
Some of the most common causes include:
- Endotracheal tube insertion
- Aspiration of bacteria
- Inappropriate body positioning
- Inadequate suctioning
- Inadequate oral care
- Circuit contamination
- Inadequate weaning
What is ventilator-associated pneumonia?
Ventilator-associated Pneumonia (VAP) Ventilator-associated pneumonia is a lung infection that develops in a person who is on a ventilator. A ventilator is a machine that is used to help a patient breathe by giving oxygen through a tube placed in a patient’s mouth or nose, or through a hole in the front of the neck.
What causes ventilator-associated pneumonia (VAP)?
Ventilator-associated pneumonia caused by potentially drug-resistant bacteria. Am. J. Respir. Crit. Care Med.157:531-539. [PubMed] [Google Scholar]
What is the most common pathogen associated with ventilator associated pneumonia?
The two most frequent pathogens of VAP were S. aureusand A. baumanii. There were no pathogenic differences between early and late onset VAP. Keywords: Pneumonia, Ventilator Associated; Staphylococcus aureus; Acinetobacter baumanii Introduction Ventilator associated pneumonia (VAP) occurs 48 hours after intubation and mechanical ventilation.
What is the prevalence of ventilator-associated pneumonia in the US?
An estimated 49,900 ventilator-associated pneumonia infections occur in non-neonatal intensive care units annually. VAP rates may exceed 10 cases per 1,000 ventilator days in some neonatal and surgical patient populations ( citation)
What bacteria causes ventilator-associated pneumonia?
Common causative pathogens of VAP include Gramnegative bacteria such as Pseudomonas aeruginosa, Escherichia coli, Klebsiella pneumoniae, and Acinetobacter species, and Gram-positive bacteria such as Staphylococcus aureus9-14.
How is ventilator-associated pneumonia acquired?
An infection may occur if germs enter through the tube and get into the patient's lungs. CDC provides guidelines and tools to the healthcare community to help end ventilator-associated pneumonia and resources to help the public understand these infections and take measures to safeguard their own health when possible.
How do you prevent ventilator-associated pneumonia?
This article reviews the top five evidence-based nursing practices for reducing VAP risk in critically ill adults.Minimize ventilator exposure. ... Provide excellent oral hygiene care. ... Coordinate care for subglottic suctioning. ... Maintain optimal positioning and encourage mobility. ... Ensure adequate staffing.
What causes ventilator-associated events?
Research suggests that most VACs are due to pneumonia, ARDS, atelectasis, and pulmonary edema [16]. These are significant clinical conditions that may be preventable. VAE rates and event characteristics in adult inpatient locations reporting data to NHSN in 2014 have been published [18].
What are the signs and symptoms of VAP?
Ventilator-associated pneumonia (VAP) occurs in patients that have been on mechanical ventilation for more than 48 hours. It presents with clinical signs that include purulent tracheal discharge, fevers, and respiratory distress in the presence of microorganisms.
What is the best indicator of ventilator-associated pneumonia?
Ventilator-associated pneumonia is usually suspected when the individual develops a new or progressive infiltrate on chest radiograph, leukocytosis, and purulent tracheobronchial secretions.
Can ventilator-associated pneumonia be cured?
The mortality in ventilator-associated pneumonia is high despite the availability of effective antibiotics. However, not all mortality is attributable to the pneumonia itself; many of the deaths are related to the patient's underlying illness. Adequacy of initial antimicrobial therapy clearly improves prognosis.
How long does ventilator-associated pneumonia last?
The role of inhaled antibiotics in the setting of failure of systemic antibiotics is unclear [1]. The usual duration of treatment for early-onset VAP is 8 days and longer in the case of late-onset VAP or if MDR organisms are suspected or identified [39–41].
What are the complications of ventilator-associated pneumonia?
Ventilator-associated pneumonia (VAP), sepsis, Acute Respiratory Distress Syndrome (ARDS), pulmonary embolism, barotrauma, and pulmonary edema are among the complications that can occur in patients receiving mechanical ventilation; such complications can lead to longer duration of mechanical ventilation, longer stays ...
What are the most common conditions that trigger ventilator-associated events?
Four common conditions that are often associated with ventilator-associated events are pneumonia, atelectasis, fluid overload and acute respiratory distress syndrome.
What are the 5 components of the VAP bundle?
The PICU 5-element VAP prevention bundle consisted of: 1) age-appropriate oral care, 2) proper airway suction technique, 3) maintenance of safe endotracheal tube cuff pressures, 4) application of aspiration precautions, and 5) head-of-bed elevation.
What is difference between VAP and VAE?
Ventilator-associated event (VAE) definitions were first released by the United States Centers for Disease Control and Prevention (CDC) in 2013. The CDC created VAE definitions to replace their longstanding surveillance definitions for ventilator-associated pneumonia (VAP).
Is ventilator-associated pneumonia hospital acquired?
Hospital-acquired (or nosocomial) pneumonia (HAP) is pneumonia that occurs 48 hours or more after admission and did not appear to be incubating at the time of admission. Ventilator-associated pneumonia (VAP) is a type of HAP that develops more than 48 hours after endotracheal intubation.
How long does it take to develop ventilator-associated pneumonia?
Ventilator-associated pneumonia (VAP) is a type of hospital-acquired pneumonia (HAP) that develops after more than 48 hours of mechanical ventilation [1].
What is the difference between community acquired and ventilator acquired pneumonia?
Pneumonia that presents sooner should be regarded as community acquired pneumonia. VAP refers to nosocomial pneumonia that develops among patients on ventilators. Ventilator-associated pneumonia (VAP) is defined as pneumonia that presents more than 48 hours after endotracheal intubation.
What are 4 causes of hospital acquired pneumonia?
MRSA, P. aeruginosa, and other gram-negative intestinal bacteria often are resistant to certain antibiotics. Viruses and fungi are increasingly being recognized as causes of hospital-acquired pneumonia.
How many pneumonia infections are ventilator related?
More than one-third (39%) of pneumonia infections in acute care hospital settings are estimated to be ventilator-associated.
How many cases of VAP per 1,000 ventilator days?
VAP rates may exceed 10 cases per 1,000 ventilator days in some neonatal and surgical patient populations ( citation) Patients with VAP require long period of mechanical ventilation, extended hospitalizations, and increased use of antibiotics. ( citation)
What is a VAP?
Ventilator-associated pneumonia (VA P) is a type of lung infection that occurs in a person who has been on a ventilator. A ventilator is a machine that helps a person breathe by giving oxygen through a tube placed in the mouth, nose, or through a hole in the front of the neck. Germs can enter the ventilator and get into the patient’s lungs, ...
How to clean hands after ventilator?
Clean their hands with soap and water or an alcohol-based hand rub before and after touching the patient or the ventilator.
Can germs enter a ventilator?
Germs can enter the ventilator and get into the patient’s lungs, causing illness. Factors that may increase a patient’s risk of developing VAP include prolonged intubation, enteral feeding, witnessed aspiration, paralytic agents, underlying illness, and age.
What is the risk of pneumonia in ventilators?
Endotracheal intubation is the major risk factor for ventilator-associated pneumonia. Endotracheal intubation breaches airway defenses, impairs cough and mucociliary clearance, and facilitates microaspiration of bacteria-laden secretions that pool above the inflated endotracheal tube cuff.
What is the most common pathogen in ventilator-associated pneumonia?
The most common pathogens are gram-negative bacilli and Staphylococcus aureus; antibiotic-resistant organisms are an important concern. In ventilated patients, pneumonia usually manifests as fever, increase in white blood cell count, worsening oxygenation, and increased tracheal secretions that may be purulent. Diagnosis is suspected on the basis of clinical presentation and chest x-ray and is sometimes confirmed by a positive blood culture for the same pathogen found in respiratory secretions or bronchoscopic sampling of the lower respiratory tract with quantitative Gram stain and cultures. Treatment is with antibiotics. Overall prognosis is poor, due in part to comorbidities.
What are the risk factors for VAP?
Other risk factors for antibiotic-resistant organisms specific to VAP include. Septic shock at time of VAP. Acute respiratory distress syndrome (ARDS) preceding VAP. Hospitalization for ≥ 5 days prior to the occurrence of VAP.
How to prevent ventilator pneumonia?
There are a number of measures that can help prevent ventilator-associated pneumonia. Semiupright or upright positioning reduces risk of aspiration and pneumonia compared with recumbent positioning and is the simplest and most effective preventive method.
When is VAP most likely to occur?
The highest risk of VAP occurs during the first 10 days after intubation. Ventilator-associated pneumonia occurs in 9 to 27% of mechanically ventilated patients.
What is the cause of fever and increased heart rate?
Pneumonia in critically ill, mechanically ventilated patients more typically causes fever and increased respiratory rate or heart rate or changes in respiratory parameters, such as an increase in purulent secretions or worsening hypoxemia.
Is inflammatory mediators in bronchoalveolar lavage fluid reliable?
Measurement of inflammatory mediators in bronchoalveolar lavage fluid or serum has not been shown to be reliable in deciding on initiation of antibiotic s. The only finding that reliably identifies both pneumonia and the responsible organism is a pleural fluid culture (obtained via thoracentesis in a patient with pleural effusion) that is positive for a respiratory pathogen.
What is ventilator-associated pneumonia?
Ventilator-associated pneumonia is usually suspected when the individual develops a new or progressive infiltrate on chest radiograph, leukocytosis, and purulent tracheobronchial secretions. Unfortunately, and unlike for community-acquired pneumonia, accepted clinical criteria for pneumonia are of limited diagnostic value in definitively establishing the presence of VAP. In a postmortem study by Fabregas et al., when findings on histologic analysis and cultures of lung samples obtained immediately after death were used as references, a new and persistent (>48-h) infiltrate on chest radiograph plus two or more of the three criteria (i) fever of >38.3°C, (ii) leukocytosis of >12 × 109/ml, and/or (iii) purulent tracheobronchial secretions had a sensitivity of 69% and a specificity of 75% for establishing the diagnosis of VAP (60). When all three clinical variables were required for the diagnosis, the sensitivity declined further (23%); the use of a single variable resulted in a decrease in specificity (33%). The poor accuracy of clinical criteria for diagnosing VAP should not be surprising considering that purulent tracheobronchial secretions are invariably present in patients receiving prolonged mechanical ventilation and are seldom caused by pneumonia. In addition, the systemic signs of pneumonia such as fever, tachycardia, and leukocytosis are nonspecific; they can be caused by any state that releases the cytokines interleukin-1, interleukin-6, tumor necrosis factor alpha, and gamma interferon (33, 34, 63, 135). Examples of such conditions include trauma, surgery, the fibroproliferative phase of ARDS, deep vein thrombosis, pulmonary embolism, and pulmonary infarction. Reasonable clinical criteria for the suspicion of VAP include a new and persistent (>48-h) or progressive radiographic infiltrate plus two of the following: temperature of >38°C or <36°C, blood leukocyte count of >10,000 cells/ml or <5,000 cells/ml, purulent tracheal secretions, and gas exchange degradation (5, 103).
Why is VAP overtreatment?
Due to poor specificity and poor positive predictive value, reliance on clinical parameters, chest X-ray findings, and non- and semiquantitative sputum analysis will result in overdiagnosis and therefore overtreatment of VAP. Such an approach will result in excess antibiotic use with its attendant cost, potential toxicity, and selection of drug-resistant organisms. A recent decision analysis suggested that more deaths occurred if patients were treated with antibiotics on the basis of only clinical suspicion of VAP than if antibiotics were withheld (190).
What is the threshold for pneumonia?
For each of the quantitative culturing methods, threshold values have been derived and are expressed in CFU per milliliter. If the number of CFU/ml is equal to or exceeds the threshold values for the particular technique, a diagnosis of pneumonia is made. Threshold values often employed for diagnosing pneumonia by quantitative cultures are ≥105to 106, ≥104, and ≥103CFU/ml for QEA, bronchoscopic BAL, and PSB, respectively, with ≥105CFU/ml being the most widely accepted value for QEA (12, 30). For “blind” distal sampling, the thresholds are ≥103CFU/ml for PSB and mini-BAL and ≥104CFU/ml for cultures obtained with BBS and unprotected BAL (Table (Table1)1) (30).
Where to sample for pulmonary infiltrate?
When in doubt, sample the posterior right lower lobe, since autopsy studies have indicated that VAP frequently involves this area (61, 92, 130, 173). Multiple specimens are no more accurate than single specimens (136).
Can a portable chest X-ray detect pneumonia?
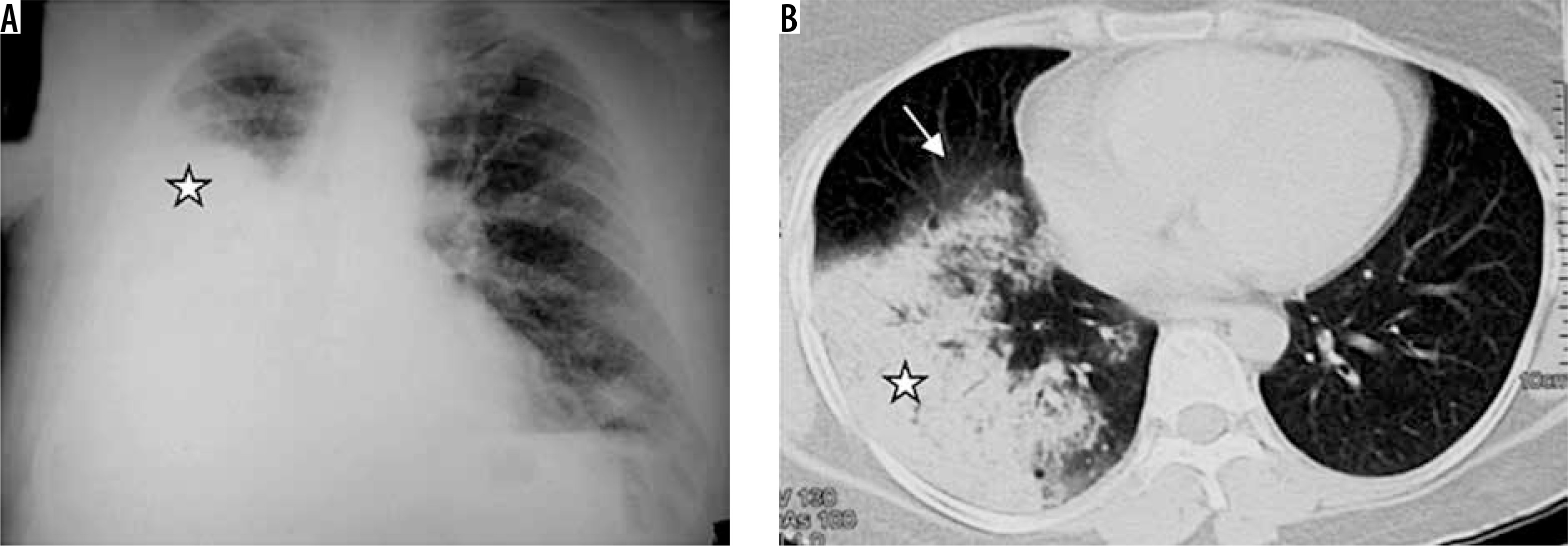
While the portable chest radiograph still remains a mandatory component in the diagnosis of ventilated patients with suspected pneumonia, as with clinical criteria for diagnosing VAP, it too has problems with both sensitivity and specificity. Poor-quality films further compromise the accuracy of chest X rays. Although a normal chest radiograph makes VAP unlikely, in one study of surgical patients , 26% of opacities were detected by computed tomography (CT) scan but not by portable chest X ray (25) . In addition, asymmetric pulmonary infiltrates consistent with VAP can be caused by numerous noninfectious disorders, including atelectasis, chemical pneumonitis, asymmetric cardiac pulmonary edema, pulmonary embolism, cryptogenic organizing pneumonia, pulmonary contusion, pulmonary hemorrhage, drug reaction, and asymmetric ARDS. The overall radiographic specificity of a pulmonary opacity consistent with pneumonia is only 27% to 35% (116, 216).
Can chest radiographs be used to diagnose pneumonia?
Nonetheless, because of their high specificity, certain chest radiograph findings can be useful in establishing the diagnosis of pneumonia when present. Based on several studies, including an autopsy study by Wunderink et al., these useful findings include rapid cavitation of the pulmonary infiltrate, especially if progressive; an air space process abutting a fissure (specificity, 96%); and an air bronchogram, especially if single (specificity, 96%). Unfortunately, such radiographic abnormalities are uncommon (216).
Is VAP a sensitivity?
The sensitivity of the clinical criteria for VAP outlined above is even lower in patients with ARDS, where it may be difficult to detect new radiographic infiltrates. In the setting of ARDS, Bell et al. reported a false-negative rate of 46% for the clinical diagnosis of VAP (11). Consequently, suspicion for VAP in the setting of ARDS should be high. The presence of even one of the clinical criteria for VAP, unexplained hemodynamic instability, or an unexplained deterioration in arterial blood gases should prompt consideration of further diagnostic testing (129).
What is ventilator pneumonia?
Ventilator-associated pneumonia is the second most common hospital-acquired infection among pediatrics and neonatal intensive care unit patients. It accounts for 7% to 32% of healthcare-associated infections and 10% of all pediatric device-related infections reported to the National Healthcare Safety Network (NHSN).
What are the symptoms of ventilator-associated pneumonia?
Ventilator-associated pneumoniaincludes clinical signs of purulent tracheal discharge, fevers, respiratory distress, and micro-biological signs of the presence of microorganisms along with white blood cells in the tracheal aspirate along withradiological evidence of pneumonia.
What is VAP in medical terms?
Ventilator-associated pneumonia (VAP) is a term used to describe pneumonia (lung infection) that develops in a patient who has been on mechanical ventilation for more than 48 hours.
What are the different types of pneumonia?
They have classified it as three types: (1) clinically defined, (2) pneumonia with laboratory findings, and (3) pneumonia in immunocompromised patients. Infants and children are usually classified to the first category. Tracheitis Versus Ventilator-associated Pneumonia.
Is pneumonia in neonates inversely proportional to birth weight?
In neonates, the rate of ventilator-associated pneumonia is inversely proportional to birth weight.
What causes VAP in the gut?
Most cases of VAP are caused by bacterial pathogens that normally colonize the oropharynx and gut, or that are acquired via transmission by health-care workers from environmental surfaces or from other patients.
What is VAP in medical terms?
The microbiology of ventilator-associated pneumonia. Ventilator-associated pneumonia (VAP) is a common complication of ventilatory support for patients with acute respiratory failure and is associated with increased morbidity, mortality, and costs.
What is VAP in healthcare?
Ventilator-associated pneumonia (VAP) is a common complication of ventilatory support for patients with acute respiratory failure and is associated with increased morbidity, mortality, and costs. Awareness of the microbiology of VAP is essential for selecting optimal antibiotic therapy and improving these outcomes. The specific microbial causes of VAP are many and varied. Most cases of VAP are caused by bacterial pathogens that normally colonize the oropharynx and gut, or that are acquired via transmission by health-care workers from environmental surfaces or from other patients. Common pathogens include Pseudomonas species and other highly resistant Gram-negative bacilli, staphylococci, the Enterobacteriaceae, streptococci, and Haemophilus species. Antibiotic-resistant pathogens such as Pseudomonas and Acinetobacter species and methicillin-resistant strains of Staphylococcus aureus are much more common after prior antibiotic treatment or prolonged hospitalization or mechanical ventilation, and when other risk factors are present. The bacterial pathogens responsible for VAP also vary depending on patient characteristics and in certain clinical circumstances, such as in acute respiratory distress syndrome or following tracheostomy, traumatic injuries, or burns. But these differences appear to be due primarily to the duration of mechanical ventilation and/or degree of prior antibiotic exposure of these patients. The causes of VAP can vary considerably by geographic location (even between units in the same hospital), emphasizing the importance of local epidemiological and microbiological data. Atypical bacteria, viruses, and fungi also have been implicated as causes of VAP, but these pathogens have not been studied systematically and their role is presently unclear. In conclusion, information about the microbiology of VAP serves to guide optimal antibiotic therapy. The risk of antibiotic-resistant pathogens can be estimated using simple clinical features and awareness of local microbiology patterns. The roles of atypical bacterial and nonbacterial pathogens in VAP are incompletely understood and should be investigated further.
What is the most common pathogen after antibiotic treatment?
Antibiotic-resistant pathogens such as Pseudomonas and Acinetobacter species and methicillin-resistant strains of Staphylococcus aureus are much more common after prior antibiotic treatment or prolonged hospitalization or mechanical ventilation, and when other risk factors are present.
How to diagnose pneumonia?
Pneumonia was diagnosed by chest radiograph and clinical and laboratory findings. If the patients, who had a new pulmonary infiltration, satisfied 2 or more conditions among the cases of body temperature 38.3℃ or higher, purulent bronchial secretions, and a leukopenia or leukocytosis (<4,000 or >11,000 mm3), they were diagnosed with pneumonia15. The patient's age, gender, a history of antibiotic therapy before hospitalization, a history of hospitalization in other hospitals, concurrent diseases, causes of mechanical ventilation, causative pathogens, antibiotic resistances, and mortality were retrospectively examined. The subjects were divided into two groups according to the development time of VAP: early VAP group where VAP occurred within 5 days after mechanical ventilation and late VAP group where VAP occurred 5 days or later after mechanical ventilation. A comparative analysis was conducted between the two groups10,15.
What are the causes of VAP?
Common causative pathogens of VAP include Gramnegative bacteria such as Pseudomonas aeruginosa, Escherichia coli, Klebsiella pneumoniae, and Acinetobacterspecies, and Gram-positive bacteria such as Staphylococcus aureus9-14. As the type of causative pathogens and the rate of drug-resistant pathogens may vary depending on region and hospital, data of microbial surveillance are required for each region. As most studies on causative pathogen, however, have been conducted in western counties, domestic data are insufficient. Accordingly, this study was conducted to investigate the bacterial pathogens of VAP in a domestic tertiary referral hospital.
What is VAP in ICU?
VAP is one of serious complications that occur at ICU. As its causative pathogens are antibiotic resistant in many cases, it is difficult to select appropriate antibiotics. In addition, the mortality has been reported to increase if an early antibiotic treatment is not provided to patients with VAP18. Thus, before the identification of causative pathogens, antibiotic selection is performed to target causative pathogens mainly identified in the corresponding region. However, most studies on causative pathogens have been conducted in western countries, and few studies have been conducted in Korea. According to the SENTRY antimicrobial surveillance program operated in US, Europe, and South America, P. aeruginosa(27%) is the most common causative pathogen taken all regions together, and S. aureus(20%), and Acinetobacterspecies (14%) follow P. aeruginosain that order. In the US, S. aureus(32%) is the most common causative pathogen, followed by P. aeruginosa(21%), Enterobacterspecies (9%), and Acinetobacterspecies (4.4%) in that order11. Meanwhile, according to a recent study on the causative pathogens of nosocomial pneumonia in Asia, S. aureus(27%) was the most common causative pathogen of nosocomial pneumonia in Korea, and Acinetobacter species(16%), P. aeruginosa(14%), and K. pneumoniae(9%) followed S. aureusin that order17. Although this was different from the result of foreign studies, it was similar to the result of this study. Thus, in Korea, causative pathogens of VAP are likely to occur at the aforementioned frequency.
What are the two most common pathogens of VAP?
The two most frequent pathogens of VAP were S. aureusand A. baumanii. There were no pathogenic differences between early and late onset VAP.
Which pathogen is most likely to cause VAP?
In this study, S. aureuswas shown to be the most common causative pathogen of VAP at ICU, and A. baumanii, P. aeruginosa, S. maltophilia, K. pneumonia, and Serratia marcescensfollowed S. aureusin that order. No difference in the causative pathogens was found between the early and late VAP groups according to the development time of VAP.
How long after intubation does pneumonia occur?
Ventilator associated pneumonia (VAP) occurs 48 hours after intubation and mechanical ventilation. It is a common infectious disease that is found in intensive care unit (ICU), which occurs in 8~38% of patients who underwent mechanical ventilation1. The incidence of pneumonia has been known to be higher in ICU patients than in general ward patients, and even 3~10-fold higher in patients who underwent mechanical ventilation2-9. In addition, the mortality of VAP has been reported to be 24~76%, which is higher than those of other hospital acquired infections10.
How many bacterial pathogens were in the VAP?
A total of 109 bacterial pathogens from 91 adult patients with VAP, who were admitted to the medical intensive care unit from January 2008 to December 2009, were examined. Clinical characteristics, bacterial pathogens, and resistance profiles were analyzed.
