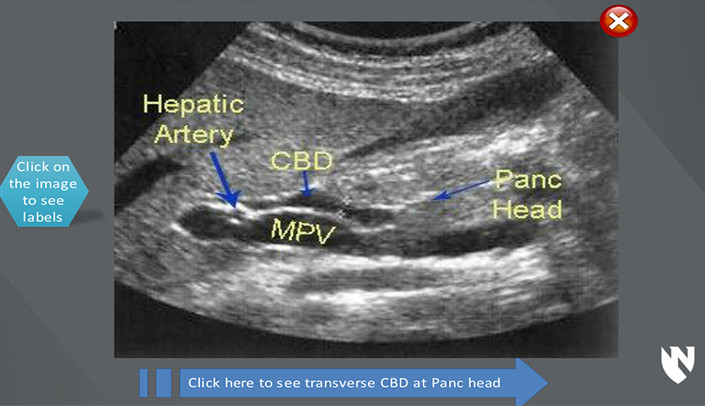
What is the path of bile through the liver?
[1] Bile formed in the liver flows through the right and left hepatic ducts into the common hepatic duct. The common hepatic duct then joins the cystic duct arising from the gallbladder to form the common bile duct.
Why is the biliary tract called biliary?
The name biliary tract is used to refer to all of the ducts, structures and organs involved in the production, storage and secretion of bile. The tract is as follows: Bile is secreted by the liver into small ducts that join to form the common hepatic duct.
What are the ducts of the biliary tract?
Ducts of the biliary tract. [edit on Wikidata] The biliary tract, (biliary tree or biliary system) refers to the liver, gall bladder and bile ducts, and how they work together to make, store and secrete bile.
Where does bile drain from the gallbladder?
These ducts ultimately drain into the common hepatic duct. The common hepatic duct then joins with the cystic duct from the gallbladder to form the common bile duct. This runs from the liver to the duodenum (the first section of the small intestine). However, not all bile runs directly into the duodenum.
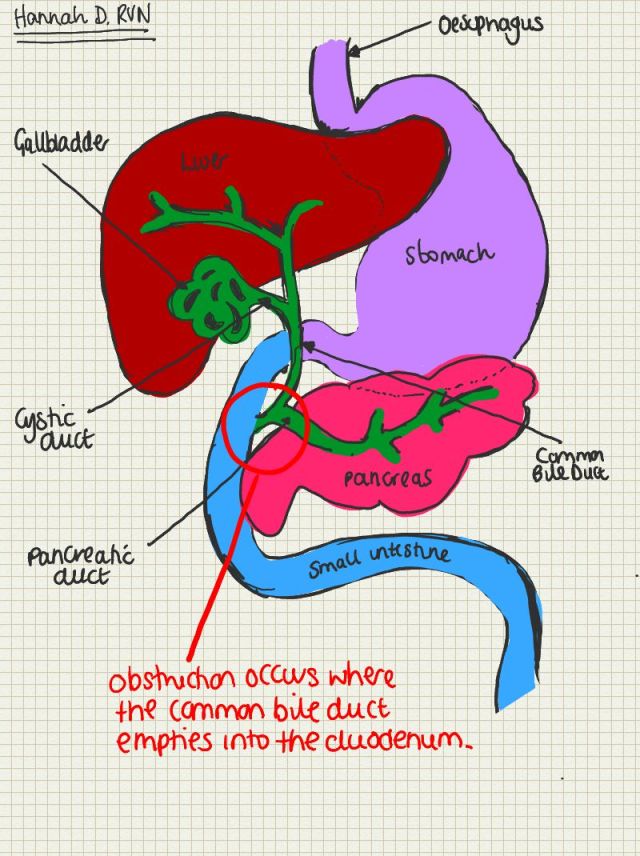
Where does the bile duct terminate?
Termination of the common bile duct at the junction of the second and third parts of the duodenum.
Where does the bile duct start and end?
A tube that carries bile from the liver and gallbladder, through the pancreas, and into the small intestine. The common bile duct starts where the ducts from the liver and gallbladder join and ends at the small intestine. It is part of the biliary system. Anatomy of the extrahepatic bile ducts.
What are the steps of the biliary system?
There are three important functions of the biliary system: Draining the waste products from the liver (into the duodenum) Secreting bile in a controlled-release manner. Transporting bile and pancreatic juices to help break down food in the small intestine.
Where do the pancreatic and common bile ducts terminate?
The common bile duct passes through the pancreas before it empties into the first part of the small intestine (duodenum). The lower part of the common bile duct joins the pancreatic duct to form a channel called the ampulla of Vater or it may enter the duodenum directly.
Where does bile go after gallbladder removal?
Normally, the gallbladder collects and concentrates bile, releasing it when you eat to aid the digestion of fat. When the gallbladder is removed, bile is less concentrated and drains more continuously into the intestines, where it can have a laxative effect.
How does bile go from liver to gallbladder?
Bile flows out of the liver through the left and right hepatic ducts, which come together to form the common hepatic duct. This duct then joins with a duct connected to the gallbladder, called the cystic duct, to form the common bile duct.
What are the three anatomic areas of the biliary system?
Anatomy of the biliary system The biliary system consists of the organs and ducts (bile ducts, gallbladder, and associated structures) that are involved in the production and transportation of bile.
What is included in the biliary tract?
The organs and ducts that make and store bile (a fluid made by the liver that helps digest fat), and release it into the small intestine. The biliary tract includes the gallbladder and bile ducts inside and outside the liver.
Which is the order of flow of secreted bile in the body quizlet?
Bile is produced in the liver, then flows through the right and left hepatic ducts to enter common hepatic duct, then flows to cystic duct and is stored in gallbladder. The gallbladder then constricts and bile flows back to cystic duct and into common bile duct, which empties into duodenum.
Does the bile duct go through the pancreas?
The common bile duct passes through part of the pancreas before it joins with the pancreatic duct and empties into the first part of the small intestine (the duodenum) at the ampulla of Vater.
Is pancreatic duct part of biliary system?
The pancreas and bile duct (biliary) systems together form an important part of the digestive system. The pancreas and liver produce juices (pancreatic juice and bile) which help in the process of digestion (i.e. the breakdown of foods into parts which can be absorbed easily and used by the body).
Where does the bile duct lead to?
The common bile duct passes through the pancreas and ends in the small intestine. Bile is made by the liver and stored in the gallbladder. When food is being digested, bile is released from the gallbladder and passes through the pancreas into the small intestine, where it helps digest fats.
What are the symptoms of bile duct problems?
Symptoms may include:Abdominal pain in the upper right side.Dark urine.Fever.Itching.Jaundice (yellow skin color)Nausea and vomiting.Pale-colored stools.
Where does the bile duct lead to?
The common bile duct passes through the pancreas and ends in the small intestine. Bile is made by the liver and stored in the gallbladder. When food is being digested, bile is released from the gallbladder and passes through the pancreas into the small intestine, where it helps digest fats.
How many bile ducts does a person have?
twoThe liver makes bile which is stored in the gallbladder. There are two main bile ducts in the liver: right hepatic duct. left hepatic duct.
What is the bile duct connected to?
The common bile duct connects the liver, gallbladder, and pancreas to the small intestine.
What is the biliary system?
Biliary tract. The biliary tract, ( biliary tree or biliary system) refers to the liver, gall bladder and bile ducts, and how they work together to make, store and secrete bile. Bile consists of water, electrolytes, bile acids, cholesterol, phospholipids and conjugated bilirubin. Some components are synthesised by hepatocytes (liver cells), ...
Where is bile stored?
Bile is secreted by the liver into small ducts that join to form the common hepatic duct. Between meals, secreted bile is stored in the gall bladder, where 80–90% of the water and electrolytes can be absorbed, leaving the bile acids and cholesterol.
What ducts enter the duodenum?
These merge to form the common hepatic duct. This exits the liver and joins with the cystic duct from gall bladder. Together these form the common bile duct which joins the pancreatic duct. These pass through the ampulla of Vater and enter the duodenum.
Why does biliary colic hurt?
Rather, pain may be caused by luminal distension, which causes stretching of the wall. This is the same mechanism that causes pain in bowel obstructions.
What is the function of the gallbladder wall?
During a meal, the smooth muscles in the gallbladder wall contract, leading to the bile being secreted into the duodenum to rid the body of waste stored in the bile as well as aid in the absorption of dietary fats and oils by solubilizing them using bile acids .
What is the name of the first part of the small intestine?
Small intestine: 19. Duodenum, 20. Jejunum. 21–22. Right and left kidneys. The front border of the liver has been lifted up (brown arrow). The biliary tract refers to the path by which bile is secreted by the liver then transported to the duodenum, the first part of the small intestine. A structure common to most members of the mammal family, ...
What is the function of the biliary system?
The biliary system's main function includes the following: 1 To drain waste products from the liver into the duodenum 2 To help in digestion with the controlled release of bile
How does bile travel through the liver?
The transportation of bile follows this sequence: When the liver cells secrete bile, it is collected by a system of ducts that flow from the liver through the right and left hepatic ducts. These ducts ultimately drain into the common hepatic duct. The common hepatic duct then joins with the cystic duct from the gallbladder to form ...
Which duct runs from the liver to the duodenum?
The common hepatic duct then joins with the cystic duct from the gallbladder to form the common bile duct. This runs from the liver to the duodenum (the first section of the small intestine).
What is the function of bile?
Bile is the greenish-yellow fluid (consisting of waste products, cholesterol, and bile salts) that is secreted by the liver cells to perform 2 primary functions: To carry away waste. To break down fats during digestion. Bile salt is the actual component that helps break down and absorb fats.
Where is the liver stored?
About 50% of the bile produced by the liver is first stored in the gallbladder. This is a pear-shaped organ located directly below the liver. Then, when food is eaten, the gallbladder contracts and releases stored bile into the duodenum to help break down the fats.
What is the tube that allows bile to go into the small intestine?
Bile ducts are thin tubes that allow bile to go from the liver and gallbladder into the small intestine, helping digest the fats in your food.
What is the biliary tree?
The extrahepatic (originating outside the liver) biliary tract , also known as the biliary tree, includes the gallbladder, bile ducts, and the sphincter of Oddi. The biliary tract collects, stores, concentrates, and delivers bile secreted by the liver to aid digestion.
What is the sphincter of Oddi?
The sphincter of Oddi (SO) is a smooth muscle approximately 10mm (4 inches) in length that surrounds the end portion of the common bile duct and pancreatic duct. This muscle relaxes during a meal to allow bile and pancreatic juice to flow into the intestine.
How much bile does the gallbladder store?
It can store about 30 to 60 milliliters of bile. When fasting, the gallbladder can handle more. Covered by a thin layer of peritoneum, it’s connected to the common hepatic duct via the cystic duct. (See bile ducts next.) The gallbladder itself be divided into four parts, the fundus, the body, the infundibulum, and the neck.
What is the gallbladder?
The gallbladder is a small, slightly elongated pear-shaped organ where bile from the liver is stored and concentrated before releasing it into the small intestine. The gallbladder is an accessory organ of the digestive tract that sits underneath the liver slightly higher and adjacent to the duodenum (the first part of the small intestine) and pancreas. The gallbladder allows the gradual entry of bile by passive and active mechanisms.
Where is the sphincter located?
Nearly 400 hundred years ago, Frances Gliesson first described a sphincter structure at the far end of the common bile duct where it enters the duodenum. Still, it was not until 1889, when Rugero Oddi described its anatomy and physiology in detail, that the function of this structure and its role in the control of the flow of bile and pancreatic juices were appreciated.
What happens when fat reaches the small intestine?
When the fat you consume reaches the small intestine, it is in the form of large fat droplets. Bile is released into the small intestine, and the bile salts mix with the large fat droplets emulsifying a breaking them down into smaller droplets.
How Does the Biliary System Work?
The first is to break down fats when food is digested. The second is to carry waste away from your digestive system. Bile contains a salt component that breaks down fat, absorbs it, and moves it through your digestive system and into your feces for removal.
What is the biliary system?
Your body’s biliary system encompasses your bile ducts, gallbladder, and the associated digestive structures. This system works together to move bile, also called digestive fluid, through your system as it is needed for digestion.
What is the function of the gallbladder?
Your gallbladder controls the amount of bile released, which depends on how much your stomach needs for digestion. Your biliary system also serves to drain waste from your liver into the duodenum, a part of your digestive system that is just below your stomach.
What is Barrett's esophagus?
Barrett's esophagus. This is a serious health condition that is usually diagnosed after suffering from reflux and GERD for a long time. Acid and bile damage your esophageal tissue so badly that the tissue is at risk for developing cancer.
What is gallbladder surgery?
Gallbladder surgery is called a cholecystectomy. The incisions made to remove your gallbladder are very small. The surgery is generally considered low-risk, and many patients go home the same day following their procedure. If a larger incision is necessary, your healing may be extended.
Where does bile come from?
Bile begins in your liver, where it is created by special cells. From there, your bile ducts collect the bile and move it through the hepatic duct until it joins the cystic duct from your gallbladder and becomes the common bile duct.
Is bile a part of GERD?
GERD. This is a different condition from bile reflux, although the symptoms are very similar. Bile may be mixed in with the stomach acid if you suffer from this condition. In fact, medical professionals suspect that bile contributes significantly to GERD.
Where does bile go in the body?
Bile then flows from the gallbladder into the small intestine to mix with food contents and perform its digestive functions. After bile enters and passes down the small intestine, about 90% of bile salts are reabsorbed into the bloodstream through the wall of the lower small intestine. The liver extracts these bile salts from ...
Where does the bile duct enter the small intestine?
The common bile duct enters the small intestine at the sphincter of Oddi (a ring-shaped muscle), located a few inches below the stomach. About half the bile secreted between meals flows directly through the common bile duct into the small intestine. The rest of the bile is diverted through the cystic duct into the gallbladder to be stored.
What is the purpose of bile salts?
Bile salts aid in digestion by making cholesterol, fats, and fat-soluble vitamins easier to absorb from the intestine. Bilirubin is the main pigment in bile. Bilirubin is a waste product that is formed from hemoglobin (the protein that carries oxygen in the blood) and is excreted in bile.
What is the gallbladder?
Videos (2) The gallbladder is a small, pear-shaped, muscular storage sac that holds bile and is interconnected to the liver by ducts known as the biliary tract. (See also Overview of the Liver and Gallbladder .) Bile is a greenish yellow, thick, sticky fluid. It consists of bile salts, electrolytes (dissolved charged particles, ...
How many times do bile salts go through the liver?
The liver extracts these bile salts from the blood and resecretes them back into the bile. Bile salts go through this cycle about 10 to 12 times a day. Each time, small amounts of bile salts escape absorption and reach the large intestine, where they are broken down by bacteria.
What is bile made of?
It consists of bile salts, electrolytes (dissolved charged particles, such as sodium and bicarbonate), bile pigments, cholesterol, and other fats (lipids). Bile has two main functions:
How much water is absorbed into the bloodstream?
In the gallbladder, up to 90% of the water in bile is absorbed into the bloodstream, making the remaining bile very concentrated. When food enters the small intestine, a series of hormonal and nerve signals triggers the gallbladder to contract and the sphincter of Oddi to relax and open. Bile then flows from the gallbladder into ...
Where does bile go in the liver?
Bile formed in the liver flows through the right and left hepatic ducts into the common hepatic duct. Fifty percent of the bile flows into the cystic duct and is then stored in the gallbladder, with the rest of the bile flowing through the common bile duct and converging and flowing through the main pancreatic duct in the head of the pancreas to empty into the duodenum through the sphincter of Oddi.
Where is bile transported?
Bile is then transported via the bile ducts into the second portion of the duodenum to assist with the metabolism of fats. [1]
What is biliary obstruction?
Biliary obstruction commonly refers to blockage of the bile duct system leading to impaired bile flow from the liver into the intestinal tract. Bile is a substance that contains bile salts, bilirubin, and cholesterol and is continuously synthesized in the liver hepatocytes.
What hormone controls the release of stored bile from the gallbladder?
The flow of bile into the duodenum is regulated by the release of the hormone Cholecystokinin (CCK) from the duodenum, which controls the release of stored bile from the gallbladder and the relaxation of the sphincter of Oddi. Biliary obstruction is generally referred to as blockage of the extrahepatic biliary system.
How many people have gallstones?
The incidence of gallstones causing biliary obstruction is approximately 5 in 1000 people, whereas 10% to 15% of the adult U.S. population will develop gallstones in their lifetime.[6] Gall stones or Cholelithiasis, including gall bladder sludge formation, is the precursor of choledocholithiasis, where gall stones pass through the cystic duct and get lodged into the common hepatic ducts causing an obstruction. Between 10 and 15% of patients with gall stones are also noted to have common bile duct stones at diagnosis. [7]
Which duct joins the gallbladder?
The common hepatic duct then joins the cystic duct arising from the gallbladder to form the common bile duct. The common bile duct then joins the pancreatic duct through its course within the head of the pancreas before opening into the duodenum through the major papilla or ampulla.
Is bilirubin in urine normal?
Jaundice is evident clinically at the level of 3 mg/dl. Normal urine contains no bilirubin; however, in patients with obstructive jaundice, conjugated bilirubin is excreted in the urine, giving it a dark color. Urinary bilirubin is detectable at a lower level of bilirubin than that needed to cause clinical jaundice.
How long does it take for a bile bag to be removed after a papillectomy?
A T-tube cholangiogram is taken about 5 to 7 days after the operation. If it appears normal, the tube is removed on day 7 or 8 by gentle traction.
Why is bile allowed to drain?
Initially, bile is allowed to drain freely into a bile bag to allow any spasm or edema of the sphincter to settle before testing the suture line of the choledochotomy . The volume drained varies, with the amount decreasing as flow increases through the sphincter. If the volume drained remains high or increases, the reason should be established. This increased volume may be due to continuing distal obstruction or to the distal limb lying within the duodenum. Similarly, there is a problem if there is no drainage of the bile, or if bile drains around the T-tube; the tube may have become blocked or dislodged from the duct.
What is the procedure called when you have to pass a cholangioscope through a peroral or per?
Cholangioscopy requires skill and patience and involves the passage of a cholangioscope through a peroral or percutaneous transhepatic tract.
What is cholangioscopy performed by?
Cholangioscopy can be performed by the per-oral transpapillary or percutaneous transhepatic route. It allows direct visual assessment of the biliary tree, tissue sampling, and therapeutic interventions.
What is the role of cholangioscopy in hepatolithiasis?
Cholangioscopy plays an indispensable role in the management of hepatolithiasis. With the recent availability of digital cholangioscopy, high-quality images of the biliary tract can be obtained. Moreover, any suspicious biliary stricture can be biopsied to rule out malignancy.
Can a per-oral cholangioscopy be performed with an axial endoscope?
Per-oral cholangioscopy can also be performed with an axial endoscope in patients with a sufficiently wide choledochoduodenal anastomosis ( Fig. 3) or following an endoscopic sphincterotomy in a patient with a Billroth II gastrectomy. Recent developments include the introduction of a videocholangioscope with narrow-band imaging, ultraslim scopes (external diameter 2.09 mm) which can be inserted without a prior sphincterotomy, and can be performed with only one operator. Ultrathin pancreatoscopes have also been developed with external diameters of between 0.5 and 0.8 mm.
Can a choledochotomy be used to examine the bile duct?
The transcystic approach to examination and stone extraction is limited to some extent by the size and number of stones and is not possible in cases of a low insertion of the cystic duct. These limitations have led to the progressive evolution of laparoscopic bile duct exploration through a choledochotomy incision, a technique that is technically more demanding, but is being used more frequently (Decker et al, 2002; Martin et al, 1998 ). In a multicenter study from France, Decker and coworkers (2003) reported results of 100 laparoscopic choledochotomies with choledochoscopy and primary closure of the duct without external biliary drainage. In this study, the authors used a standard laparoscopic cholecystectomy approach, placing a fifth port (10 mm) in the right subcostal area after confirming choledocholithiasis. Through this port, a 3.5-mm or 5.8-mm fiberoptic choledochoscope was inserted and used to examine the bile duct through a longitudinal or transverse choledochotomy. Successful stone extraction was performed using a variety of means, including a Dormia basket passed through the operating channel of the choledochoscope. After completion, choledochoscopy showed no residual stones; the choledochotomy was closed primarily, after which methylene blue dye was injected through a transcystic cholangiogram catheter. Operative morbidity in this study was low, and excellent short-term and long-term results were documented.
Topics in the Surgery of the Biliary Tree
1. Choose citation style Select style Vancouver APA Harvard IEEE MLA Chicago
Abstract
Injuries of the biliary system are rare. They can broadly be divided into traumatic biliary injuries and iatrogenic biliary injuries.
1. Introduction
Isolated traumatic injuries of the biliary tract are extremely rare.
2. Classification
Traumatic injuries to the biliary system can be intrahepatic or extrahepatic.
3. Etiology and mechanism of injuries
Injuries to the liver, biliary tree and pancreas are commonly referred to as the “surgical soul”. They can be deadly and challenging to treat and they demand multidisciplinary approach in establishing correct diagnosis which then will provide best treatment plan, and as a result, have optimal treatment outcome.
4. Diagnosis and presentation
Imaging modalities are very important in establishing the diagnosis, delineating the extent of injury and planning appropriate intervention.
5. Treatment options
Traumatic biliary tract injuries are not common so there can be a challenge and difficulty in their diagnosis. If they are recognized late and thus, managed inappropriately they can have fatal consequences. The approach to the treatment is dependant primarily on the hemodynamic status of the patient.
