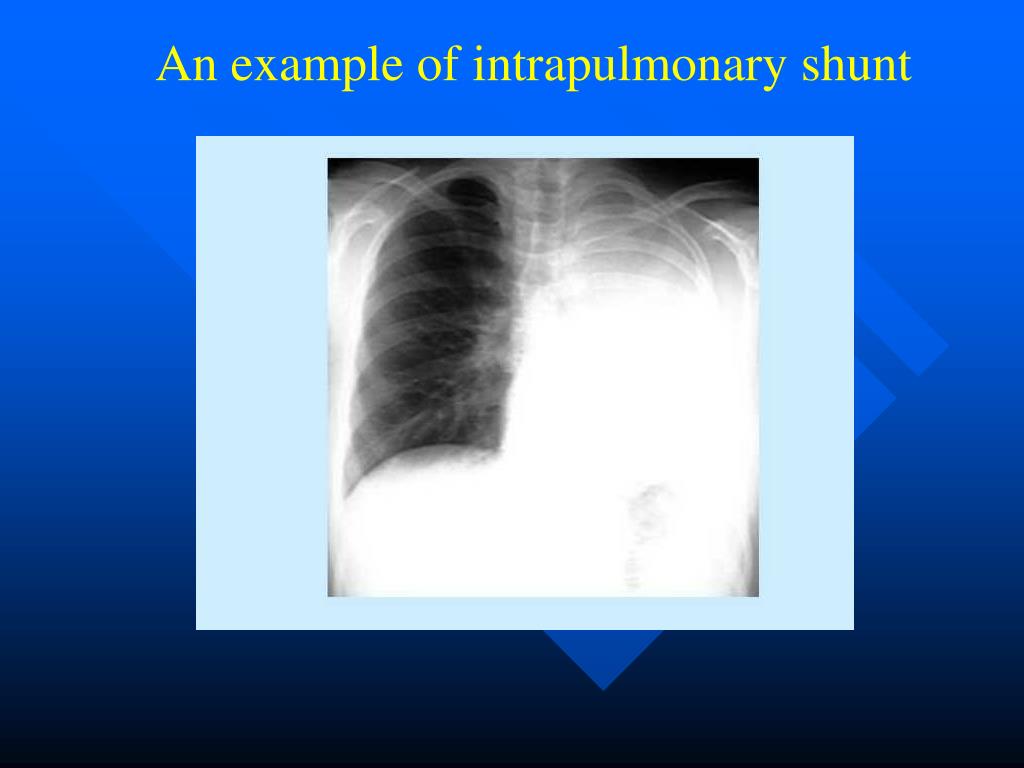
Intrapulmonary shunting is most commonly demonstrated by contrast TTE when bubbles from agitated saline are visualized in the left atrium within 3–6 beats after being noted in the right side of the heart. Bubbles are not normally observed in the absence of vascular dilatation because lung capillaries act as filters.
Full Answer
What is intrapulmonary shunt?
Intrapulmonary shunting is the primary cause of hypoxemia (lack of blood oxygen) in pulmonary edema. Including other ailments like pneumonia that affect the lungs ( 5) So, what causes shunting in the lungs?
What is the pathophysiology of shunting?
II Intrapulmonary Shunting A A pathophysiologic process in which blood enters the left side of the heart without having been oxygenated by the lungs. The mixing of venous blood with oxygenated blood from the pulmonary capillaries to form arterial blood.
What is the relationship between shunt fraction and pulmonary contusion?
In pathological conditions such as pulmonary contusion, the shunt fraction is significantly greater and even breathing 100% oxygen does not fully oxygenate the blood.
Is intrapulmonary shunt a potential facilitator of ischemic stroke?
Intrapulmonary shunt is a potentially unrecognized cause of ischemic stroke and transient ischemic attack These results suggest that intrapulmonary shunt is a potentially unrecognized facilitator of CVA and TIA, especially in patients with cryptogenic CVA and TIA.

What does intrapulmonary shunting mean?
As stated previously, the intrapulmonary shunt is defined as that portion of the cardiac output entering the left side of the heart without undergoing perfect gas exchange with completely functional alveoli.
What causes an intrapulmonary shunt?
Causes of shunt include pneumonia, pulmonary edema, acute respiratory distress syndrome (ARDS), alveolar collapse, and pulmonary arteriovenous communication.
How is pulmonary shunting diagnosed?
Diagnosis requires the presence of liver disease, inadequate oxygenation, and confirmation of intrapulmonary shunting, generally by contrast-enhanced echocardiography. Occasionally, it can be difficult to decipher between intracardiac and intrapulmonary shunting.
What is the definition of absolute shunt?
Absolute shunt: is defined as hypoxemia resulting from all anatomic shunts and alveoli that have collapsed or consolidated to a level where there is zero ventilation occurring.
Is PE shunt or dead space?
Pulmonary embolism (PE) is an example of increased dead space resulted in decreasing perfusion relative to ventilation.
How is intrapulmonary shunting treated?
How is intrapulmonary shunting treated? Treating an intrapulmonary shunt will vary from person to person. Some patients need oxygen therapy, while others will rely on mechanical ventilation. Long-term oxygen therapy can be a viable opportunity for a more complicated health issue.
What is a right to left intrapulmonary shunt?
A shunt is an abnormal communication between the right and left sides of the heart or between the systemic and pulmonary vessels, allowing blood to flow directly from one circulatory system to the other. A right-to-left shunt allows deoxygenated systemic venous blood to bypass the lungs and return to the body.
How do you calculate intrapulmonary shunt?
The pulmonary shunt fraction was calculated using the established classical equation: Qs/Qt = (Cc,O2 - Ca,O2)/(Cc,O2 - Cv,O2), in which Qs/Qt is the RLS as a fraction of the cardiac output, Cc,O2 is the oxygen content at the end of the pulmonary capillary, Ca,O2 is the oxygen content of arterial blood and Cv,O2 is the ...
What is the difference between shunt and VQ mismatch?
V/Q mismatch is common and often effects our patient's ventilation and oxygenation. There are 2 types of mismatch: dead space and shunt. Shunt is perfusion of poorly ventilated alveoli. Physiologic dead space is ventilation of poor perfused alveoli.
What are the two types of V Q mismatch?
The two major types of V/Q mismatch that result in dead space include: anatomical dead space (caused by an anatomical issue) and physiological dead space (caused by a functional issue with the lung or arteries ).
Why does shunting occur?
If the right ventricular pressure exceeds left ventricular pressure, then blood can flow down the new pressure gradient, and a right to left shunt occurs.
What is true shunt?
"True" intrapulmonary shunt, in contrast, is the volume of venous blood which actually bypassed the aerated alveoli, and returned deoxygenated blood to the left heart via the pulmonary circulation.
Why does shunting occur?
If the right ventricular pressure exceeds left ventricular pressure, then blood can flow down the new pressure gradient, and a right to left shunt occurs.
Does PE cause shunt?
In acute PE, intracardiac shunting usually occurs through a patent foramen ovale; right atrial pressure exceeds left atrial pressure, even if both pressures are normal.
What causes blood shunting?
In shunting, venous blood enters the bloodstream without passing through functioning lung tissue. Shunting of blood may result from abnormal vascular (blood vessel) communications or from blood flowing through unventilated portions of the lung (e.g., alveoli filled with fluid or inflammatory material).
What is shunting in the heart?
A shunt is a passage by which blood moves from one area (blood vessel or heart chamber) to another in a pattern that isn't normal. A cardiac shunt is a congenital heart defect, meaning it's present at birth. Cardiac shunt symptoms can vary widely.
Why is intrapulmonary shunt important?
Intrapulmonary shunt accounts for much of the Pao 2 −Pao 2 in atelectasis, pneumonia, and ARDS in children and adults, mainly because of continued perfusion of unventilated alveoli. In pneumococcal pneumonia, this continued perfusion is due to impairment of hypoxic pulmonary vasoconstriction, possibly by bacterial products or by immune mediators. 73,74 The cause of venous admixture in cystic fibrosis varies from patient to patient. In some patients, intrapulmonary shunt accounts for most of the Pao 2 −Pao 2 difference, and the degree of shunt may increase with exercise. 75
What chapter is pulmonary shunt?
For a more detailed discussion of pulmonary shunts, see Chapter 61 which discusses pulmonary arteriovenous malformations and other pulmonary vascular abnormalities.
What causes pulmonary arterial oxygenation to be impaired?
Intrapulmonary arterial oxygenation can be impaired by alveolar ventilation-perfusion imbalance, increased intrapulmonary shunt, and diffusion defects, 30 and all of these mechanisms may be present in HPS. 3,31-39 However, the response to the administration of 100% oxygen is typically preserved; shunts appear to be functional rather than anatomical. Diffusion limitation and ventilation-perfusion mismatch appear to be predominant factors. The common finding of a low diffusing capacity of lung for carbon monoxide (DLCO) supports diffusion impairment. This most likely results from the increased distance between the alveoli and the red blood cells in the central stream of the dilated pulmonary capillary ( Fig. 39-3 ). The hyperdynamic circulation (high rate of blood flow) found in cirrhotic patients decreases the exposure time of the red blood cell to the alveolus, further worsening the diffusion impairment.
How to improve shunt fraction?
Improvement of the shunt fraction can be accomplished by decreasing blood flow or supplying O 2 to the nondependent lung. Hypoxic pulmonary vasoconstriction is a powerful reflex that increases the PVR of the hypoxic lung and the atelectatic lung, diverting blood to the well-oxygenated areas of lung.
What are the right to left shunts?
These shunt vessels include bronchial veins, mediastinal-to-pulmonary veins, and thebesian vessels (left ventricular muscle to left ventricular cavity). In some patients, intracardiac shunts, pulmonary arteriovenous malformations, or perfusion of nonventilated alveoli produce pulmonary shunts. Most shunts in patients with pulmonary disorders involve perfusion of nonventilated alveoli. For clinical purposes the amount of right-to-left shunt may be estimated from the fall in arterial P o2 below the expected value of 673 mm Hg, as long as the P o2 is sufficient to saturate hemoglobin (i.e., more than 200 mm Hg). For every 2% shunt, P o2 decreases 35 mm Hg.
What is the V/Q ratio of an intrapulmonary shunt?
Intrapulmonary shunt involves blood flow through areas of lung with excessive perfusion for the amount of ventilation (low V/Q ratio) or through areas with no ventilation at all (V/Q = 0).
What causes hypoxia during weaning from PPV?
Hypoxia during weaning from PPV usually results from ventilation/perfusion mismatch (intrapulmonary shunt). As PEEP and peak airway pressures are reduced, atelectasis may develop with resultant loss of lung volume and increased intrapulmonary shunt. Impaired gas exchange from right-to-left intrapulmonary shunting can be identified by the presence of an elevated alveolar-arterial oxygen tension gradient, P (A−a) O 2. When hypoxemia is encountered, an increased FiO 2 may be necessary. If the hypoxemia persists, the cause of the hypoxemia must be investigated and corrected. If loss of lung volume is the cause of the ventilation/perfusion mismatch, an increase in PEEP may be necessary and weaning suspended until improvements in pulmonary compliance are seen.
What is intrapulmonary shunt?
Intrapulmonary shunt is a potentially unrecognized cause of ischemic stroke and transient ischemic attack
Is intrapulmonary shunt a facilitator?
These results suggest that intrapulmonary shunt is a potentially unrecognized facilitator of CVA and TIA, especially in patients with cryptogenic CVA and TIA. Future studies assessing the prognostic significance of intrapulmonary shunt on cerebral vascular event recurrence rates in patients after in …
What is the process of shunting blood?
Capillary shunting is blood that passes through capillaries of unventilated alveoli or deoxygenated blood flowing directly from pulmonary arterioles to nearby pulmonary veins through anastomoses, bypassing the alveolar capillaries . In addition, some of the smallest cardiac veins drain directly into the left ventricle of the human heart.
What causes a shunt in the lung?
Pulmonary shunting causes the blood supply leaving a shunted area of the lung to have lower levels of oxygen and higher levels of carbon dioxide (i.e., the normal gas exchange does not occur). A pulmonary shunt occurs as a result of blood flowing right-to-left through cardiac openings or in pulmonary arteriovenous malformations.
What is the ratio of ventilation to perfusion in a pulmonary shunt?
While in a pulmonary shunt, the ventilation/perfusion ratio is zero, lung units with a V/Q (where V = ventilation, and Q = perfusion) ratio of less than 0.005 are indistinguishable from shunt from a gas exchange perspective.
What would happen if every alveolus was ventilated?
If every alveolus was perfectly ventilated and all blood from the right ventricle were to pass through fully functional pulmonary capillaries, and there was unimpeded diffusion across the alveolar and capillary membrane, there would be a theoretical maximum blood gas exchange, and the alveolar PO 2 and arterial PO 2 would be the same. The formula for shunt describes deviation from this ideal.
Why is 100% inspired oxygen unable to overcome hypoxia?
Because shunt represents areas where gas exchange does not occur, 100% inspired oxygen is unable to overcome the hypoxia caused by shunting .
What causes vasoconstriction in the alveoli?
For example, when alveoli fill with fluid, they are unable to participate in gas exchange with blood , causing local or regional hypoxia, thus triggering vasoconstriction. This vasoconstriction is triggered by a smooth muscle reflex, as a consequence of the low oxygen concentration itself.
Is a lung perfused?
A normal lung is imperfectly ventilated and perfused, and a small degree of intrapulmonary shunting is normal. Anatomical shunting occurs when blood supply to the lungs via the pulmonary arteries is returned via the pulmonary veins without passing through the pulmonary capillaries, thereby bypassing alveolar gas exchange.