Treatment
- Anticoagulants. Anticoagulants (commonly referred to as “blood thinners”) are the medications most commonly used to treat DVT or PE.
- Thrombolytics. Thrombolytics (commonly referred to as “clot busters”) work by dissolving the clot. ...
- Inferior vena cava filter. ...
Are hospitals delivering appropriate VTE prevention?
Study trends in both the use of risk-appropriate methods in hospitals to prevent VTE (known as prophylaxis) and the occurrence of HA-VTE and related health problems. HA-VTE is the subject of a number of patient safety and public health programs developed and promoted by federal agencies.
How is mechanical prophylaxis used in VTE prevention?
- Apixaban ;
- Rivaroxaban ;
- LMWH for at least 5 days followed by either dabigatran etexilate (if estimated creatinine clearance is 30 ml/min or above) or edoxaban ;
- LMWH or heparin (unfractionated), given concurrently with a vitamin K antagonist for at least 5 days or until the INR is at least 2.0 for 2 consecutive readings, followed by ...
How to prevent VTE?
You can:
- Learn strategies for improving performance in blood clot prevention , including risk-stratification, risk-appropriate ordering and nurse education
- Find patient education resources, including a video and handouts in multiple languages
- Watch videos from the VTE Symposium, hosted every year in March
What is the optimal duration of treatment for DVT?
Treatment
- Prevent the clot from getting bigger.
- Prevent the clot from breaking loose and traveling to the lungs.
- Reduce your chances of another DVT.

What medication is used for VTE?
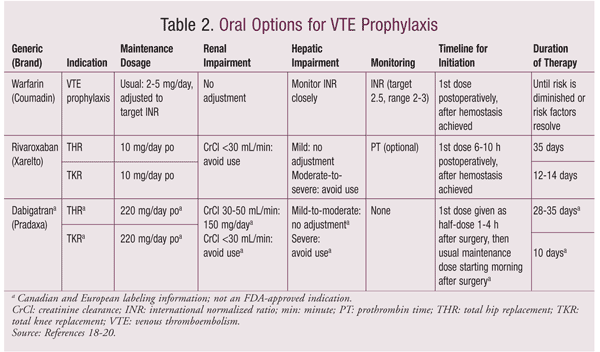
Apixaban, dabigatran, rivaroxaban, edoxaban, and betrixaban are alternatives to warfarin for prophylaxis or treatment of deep venous thrombosis (DVT) and pulmonary embolism (PE). Apixaban, edoxaban, rivaroxaban, and betrixaban inhibit factor Xa, whereas dabigatran is a direct thrombin inhibitor.
How do you reduce VTE?
Preventing DVTGet up and walk around every 1 to 2 hours.Exercise your legs while you're sitting by: Raising and lowering your heels while keeping your toes on the floor. Raising and lowering your toes while keeping your heels on the floor. Tightening and releasing your leg muscles.Wear loose-fitting clothes.
Can VTE be cured?
When a clot like this forms (also known as a thrombus), it can have varied health effects depending on where it occurs. Depending on your general condition, thrombosis may be a singular incident or a more chronic problem. However, the good news is that generally, Thrombosis can be cured.
What is VTE protocol?
A VTE prevention protocol includes a VTE risk assessment, a bleeding risk assessment, and clinical decision support (CDS) on prophylactic choices based on the combination of VTE and bleeding risk factors.
What is the difference between DVT and VTE?
Venous thromboembolism (VTE), also known as blood clots, is a disorder that includes deep vein thrombosis and pulmonary embolism. A deep vein thrombosis (DVT) occurs when a blood clot forms in a deep vein, usually in the lower leg, thigh, or pelvis.
How is VTE diagnosed?
How is it diagnosed? Blood work may be done initially, including a test called D-dimer, which detects clotting activity. For PE: Computed tomography, or CT scan, or CAT scan is most often used. Sometimes ventilation-perfusion lung scan is used.
How do they remove blood clots from legs?
The doctor will make a cut in the area above your blood clot. He or she will open the blood vessel and take out the clot. In some cases, a balloon attached to a thin tube (catheter) will be used in the blood vessel to remove any part of the clot that remains. A stent may be put in the blood vessel to help keep it open.
How long does it take for a blood clot to dissolve with blood thinners?
Blood clots can take weeks to months to dissolve, depending on their size. If your risk of developing another blood clot is low, your doctor may prescribe you 3 months of anticoagulant medication, as recommended by the American Heart Association . If you're at high risk, your treatment may last years or be lifelong.
Do blood clots go away in leg?
Blood clots do go away on their own, as the body naturally breaks down and absorbs the clot over weeks to months. Depending on the location of the blood clot, it can be dangerous and you may need treatment.
What are the 3 proven methods to prevent VTE in the hospital setting?
Methods of DVT prophylaxis include general measures: the use of aspirin, mechanical prevention with graduated compression stockings, and intermittent pneumatic compression devices.
What are VTE quality measures?
A Suggested Ideal Defect-Free VTE Process Quality Measure This process measure should have 3 components: (1) documentation of a standardized VTE risk assessment; (2) prescription of optimal, risk-appropriate VTE prophylaxis; and (3) administration of every dose of risk-appropriate VTE prophylaxis as prescribed.
What is a VTE risk assessment?
The Venous Thromboembolism Risk Assessment Tool is a type of ASSESSMENT TOOL. The Venous Thromboembolism Risk Assessment Tool is used to assess PATIENTS (aged 16 or over) admitted to a Hospital Provider, for the risk of Venous Thromboembolism.
What is a VTE?
How is it treated? VTE includes deep vein thrombosis (DVT), when a blood clot forms in a deep vein, usually in the leg. And it includes pulmonary embolism (PE), when the clot breaks off and travels from the leg up to the lungs.
How long do you have to take a VTE medication?
These medications are used for a number of months. If the VTE occurred after a provoking factor like surgery, trauma, pregnancy, hospital stay, or with use of hormone treatments, this is usually given for a fixed number of months. For patients without these provoking factors treatment can be recommended for longer durations.
What is thrombolytic therapy?
Thrombolytic therapy, which includes drugs such as a tissue plasminogen activator (tPA), — a clot-dissolving enzyme. This can be given through an arm vein, and also by inserting catheters directly into the blood clot in the vein or lung. Surgical procedures may also be used.
How to lower your chances of getting another VTE?
There are also things that everyone can do to lower their chances of a VTE: Get regular exercise. Be at a healthy weight.
How long do you need blood thinners after a VTE?
Even after you recover from a VTE and you're out of the hospital, you'll probably still need treatment with blood thinners for at least 3 months. That's because your chances of having another VTE will be higher for a while. VTE Prevention. There's a lot you and your doctors can do to cut your odds of getting a VTE.
What happens when a DVT breaks loose?
A pulmonary embolism is a life-threatening emergency. It can make it hard to breathe and cause a fast heart rate, chest pain, and dizziness. It can also cause you to become unconscious.
What causes VTE in the body?
VTEs can happen if your blood flow changes or slows down somewhere in your body. Lots of things can cause that, like some diseases, medical treatments, and long airplane flights where your legs are stuck in the same position. Things that raise your chances of having a VTE include: Medical treatments.
What test is done for pulmonary embolism?
A radiologist or someone who’s specially trained has to look at the images to explain what's going on. For a pulmonary embolism, you might also get: Pulse oximetry: This is often the first test. The doctor will put a sensor on the end of your finger that measures the level of oxygen in your blood.
Why do you have higher chances of getting a VTE?
Health conditions. Your VTE risk is higher if you have cancer, lupus or other immune problems, health conditions that make the blood thicker, or you're obese.
Where does VTE develop?
Deep vein thrombosis (DVT). As the name suggests, it develops deep in your veins, usually in the legs. You can get one in your arm, though.
What is a VTE?
Venous thromboembolism (VTE), a term referring to blood clots in the veins, is an underdiagnosed and serious, yet preventable medical condition that can cause disability and death. The American Society of Hematology. external icon.
What is the best treatment for PE?
Immediate medical attention is necessary to treat PE. In cases of severe, life-threatening PE, there are medicines called thrombolytics that can dissolve the clot. Other medicines, called anticoagulants, may be prescribed to prevent more clots from forming.
What is a deep vein thromboembolism?
Deep vein thrombosis (DVT) is a medical condition that occurs when a blood clot forms in a deep vein.
What is the most serious complication of DVT?
Complications of DVT. The most serious complication of DVT happens when a part of the clot breaks off and travels through the bloodstream to the lungs, causing a blockage called pulmonary embolism ( PE). If the clot is small, and with appropriate treatment, people can recover from PE.
What are the factors that increase the risk of DVT?
Heart disease. Lung disease. Cancer and its treatment. Inflammatory bowel disease (Crohn’s disease or ulcerative colitis) Other factors that increase the risk of DVT include: Previous DVT or PE. Family history of DVT or PE. Age (risk increases as age increases) Obesity.
Why is it important to know about DVT?
It is important to know about DVT because it can happen to anybody and can cause serious illness, disability, and in some cases, death. The good news is that DVT is preventable and treatable if discovered early.
What are the causes of DVT?
Following is a list of factors that increase the risk of developing DVT: Injury to a vein, often caused by : Fractures, Severe muscle injury, or. Major surgery (particularly involving the abdomen, pelvis, hip, or legs). Slow blood flow, often caused by: Confinement to bed.
What is the first line of treatment for acute DVT?
Patients with submassive (intermediate-high risk) or massive PE as well as patients at high risk for bleeding may benefit from hospitalization. Use of direct oral anticoagulants (DOACs) are recommended as first-line treatment of acute DVT or PE.
How long does it take to treat DVT?
The ASH guidelines define the treatment period of acute DVT/PE as “initial management” (first 5-21 days), “primary treatment” (first 3-6 months), and “secondary prevention” (beyond the first 3-6 months).
What is the ASH recommendation for DVT?
The ASH guidelines suggest against the routine use of prognostic scores, D-dimer testing, or venous ultrasound to guide the duration of anticoagulation. For patients with breakthrough DVT and/or PE while on therapeutic VKA treatment, the ASH guidelines suggest using low molecular weight heparin over DOAC therapy.
How often do DVT and PE occur?
The ASH assembled a multidisciplinary writing committee to provide evidence-based guidelines for management of DVT and PE, which occur 300,000-600,000 times annually in the United States. The ASH guidelines suggest home treatment over hospitalization for patients with uncomplicated acute DVT.
Can you use compression stockings for DVT?
For patients with acute DVT who are not at high risk for post-thrombotic syndrome, the ASH guidelines recommend against the routine use of compression stockings. However, select patients may benefit from compression stockings to help with edema and pain associated with acute DVT. Share via:
Is thrombolysis considered a high risk procedure?
Thrombolysis is reasonable to consider for patients at low bleeding risk who are at high risk for decompensation. For patients with extensive DVT in whom thrombolysis is considered appropriate, the ASH guidelines suggest using catheter-directed thrombolysis over systemic thrombolysis.