Why does the INR rise in liver disease? The liver produces the majority of the clotting proteins needed for the blood clotting cascade. Severe liver injury leads to reduced hepatic synthesis of coagulation factors and, therefore, prolonged PT or increased INR, which is a method to homogenize PT level reports across the world.
What is the INR of a patient?
What does it mean when INR is 1.0?
About this website
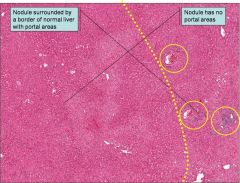
How does liver disease affect INR?
INR is related to the prothrombin time (PT). If there is serious liver disease and cirrhosis, the liver may not produce the proper amount of proteins and then the blood is not able to clot as it should.
Can liver disease cause high INR?
Most patients with liver cirrhosis or other chronic liver diseases hospitalized with ALI have coagulation disorders, which are associated with significantly prolonged prothrombin time (PT) and an increased international normalized ratio (INR) (6).
What does INR tell you about liver function?
International normalized ratio (INR), formally called prothrombin time (PT) test. This test measures how long it takes for blood to clot. Blood clotting needs vitamin K and a protein that is made by the liver. Prolonged clotting may indicate liver disease or other deficiencies in specific clotting factors.
How does liver disease impact coagulation?
The liver plays a central role in the clotting process, and acute and chronic liver diseases are invariably associated with coagulation disorders due to multiple causes: decreased synthesis of clotting and inhibitor factors, decreased clearance of activated factors, quantitative and qualitative platelet defects, ...
What does a high INR level indicate?
An international normalized ratio (INR) is a blood test that indicates how well the blood is able to clot. People who take warfarin (Coumadin) need to monitor this level to make sure it doesn't go too high or too low. If the INR is too high, you are at increased risk of bleeding.
How does cirrhosis affect coagulation?
Cirrhosiscan lead to both a coagulopathic and procoagulant state [1]. There is decreased synthesis of Vitamin K-dependent and independent clotting factors and anticoagulants, platelet production abnormalities, and hypersplenism with platelet consumption [1–4].
What blood tests show cirrhosis of the liver?
If you have symptoms of cirrhosis or you're at risk for the disease, your doctor will take a sample of your blood. These help spot signs of cirrhosis liver damage....These tests include:Alanine transaminase (ALT) and aspartate transaminase (AST). ... Albumin test. ... Bilirubin level. ... Creatinine.More items...•
What blood tests show liver problems?
Some common liver function tests include:Alanine transaminase (ALT). ... Aspartate transaminase (AST). ... Alkaline phosphatase (ALP). ... Albumin and total protein. ... Bilirubin. ... Gamma-glutamyltransferase (GGT). ... L-lactate dehydrogenase (LD). ... Prothrombin time (PT).
Why does liver cause coagulopathy?
Opinion statement. Coagulopathy in patients with liver disease results from impairments in the clotting and fibrinolytic systems, as well as from reduced number and function of platelets. Parenteral vitamin K replacement corrects coagulopathy related to biliary obstruction, bacterial overgrowth, or malnutrition.
Why do liver failure patients bleed?
As the blood pressure in the portal vein system continues to increase, the walls of these expanded veins become thinner, causing veins to rupture and bleed.
Why are liver patients hypercoagulable?
Hypercoagulability in patients with ESLD is associated with fundamental changes in the coagulation profile at the level of primary, secondary and tertiary hemostasis. Though the cause of hypercoagulability is multifactorial, endothelial dysfunction (ED) likely plays a central role.
What happens when PT INR is low?
When the INR is higher than the recommended range, it means that your blood clots more slowly than desired, and a lower INR means your blood clots more quickly than desired.
What does a low INR mean?
PT/INR too low- A low INR means indicates the patient's anticoagulation dose is too low and their blood is clotting too quickly putting them at risk for a blood clot. Symptoms of a low INR- Patients may not always know if their INR levels are too low until they experience symptoms of a clot, either DVT, PE or CVA.
What does an INR of 1.0 indicate?
A result of 1.0, up to 1.5, is therefore normal. A low INR result means your blood is 'not thin enough' or coagulates too easily and puts you at risk of developing a blood clot. A high INR result means your blood coagulates too slowly and you risk bleeding.
What Increases My Risk For An Elevated INR?
1. Too much anticoagulant medicine, a type of blood thinner that helps prevent clots 2. Other medicines, such as aspirin, NSAIDs, and some antibiot...
What Are The Signs and Symptoms of An Elevated INR?
You may have small cuts that bleed more than normal, and for longer than normal. You may bruise easily, have frequent nosebleeds, or notice your gu...
How Is An Elevated INR Treated?
Treatment depends on whether you currently have bleeding and how severe it is. If you take an anticoagulant medicine, your healthcare provider may...
How Can I Prevent An Elevated INR?
1. Have your INR measured regularly. Your healthcare provider may want your INR to be measured every few days until it is stable, and then only onc...
How Can I Decrease My Risk of bleeding?
1. Avoid activities that may cause bleeding or bruising. 2. Brush and shave gently. Use a soft toothbrush and an electric razor to avoid bleeding....
When Should I Contact My Healthcare Provider?
1. Your menstrual period is heavier than normal. 2. You see blood in your urine. 3. Your bowel movement is bloody or black. 4. You bruise or bleed...
When Should I Seek Immediate Care Or Call 911?
1. You throw up blood, or your vomit looks like coffee grounds. 2. You have any kind of bleeding that does not stop in 15 minutes. 3. Your leg feel...
A Guide to INR Levels - North American Thrombosis Forum
The North American Thrombosis Forum (NATF) is a 501(c)3 nonprofit organization incorporated by the Commonwealth of Massachusetts. NATF is dedicated to improving the lives of those affected by blood clots and related diseases. Through our comprehensive resources and innovative programming, we strive to educate patients and healthcare providers about thrombosis and its complications.
International Normalized Ratio - University of Rochester
International Normalized Ratio Does this test have other names? INR, standardized prothrombin time. What is this test? This blood test looks to see how well your blood clots.
Elevated INR: Causes, Signs, Treatment, Prevention - Drugs.com
Drugs.com provides accurate and independent information on more than 24,000 prescription drugs, over-the-counter medicines and natural products. This material is provided for educational purposes only and is not intended for medical advice, diagnosis or treatment. Data sources include IBM Watson Micromedex (updated 1 Sep 2022), Cerner Multum™ (updated 5 Sep 2022), ASHP (updated 1 July 2022 ...
What is an elevated INR?
The INR, or International Normalized Ratio, is a measure of how long it takes your blood to clot. A prothrombin time (PT) is a another blood test done to help measure your INR. The higher your PT or INR, the longer your blood takes to clot. An elevated PT or INR means your blood is taking longer to clot than your healthcare provider believes is healthy for you. When your PT or INR is too high, you have an increased risk of bleeding.
How is an elevated INR treated?
Treatment depends on whether you currently have bleeding and how severe it is. If you take an anticoagulant medicine, your healthcare provider may change your dose, or tell you to skip one or more doses. You may need one of the following treatments:
What are the signs and symptoms of an elevated INR?
You may have small cuts that bleed more than normal, and for longer than normal. You may bruise easily, have frequent nosebleeds, or notice your gums bleeding.
How can I prevent an elevated INR?
Have your INR measured regularly. Your healthcare provider may want your INR to be measured every few days until it is stable, and then only once a month. You may have blood drawn at your healthcare provider's office. Some people can test their blood at home.
How to keep INR stable?
Eat the same amount of vitamin K daily to keep your INR stable. Vitamin K changes how your blood clots and affects your INR. Vitamin K is found in green leafy vegetables, broccoli, grapes, and other foods. Ask your healthcare provider for more information about what to eat when you have an elevated INR.
What does it mean when your PT is too high?
When your PT or INR is too high, you have an increased risk of bleeding.
Does alcohol increase INR?
Limit alcohol. Alcohol increases your INR. Ask your healthcare provider how much alcohol is safe for you.
How to test for INR?
It is recommended by the Clinical and Laboratory Standard Institutes (2017) that the blood specimens for INR/PT testing in the laboratory setting should be collected from venous blood and it is directly obtained into a tube with a light blue top. The tube contains an anticoagulant. The acceptable anticoagulant is the concentration of sodium citrate 3.2%. The tubes must be filled to within 90% of the full collection volume. The tube should be then inverted a few times, gently and as soon as possible, for proper mixing with the anticoagulant. The total time between sample collection and testing should not exceed 24 hours.
What is the INR range for a patient on anticoagulation?
For normal patients who are not on anticoagulation, the INR is usually 1.0 regardless of the ISI or the particular performing laboratory. [8]For patients who are on anticoagulant therapy, the therapeutic INR ranges between 2.0 to 3.0. INR levels above 4.9 are considered critical values and increase the risk of bleeding. The therapeutic INR range differs in a patient with prosthetic valve:
What is the INR for VKA?
International normalized ratio (INR) is the preferred test of choice for patients taking vitamin K antagonists (VKA). It can also be used to assess the risk of bleeding or the coagulation status of the patients. Patients taking oral anticoagulants are required to monitor INR to adjust the VKA doses because these vary between patients. The INR is derived from prothrombin time (PT) which is calculated as a ratio of the patient’s PT to a control PT standardized for the potency of the thromboplastin reagent developed by the World Health Organization (WHO) using the following formula:
What is the target INR for a bileaflet?
For patients with a bileaflet (other than On-X) or current generation, single-tilting disk, mechanical, aortic, prosthetic valve with no other risk factors for thromboembolism, the target INR is 2.5.
How long does it take to get an INR after a valve surgery?
For patients with an On-X mechanical bileaflet aortic valve with no other risk factors for thromboembolism, the INR goal is 2 to 3 for the first three months after valve surgery; and after three months the goal is 1.5 to 2.
Why is warfarin adapted to INR?
The dose of warfarin is adapted based on INR scores so that it remains in the therapeutic range to prevent thrombosis from subtherapeutic INR or hemorrhagic complications from supratherapeutic INR. The anticoagulant effect of warfarin indicated by an INR in the target range also guides us when to discontinue heparin.
What is the target INR for a mitral valve?
For patients with a mechanical mitral prosthetic valve (including On-X valve) or mechanical tricuspid prosthetic valve, the target INR is 3.
What causes an increase in INR?
NUTRITIONAL CONDITION – A poor nutritional state may cause an increase in the level of INR.
Does Vitamin K increase INR?
REDUCED INTAKE OF VITAMIN K – The amount of Vitamin k in our diet should be consistent. If you take less, your INR level may increase. Any changes in the amount of Vitamin K may alter the metabolism of WARFARIN [COUMADIN] in your body.
What is the INR of a neuraxial block?
6 Current American Society of Regional Anesthesia (ASRA) guidelines recommend an INR value of ≤1.4 for performing neuraxial blocks, specifically for patients actively anticoagulated with warfarin. 7 In the conclusion, the authors state that “ [consensus statements] are based on case reports, clinical series, pharmacology, hematology, and risk factors for surgical bleeding. An understanding of the complexity of this issue is essential to patient management; a ‘cookbook’ approach is not appropriate. Rather, the decision to perform spinal or epidural anesthesia/analgesia and the timing of catheter removal in a patient receiving antithrombotic therapy should be made on an individual basis, weighing the small, although definite risk of spinal hematoma with the benefits of regional anesthesia for a specific patient.” 7
How do RBCs affect blood viscosity?
RBCs increase blood viscosity through a process termed reversible aggregation, where reversible linear rouleaux complexes are formed, and formation of these aggregates strongly correlates with high plasma fibrinogen concentrations and is enhanced by high hematocrits. ABO blood groups have also been shown to impact coagulation. The statistically significant higher incidence of VTEs, myocardial infarction, coronary artery disease, peripheral vascular disease, and arterial cerebral ischemia in non–O-type blood is thought to be caused by the higher von Willibrand and FVIII levels found in those with non–O-type blood. Hemoglobin is responsible for nitric oxide transport. Nitric oxide is a known potent vasodilator and inhibitor of platelet aggregation, and 1 study showed that processing and storing RBCs with nitric oxide improve deformability and reduce erythrocyte adhesion. 23 RBCs play a multifactorial role in coagulation and are sure to be included in a future model of coagulation. Other factors such as temperature and pH will likely be included as well.
Does nitric oxide help with platelet aggregation?
Nitric oxide is a known potent vasodilator and inhibitor of platelet aggregation , and 1 study showed that processing and storing RBCs with nitric oxide improve deformability and reduce erythrocyte adhesion. 23 RBCs play a multifactorial role in coagulation and are sure to be included in a future model of coagulation.
What is the INR of a patient?
The INR is another way of measuring the blood-clotting time and it is easier to determine than the PT. < Previous. Just Diagnosed Main. Next >.
What does it mean when INR is 1.0?
A normal INR is 1.0. Each increase of 0.1 means the blood is slightly thinner (it takes longer to clot). INR is related to the prothrombin time (PT). If there is serious liver disease and cirrhosis, the liver may not produce the proper amount of proteins and then the blood is not able to clot as it should. When your provider is evaluating the function of your liver, a high INR usually means that the liver is not working as well as it could because it is not making the blood clot normally.