of the picture , thus indicating the presence of a fistula from the small bowel to the sigmoid colon. Inflammatory bowel disease.
