What is the function of mucosal tissues?
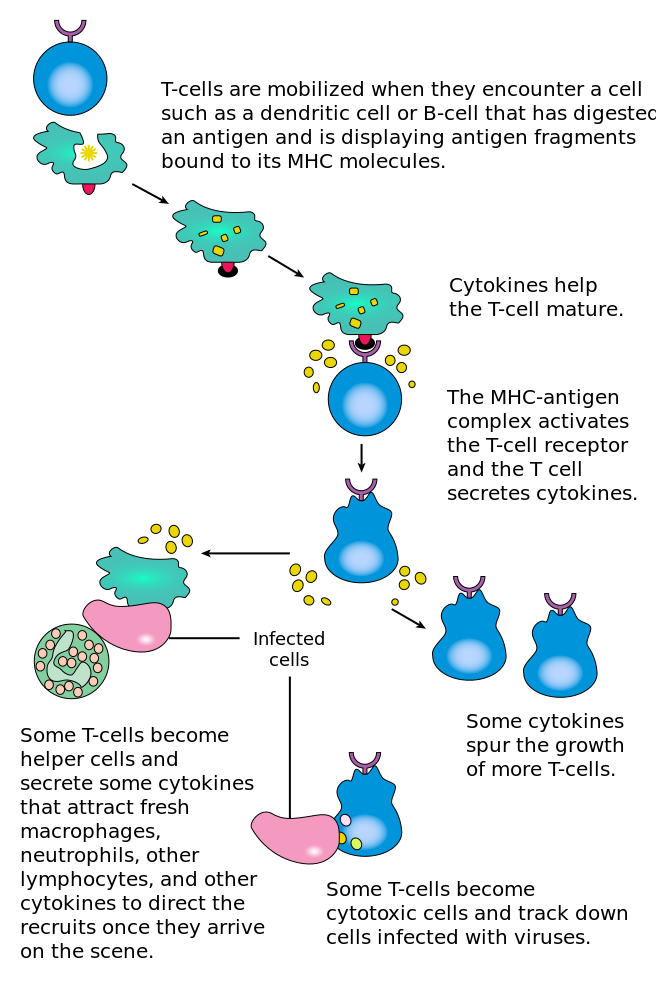
C.J. Field, in Encyclopedia of Food Sciences and Nutrition (Second Edition), 2003 Mucosal tissues (contain components of both the innate and acquired immune system) are strategically located in areas where external pathogens enter the body. Immune cells that reside in mucosal tissues protect against the entry of infectious agents.
What is the function of mucous cells in the stomach?
Mucous cells are located on the surface and in the neck of the gastric glands (GGs). SMs that line the stomach lumen and the GPs have a columnar shape and secrete an alkaline, highly viscous mucous substance rich in bicarbonate ions that helps to protect the stomach mucosa from abrasive food particles and erosive gastric acid.
What is the function of mucous membrane?
Mucous membrane, membrane lining body cavities and canals that lead to the outside, chiefly the respiratory, digestive, and urogenital tracts.
What is the mucosal associated lymphoid tissue?
The Mucosal Associated Lymphoid Tissue. Mucosal tissues (contain components of both the innate and acquired immune system) are strategically located in areas where external pathogens enter the body. Immune cells that reside in mucosal tissues protect against the entry of infectious agents.
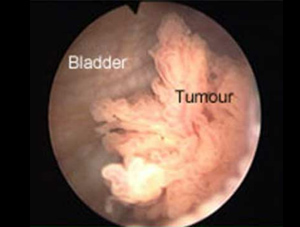
Why do we need mucous cells in our stomach?
The mucus layer is the first line of defense against infiltration of microorganisms, digestive enzymes and acids, digested food particles, microbial by-products, and food-associated toxins.
What type of cells are mucosal cells?
The mucosa is composed of one or more layers of epithelial cells that secrete mucus, and an underlying lamina propria of loose connective tissue.
Where are mucous cells found?
Mucus is produced by mucous cells, which are frequently clustered into small glands located on the mucous membrane that lines virtually the entire digestive tract. Large numbers of mucous cells occur in the mouth, where mucus is used both to moisten food and to keep the oral membranes moist…
What does the mucosa mean?
(myoo-KOH-suh) The moist, inner lining of some organs and body cavities (such as the nose, mouth, lungs, and stomach). Glands in the mucosa make mucus (a thick, slippery fluid). Also called mucous membrane.
What are the 4 types of cells in the stomach?
Four different types of cells make up the gastric glands:Mucous cells.Parietal cells.Chief cells.Endocrine cells.
What are the mucosal tissues?
Mucosa is the soft tissue that lines the body's canals and organs in the digestive, respiratory and reproductive systems. It's also called the mucous membrane. Mucosa has three layers: epithelium, lamina propria and muscularis mucosae. It plays an important part in immunity.
What type of cell is a stomach cell?
Parietal cells (also called oxyntic cells) are the stomach epithelium cells which secrete gastric acid.
What is the mucosa layer made of?
The mucosa consists of epithelium, an underlying loose connective tissue layer called lamina propria, and a thin layer of smooth muscle called the muscularis mucosa. In certain regions, the mucosa develops folds that increase the surface area. Certain cells in the mucosa secrete mucus, digestive enzymes, and hormones.
What is the apex of a mucous cell?
Mucous Cells. Mucous cells (Figs. 1B and 2B) are large cells shaped like a truncated pyramid. The apex of the cell has a larger lumenal surface than serous cells, but intercellular canaliculi usually are not present between mucous cells. They are joined to their neighbors by junctional complexes and gap junctions.
Which cells have a thin mucoid glycocalyx?
Apart from the mucus secreted by mucous cells in the surface epithelium and submucosal glands (see below), non-secretory cells such as the ciliated cells have a thin mucoid glycocalyx forming the outer part of their cell membrane. 57 This differs chemically from the main mucous lining and is probably formed by the cell of which it forms the outermost part. The glycocalyx of the cilia differs chemically from that of the microvilli on the same cell, whilst in the alveolus, different lining cells have chemically different forms of glycocalyx. 65
What are mucins in the respiratory tract?
Mucins are high-molecular-weight glycoproteins in which oligosaccharide side chains are attached to an elongated protein core. 57 The mucous granules of the surface mucous cells contain an acidic mucin, with sialic acid or sulphate groups at the end of the oligosaccharide side chains of the peptide core. The amount and viscoelasticity of the mucus are important to airway clearance and the chemical structure of the mucus probably influences its physical properties and hence the ease with which it is cleared by ciliary activity or coughing. Out of the nine different mucin genes identified in human tissues, seven are expressed in the respiratory tract: MUC1–MUC4, MUC5AC, MUC5B and MUC7. 58,59 While MUC5B and MUC7 expression is predominantly restricted to cells of the submucosal glands, 60 MUC2 and MUC5AC mucins are located more in the surface epithelium. 61 The predominant components of respiratory mucus are MUC5AC and MUC5B, 62 and these are upregulated by various stimuli such as air pollutants or bacteria and also in asthma and cystic fibrosis. 63,64 The number of mucous cells increases in response to irritation. This also induces inflammation and, although the viscosity of mucus is primarily dependent on its glycoprotein content, it is markedly augmented by DNA released from effete inflammatory cells. It is impossible to state at exactly what point goblet cell hyperplasia begins as numbers vary dependent on the site of the biopsy, but a crude figure is more than 3 per 10 cells at any point in the respiratory tract.
What is the role of eosinophils in the production of mucus?
Role of Eosinophils in the Production of Mucus. Intestinal mucus barriers are the first line of defense against a wide range of potentially damaging agents of microbial, endogenous, and dietary origins that the intestinal epithelia may encounter.
What is the apical cytoplasm?
The apical cytoplasm contains mucous secretory granules that typically are irregular in shape and have a pale content, with some fine granular or filamentous material. The membranes of the granules often are disrupted and/or fused with those of adjacent granules.
What percentage of the acinar volume is mucous?
Mucous cells in the submandibular gland most often occupy <10% of the total acinar volume, although the proportion of mucous cells can vary between 1% and 33%. The appearance of mucous acini with serous demilunes has been well known since the 19th century (Fig. 5.1 ). However, this reproducible picture is a reproducible artifact caused by conventional fixation. The method of rapid freezing and freeze-substitution has revealed that in reality, all the serous cells align with mucous cells to surround a common lumen, leaving no demilune structure, whereas samples fixed by conventional methods result in greatly distended mucous cells that displace the serous cells towards the basal portion of the acinus to form the demilune structure. 8 The mucous secretory granules expand in conventional fixation, which accounts for the distended mucous cell with distorted nucleus displaced to the base. Nevertheless, only conventional fixation with formaldehyde is feasible routinely, and it has the advantage of producing a reproducible picture, which is of value in diagnostic histopathology.
How much of a tumor is mucous?
In many tumors, they outnumber other cell types. Mucous cells rarely constitute as much as 10% of a tumor, and identification often requires special histochemical stains, such as mucicarmine. Epidermoid differentiation is often focal, and distinct keratinization is rare.
Why is mucosal tissue important?
Immunization of mucosal tissues has the advantage of depositing the vaccine into or close to the primary site or route of infection for some pathogens, resulting in more natural cellular and humoral responses such as IgA secretion.70 A key benefit of the mucosal, and specifically oral, route is that these are much easier to administer than any parenterally administered vaccine and thus are less likely to transmit any blood-borne diseases. 71
Where are mucosal lymphoid tissues located?
Mucosal tissues (contain components of both the innate and acquired immune system) are strategically located in areas where external pathogens enter the body. Immune cells that reside in mucosal tissues protect against the entry of infectious agents.
What are DCs in the body?
DCs in spleen, peripheral organs, and LNs capture and process antigens to induce and direct primary T and B cell response s. In the thymus and periphery, DCs also select the repertoire of T cells and determine the induction of regulatory immune responses by T and B cells. Originally considered to be one homogenous cell population, it is now clear that there are different subsets of DCs, each with clearly distinct functional properties in immunity and tolerance induction. Broadly speaking, DCs in mouse and human are divided first in conventional (cDC), plasmacytoid (pDC), and monocyte-derived (moDC) subsets. Subpopulations of DCs have been defined based on unique surface marker expression, localization, gene expression, and functional analysis in vitro and in vivo. cDCs, which include the majority of tissue and resident DCs, can be clearly distinguished from pDCs, which are not DCs per se, but plasmacytoid-shaped cells, which on activation with viruses or nucleic acids produce high amounts of type 1 interferon and then differentiate into antigen-presenting DCs. Only recently have the precise developmental pathways, lineage-defining transcription factors, and transcriptional profiles defining DCs and macrophages been identified ( Gautier et al., 2012; Merad et al., 2013; Segura et al., 2013 ). This has led to tools to specifically address the function of DC subsets and macrophages in mucosal immunity.
What are the major portals of entry for microbes and environmental antigens?
Mucosal tissues, such as the nose and lung and gut and genitourinary tract , constitute major portals of entry for microbes and environmental antigens. Multiple dendritic cell (DC) populations have been defined largely in mice by their cellular origin, maturation pathways, surface phenotypes, and tissue-specific immune functions that appear to have functional equivalents in humans. DC populations have distinct anatomical locations, capture antigens and microbes by different mechanisms, and unique immunological functions under steady-state, infectious, and inflammatory conditions. Furthermore, recent studies have begun to provide insight into the fundamental role of DC populations in the pathogenesis of inflammatory and allergic disease, such as Crohn's disease and asthma. This chapter provides a discussion of general aspects of DC biology, followed by summaries of studies indicating that DC populations play primary roles in maintaining the balance among tolerance, immunity, and control of barrier function in the gastrointestinal, pulmonary, and genitourinary tracts.
Where are lymphocytes found in the nasal cavity?
Lymphocytes are found in the nasal mucosa, the lateral nasal glands and their secretory ducts. In the nasal cavity, lymphocytes are primarily present in, or below, the respiratory epithelium and are relatively infrequent in the vestibular region at the nasal entrance and in the olfactory region [41]. While CD8 + cells are distributed in the epithelium and the lamina propria, CD4 + T cells are largely confined to organized lymphoid structures that develop in the subepithelial layer. These structures are called the nasal-associated lymphoid tissue (NALT) [41] and are considered to be part of a common mucosal immune system, as defined for several mammalian species [42]. The major characteristics of chicken NALT are the formation of circumscribed B cell areas, occasionally displaying GC, that are covered by a cap of CD4 + T cells. The surface of these lymphoid follicles is covered by a non-ciliated epithelium. Ig + B cells are found within the NALT structures and distributed throughout the epithelium, similarly to the CD8 + cells. The dominant Ig isotype in both locations is IgY, whereas IgM + cells are less frequent and IgA + cells are relatively rare [41].
Why is the gastrointestinal system important?
The gastrointestinal system serves as a primary reservoir for bacteria that have the potential, if not properly controlled, to induce life-threatening infections.
What is the reproductive tract?
Unlike other mucosal tissues, the reproductive tract is characterized by progressive tissue growth and remodeling, which occurs during each menstrual cycle and the sloughing off of the outer two-thirds of the uterine mucosa during menses.
Which mucosa cells release histamine in response to gastrin and other stimuli?
Gastric fundic mucosa cells that release histamine in response to gastrin and other stimuli.
What are the factors that affect the oral mucosa?
Three essential factors are known to be necessary to engineer human oral mucosa: cells; an extracellular matrix (ECM); and cytokines [ 3 ]. Recently, in addition to these, vascularization and time can be considered as other critical factors [ 9 ]. Similar to skin TE, the essential goals of oral mucosa TE are the duplication of anatomic structures and physiologic functions to emulate restoration of the epithelial barrier, effective wound healing, and lack of host toxicity or immune rejection. In full-thickness mucosa damage, replacement of the epithelial and underlying connective tissues is the preferred approach, which can minimize scarring and restore acceptable function and cosmetics [ 5, 10 ]. Therefore, the composite grafts of oral mucosa substitutes should be biodegradable and non-toxic, have sufficient physical properties of strength, have a compliance and density similar to oral mucosa, be capable of promoting cell attachment, be remodelable by host and/or grafted tissue cells, have low immunogenicity, be suturable, be a suitable substrate for ECM formation, and encourage neovascularization [ 6, 11 ].
What is the mucosal immune system?
The immune system may be viewed as an organ that is distributed throughout the body to provide host defense against pathogens wherever these may enter or spread. Within the immune system, a series of anatomically distinct compartments can be distinguished, ...
Which receptors are bound by lymphocytes?
The second is that lymphocytes are restricted to particular compartments by expression of homing receptors that are bound by ligands, known as addressins, that are specifically expressed within the tissues of the compartment.
Where are epithelial mucous surface cells located?
Epithelial mucous surface cells (A) extend into the gastric pits (B) of the mucosal lining in the lumen of the stomach (C, gastric glands; D , muscularis mucosa of the stomach). With rare exception, pathogenic organisms cannot penetrate the intact covering and linings of the body. Indeed, if one were to take samples...
What is the main substance secreted from the mucous membrane?
The term mucous membrane comes from the fact that the major substance secreted from the membranes is mucus; the principal constituent of mucus is a mucopolysaccharide called mucin. Surface mucous cell on the stomach lumen secreting mucus (pink stain). Underwood J (2006) The Path to Digestion Is Paved with Repair.
What is the membrane that lines the mouth, nose, eyelids, trachea, and lungs?
Mucous membrane, membrane lining body cavities and canals that lead to the outside, chiefly the respiratory, digestive, and urogenital tracts. Mucous membranes line many tracts and structures of the body, including the mouth, nose, eyelids, trachea (windpipe) and lungs, stomach and intestines, and the ureters, urethra, and urinary bladder.
What is the epithelium tough?
These types of epithelium are notably tough—able to endure abrasion and other forms of wear that are associated with exposure to external factors (e.g., food particles). They also typically contain cells specially adapted for absorption and secretion.
Which layer of the respiratory tract is a mechanical barrier?
Like the outer layer of the skin but much softer, the mucous membrane linings of the respiratory, gastrointestinal, and genitourinary tracts provide a mechanical barrier of cells that are constantly being renewed. The lining of the respiratory tract has cells that secrete mucus…
Can pathogenic organisms penetrate the lining of the body?
With rare exception, pathogenic organisms cannot penetrate the intact covering and linings of the body. Indeed, if one were to take samples... Mucous membranes vary in structure, but they all have a surface layer of epithelial cells over a deeper layer of connective tissue.
Where are mucoid cells located?
(2) Zymogenic, or chief, cells are located predominantly in gastric glands in the body and fundic portions of the stomach.
What type of cells secrete gastric mucus?
In addition to the tall columnar surface epithelial cells mentioned above, there are five common cell types found in the various gastric glands. (1) Mucoid cells secrete gastric mucus and are common to all types of gastric glands.
How many glands are there in the stomach?
Three to seven individual gastric glands empty their secretions into each gastric pit. Beneath the gastric mucosa is a thin layer of smooth muscle called the muscularis mucosae, and below this, in turn, is loose connective tissue, the submucosa, which attaches the gastric mucosa to the muscles in the walls of the stomach.
What is the inner surface of the stomach covered by?
The inner surface of the stomach is lined by a mucous membrane known as the gastric mucosa. The mucosa is always covered by a layer of thick mucus that is secreted by tall columnar epithelial cells.
Which cells are responsible for gastric acid secretion?
Those stimuli that cause gastric acid secretion—in particular, vagal nerve stimulation—also promote the secretion of the pepsinogens. (3) Gastrin cells, also called G cells, are located throughout the antrum.
What is the protective layer of the stomach?
This protective layer is a defense mechanism the stomach has against being digested by its own protein-lyzing enzymes, and it is facilitated by the secretion of bicarbonate into the surface layer from the underlying mucosa.
Which cells produce the most water?
Parietal cells produce most of the water found in gastric juice; they also produce glycoproteins called intrinsic factor, which are essential to the maturation of red blood cells, vitamin B 12 absorption, and the health of certain cells in the central and peripheral nervous systems.
How long does mucosal melanoma last?
The survival rate of mucosal melanoma is based on those that survive a minimum of 5 years after they are diagnosed. The survival rate also varies by the location of the mucosal melanoma.
Why is the staging for the progression of mucosal melanoma vague?
Mucosal melanoma staging. The staging for the progression of mucosal melanoma is vague because of how rare this type of melanoma is. The staging and survival rates vary based on the location of the mucosal melanoma.
What classification is used for mucosal melanoma of the head and neck?
Staging for mucosal melanoma of the head and neck as well as vulval melanomas use the AJCC-TNM (The American Joint Committee on Cancer — Tumor, Node, and Metastasis) classification.
Why is mucosal melanoma considered aggressive?
Mucosal melanoma is considered an aggressive form of melanoma. It’s considered aggressive because it’s usually not discovered until it’s already in an advanced stage. By the time it enters the advanced stages, the treatment options are limited. It also usually moves into metastasis soon after diagnosis.
What is the primary complication of mucosal melanoma?
The primary complication of mucosal melanoma occurs when it moves into the distant metastasis stage. At this stage, there are very few treatment options available. The survival rate also becomes very low. Other complications are due to the lack of early detection and diagnosis.
What are the risk factors for mucosal melanoma?
Some possible risk factors for mucosal melanoma may include: In the areas in or near the mouth: dentures that don’t fit properly. smoking. carcinogens in the environment that have been inhaled or ingested.
Can UV rays cause mucosal melanoma?
Mucosal melanoma is not caused by exposure to UV rays like other melanomas. Most people with mucosal melanoma are over the age of 65, and the risk increases as age increases. The specific cause is still unknown since this type of melanoma is rare.