What is the QRS complex in ECG?
The QRS complex (ventricular complex): normal and abnormal configurations and intervals A complete QRS complex consists of a Q-, R- and S-wave. However, all three waves may not be visible and there is always variation between the leads. Some leads may display all waves, whereas others might only display one of the waves.
Why are the leads on an ECG different in shape?
Each individual lead’s ECG recording is slightly different in shape. This is because each lead is recording the electrical activity of the heart from a different direction (a.k.a viewpoint). When the electrical activity within the heart travels towards a lead you get a positive deflection.
Does the position during electrocardiogram (ECG) recording alter the ECG curve?
The aim of this study was to evaluate whether change in the patients' position during the electrocardiogram (ECG) recording alters the various components of the ECG curve. Concerns whether ECGs in medically compromised patients recorded in a sitting position should be considered "standard" tracings …
Can QRS morphology on EKG predict the site of origin of PVCs?
The QRS morphology on EKG can predict the PVCs site of origin. As a broad general rule, the right ventricular ectopic pacemaker generates a ventricular complex with left bundle branch block (LBBB) pattern, and the left ventricular ectopic pacemaker generates a ventricular complex with right bundle branch block (RBBB) pattern 2.

Why are some ECG complexes inverted?
It is normally upside down in VR and V1. If it is upside down in any other lead, then the likely causes are ischaemia or ventricular hypertrophy (Fig. 1.12).
Which position is best for EKG?
Answer. The standard 12-lead ECG is generally performed with the patient lying quietly in the supine position. Care should be taken to ensure that the skin is clean and trimmed of excess hair in the areas in which the leads are to be placed.
Why is QRS complex a downward?
Why QRS complex is a downward deflection? Solution : QRS complex is caused due to ventricular depolarization resulting in ventricular contraction, and hence it is a dowward deflection.
Why is the T wave upright?
Furthermore, tall or wide QRS complex with an upright T wave is further suggestive of the posterior infarction. Wellens' syndrome is caused by the injury or blockage of the left anterior descending artery, therefore resulting in symmetrical T wave inversions from V2 to V4 with depth more than 5 mm in 75% of the cases.
Can you do an EKG standing up?
Background: The electrocardiogram (ECG) is a critical component of cardiovascular diagnosis. ECGs are standardly recorded in the supine position; however, due to time and space constraints as well as patient limitations, they are often performed in other positions (sitting, standing).
Do you have to lay flat for an EKG?
It will be important for you to lie still and not talk during the ECG, so that you don't alter the tracing. If your chest, arms, or legs are very hairy, the technician may shave or clip small patches of hair, as needed, so that the electrodes will stick closely to the skin.
What does a tall QRS complex mean?
Increased QRS voltage is often taken to infer the presence of left ventricular hypertrophy. However, high left ventricular voltage (HLVV) may be a normal finding in patients less than 40-45 years of age, particularly slim or athletic individuals.
When labeling a QRS complex what is the first downward deflection called?
1. When the initial deflection of the QRS complex is negative (below the baseline), it is called a Q wave.
What is the first downward deflection called?
the Q waveThe first downward deflection is called the Q wave. The first upward deflection is called the R wave. The second downward deflection after the R wave is called the S wave.
What does it mean if you have an inverted T wave?
T wave inversions in the right chest leads may be caused by right ventricular overload (e.g., acute or chronic pulmonary embolism) and in the left chest leads by left ventricular overload (Chapter 7). Diffusely inverted T waves are seen during the evolving phase of pericarditis or myocarditis.
What does an upright T wave in V1 mean?
Upright T wave in precordial lead V1 indicates the presence of significant coronary artery disease in patients undergoing coronary angiography with otherwise unremarkable electrocardiogram.
What does inverted T waves mean?
T‐wave inversion (TWI) is defined as negative T‐wave of ≥1 mm in depth in two or more contiguous leads, with exclusion of leads aVR, III, and V1. 1. The presence of TWI at 12‐lead electrocardiogram (ECG) in competitive athletes is one of the major diagnostic challenges for sports physicians and consulting cardiologists ...
When taking an ECG the position of the first chest lead V1 is?
This gap is the 2nd Intercostal space. From this position, run your fingers downward across the next rib, and the next one. The space you are in is the 4th intercostal space. Where this space meets the sternum is the position for V1.
How do you perform an EKG on a patient?
4:409:24EKG 01: How to perform an EKG - YouTubeYouTubeStart of suggested clipEnd of suggested clipThe left arm one goes in about the same position except on the left arm. The left leg goes justMoreThe left arm one goes in about the same position except on the left arm. The left leg goes just lateral to the calf muscle. And the right leg goes lateral to the calf muscle on the right leg.
How do you do an EKG test?
Small pads or patches (electrodes) will be placed, like stickers, on your skin on each arm and leg and on your chest. The electrodes are hooked to a machine that traces your heart activity onto a paper. During the test, lie very still and breathe normally. Do not talk during the test.
How many squares are in an EKG?
Each of the small squares equal 0.4 second of time. Five small squares equal 0.20 seconds. Fifteen of the 0.20 squares represent 3 seconds. These 3 – second time intervals are marked on the paper by darker lines as shown below.
Where is the pacemaker site of a normal QRS complex?
The pacemaker site of a normal QRS complex is the SA node or an ectopic pacemaker in the atria of AV junction. (The origin of the QRS is originally from the SA node, and then spreads down through the atria to the AV node, etc.) The onset of the QRS Complex is identified as the point where the first wave of the complex just begin to deviate, abruptly or gradually, from the baseline.
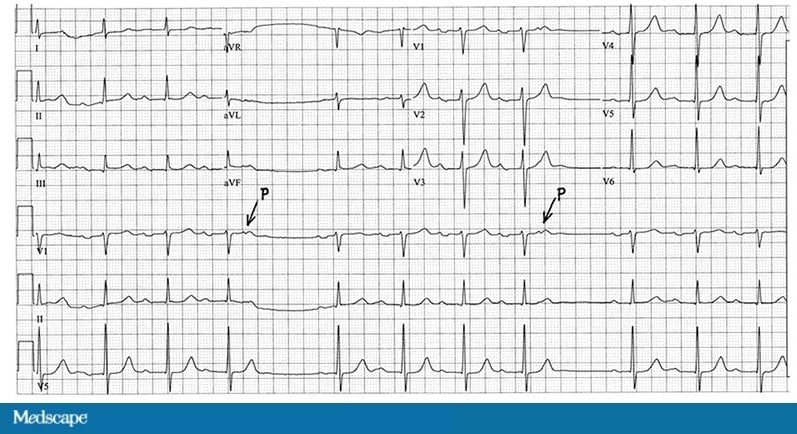
What does a sinus P wave mean?
A normal sinus P Wave indicates that the electrical impulse responsible for the P Wave originated in the SA node and that normal depolarization of the right and left atria has occurred. SA node is the pacemaker site.
What is the junction of the QRS complex and the S-T segment?
This point the junction between the QRS complex and the S-T segment is called the “JUNCTION” or “J POINT.” A normal QRS Complex indicates that the electrical impulse has progressed normally from the bundle of HIS to the Purkinje network through the right and left bundle branches, and that normal depolarization of the right and left ventricles has occurred. Of course, there can be several “normal” variations of the QRS Complex. These will be discussed later in the course.
How long is the QRS complex?
The DURATION of the QRS Complex is 0.06 to 0.10 seconds in adults and 0.08 or less in children.
What part of the sinus P wave represents depolarization?
The first part of the normal sinus P Wave represents depolarization of the right atrium; the second part represents depolarization of the left atrium.
What does the P wave represent?
The P wave represents depolarization of the right and left atria.
Where is the most common site of origin for PVC in the absence of structural heart disease?
The right or left ventricular outflow tracts and aortic cusp are the most common sites of origin for PVC in the absence of structural heart disease.
What is a premature ventricular complex?
Premature ventricular complexes reflect activation of the ventricles from a site below the AV node.
What pattern does a left ventricular ectopic pacemaker have?
As a broad general rule, the right ventricular ectopic pacemaker generates a ventricular complex with left bundle branch block (LBBB) pattern, and the left ventricular ectopic pacemaker generates a ventricular complex with right bundle branch block (RBBB) pattern 2.
Why do PVCs occur?
PVCs caused by triggered activity are often seen in patients with ventricular arrhythmias due to digoxin toxicity and reperfusion therapy after an acute myocardial infarction. The mechanism of PVCs in patients without structural heart disease is thought to be enhanced automaticity versus triggered activity.
What is the term for the cycle after the PVC is longer than the basic cycle?
Premature ventricular complexes are typically followed by a compensatory pause. That means that the cycle length after the PVC is longer than the basic cycle.
What is fusion beat?
Fusion beats or fusion complexes occur when a supraventricular impulse reaches the ventricles during a ventricular beat and they coincide to produce a hybrid complex. The morphology and duration of fusion beats are usually intermediate between the morphologies and durations of two QRS complexes.
How many sinus beats does PVC occur?
Trigeminy: PVC occurring every third beat (two sinus beats followed by a PVC).
What is the first step in an EKG assessment?
First Step. The first step in your assessment should be to get a general sense of the EKG. Mentally note if you see something out of the ordinary and come back to it as you go through your assessment.
What is the second step in an EKG?
The second step begins our formal analysis of the 12-lead EKG. Check the calibration block on the 12-lead. Is it standard, half-standard, or 2 times standard? Don't forget to do this.
How to tell if you have left atrial enlargement?
Atrial enlargement:First, take another scan of p-waves in each lead, but pay most attention to the p-waves in Lead II and V1 (best leads to look in for p-waves!!). In Lead II, are the p-waves greater than 2.5 mm in height with a peaked look to them? If they do, you may have right atrial enlargement. Do the p-waves have a double peak and are greater than .11 sec in duration? If so, you may have left atrial enlargement. Next, look at p-waves in V1. Normally, V1 has an equiphasic look to it. If the first, upright portion of the p-wave is greater than 1 mm in height and width, and much larger than the downward portion, you may have right atrial enlargement. The opposite is true for left atrial enlargement (downward portion is larger than upright portion of p-wave).
What is the seventh step in the 12 lead checklist?
The seventh step in our 12 lead checklist deals with diagnosing bundle branch blocks. Diagnosing both kinds of blocks requires looking in the same leads; however, the QRS will look much different between the two blocks. But, the QRS complex, for both blocks, has to exceed a duration of greater than or equal to .12 sec.
What are the leads to look for in a right bundle branch block?
Right bundle branch block:The leads to look in first for right bundle branch block (RBBB for short) are leads V1 & V2. In RBBB, the QRS complex has two R-waves which give the QRS a double-peaked appearance. This is called the “R-S-R1” wave. This must be present for RBBB. Next, to give further support to your diagnosis, look in leads I, V5, & V6. A good sign of RBBB is if the S wave has a “slurred” appearance or the end of the wave doesn’t return sharply back up to baseline.
What are the leads to look for lateral MI?
Lateral MI:The leads to look in for lateral MI are leads I , AVL, V5, & V6. A significant Q wave in leads I & AVL is called an “old high lateral MI”, whereas ST segment elevation in these leads is called an “acute high lateral MI”. V5 & V6 look at the “low” lateral surface, so Q waves or ST segment elevation in these leads show old and acute “low lateral MI’s”.
What are the leads to look in next?
Inferior MI:The leads to look in next are leads II, III, & AVF. Look for Q waves and ST elevation.
What is the standard for EKG?
Before you read the EKG, look for: Standardization: full standard is two large squares (1 mV, 10 mm) and half standard is one large square (0.5mV, 5 mm) Paper speed: the standard is 25 mm/sec, the faster the paper speed the slower the HR will look and vice versa.
Which wave is preceded by a narrow QRS complex?
Characterized by narrow QRS complexes preceded by P waves that do not fulfill one or more of the normal sinus rhythm (NSR) criteria mentioned earlier.
What happens when the atrial focus fails?
When the atrial focus fails, the AV node will take over. Subsequently, if the AV node fails, the ventricular focus, which is the slowest, will take over as a pacemaker. Each time the focus is downgraded, the heart rate becomes slower based on the inherent automaticity of the pacemaker.
Why is the P wave inverted?
An inverted P wave may be seen following the QRS due to retrograde conduction.
When does the T wave become upright?
T wave remains inverted in V1 throughout early childhood. T wave becomes upright in V1 in late childhood and early adolescence and is no longer diagnostic of RVH.
Which cell has the fastest pacemaker?
The SA nodal cells have the fastest automaticity (pacemaker) and hence control the heart rate and rhythm. There are 4 levels of conductions and potential pacemakers in the heart from fastest to slowest: SA node → atria → AV node → ventricles.
What leads are QRs on an electrocardiogram?
qRs: small initial non-pathological Q wave, followed by a tall R wave and a small S wave. On a normal electrocardiogram, it can be seen in leads V5 and V6.
What does it mean when a QRS complex is positive?
When the QRS complex is clearly positive, it means that the electric impulse flows towards the lead; if the QRS complex is negative, the impulse flows away from the lead; if the QRS complex is biphasic it means the direction of the impulse is perpendicular to the lead.
Why is complex polarity important?
QRS complex polarity is important in order to determine the QRS axis, when the QRS polarity in leads I and III allow us to quickly estimate whether it is normal or not.
When the amplitude of the largest positive wave (R or R') is smaller than the amplitude of?
When the amplitude of the largest positive wave (R or R') is smaller than the amplitude of the deepest negative wave (Q or S).
What does QS mean on an AVR?
When found in other leads, it is a sign of myocardial infarction (previous STEMI) in the corresponding heart area. QS: a lone, deep negative wave. It is a sign of myocardial infarction in the region near to the electrocardiogram leads, it should not be present on a normal EKG.
How to find out if an ECG is irregular?
The second step in analyzing an ECG. To find this you measure the distance between all the R-R waves on the strip and if they are all the same the rhythm is called regular, if not the rhythm is called irregular and irregular rhythms are considered abnormal. You can also measure the P-waves and this is called the P-P interval to see if they are regular
How many millimeters per second does an electrocardiogram take?
The results of the electrocardiogram are printed on a special graph paper which travels through the electrocardiogram at a rate of about 25 millimeters per second. The graph paper has both horizontal and vertical lines which serve to divide the paper into squares that are 5 millimeters in width and height.
What are the three layers of the heart?
The heart consists of three layers: the pericardium, the myocardium, the epicardium and the endocardium. Located within the myocardium is the electrical conduction system. This is the system responsible for the regulation of the pumping action of the heart, as well as the conduction of the electrical impulses that causes the myocardium to contract. Cardiac depolarization and repolarization occur when these electrical impulses develop and spread through the myocardium. The rate and rhythm of the heart are controlled by pacemaker cells, an essential part of the conduction system. These cells, also known as cardiac muscle cells, can be characterized by any of the following terms: excitability, conductivity, contractility, and automaticity.
How to separate the P wave?
You can separate the P-wave into two parts the first half of the P-wave is the depolarization of the right atrium and the second half is the depolarization to the left atrium. If there is a dilation of the right atrium then the P-wave will have higher amplitude and be tall and rounded, if there is a dilation of the left atrium then the P-wave will be notched or elongated.
Where does deoxygenated blood go?
Deoxygenated blood arrives at the right atrium, also known as the upper right chamber of the heart. The blood then continues on its way through the tricuspid valve which leads to the Right Ventricle. Once the right ventricle contracts the blood then flows towards the pulmonary valve, and finally the pulmonary arteries.
What is the condition caused by a lack of oxygen-rich blood in the heart?
Also known as angina, is a condition caused by a lack of oxygen-rich blood in the heart.
How to find heart rate with two R waves?
Count number of small squares between two consecutive R-waves and divide that number by 1500, it is the most accurate method of obtaining the heart rate but can only be used on regular rhythms.
Why does the vector during activation of the ventricular free walls not come to expression?
The vector resulting from activation of the right ventricle does not come to expression, because it is drowned by the many times larger vector generated by the left ventricle. Thus, the vector during activation of the ventricular free walls is actually the vector generated by the left ventricle.
What is a QRS complex?
The QRS complex (ventricular complex): normal and abnormal configurations and intervals. A complete QRS complex consists of a Q-, R- and S-wave. However, all three waves may not be visible and there is always variation between the leads. Some leads may display all waves, whereas others might only display one of the waves.
What is the duration of a QRS complex?
Prolongation of QRS duration implies that ventricular depolarization is slower than normal. The QRS duration is generally <0,10 seconds but must be <0,12 seconds. If QRS duration is ≥ 0,12 seconds (120 milliseconds) then the QRS complex is abnormally wide (broad). This is very common and a significant finding. The reason for wide QRS complexes must always be clarified. Clinicians often perceive this as a difficult task despite the fact that the list of differential diagnoses is rather short. The following causes of wide QRS complexes must be familiar to all clinicians:
How many vectors are generated by depolarization of the ventricles?
Depolarization of the ventricles generate three large vectors, which explains why the QRS complex is composed of three waves. It is fundamental to understand the genesis of these waves and although it has been discussed previously a brief rehearsal is warranted. Figure 7 illustrates the vectors in the horizontal plane. Study Figure 7 carefully, as it illustrates how the P-wave and QRS complex are generated by the electrical vectors.
Why are R waves high?
It is important to assess the amplitude of the R-waves. High amplitudes may be due to ventricular enlargement or hypertrophy. To determine whether the amplitudes are enlarged, the following references are at hand:
Where does the ventricular free wall occur?
Activation of the ventricular free wall proceeds from the endocadrium to the epicardium. This is because the Purkinje fibers run through the endocardium, where they deliver the action potential to contractile cells. The subsequent spread of the action potential occur from one contractile cell to another, starting in the endocardium and heading towards the epicardium.
Which side of the ventricular septum is depolarized?
The ventricular septum receives Purkinje fibers from the left bundle branch and therefore depolarization proceeds from its left side towards its right side . The vector is directed forward and to the right. The ventricular septum is relatively small, which is why V1 displays a small positive wave (r-wave) and V5 displays a small negative wave (q-wave). Thus, it is the same electrical vector that results in an r-wave in V1 and q-wave in V5.
Why is the shape of the ECG different?
This is because each lead is recording the electrical activity of the heart from a different direction (a.k.a viewpoint). When the electrical activity within the heart travels towards a lead you get a positive deflection.
What is an ECG?
ECG is the abbreviated term for an electrocardiogram. It is used to record the electrical activity of the heart from different angles to both identify and locate pathology. Electrodes are placed on different parts of a patient’s limbs and chest to record the electrical activity.
What is an ECG electrode?
An ECG electrode is a conductive pad that is attached to the skin to record electrical activity.
How does the 12 lead ECG work?
How the 12 lead ECG works. It is important to understand the difference between an ECG electrode and an ECG lead. An ECG electrode is a conductive pad that is attached to the skin to record electrical activity. An ECG lead is a graphical representation of the heart’s electrical activity which is calculated by analysing data from several ECG ...
What wave should precede each QRS complex?
In healthy individuals, there should be a P wave preceding each QRS complex.
Why is it important to understand which leads represent which anatomical territory of the heart?
It’s important to understand which leads represent which anatomical territory of the heart, as this allows you to localise pathology to a particular heart region.
Which axis gives us an idea of the overall direction of electrical activity?
Whenever the direction of electrical activity moves away from a lead a negative deflection is produced. The cardiac axis gives us an idea of the overall direction of electrical activity. Cardiac conduction. Cardiac axis.