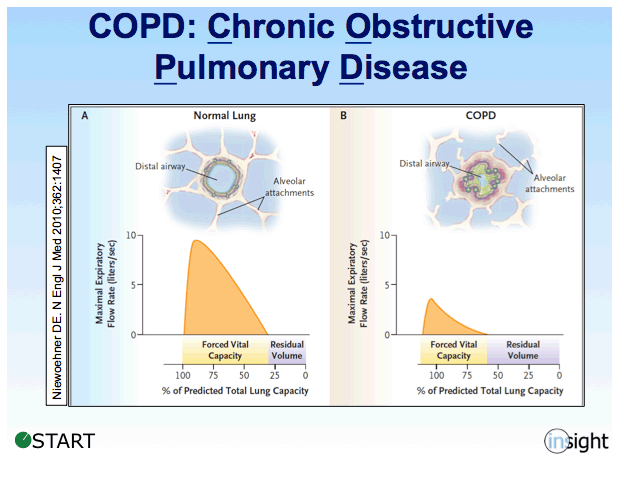
The exact mechanism for why people with COPD have an increased risk of developing hypertension is not completely clear, but chronically low oxygen levels appear to be a factor. COPD causes impaired gas exchange in the lungs, limiting oxygen intake and carbon dioxide release. This leads to decreased blood oxygen levels in the body.
Why are CO2 levels high in people with COPD?
Patients with late-stage chronic obstructive pulmonary disease (COPD) are prone to CO2 retention, a condition which has been often attributed to increased ventilation-perfusion mismatch particularly during oxygen therapy. How does COPD affect CO2? COPD patients have a reduced ability to exhale carbon dioxide adequately, which leads to hypercapnia.
What is the normal oxygen level for someone with COPD?
A normal oxygen level for a patient suffering from COPD is between 95 and 100 percent, according to About.com. Although some people are able to function normally with an oxygen level as low as 90 percent, a doctor should always be consulted with regard to optimal saturation level. When the oxygen level falls below normal values, a person should ...
What does an elevated CO2 level mean?
Share on Pinterest A higher-than-normal CO2 level can indicate a breathing disorder. An abnormal CO2 test result could mean that there are either high or low CO2 levels in the body. Changes in CO2 levels may suggest that someone is losing or retaining normal body fluids.
What causes high levels of CO2 in the body?
What Causes High Levels of CO2 in the Blood? Causes of high levels of carbon dioxide in the blood include vomiting, dehydration and overuse of bicarbonate medicine such as antacids, according to WebMD.
See more
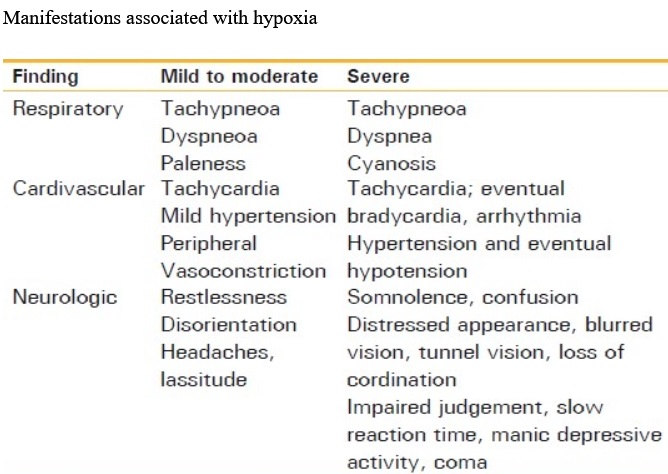
What is normal CO2 for COPD?
Normal values are between 7.38 and 7.42. The acidity or alkalinity of the blood is linked with the amount of carbon dioxide in the blood. Acidic blood (pH less than 7.38) has high carbon dioxide levels in the blood.
Do all COPD patients retain CO2?
Patients with late-stage chronic obstructive pulmonary disease (COPD) are prone to CO2 retention, a condition which has been often attributed to increased ventilation-perfusion mismatch particularly during oxygen therapy.
Does COPD increase CO2?
Acute exacerbation of COPD is a common reason for adult hospital admissions, with some of the highest costs attributed to patients with COPD admitted to the intensive care unit (ICU), with an elevated partial pressure of carbon dioxide in arterial blood (PaCO2).
Why is CO2 decreased in emphysema?
Emphysema destroys the walls between the alveoli. This leaves the lungs less able to absorb oxygen into the bloodstream and remove carbon dioxide from the blood.
What are the signs that COPD is getting worse?
The following are signs that may indicate that a person's COPD is getting worse.Increased Shortness of Breath. ... Wheezing. ... Changes in Phlegm. ... Worsening Cough. ... Fatigue and Muscle Weakness. ... Edema. ... Feeling Groggy When You Wake Up.
How is low CO2 treated?
Some studies show that treatment with sodium bicarbonate or sodium citrate pills can help improve metabolic acidosis. Eating more fruits and vegetables (and fewer meats, eggs, cheese and cereal grains) can also help. Talk to your healthcare provider about the safest ways to balance the CO2 levels in your blood.
What causes low carbon dioxide?
A low CO2 level can be a sign of several conditions, including: Kidney disease. Diabetic ketoacidosis, which happens when your body's blood acid level goes up because it doesn't have enough insulin to digest sugars. Metabolic acidosis, which means your body makes too much acid.
Can you have COPD with normal oxygen levels?
Because of that, people with COPD may be relying as much on their oximetry results as their actual symptoms when evaluating their breathing status. And that can cause confusion. The reason is that you can have "normal" oxygen saturation levels while feeling extremely short of breath.
At what stage of COPD do you need oxygen?
Supplemental oxygen is typically needed if you have end-stage COPD (stage 4). The use of any of these treatments is likely to increase significantly from stage 1 (mild COPD) to stage 4.
What is the last stage of COPD?
End-stage, or stage 4, COPD is the final stage of chronic obstructive pulmonary disease. Most people reach it after years of living with the disease and the lung damage it causes. As a result, your quality of life is low. You'll have frequent exacerbations, or flares -- one of which could be fatal.
What are the final stages of COPD before death?
Still, signs that you're nearing the end include:Breathlessness even at rest.Cooking, getting dressed, and other daily tasks get more and more difficult.Unplanned weight loss.More emergency room visits and hospital stays.Right-sided heart failure due to COPD.
How long does a COPD flare up last?
Chronic obstructive pulmonary disease (COPD) exacerbations may last for two days or even two weeks, depending on the severity of the symptoms. Sometimes, COPD exacerbations may require antibiotics, oral corticosteroids and hospitalization.
How do you know if you are retaining CO2?
Symptoms of HypercapniaAnxiety.Shortness of breath.Daytime sluggishness.Headache.Daytime sleepiness even when you slept a lot at night (your doctor might call this hypersomnolence)
How can you prevent CO2 retention?
Options include:Ventilation. There are two types of ventilation used for hypercapnia: ... Medication. Certain medications can assist breathing, such as:Oxygen therapy. People who undergo oxygen therapy regularly use a device to deliver oxygen to the lungs. ... Lifestyle changes. ... Surgery.
Why do COPD patients retain CO2 when given too much oxygen?
Patients with late-stage chronic obstructive pulmonary disease (COPD) are prone to CO2 retention, a condition which has been often attributed to increased ventilation-perfusion mismatch particularly during oxygen therapy.
What causes you to retain CO2?
Metabolic Changes Illnesses, infections, and severe trauma can cause an alteration in the body's metabolism, resulting in excess CO2 production. If your breathing can't catch up with your need to exhale CO2 from your body, you can develop an elevated blood CO2 level.
What are the factors that affect COPD?
Several key factors affect the outlook for a person with COPD, including: 1 age 2 body mass index ( BMI) 3 how often they experience COPD flares 4 level of breathlessness after physical activity 5 degree of hypoxemia 6 pulmonary artery pressures 7 results of a pulmonary function test 8 resting heart rate 9 smoking status 10 other health conditions unrelated to the lungs
How does COPD affect the body?
COPD can have harmful effects on the body when it interferes with oxygen levels. If hypoxia progresses too far, it can lead to disability and death. Oxygen passes into the blood from lung tissue through the alveoli, or air sacs. Oxygenated blood then leaves the lungs and travels around the body to other tissues.
What happens when oxygen is lost in the lungs?
Oxygenated blood then leaves the lungs and travels around the body to other tissues. Vital organs and systems, especially the brain and heart, need enough oxygen to survive. COPD damages the air sacs in the lungs and interferes with this process. If the damage reaches a critical point, a person may develop hypoxia.
What is the best treatment for COPD?
Along with nutritional counseling, pulmonary rehabilitation therapy can help a person with COPD improve their breathing and oxygen levels around the body. If a person has severe hypoxemia due to COPD, a doctor will commonly recommend oxygen therapy.
What is the name of the condition that affects breathing?
Chronic obstructive pulmonary disease, or COPD, is a name for several conditions that affect breathing, including chronic bronchitis and emphysema. Hypoxia is one of the harmful effects of COPD when not enough oxygen moves around the body, impacting organ function. COPD occurs when obstructions block the flow of air through the lungs.
How does COPD happen?
COPD occurs when obstructions block the flow of air through the lungs. Over time, inflammation and damage in the lungs become progressively worse. According to the Centers for Disease Control and Prevention (CDC), around 16 million people. Trusted Source.
What are some examples of chronic lack of oxygen?
A chronic lack of oxygen can cause inflammation in the body’s tissues, which can lead to several conditions. Examples include atherosclerosis, which makes the arteries harden. Atherosclerosis increases the risk of heart disease, heart attack, and stroke. Read more on atherosclerosis.
What is the best way to manage COPD?
The complex management of COPD involves patient education, self-management, and pulmonary rehabilitation in addition to the above. Physicians and respiratory therapists assist with patient education, which primarily includes behavior/lifestyle modification, for example, smoking cessation, education about symptoms of COPD exacerbation, the importance of regular medications, and the proper use of prescribed medications. Self-management plan includes taking medications regularly, awareness of severe symptoms, and learning to live with their disease. Pulmonary rehabilitation is also an important intervention that improves dyspnea and exercises tolerance, and substantially reduces hospital admission rates. A physiotherapist can assist in pulmonary rehabilitation programs to help with exercise and overall conditioning. The nurse can assist with patient monitoring, education, and coordination of follow-up care. The pharmacist can help avoid drug-drug interactions and make recommendations in regards to appropriate therapy and dosing. Dieticians can assist patients who are overweight or underweight. Family physicians play an important role in discussing end-of-life and palliative care with the patients.
How does COPD maintain the V/Q ratio?
Therefore, the body tries to maintain the V/Q ratio by localized vasoconstriction in the affected lung areas that are not oxygenated well.
How long does it take for a COPD patient to recover from acidosis?
It usually takes about 3 to 5 days for the maximum response. This helps in maintaining acid-base balance near normal and prevents the pH from becoming dangerously low. [15]
Which organs are responsible for maintaining pH in COPD patients?
Renal compensation to maintain near-normal pH in COPD patients [12]: The lungs and the kidneys are the key organs responsible for keeping our body’s pH in balance. In COPD patients, kidneys compensate by retaining bicarbonate to neutralize pH.
Is COPD a complex disease?
COPD is a complex disease and a cause of significant morbidity and mortality. It requires interprofessional care and the involvement of more than one subspecialties. This patient-centered approach involving a physician with a team of other health professionals, physiotherapists, respiratory therapists, dieticians, social workers, clinical psychologists, nurses, and support groups working together for the patient plays an important role in improving the quality of care in COPD patients. It not only decreases the hospital admission rates but also positively affects the disease outcome.
Does COPD cause acidosis?
In COPD patients, chronically elevated carbon dioxide shifts the normal acid-base balance toward acidic .[13] There is the retention of carbon dioxide, which is hydrated to form carbonic acid. Carbonic acid is a weak and volatile acid that quickly dissociates to form hydrogen and bicarbonate ions. This results in respiratory acidosis. This primary event is characterized by increased pCO2 and a fall in pH on arterial blood gas analysis.
Does smoking cause COPD?
Tobacco smoking accounts for most cases of COPD in developed nations. The severity of the disease depends on the number of pack-years smoked and the duration of smoking. This leads to progressive loss of lung function due to damage of air sacs.
Hyperventilation
Hyperventilation — breathing too rapidly or deeply than your body requires — is a leading cause of a low blood CO 2 level. When you hyperventilate, you exhale too much CO 2 causing a drop in your blood level. Hyperventilation triggered by severe pain, overwhelming fear or anxiety, or a panic attack can cause a short-term dip in your CO 2 level.
Excess Blood Acids
Excess acids in your bloodstream drive down your blood CO 2 level. This occurs with conditions that increase acid production in your body and with ingestion of certain types of medications or toxic substances. Examples include:
Excess Bicarbonate Loss
You might recall from a high school or college chemistry class that a buffer system refers to dissolved chemicals that help maintain a relatively constant pH. Bicarbonate in your body serves as potent buffer that helps keep your blood pH stable.
What It Feels Like
A sudden drop in your blood CO 2 level due to hyperventilation typically causes an array of symptoms, including lightheadedness, tingling in your arms and legs and around your mouth, foggy thinking, and possibly fainting.
What does low CO2 mean?
As discussed so far, low CO2 levels may indicate problems with acid-base balance in the blood, which may require urgent medical attention. In the section below, we’ll discuss the health risks of chronically low CO2 levels, according to research. However, low CO2 levels do not always indicate that there is a problem.
What to do if CO2 is low?
If your CO2 levels are too low, the first step your doctor will take is treating the underlying condition that is causing the imbalance. This could mean anything from treating possible kidney or lung issues to stopping certain medications [ 2 ].
How to reduce carbon dioxide levels?
Maintaining Carbon Dioxide Levels 1 Drink plenty of water, dehydration is a common cause of metabolic acidosis [ 11] 2 Limit alcohol consumption, drinking too much can lead to metabolic acidosis [ 12] 3 Keep diabetes well controlled [ 13] 4 Breathing exercises (like yoga breathing, Buteyko breathing) and relaxation techniques may help with hyperventilation for those with anxiety [ 14, 15]
What are the effects of carbon dioxide on the body?
3) Connections to Anxiety and Panic Disorder. Maintaining Carbon Dioxide Levels. Learn More. Takeaway. Carbon dioxide is in the air, in the ocean, and even in soda. In your body, carbon dioxide controls breathing and maintains the pH of your blood.
How is carbon dioxide created?
Most of the carbon dioxide (CO 2) in the body is created as a byproduct by cells when they convert sugars and fats into energy . This provides a steady source of CO 2, which then leaves the body whenever a person breathes out [ 1, 2 ].
What are the symptoms of respiratory alkalosis?
Some symptoms of respiratory alkalosis include irregular heart rhythm, sweating, and convulsions [ 6 ].
What are the symptoms of metabolic acidosis?
Symptoms of metabolic acidosis vary greatly depending on the underlying cause and may include headache, confusion, anxiety, and coma [ 3, 4 ].
Symptoms
Chronic obstructive pulmonary disease may cause the following respiratory symptoms:
Causes
Most cases of COPD are due to exposure to tobacco smoke or other lung irritants, such as:
Receiving a prescription for oxygen treatment
A person who is just starting oxygen treatment will require tests from their doctor. The tests will determine how much oxygen is in the person’s blood while they are resting and moving. Doctors will use the results of these tests to prescribe an appropriate type and level of oxygen treatment.
What test is used to measure oxygen and carbon dioxide levels in the blood?
Or you might need a tube that goes into your airway and connects to a machine that helps you breathe (ventilation). Order blood tests: Arterial blood gas test: This test measures the oxygen and carbon dioxide levels in your blood. The doctor will take some blood from an artery, usually in your wrist.
What happens if you don't treat hypercapnia?
Acute hypercapnia is a life-threatening emergency. If you don't treat it promptly, you could stop breathing, have a seizure, or go into a coma.
What Happens When You Have Hypercapnia?
Hypercapnia changes the pH balance of your blood, making it too acidic. This can happen slowly or suddenly. If it happens slowly, your body may be able to keep up by making your kidneys work harder. Your kidneys release and reabsorb bicarbonate, a form of carbon dioxide, which helps keep your body's pH level balanced.
What is hypercapnia in the blood?
What is Hypercapnia? Hypercapnia is a buildup of carbon dioxide in your bloodstream. It affects people who have chronic obstructive pulmonary disease (COPD).
What to do if you take supplemental oxygen?
You can use it to make sure your oxygen levels aren't getting too high, which raises your odds of getting hypercapnia.
Can hypercapnia cause a coma?
If untreated, it can eventually lead to a coma. Severe hypercapnia can involve: Hand tremors (asterixis) Sudden brief muscle jerks (myoclonus) Seizures. Pressure in your brain ( papilledema) that makes your optic nerve swell and can lead to: Headaches. Nausea. Trouble seeing.
Can you get hypercapnia from sedatives?
You could also get acute hypercapnia if you start taking a medicine that makes you sleepy, like a narcotic pain reliever, after an injury or surgery. These drugs, known as sedatives, can slow down your rate of breathing. Acute hypercapnia is a life-threatening emergency.
Why Do Patients With COPD Develop Anemia?
Researchers believe COPD precipitates the development of anemia by several means. Chronic inflammation and an altered immune response appear to be involved.
Why is iron not available in COPD?
It remains in tissues, rather than circulating and carrying oxygen. If you have COPD, difficulty breathing and fatigue may prevent you from eating an adequate diet, so you may not consume the iron-rich foods your body needs.
What is the best medicine for COPD?
Some medications commonly used to treat COPD are known to cause anemia, such as theophylline and ACE inhibitors. The ophylline is commonly prescribed as a breathing aid, and ACE inhibitors are used to relieve the cardiac problems many sufferers of COPD have. Many people who have COPD also have kidney problems.
What foods can you eat to help with COPD?
The best sources of iron include oysters, organ meats, dark green leafy vegetables, blackstrap molasses, dried fruits, whole grains, egg yolks, dried peas and dried beans. Much remains to be learned about the relationship between anemia and COPD. What is known is that both conditions have the ability to affect your entire ...
Does bone marrow help with COPD?
The bone marrow speeds up the production of red blood cells when a lack is sensed by the body, but this ability is impaired among individuals who have COPD. The body cannot keep up with the ongoing demand for rapidly produced red blood cells, so anemia ensues. The iron needed by your body may not be as available when COPD is present.
Can COPD cause kidney problems?
Many people who have COPD also have kidney problems. This can affect hormones needed to maintain healthy blood cells and oxygen levels throughout the body, resulting in anemia.
Is COPD anemic or anemic?
People who suffer from chronic obstructive pulmonary disease (COPD) are more likely to be anemic when compared with the rest of the population. Let’s take a look at why anemia and COPD are linked, and what you can do to prevent anemia and the complications it causes. Anemia is a deficiency in the number of red blood cells or a decrease in ...