
What are the functions of mineralocorticoids and glucocorticoids?
Locally synthesized glucocorticoids regulate activation of immune cells, while locally synthesized mineralocorticoids regulate blood volume and pressure.
What is the function of mineralocorticoids and from where are they secreted?
Mineralocorticoids are a class of corticosteroids, which in turn are a class of steroid hormones. Mineralocorticoids are produced in the adrenal cortex and influence salt and water balances (electrolyte balance and fluid balance). The primary mineralocorticoid is aldosterone.
Do mineralocorticoids increase blood pressure?
Reduced cortisol causes elevated ACTH and overproduction of aldosterone causes suppression of renin. Clincial manifestations are secondary to the overproduction or deficiency of metabolites. Mineralcorticoid overactivity causes hypertension, salt retention, and hypokalemia with suppression of plasma renin.
Is cortisol a mineralocorticoid?
Cortisol has significant mineralocorticoid activity. Approximately 20 mg of cortisol or cortisone intravenously has a mineralocorticoid action equivalent to 0.1 mg of 9α-fluorocortisol.
What is the function of the mineralocorticoids secreted by the adrenal gland quizlet?
mineralocorticoid hormone secreted by the adrenal cortex to increase sodium reabsorption by the kidneys and indirectly regulate blood levels of potassium, sodium, and bicarbonate; also regulates pH, blood volume, and blood pressure.
Where is mineralocorticoid found in the body?
Mineralocorticoid receptors (MR) bind both mineralocorticoids and glucocorticoids with high affinity (deoxycorticosterone = corticosterone >/= aldosterone = cortisol), and are found in both Na(+) transporting epithelia (e.g. kidney, colon) and nonepithelial tissues (e.g. heart, brain).
Which part the adrenal gland secretes mineralocorticoids?
(i) Mineralocorticoids are secreted by Zona Fasciulata. (ii) Zona Glomerulosa regulates the balance of water and Na+2. (iii) Sex corticoids are secreted by both Zona Fasciculata and Zona Reticularis.
What are the roles of mineralocorticoids in the body?
Mineralocorticoids play a critical role in regulating concentrations of minerals – particularly sodium and potassium – in extracellular fluids to influence salt and water balances (electrolyte balance and fluid balance).
What is it called when the adrenal gland releases too much aldosterone into the blood?
Hyperaldosteronism is a disorder in which the adrenal gland releases too much of the hormone aldosterone into the blood.
How does cortisol affect the body?
Cortisol also known as hydrocortisone, is the major glucocorticoid and increases in response to stress which activates the hypothalamic-pituitary-adrenal (HPA) axis axis. Therefore, all of its functions can be thought of as allowing the body to function with increased stress. Upon engaging glucocorticoid receptors, cortisol increases the expression of genes that will regulate metabolism, the immune system, cardiovascular function, growth, and reproduction. Cortisol is essential for maintaining blood pressure because it increases the sensitivity of vascular smooth muscle to vasoconstrictors like catecholamines and suppresses the release of vasodilators like nitrous oxide 34). Cortisol suppresses the immune system, which is the basis for immunosuppressive drug therapy with glucocorticoids. Regarding metabolism, cortisol increases gluconeogenesis and decreases peripheral glucose uptake. These oppose the actions of insulin, and the net effect is an increase in serum glucose. Cortisol also activates lipolysis and stimulates adipocyte growth, which leads to fat deposition. Generally, growth is inhibited, leading to muscle atrophy, increased bone resorption, and thinning of the skin. Of note, glucocorticoids can act on mineralocorticoid receptors. However, aldosterone effects predominate in the kidney because the renal enzyme, 11-beta-hydroxysteroid dehydrogenase-2 converts cortisol to cortisone 35). The 11-beta-hydroxysteroid dehydrogenase-1 converts cortisone into cortisol. Hence, these enzymes add another layer of regulation to cortisol. Licorice toxicity inhibits 11-beta-hydroxysteroid dehydrogenase-2, causing hypertension and hypokalemic alkalosis with normal aldosterone levels. Also, there can be a loss of function mutations in 11-beta-hydroxysteroid dehydrogenase-2, resulting in hypertension with low aldosterone 36).
Why does hyperaldosteronism cause high blood pressure?
Primary hyperaldosteronism is due to a problem of the adrenal glands themselves, which causes them to produce too much aldosterone, causing you to lose potassium and retain sodium. The excess sodium in turn holds on to water, increasing your blood volume and blood pressure. Primary aldosteronism leads to high blood pressure.
Why is aldosteronism important?
Diagnosis and treatment of primary aldosteronism are important because people with this form of high blood pressure have a higher risk of heart disease and stroke. Also, the high blood pressure associated with primary aldosteronism may be curable.
What is the main target of aldosterone?
The major target of aldosterone is the distal tubule of the kidney, where it stimulates exchange of sodium and potassium. Three primary physiologic effects of aldosterone result:
Which hormone is secreted by the central nervous system?
Cortisol and other glucocorticoids are secreted in response to a single stimulator: adrenocorticotropic hormone (ACTH) from the anterior pituitary. ACTH is itself secreted under control of the hypothalamic peptide corticotropin-releasing hormone (CRH). The central nervous system is thus the commander and chief of glucocorticoid responses, providing an excellent example of close integration between the nervous and endocrine systems.
How does renin affect blood pressure?
The kidneys release renin when there is a drop in blood pressure or a decrease in sodium chloride concentration in the tubules in the kidney. Renin cleaves the blood protein angiotensinogen to form angiotensin 1, which is then converted by a second enzyme to angiotensin 2. Angiotensin 2 causes blood vessels to constrict, and it stimulates aldosterone production. Overall, this raises blood pressure and keeps sodium and potassium at normal levels.
What is the role of aldosterone in blood pressure?
Mineralocorticoid aldosterone is a hormone that plays an important role in maintaining normal sodium and potassium concentrations in blood and in controlling blood volume and blood pressure . Aldosterone increases sodium re-absorption by an action on the distal tubules of the kidney.
What is the function of renin?
Renin is an enzyme that controls aldosterone production. Aldosterone is produced by the adrenal glands located at the top of each kidney, in their outer portion (called the adrenal cortex). Aldosterone stimulates the retention of sodium (salt) and the elimination of potassium by the kidneys.
How does fludrocortisone work?
Fludrocortisone works by decreasing the amount of sodium that is lost (excreted) in your urine. Fludrocortisone is also used to increase blood pressure. Fludrocortisone comes as a tablet to be taken by mouth. Your doctor will prescribe a dosing schedule that is best for you.
What is the purpose of fludrocortisone?
Fludrocortisone is used to treat Addison’s disease and syndromes where excessive amounts of sodium are lost in the urine. Fludrocortisone works by decreasing the amount of sodium that is lost (excreted) in your urine.
Which hormone is responsible for salt and water balance?
Mineralocorticoids are corticosteroid hormones. Mineralocorticoids are synthesized in the adrenal cortex located at the top of each kidney and influence salt and water balances (electrolyte balance and fluid balance). Aldosterone, the main mineralocorticoid, is necessary for regulation of salt and water in your body.
Can aldosterone cause hyperaldosteronism?
A variety of conditions can lead to aldosterone overproduction (hyperaldo steronism, usually just called aldosteronism) or underproduction (hypoaldosteronism). Since renin and aldosterone are so closely related, both substances are often tested together to identify the cause of an abnormal aldosterone.
What is H02AA a chemical?
H02AA. Biological target. Mineralocorticoid receptor. Chemical class. Steroids. In Wikidata. Mineralocorticoids are a class of corticosteroids, which in turn are a class of steroid hormones. Mineralocorticoids are produced in the adrenal cortex and influence salt and water balances ( electrolyte balance and fluid balance ).
What are some examples of synthetic mineralocorticoids?
An example of a synthetic mineralocorticoid is fludrocortisone (Florinef).
Which hormone receptors are not ligand binding?
The hormone receptor without ligand binding interacts with heat shock proteins and prevents the transcription of targeted genes. Aldosterone and cortisol (a glucosteroid) have similar affinity for the mineralocorticoid receptor; however, glucocorticoids circulate at roughly 100 times the level of mineralocorticoids.
What is the name of the hormone that is involved in the retention of sodium?
The name mineralocorticoid derives from early observations that these hormones were involved in the retention of sodium, a mineral. The primary endogenous mineralocorticoid is aldosterone, although a number of other endogenous hormones (including progesterone and deoxycorticosterone) have mineralocorticoid function.
How are mineralocorticoids mediated?
The effects of mineralocorticoids are mediated by slow genomic mechanisms through nuclear receptors as well as by fast nongenomic mechanisms through membrane-associated receptors and signaling cascades .
What enzyme is used to prevent overstimulation?
An enzyme exists in mineralocorticoid target tissues to prevent overstimulation by glucocorticoids. This enzyme, 11-beta hydroxysteroid dehydrogenase type II ( Protein:HSD11B2 ), catalyzes the deactivation of glucocorticoids to 11-dehydro metabolites.
What is the cause of hyperaldosteronism?
Hyperaldosteronism (the syndrome caused by elevated aldosterone) is commonly caused by either idiopathic adrenal hyperplasia or by an adrenal adenoma. The two main resulting problems: Hypertension and edema due to excessive Na+ and water retention. Accelerated excretion of potassium ions (K+).
What are the mechanisms of mineralocorticoid and glucocorticoid?
Mineralocorticoid and glucocorticoid mechanisms are very different but the former may participate in diseases primarily characterized by glucocorticoid excess. Severe hypokalemia, metabolic alkalosis, or therapeutic responses to spironolactone, which are not common in pure glucocorticoid hypertension, may become prominent clinical features if there is excess mineralocorticoid activity. The steroid responsible for the latter may actually be cortisol itself, when the catalytic capacity of 11bHSD2 (close to saturation at the physiologic range) is surpassed by very high cortisol levels, or when the activity of the enzyme is impaired.
What is PHA in medical terms?
Mineralocorticoid resistance is also known as pseudohypoaldosteronism (PHA). Both sporadic and familial cases with either autosomal-dominant or autosomal-recessive cases have been reported.863-867 Clinical presentation of patients with PHA ranges from asymptomatic salt wasting; to growth failure; to chronic failure to thrive, lethargy, and emesis; to life-threatening dehydration accompanied by severe salt wasting.864-866,868-870 Patients with the severe forms of PHA typically present within a year of birth and may even present in utero with polyhydramnios due to polyuria.871 Biochemically, the condition is characterized by urinary salt wasting, hyponatremia, elevated plasma potassium, aldosterone, and renin activity and urinary aldosterone metabolism that are unresponsive to the mineralocorticoid treatment.872-874
What is mineralocorticoid replacement therapy?
Mineralocorticoid replacement therapy is required to prevent sodium loss, intravascular volume depletion, and hyperkalemia. It is given in the form of fludrocortisone (9α-fluorohydrocortisone) in a dose of 0.1 mg daily. The dose of fludrocortisone is titrated individually based on the findings of clinical examination (mainly body weight and arterial blood pressure) and the levels of plasma renin activity. Patients receiving prednisone or dexamethasone may require higher doses of fludrocortisone to lower their plasma renin activity to the upper normal range, whereas patients receiving hydrocortisone, which has some mineralocorticoid activity, may require lower doses. The mineralocorticoid dose may have to be increased during the summer, particularly if patients are exposed to temperatures higher than 29 °C (85 °F).
How does mineralocorticoid deficiency affect renal function?
Mineralocorticoid deficiency results in progressively worsening hyperkalemia as a result of diminished renal perfusion, which reduces glomerular filtration and depresses cation exchange by the distal convoluted renal tubules. Hyperkalemia is worsened by metabolic acidosis, which promotes a shift of potassium ions from the intracellular to the extracellular space. The most prominent manifestation of hyperkalemia is the deleterious effect on cardiac function. Hyperkalemia causes decreased myocardial excitability, an increase in the myocardial refractory period, and slowed conduction. Hypoxia, secondary to hypovolemia and poor tissue perfusion, contributes to myocardial dysfunction. Ventricular fibrillation or cardiac standstill may eventually occur as the plasma potassium concentration exceeds 10 mEq/L.
What is the difference between PHAI and PHAI?
Autosomal recessive (generalized) PHAI results from mutations in the epithelial sodium channel (ENaC), whereas autosomal dominant (renal) PHAI is due to mutations in the mineralocorticoid receptor (MR).
How long does anorexia last in cats?
Signs of weakness, lethargy, and anorexia may persist for 3 to 5 days in cats with acute adrenocortical insufficiency, despite appropriate management. This is in direct contrast to dogs, in which the major clinical signs of primary hypoadrenocorticism usually resolve rapidly within a day or two of treatments. 37,53
Does licorice cause hypertension?
(1968) showed that the picture of hypokalemic alkalosis and hypertension is associated with suppressed plasma renin activity . The active principle, ammonium glycyrrhizate ( Conn et al., 1968 ), exerts its effect directly as a mineralocorticoid, rather than through any secondary adrenal stimulation, and so the aldosterone levels are low rather than high ( Conn et al., 1968 ). This may be a useful diagnostic feature.
How do mineralocorticoids affect sodium reabsorption?
Mineralocorticoids stimulate sodium reabsorption and potassium secretion in principal cells of the distal tubule and cortical collecting duct.54 Aldosterone action requires its initial binding to the mineralocorticoid receptor, followed by translocation of the hormone-receptor complex to the nucleus in which specific genes are stimulated to code for physiologically active proteins (e.g., Na+, K + -ATPase). Early effects of an elevation in circulating levels of mineralocorticoids include increases in the permeability of the luminal membrane to sodium, basolateral Na +, K + -ATPase activity, intracellular potassium concentration, and transepithelial voltage (increased lumen negativity), the latter resulting from enhanced sodium reabsorption. 31 Late steroid-induced effects include increases in number of basolateral sodium-potassium pumps and conducting apical potassium channels. Thus, mineralocorticoids affect both the luminal permeability and the electrochemical gradient across the distal nephron and favor potassium secretion. A reduction in plasma concentration of aldosterone results in a fall in urinary potassium secretion by mechanisms opposite to those just described.
How does mineralocorticoid signaling affect blood pressure?
Mineralocorticoid signaling is primarily implicated in the maintenance of water and salt homeostasis by regulating sodium reabsorption and potassium excretion across tight epithelia. As such, it plays a key role in the control of blood pressure, and in turn, the dysregulated aldosterone secretion and/or mineralocorticoid action are involved in many human diseases such as hypertension, heart failure and chronic kidney diseases associated with increased activation or upregulated mineralocorticoid signaling, while dehydration and sodium loss are related to downregulated or defective mineralocorticoid signaling. In nonepithelial target cells, mineralocorticoid signaling has been linked to various physiological processes, such as memorization and learning, stress response, neuroprotection and regulation of sodium appetite (hippocampus), thermogenesis and differentiation of preadipocytes into mature adipocytes (adipose tissue) and cardiac remodeling.
What is the role of mineralocorticoids in renal sodium conservation?
Mineralocorticoid activity plays an important role in renal sodium conservation. Decreased activity and renal resistance to mineralocorticoids are causes of renal sodium-wastage.217 The most clinically relevant form of mineralocorticoid deficiency results from primary diseases of the adrenal cortex. These diseases may either be acquired or congenital in origin. Subnormal aldosterone secretory rates lead to decreased reabsorption of sodium chloride in the cortical collecting tubule of the kidney. The kidney is fundamentally intact and the cortical collecting tubule cell responds normally to exogenously administered mineralocorticoids.
How do mineralocorticoids affect the kidneys?
Mineralocorticoids are an important determinant of net acid excretion by the kidneys (282, 283) and may mediate the effects of extracellular fluid volume on distal nephron acidification ( 569 ). Several mechanisms explain the stimulation of H secretion in the distal nephron. First, mineralocorticoids are well known to stimulate Na reabsorption and the lumen-negative transepithelial voltage in the CCD; H secretion will increase secondary to the altered voltage. Second, mineralocorticoids directly stimulate H secretion in the CCD and OMCD is, independent of Na transport ( 330, 555 ). Some of this response occurs after only a few hours and can be observed in vitro. A rapid nongenomic stimulation of H-ATPase activity by aldosterone was reported in OMCD ( 678 ); a transient rise in intracellular calcium and a requirement for PKC were found in this response. Chronic mineralocorticoids also increase NEM-sensitive ATPase ( 203, 424 ). Therefore mineralocorticoid stimulation of H secretion may have early and late mechanisms of action, as has been shown for stimulation of Na transport. Mineralocorticoids also stimulate inner medullary collecting duct H secretion, probably independent of Na reabsorption ( 168 ). Another potential mechanism of mineralocorticoid stimulation of H secretion is via potassium depletion, discussed in the following paragraphs.
What is mineralocorticoid excess?
Mineralocorticoid excess is classically characterized by volume expanded hypertension and hypokalemia. The commonest cause of mineralocorticoid excess is primary aldosteronism which now accounts for approximately 10% of cases of primary hypertension and up to 20% of cases of resistant hypertension. Hypertension due to primary aldosteronism results in an excess of cardiovascular morbidity compared to equivalent primary hypertension. Despite this, there remains debate over who to screen and how to best diagnose primary aldosteronism. This article will outline mineralocorticoid production, regulation and action and will describe in detail how to recognize and diagnose primary aldosteronism as well as other, rarer but significant, causes of mineralocorticoid hypertension.
What hormones are involved in the distal nephron?
Mineralocorticoid hormones are key regulators of distal nephron and collecting duct H+ secretion. Two mechanisms appear to be involved. First, mineralocorticoid hormone stimulates Na + absorption in principal cells of the cortical collecting duct (see Fig. 11.5 ). This leads to a more lumen-negative voltage that then stimulates H + secretion. This mechanism is indirect in that it requires the presence of Na + and of Na + transport.
Where are mineralocorticoids synthesized?
Mineralocorticoids are synthesized in the zona glomerulus, the region situated just beneath the adrenal capsule (Fig. 74-1 ). Endogenous mineralocorticoids include desoxycorticosterone (the first mineralocorticoid identified), progesterone, and aldosterone (the most potent). About 100 to 150 μg per day of aldosterone are secreted under normal conditions. A cytochrome P-450 enzyme, CYP11B2 (aldosterone synthase, CYP11B2), catalyzes synthesis by converting desoxycorticosterone to corticosterone and subsequently to aldosterone. 3 Of note, aldosterone can be synthesized in the brain, 4 blood vessels, 5 and heart. 6 Aldosterone synthesis is regulated primarily by the renin-angiotensin system through adrenal angiotensin I receptors. Small changes in blood electrolyte levels also affect production. Potassium acts directly on aldosterone-secreting cells. ACTH has little effect normally but may become important under specific conditions.
What is the difference between mineralocorticoids and corticoids?
With mineralocorticoids, “corticoids” refers to the steroid hormones produced by the adrenal cortex, and “mineral” refers to how these hormones regulate sodium reabsorption and potassium excretion in the distal convoluted and collecting tubules of the kidney.
Why are mineralocorticoid receptor agonists used?
Now, mineralocorticoid-receptor agonists are used to treat pathological conditions where the mineralocorticoid level in the body is lower than normal.
What are the effects of mineralocorticoid receptor agonists?
It’s important to note that high doses of mineralocorticoid-receptor agonists are associated with myopathy, adrenal suppression, and hypothalamic-pituitary-adrenal axis suppression.
Which glands secrete aldosterone?
In the adrenal glands, it triggers the secretion of aldosterone. In the kidneys, aldosterone affects two types of cells along the distal convoluted and collecting tubule of the nephron. First, it binds to mineralocorticoid receptors in the cytoplasm of principal cells, forming an aldosterone-receptor complex. ...
How long does fludrocortisone last after adrenalectomy?
Because of its long duration of action, approximately 8-12 hours, fludrocortisone is also favored for replacement therapy after adrenalectomy.
Why is it called primary?
The reason it’s called “primary” is that the underlying problem is due to damage to the adrenal glands themselves.
What are the conditions that are treated with mineralocorticoid receptor antagonists?
Now, common conditions that are treated with mineralocorticoid-receptor antagonists include hypertension, or high blood pressure, and edematous states like pulmonary edema or ascite s, where fluid builds up in the extracellular space.
What is the effect of activation of the mineralocorticoid receptor?
Activation of the mineralocorticoid receptor, upon the binding of its ligand aldosterone, results in its translocation to the cell nucleus, homodimerization and binding to hormone response elements present in the promoter of some genes. This results in the complex recruitment of the transcriptional machinery and the transcription into mRNA ...
What is MR in biology?
MR is a receptor with equal affinity for mineralocorticoids and glucocorticoids. It belongs to the nuclear receptor family where the ligand diffuses into cells, interacts with the receptor and results in a signal transduction affecting specific gene expression in the nucleus.
Where is MR expressed?
MR is expressed in many tissues, such as the kidney, colon, heart, central nervous system ( hippocampus ), brown adipose tissue and sweat glands. In epithelial tissues, its activation leads to the expression of proteins regulating ionic and water transports (mainly the epithelial sodium channel or ENaC, Na+/K+ pump, serum and glucocorticoid induced kinase or SGK1) resulting in the reabsorption of sodium, and as a consequence an increase in extracellular volume, increase in blood pressure, and an excretion of potassium to maintain a normal salt concentration in the body.
Where is the MR gene located?
The mineralocorticoid receptor (or MR, MLR, MCR ), also known as the aldosterone receptor or nuclear receptor subfamily 3, group C, member 2, ( NR3C2) is a protein that in humans is encoded by the NR3C2 gene that is located on chromosome 4q31.1-31.2. MR is a receptor with equal affinity for mineralocorticoids and glucocorticoids.
Where is the mineralocorticoid receptor located?
The mineralocorticoid receptor (or MR, MLR, MCR ), also known as the aldosterone receptor or nuclear receptor subfamily 3, group C, member 2, ( NR3C2) is a protein that in humans is encoded by the NR3C2 gene that is located on chromosome 4q31.1-31.2. MR is a receptor with equal affinity for mineralocorticoids ...
Which enzyme is selectively inactivated by mineralocorticoids?
The selective responsive of some tissues and organs to mineralocorticoids over glucocorticoids occurs because mineralocorticoid-responsive cells express Corticosteroid 11-beta-dehydrogenase isozyme 2, an enzyme which selectively inactivates glucocorticoids more readily than mineralocorticoids.
Is cortisol an agonist or antagonist?
Ligands. Aldosterone, 11-deoxycorticosterone, and cortisol are endogenous agonists of the MR. Fludrocortisone is a synthetic agonist of the MR which is used clinically. Progesterone is a potent endogenous antagonist of the MR.
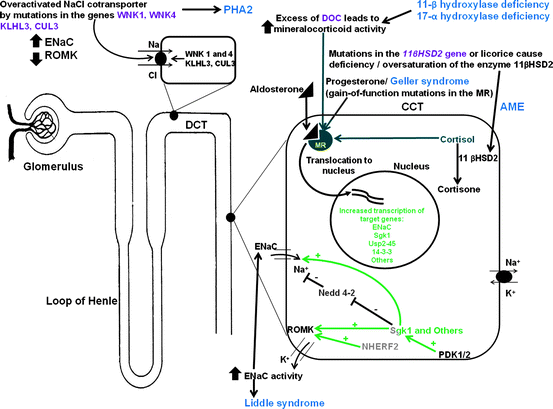
Overview
Mineralocorticoids are a class of corticosteroids, which in turn are a class of steroid hormones. Mineralocorticoids are produced in the adrenal cortex and influence salt and water balances (electrolyte balance and fluid balance). The primary mineralocorticoid is aldosterone.
Physiology
The name mineralocorticoid derives from early observations that these hormones were involved in the retention of sodium, a mineral. The primary endogenous mineralocorticoid is aldosterone, although a number of other endogenous hormones (including progesterone and deoxycorticosterone) have mineralocorticoid function.
Aldosterone acts on the kidneys to provide active reabsorption of sodium and an associated pa…
Mode of action
The effects of mineralocorticoids are mediated by slow genomic mechanisms through nuclear receptors as well as by fast nongenomic mechanisms through membrane-associated receptors and signaling cascades.
Mineralocorticoids bind to the mineralocorticoid receptor in the cell cytosol, and are able to freely cross the lipid bilayer of the cell. This type of receptor become…
Pathophysiology
Hyperaldosteronism (the syndrome caused by elevated aldosterone) is commonly caused by either idiopathic adrenal hyperplasia or by an adrenal adenoma. The two main resulting problems:
1. Hypertension and edema due to excessive Na+ and water retention.
2. Accelerated excretion of potassium ions (K+). With extreme K+ loss there is muscle weakness and eventually paralysis.
Pharmacology
An example of a synthetic mineralocorticoid is fludrocortisone (Florinef).
Important antimineralocorticoids are spironolactone and eplerenone.
See also
• List of corticosteroids
Further reading
• Stewart P (2008): "The Adrenal Cortex " In: Kronenberg, Melmed, Polonsky, Larsen (eds.) Williams Textbook of Endocrinology (11 ed)., Saunders Elsevier, Philadelphia, pp. 445–504.
• Bennett PN and Brown MJ (2008) "Adrenal corticosteroids, antagonists, corticotropin", in Clinical Pharmacology (10ed), Churchill Livingstone Elsevier, Publ. pp. 593–607.
External links
• Mineralocorticoids at the US National Library of Medicine Medical Subject Headings (MeSH)