Full Answer
How does bronchial smooth muscle modulate resistance to airflow?
Many individuals whose airways display pathologically excessive resistance to airflow may breathe at higher lung volumes to enhance this radial traction. Bronchial smooth muscle surrounding bronchi and bronchioles can significantly modulate the diameter and thus resistance of these airways.
What is airway resistance in respiratory system?
Airway Resistance. Airway resistance is the resistance to the flow of air through the respiratory tract during inhalation and expiration. The level of resistance depends on many things, particularly the diameter of the airway and whether flow is laminar or turbulent.
Why do the lungs have the highest resistance to air flow?
This reduces the total resistance to air flow. So, due to the vast number of bronchioles that are present within the lungs running in parallel, the highest total resistance is actually in the trachea and larger bronchi. The autonomic nervous system usually determines airway diameter.
Why is the total resistance to air flow in the trachea?
However, the branching of the airways means that there are many more of the smaller airways in parallel, reducing the total resistance to air flow. So due to the vast number of bronchioles that are present within the lungs running in parallel, the highest total resistance is actually in the trachea and larger bronchi.
What is the role of the bronchioles in the respiratory system?
The bronchi carry air into your lungs. At the end of the bronchi, the bronchioles carry air to small sacs in your lungs called alveoli. The alveoli perform your body's gas exchange.
What part of the airway affects resistance?
One of the most important factors influencing airway resistance is the diameter of the airway. In general, the opposition of flow can be described as the pressure divided by the rate of flow (R = change in P/V).
What is primarily responsible for airway resistance?
Airway resistance is determined by lung volume, bronchial smooth muscle tone, and dynamic airway compression. At lower lung volumes, radial traction supporting the bronchi is lost and airway caliber is reduced. Bronchial muscle contraction narrows airways and increases resistance.
How can innervation of the bronchioles effect airway resistance?
Sympathetic innervation causes relaxation of bronchial smooth muscle via beta-2 receptors, which causes an increase in airway diameter to allow more airflow. This is useful in situations such as exercise, when sympathetic stimulation triggers airway muscle relaxation to allow more air into the lungs.
When bronchioles constrict what happens to resistance?
63 Cards in this SetBoyle's LawThe relationship between pressure and volume ⬆️vol= ⬇️pressure (inspiration) ⬇️vol= ⬆️pressure (exhalation)Intrapulmonary pressure is most negative duringInspirationWhen the bronchiole constricts, what will happen to resistance?⬆️goes up60 more rows
What role does Bronchiole diameter play in determining air flow?
Larger airway diameter results in greater turbulence for the same relative flow velocity (e.g., between a particle and air) . Therefore, flow may be turbulent in the large airways of humans, whereas for an identical flow velocity, it would be laminar in the smaller experimental animal .
Where in the bronchial tree is resistance to flow the highest?
midsize bronchiolesFigure 5.4: Airway resistance down the bronchial tree. The highest point of resistance is actually the midsize bronchioles.
Where does the most airway resistance in our respiratory system occur?
In healthy lungs, the overall resistance in the conducting zone is high. The radius of an individual bronchiole is low, but the overall cross-sectional area of all the bronchioles is quite high. During quiet breathing, the difference between Palv and Patm is less than 2 mmHg.
Where is the major site of airway resistance explain the reason why?
An individual small airway has much greater resistance than a large airway, however there are many more small airways than large ones. Therefore, resistance is greatest at the bronchi of intermediate size, in between the fourth and eighth bifurcation.
What determines airway resistance in the respiratory passageways?
What primarily determines airway resistance in the respiratory passageways? Alveolar surface tension determines lung compliance.
Which factors can increase airway resistance quizlet?
Airway resistance will increase as we move towards lower lung volumes.... strength of chest and abdominal muscles. airway resistance. lung size and. elastic properties.
Which of the following will decrease airway resistance?
Stimulation by sympathetic fibers Sympathetic stimulation of the airways results in a relaxation of airways, decreasing resistance.
What determines airway resistance in the respiratory passageways?
What primarily determines airway resistance in the respiratory passageways? Alveolar surface tension determines lung compliance.
Where does the most airway resistance in our respiratory system occur?
In healthy lungs, the overall resistance in the conducting zone is high. The radius of an individual bronchiole is low, but the overall cross-sectional area of all the bronchioles is quite high. During quiet breathing, the difference between Palv and Patm is less than 2 mmHg.
Where in his airway The resistance is highest and why?
Resistance is highest in the medium-sized conducting airways and lower in the large airways because of their large diameters. As the air travels into the medium-sized bronchi, it faces greater resistance due to the drop in diameter of the airway.
Which factors can increase airway resistance quizlet?
Airway resistance will increase as we move towards lower lung volumes.... strength of chest and abdominal muscles. airway resistance. lung size and. elastic properties.
How does airway resistance change?
Airway resistance also changes between inspiration and expiration. The majority of airways within the lung parenchyma are tethered by alveolar attachments that transmit an outward force on these airways, which increases as the lungs expand. This increasing outward force increases airway radius, thus decreasing airway resistance. On expiration, this outward tethering force diminishes, and inward elastic recoil forces increase causing a decrease in airway radius, which leads to increased airway resistance. [1]
What is the most important factor in airway resistance?
Given this equation, it is clear that the radius is the most important factor in airway resistance and that small changes in radius can lead to significant changes in airway resistance. For example, if the radius of the tube doubles, the resistance decreases by a factor of 16.
How does heliox work?
Heliox is often an adjunctive therapy alongside albuterol for reducing airway resistance. With severe airway narrowing, gas velocity increases, and airflow becomes turbulent. This turbulent airflow increases airway resistance. Helium is seven-times less dense than air, and when mixed with oxygen to form heliox, the lower density causes the turbulent airflow to revert to a state of laminar flow, decreasing airway resistance. This return to laminar flow and reduced resistance helps albuterol get to the distal airways where it can act on distant beta-2 receptors and also helps to maintain ventilation to the distal airways, preventing progression to respiratory failure.
How to measure airway resistance?
Whole-body plethysmography is the most common method for measuring airway resistance. A plethysmograph is an air-tight chamber that the participant sits inside, which contains a tube that the patient puts in their mouth. There are two transducers within the plethysmograph: one located in the chamber that measures chamber pressure, and one inside of the tube that measures mouth pressure. There is also a flowmeter in the tube that measures the flow rate. During the test, the patient is asked to breathe normally while the tube is left open. When the participant breaths into the open tube, mouth pressure, and flow rate are recorded. A shutter then occludes the tube, and the participant is asked to try to breathe normally. With the participant attempting to breathe against the closed tube, there is no airflow, and mouth pressure approximates alveolar pressure.[7] After obtaining the values for mouth pressure (kPa), alveoli pressure (kPa), and flow rate (L/s), airway resistance (kPa s L) can be calculated using the equation below.
What is the role of the lungs in the body?
The lungs are an intricately designed organ that acts as the body's center for gas exchange, inhaling and exhaling approximately 7 to 8 mL of air per minute while exchanging oxygen for carbon dioxide. Airway resistance is an essential parameter of lung function and results from the frictional forces of the airways, which oppose airflow. At physiologic levels, airway resistance in the trachea is responsible for turbulent airflow, while airway resistance in the bronchi and bronchioles allows for more laminar airflow, in which air smoothly flows to the distal segments of the lungs. When airway resistance is elevated, as seen with certain pulmonary diseases, air can become trapped in the lungs, limiting gas exchange and possibly causing respiratory failure in severe cases.[1]
Why does asthma cause chest tightness?
The increased airway resistance associated with asthma is responsible for many of the signs and symptoms a patient will experience during an asthma exacerbation, including wheezing, dyspnea, chest tightness, and air trapping. Air trapping within the distal segments of the lungs is due to an inability to produce enough expiratory pressure to overcome the airway resistance of the more proximal bronchi and bronchioles. Since this airway resistance cannot be overcome, the air gets trapped in the distal segments of the lungs. [9][10]
Which bronchi have the smallest radius?
The medium-sized bronchi collectively have the smallest radius. If we use the principle outlined above, it makes sense that since the medium-sized bronchi collectively have the smallest radius, then it would also be the site of greatest airway resistance. Using this same principle, we can also conclude that the terminal bronchioles have the lowest resistance since collectively it has the largest radius. [5]
What is airway resistance?
bookmarks Recommended reading. Airway resistance refers to degree of resistance to the flow of air through the respiratory tract during inspiration and expiration. The degree of resistance depends on many things, particularly the diameter of the airway and whether flow is laminar or turbulent. Alveolar expansion is also dependent on surfactant, so ...
Which airways have the highest resistance to air flow?
Therefore, smaller airways such as bronchioles and alveolar ducts all individually have much higher flow resistance than larger airways like the trachea. However, the branching of the airways means that there are many more of the smaller airways in parallel, reducing the total resistance to air flow. So due to the vast number of bronchioles that are present within the lungs running in parallel, the highest total resistance is actually in the trachea and larger bronchi.
Why is it harder to expand the alveoli?
Therefore, further expansion of the alveoli is resisted. This explains why once the lungs are mostly filled , it is harder to expand the lungs further to allow the entry of additional air.
How does sympathetic innervation affect airway diameter?
Sympathetic innervation causes relaxation of bronchial smooth muscle via beta-2 receptors, which increases diameter to allow more airflow. This is useful in situations such as exercise, as sympathetic nerve stimulation triggers airway muscle relaxation, increasing the diameter to allow more air into the lungs. This increases the rate of gas exchange at alveolar level compared to normal breathing.
How does resistance differ between inspiration and expiration?
On inspiration, the positive pressure within the alveoli and small airways causes their diameter to increase, and therefore resistance to decrease. The opposite is true for expiration, as airways narrow due to the reduced pressure, thus increasing resistance.
What is the degree of resistance to the flow of air through the respiratory tract during inspiration and expiration?
Airway Resistance. Airway resistance refers to degree of resistance to the flow of air through the respiratory tract during inspiration and expiration. The degree of resistance depends on many things, particularly the diameter of the airway and whether flow is laminar or turbulent.
Why are my airways narrowed?
In an asthma exacerbation , the already narrowed airways (due to mucosal inflammation and smooth muscle hypertrophy) are further constricted due to increased smooth muscle tone. This can decrease the diameter of the airways significantly, causing resistance to airflow to become very high.
Where does resistance reside in the vascular system?
1. In the vascular system, most resistance resides in small arterioles.
Which type of airflow tends to be turbulent?
1. Airflow in trachea and large ariways tends to be turbulent (eddies), whereas flow in smaller airways (bronchioles) tends to be laminar.
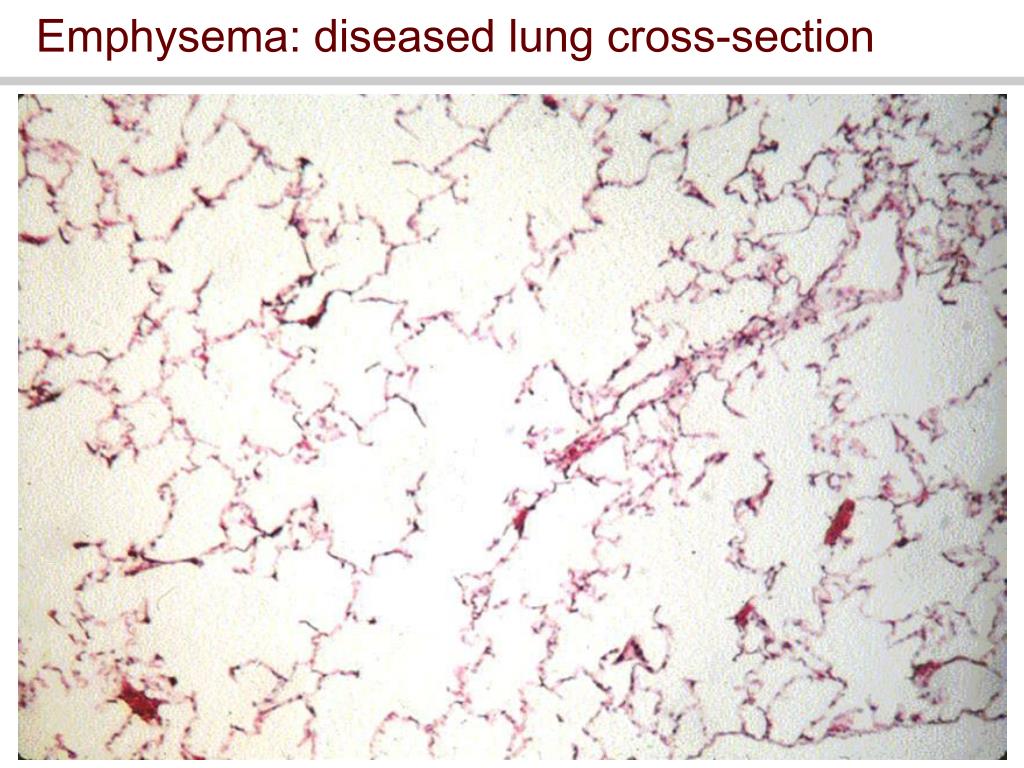
Why are my lungs flabby?
1. Flabby lungs due to destruction of elastic elements of the lung alveoli, intersitium, and bronchioles by proteases
Why is active exhalation inefficient?
2. Active exhalation is also inefficient due to airway compression
What is the function of ACh in the parasympathetic nerve?
Release of ACh by parasympathetic nerve fiebrs activate muscarinic receptors of smooth muscles and submucosal glands, triggering contraction of airways and increased mucus secretion
Why are small alternating Palv gradients sufficient for air motion?
Small alternating Palv (-1 to +1 mmHg) gradients are sufficient for air motion because normally R is very low. Airflow. 1. Airflow in trachea and large ariways tends to be turbulent (eddies), whereas flow in smaller airways (bronchioles) tends to be laminar.
What is the resistance to laminar flow?
1. Resistance to laminar flow is inversely proportional to the fourth power of radius (r)
Which muscle provides the autonomic nerves to the airways?
The upper thoracic sympathetic ganglia, and the dorsal motor nucleus of the vagus provide the autonomic nerves to the airways. Airways Smooth Muscle.
What is the autonomic innervation of the respiratory tract?
Autonomic Innervation of the Respiratory TractTarget Tissues in the Respiratory TractEffects of ANS in the Respiratory TractAutonomic Nerves and Asthma
How does the cilia beat?
The cilia beat in such as way as to move the mucus towards the pharynx, thus removing it from the bronchial tree; it is normally removed from the pharynx by coughing. Failure of mucociliary clearance is associated with (a) thick mucus, and (b) failure of ciliary movement. Effects of autonomic nerves Top.
Why do beta-2 agonists increase the force of expiratory volume?
As a consequence they allow air to move in and out of the lungs more easily because of the dilated airways. Beta-2 agonists therefore increase the Forced Expiratory Volume and the ratio of FEV1.0 / FVC . Muscarinic antagonists are also commonly used to counter the contractile effects of the parasympathetic nerves.
What muscle is affected by asthma?
The tone of bronchial muscle influences airway resistance, which is also affected by the state of the mucosa and activity of the glands in patients with asthma and bronchitis.
Does smoke cause cough reflex?
Excitation of the irritant receptors, e.g. by smoke, causes reflex activation of the parasympathetic, resulting in bronchoconstriction and mucus secretion, and possibly an increase in mucociliary clearance; they also induce the cough reflex.
Which system is responsible for bronchodilation?
Bronchodilation is mediated by neurons of the Sympathetic Nervous System which activate beta2 receptors on bronchial smooth muscle cells. In this way, the autonomic nervous system can exert powerful effects on airflow and can be used to pharmacologically intervene in scenarios of pathological bronchoconstriction.
What are the factors that influence airway resistance?
As discussed below, a number of factors can influence airway resistance and can play important roles in certain pathologies. Lung Volume. Small bronchi and bronchioles in the lung have little to no supporting cartilage and depend on radial stretching by the elastic lung parenhcyma to maintain their patency.
What is the role of the length of a tube in determining the resistance to flow?
In addition to the diameter, the length of a tube is an important factor in determining its resistance to flow (See: Resistance ). As air passes through an airway, the progressive resistance it encounters gradually reduces the pressure gradient between the distally moving air and atmospheric pressure. Consequently, during expiration, the highest intra-airway pressures are found near the alveoli and these values gradually decline as air arrives near the mouth and nose. As described previously, small airways are not supported by any cartilage and depend on the elastic recoil of the lung to remain patent.
How does the pressure of air in the airways change during forced expiration?
In normal quiet expiration, the intra-airway pressure never declines below that of the intrapleural pressure and thus airways remain patent throughout their length. However, during forced expiration the intrapleural pressure in a healthy lung can sufficiently rise above the intra-airway pressure to overcome the natural radial traction maintaining airway patency. This yields dynamic airway collapse and limits airflow. In certain pathologies, such as emphysema, the radial traction of the lung maintaining airway patency can become so tenuous that even normal quiet expiration can yield dynamic airway collapse. These individuals can display airflow limitation even at rest.
What is resistance to airflow?
In many ways, resistance to airflow follows the same principles as resistance to blood flow (See: Resistance ). The most important principle to consider is that the resistance of a tube, such as a pulmonary airway, is most influenced by the airway's diameter. Reduction of the airway diameter drastically increases its resistance, ...
How does air flow between two points in a closed space?
Ultimately, airflow between two points in a closed space is actuated by differences in the air pressure between those two points . However, the rate at which this movement occurs is dependent on the relative resistance of the environment to air movement. In many ways, resistance to airflow follows the same principles as resistance to blood flow (See: Resistance ). The most important principle to consider is that the resistance of a tube, such as a pulmonary airway, is most influenced by the airway's diameter. Reduction of the airway diameter drastically increases its resistance, whereas dilation of the airway can significantly reduce its resistance. As discussed below, a number of factors can influence airway resistance and can play important roles in certain pathologies.
Can intrapleural pressures collapse the airway?
However, even small external pressures exerted by the intrapleural space can collapse the airway. During normal expiration the pressures within the intrapleural space are negative and thus aid in maintaining airway patency; however, during forced expirations powerful contraction of the chest wall can give the intrapleural space substantial positive pressures, above that of atmospheric pressure. At a certain distance within the airway, the declining intra-airway pressure will dip far enough below the positive intrapleural pressure during forced expiration that the elastic recoil of the lung maintaining airway patency will be overcome. In normal individuals, the elastic recoil of the lung is strong enough that this threshold segment is reached at a point where cartilage exists within the airways, thus preventing airway collapse.
