What is the first stage of plaque formation?
- Stage 1: Formation of an acellular layer.
- Stage 2: Initial attachment.
- Stage 3: Irreversible attachment.
- Stage 4: Early Maturation (also called Maturation I).
- Stage 5: Late Maturation (also called Maturation II).
- Stage 6: Dispersion.
What is the first step in plaque formation?
First step in plaque formation is: Adhesion and attachment Of Bacteria 31. Bacterial Adherence During initial adherence, interactions occur mainly between specific bacteria and the pellicle.
What is plaque formation and its characteristics?
Plaque formation. Dental plaque is a biofilm that attaches to tooth surfaces, restorations and prosthetic appliances (including dentures and bridges) if left undisturbed. Understanding the formation, composition and characteristics of plaque helps in its control.
What is the meaning of plaque activity?
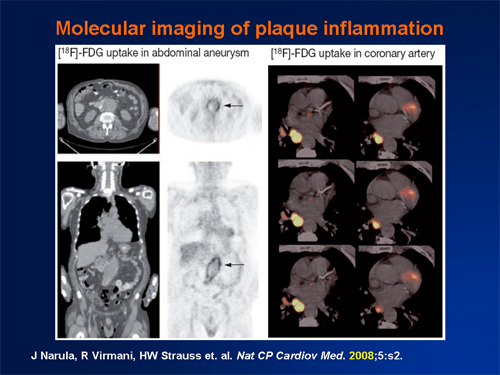
It is a difficult concept because disease or plaque activity does not have a simple, defined meaning. Often it is taken to mean inflammation, measured for instance as the density of macrophages in plaques. This is reasonable given the central role of vascular inflammation in plaque development.
What is the pathophysiology of dental plaque?
Dental plaque is an adherent, bacterial film, and is the main pathological agent for periodontal diseases. The formation of dental plaque can occur both supragingivally and subgingivally. The development of plaque is a three-step process. Following the formation of a pellicle, pioneer micro-organism …

What are the phases of plaque formation?
The development of plaque is a three-step process. Following the formation of a pellicle, pioneer micro-organisms will adhere to it, proliferate and form colonies. The final stage involves the aggregation of filamentous organisms and spirochetes into a cohesive biofilm.
What is the life cycle of plaque?
Four stages of dental plaque biofilm growth: Stage I attachment (lag [not inert, but metabolically reduced]), Stage II growth (log [exponential growth]), Stage III maturity (stationary) and Stage IV dispersal (death) ( Thomas et al 2006).
What is the bacteria that 1st to colonize plaque?
These studies consistently demonstrated that the early plaque microbiota is constituted primarily by Streptococcus species, in particular Streptococcus mitis and Streptococcus oralis, with a subset of nonstreptococcal species, such as Neisseria, Rothia, and Gemella.
What comes first plaque or calculus?
If plaque is not cleaned and is allowed to accumulate over the teeth, it hardens over time and becomes calculus or tartar. Calculus also provides a safe breeding ground for harmful bacteria which promotes gum and periodontal disease.
What is plaque formation?
Plaque is a sticky film of bacteria that constantly forms on teeth. Bacteria in plaque produce acids after you eat or drink. These acids can destroy tooth enamel and cause cavities and gingivitis (gum disease). Plaque can also develop under the gums on tooth roots and break down the bones that support teeth.
What are 4 steps of forming a dental biofilm?
Biofilm formation is commonly considered to occur in four main stages: (1) bacterial attachment to a surface, (2) microcolony formation, (3) biofilm maturation and (4) detachment (also termed dispersal) of bacteria which may then colonize new areas [2].
What is the primary composition of plaque?
Components of plaque Approximately 80–90% of the weight of plaque is water. While 70% of the dry weight is bacteria, the remaining 30% consists of polysaccharides and glycoproteins.
Which of the following is an early colonizer initiating dental plaque formation?
The initial colonizers of the teeth are streptococci, which proliferate and in turn become colonized by other bacteria present in saliva, such as various Actinomyces species and Veillonella.
What bacteria causes plaque?
Dental plaque contains bacteria that are both acidogenic and aciduric. Although many bacterial subspecies have been shown to be associated with caries, Streptococcus mutans is still believed to be the most important bacterium in the initiation and progress of this disease in combination with lactobacilli.
How quickly does plaque form on teeth?
For each deposit, millions of bacteria congregate, feeding on the simple sugars leftover from your meals. Generally, this plaque starts building on the teeth between four and 12 hours after brushing and tends to collect between the teeth and along the gum line.
When does plaque become calculus?
Plaque can harden into calculus in as little as four to eight hours. The average length of time for mineralization, however, is 10 to 12 days. Calcification times can vary from person to person, depending on their salivary pH and the amount of calcium and other substances in their saliva.
What is tartar vs plaque?
Tartar is what accumulates on your teeth when plaque is not removed. If plaque is left on your teeth for too long, it will harden into tartar and is much more difficult to remove. In fact, tartar can only be removed by a dental professional–you can't get rid of it with regular brushing and flossing.
What is dental plaque?
What’s the Dental plaque ? Dental Plaque is an adherent intercellular matrix consisting primarily of proliferating microorganisms, along with a scattering of epithelial cells, leukocytes and macrophages. 3.
What color is supragingival plaque?
Small amounts of plaque can be visualized by using disclosing agents. The color varies from gray to yellowish-grey to yellow. 12. Disclosing Agents.
What are the bacteria in dental plaque?
Other than bacteria, mycoplasma, fungi, protozoa and viruses may be present. The material among the bacteria in dental plaque is termed as intermicrobial/ cellular matrix. It contains organic and inorganic portions.
Is dental plaque a bacterial community?
Dental plaque Structure Dental plaque is now considered to be a complex and dynamic microbial community , It contains areas of high and low bacterial biomass interlaced with Aqueous channels of bact. Colony. 9.
How long does it take for a plaque to mature?
In the mature plaque (after about 7 days) the percentage of cocci in the plaque decreases rapidly and filaments and rods constitute about 50% of organisms in plaque.
When was dental plaque first observed?
Dental plaque was first observed by van Leeuwenhoek in the 17th century and was associated with the common dental diseases. The proposed hypothesis at that time was that dental infections were caused by an overgrowth of all of the microorganisms in dental plaque.
How long does it take for gingivitis to show?
Within 5 days, plaque is easily visible and clinical signs of gingival inflammation can be observed in localized areas. In 2 to 3 weeks, generalized gingivitis becomes apparent. 5,6 Prevention of gingivitis relies on supragingival plaque removal at appropriate, regular intervals to return the gingiva to a healthy state.
What is dental plaque?
Dental plaque is a complex biofilm attached to teeth. The first stage in development of this oral biofilm is the acquired pellicle, which forms immediately on exposure of a clean tooth surface to saliva. The acquired pellicle allows adhesion of naturally occurring oral bacteria that produce exopolysaccharides to enhance further accumulation ...
What is plaque made of?
Dental plaque is a colourless or whitish substance that builds up on teeth and gums, particularly at the gum margin ( Figure C.4.2 ). It is a biofilm made up of billions of bacteria, the majority of which are only found in the oral cavity [ 41 ]. These grow in a mass of soluble and insoluble carbohydrates synthesised by the bacteria, called the plaque matrix [ 42] and if oral hygiene is neglected or discontinued, plaque growth reaches its maximum extent within 4 days [ 43 ].
What is the term for the accumulation of plaque on the surface of the teeth?
Periodontitis. Dental plaque is a substance that consists of bacteria enmeshed in a biofilm that covers the surface of the teeth. Accumulation of dental plaque can lead to gingivitis (inflammation of the gums and soft tissues in the oral cavity) and also periodontitis.
What is the plaque on the edge of the gum?
Dental plaque found on the edge of gingiva gives rise to gingivitis and consequent degeneration of deep tooth supporting tissues, i.e., gum, periodontal ligaments, alveolar bone, and dental cementum (Goyal et al., 2014).
Where does plaque rupture occur?
Plaque rupture occurs where the cap is thinnest and most infiltrated by foam cells (macrophages). In eccentric plaques, the weakest spot is often the cap margin or shoulder region, 86 and only extremely thin fibrous caps are at risk of rupturing.
What is plaque burden?
To characterize the severity and prognosis of plaques, several terms are used. Plaque burden denotes the extent of disease, whereas plaque activity is an ambiguous term, which may refer to one of several processes that characterize progression.
What is atherosclerosis in the heart?
Atherosclerosis is a multifocal disease that attacks reproducible regions of the arterial tree. Sites with low or oscillatory endothelial shear stress, located near branch points and along inner curvatures, are most susceptible, 20 and the abdominal aorta, coronary arteries, iliofemoral arteries, and carotid bifurcations are typically the most affected. Before development of atherosclerosis, these predilection sites are characterized by changes in endothelial turnover and gene expression, 20 presence of subendothelial dendritic cells, 21 and, in humans, by the presence of adaptive intimal thickening ( Figure 1A ). 15, 22 Adaptive intimal thickenings develop spontaneously after birth and may grow to be as thick as the underlying media. 15 They may provide a soil for initial lesion development, 22 and the rate of progression remains higher here than at other arterial sites. However, with time, the disease spreads to adjacent intima, 23 and in elderly patients dying from MI, most of the epicardial coronary arteries are affected by plaques. 24
How do LDLs cause atherosclerosis?
LDLs cause atherosclerosis by accumulating in the arterial intima where they may be modified by oxidation and aggregation. 26 The modified LDLs, and oxidized lipid moieties deriving from them, in turn act as chronic stimulators of the innate and adaptive immune response. They induce endothelial cells and SMCs to express adhesion molecules (eg, vascular cell adhesion molecule–1 and intercellular adhesion molecule–1), chemoattractants (eg, monocyte chemoattractant protein-1), and growth factors (eg, macrophage colony-stimulating factor and granulocyte-macrophage colony-stimulating factor) that interact with receptors on monocytes and stimulate their homing, migration, and differentiation into macrophages and dendritic cells. 27, 28
Can plaque rupture cause angina pectoris?
Mechanisms of Plaque Rupture, Erosion, and Thrombosis. Atherosclerosis alone may obstruct coronary blood flow and cause stable angina pectoris, but this is rarely fatal in the absence of scarring of the myocardium, which can elicit an arrhythmia presenting as sudden cardiac death.
Is thrombus without rupture a morphological feature?
The surface endothelium under the thrombus is usually absent, but no distinct morphological features of the underlying plaque have been identified.
Where is plaque found?
It is commonly found between the teeth, on the front of teeth, behind teeth, on chewing surfaces, along the gumline, (supragingival) or below the gumline cervical margins (subgingival). Dental plaque is also known as microbial plaque, oral biofilm, dental biofilm, dental plaque biofilm or bacterial plaque biofilm.
What is plaque in dentistry?
Dental plaque is a biofilm that attaches to tooth surfaces, restorations and prosthetic appliances (including dentures and bridges) if left undisturbed. Understanding the formation, composition and characteristics of plaque helps in its control. An acquired pellicle is a layer of saliva that is composed of mainly glycoproteins ...
What is dental plaque?
Dental plaque. From Wikipedia, the free encyclopedia. Jump to navigation Jump to search. biofilm of microorganisms that grows on teeth. Dental plaque is a biofilm of microorganisms (mostly bacteria, but also fungi) that grows on surfaces within the mouth. It is a sticky colorless deposit at first, but when it forms tartar, ...
Where does supragingival biofilm form?
It commonly forms in between the teeth, in the pits and grooves of the teeth and along the gums. It is made up of mostly aerobic bacteria, meaning these bacteria need oxygen to survive.
How to tell if a tooth has biofilm?
Visual or tactile detection . Dental biofilm begins to form on the tooth only minutes after brushing. It can be difficult to see dental plaque on the hard tissue surfaces, however it can be felt as a rough surface. It is often felt as a thick, fur-like deposit that may present as a yellow, tan or brown stain.
Why is plaque important in periodontitis?
Plaque accumulation is vital in the progression of periodontitis as the bacteria in plaque release enzymes which attack the bone and cause it to break down , and at the same time osteoclasts in the bone break down the bone as a way to prevent further infection.
Why is it important to be aware of plaque?
It is important to be aware that everyone has dental plaque, however, the severity of the build-up and the consequences of not removing the plaque can vary.