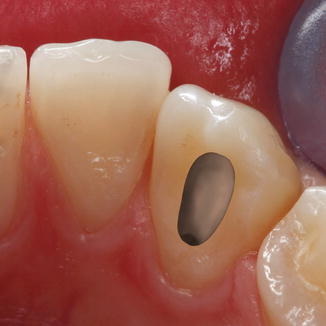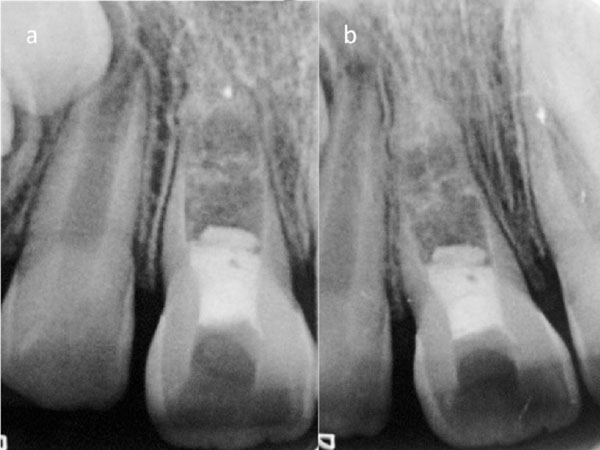
What is apical dentistry? In dental anatomy, the apical foramen, literally translated “small opening of the apex,” is the tooth’s natural opening, found at the root’s very tip—that is, the root’s apex—whereby an artery, vein, and nerve enter the tooth and commingle with the tooth’s internal soft tissue, called pulp.
What is apical surgery?
Apical surgery belongs to the field of endodontic surgery that also includes incision and drainage, closure of perforations, and root or tooth resections. The objective of apical surgery is to surgically maintain a tooth that has an endodontic lesion which cannot be resolved by conventional endodontic (re-)treatment (von Arx, 2005a,b).
What is an apicoectomy?
It’s also called apical surgery, which refers to the “apex,” or end, of the tooth. If your dentist tells you that you need an apicoectomy, it’s probably because even though your tooth has already had a root canal, there’s residual inflammation or infection near the root tip that reaches into your jawbone.
Where is the apical foramen on a tooth?
However, it takes finesse to locate the apical foramen because it is small and varies in the exact location from tooth to tooth. According to Columbia University, your apical foramen is typically between 0.5mm to 1.5mm from the apex of your root.
Does an apical lesion mean the affected tooth has to go?
The following case report on a 10-year-old patient shows that an apical lesion does not necessarily mean the affected tooth has to go. Using flexible nickel-titanium (NiTi) files, even root canals with curves or special features can be cleaned safely and with long term success.
What is apical surgery?
How successful is apical surgery?
How deep should a retrocavity be?
What is the use of a microscope in apical surgery?
What is CBCT in dentistry?
What is the use of a surgical microscope?
What is the best material for root end filling?
See 4 more
About this website
Is apical and periapical the same?
Apical is used to describe a problem originating at the tooth's root tip while periapical implies that it began somewhere around the root tip. The inflammatory response is dependent on the severity of the bacterial infection around the tooth root apex.
What is the difference between a root canal and an apicoectomy?
While root canal treatment takes place on the crown of the tooth (the part above the gum that we chew with) an apicoectomy takes place on the root of the tooth. The infected tissue is accessed via the root tip, also called the apex, of the tooth, and a filling is then placed to seal the end of the root.
Is apical surgery painful?
How Painful Is an Apicoectomy? A root end surgery causes very little discomfort. It is a minor procedure done in your dentist's office, and it doesn't require any general anesthetic. You can usually drive yourself home afterward and go back to your normal activities the next day.
What is the average cost of an apicoectomy?
Cost of Common ProceduresCODEDESCRIPTIONFee3410Apicoectomy–Anterior tooth$1,1983421Apicoectomy–Bicuspid tooth$1,2613425Apicoectomy–Molar tooth$1,5223430Retrograde Filling$30311 more rows
Are you put to sleep for a apicoectomy?
An apicoectomy is surgical removal of the tip (apex) of a tooth's root. It's a minor surgery done in our office under local anesthesia. This means you're awake for the procedure and can drive yourself home afterward. It also means you shouldn't feel any pain while one of our specialists completes the apex removal.
Does bone grow back after apicoectomy?
Post-Operative Apicoectomy Recovery The bone of the jaw will take several months to grow back around the tooth. As with any surgery, there will usually be a slight swelling around the tooth and some discomfort, which is usually easily managed with over-the-counter medications.
How long does it take to fully heal from an apicoectomy?
How long does it take to recover from an apicoectomy? Within a day or two, you should be able to return to your regular daily activities. In two weeks, your gums should heal, and then in about six months, bone will have grown in the cavity left by the removed root tip.
What are the risks of an apicoectomy?
Here are a few risks that can occur with an apicoectomy: Tooth extraction: Surgery may be unsuccessful, and your tooth may need to be extracted. Infection in sinuses: Depending on the location of the infected tooth, if it sits toward the back of your upper jaw, the infection may include your sinus.
How long does it take for a bone to heal after apicoectomy?
While the gum area heals within a few days, it will take several months for the bone to heal completely. During this time, the healing process will be checked with x-rays and by direct examination.
Is an apicoectomy worth it?
It can be very important in preventing serious complications involving the health of your mouth and jaw. Apicoectomies are usually recommended if a root canal procedure was unsuccessful and there's an infection present around the root tip of a tooth.
How long does tooth hurt after apicoectomy?
Pain: Pain or discomfort following surgery is expected to last 4-5 days. For many patients, it seems the third and fourth day may require more pain medicine than the first and second day. Following the fourth day pain should subside more and more every day.
Do you need antibiotics after apicoectomy?
Recovery from Apicoectomy Pain and discomfort are common after undergoing an apicoectomy. Thankfully, pain medication (either prescription or over-the-counter) can be taken to address this discomfort. Patients may also be prescribed antibiotics to help manage potential spread of infection following the procedure.
Is an apicoectomy more painful than a root canal?
In fact, many patients have reported that the apicoectomy was even less painful than the original root canal treatment! Recovery: You may be sore or numb for a few days after the procedure, but usually over-the-counter anti-inflammatory drugs (NSAIDs) such as ibuprofen are all that is needed to control the pain.
Can apicoectomy be done without root canal?
While only performed when conventional root canal retreatment is not practical, apicoectomy for failing root canal-treated teeth can save them, returning the tooth, bone and gum tissues to health for many years.
Is an apicoectomy worth it?
It can be very important in preventing serious complications involving the health of your mouth and jaw. Apicoectomies are usually recommended if a root canal procedure was unsuccessful and there's an infection present around the root tip of a tooth.
What is the success rate of apicoectomy?
[Endodontic surgery (apicoectomy)--success rate of more than 90% using dental operating microscope and ultrasonic tips]
Cost of an Apicoectomy - 2022 Healthcare Costs - CostHelper
How much you can expect to pay out of pocket for an apicoectomy, including what people paid. Without dental insurance, an apicoectomy typically costs $900-$1,300 or more, depending on the position and type of tooth, local rates, and the qualifications and training of the endodontist or oral surgeon performing the procedure.
Apical surgery: A review of current techniques and outcome
Apical surgery is considered a standard oral surgical procedure. It is often a last resort to surgically maintain a tooth with a periapical lesion that cannot be managed with conventional endodontic (re-)treatment.
Apicectomy Procedure, Risks, And Healing - Steady. Health
It can be scary to be told that you need to undergo a surgical procedure, especially one that takes place in your mouth. An apicoectomy, though, might well be the only thing that can help save your tooth.
What Can Go Wrong?
The hard outer layers of your teeth protect the sensitive insides from damage and infection. The tops (crowns) of your teeth are protected by enamel, whereas your teeth' roots are guarded by cementum.
How does a root canal save a tooth?
By removing the pulp of your tooth all the way down through the root canal, your dental professional can often save your tooth from removal and prevent infection from spreading to the bone . After the infected tissue is removed, the resulting space is filled with inorganic material to keep your teeth strong and prevent infection from reoccurring.
How to clean between teeth?
Clean between your teeth once daily using floss, an interdental brush, or a flossing device. Rinse using antiseptic mouthrinse to reduce bacterial dental plaque, remove food matter, and help prevent gum disease . Eat a balanced, healthy diet that’s low in sugary and acidic foods and beverages.
What is the apical foramen?
Apical Foramen: What Is It? To best understand apical foramen, it’s a good idea to cover some dental anatomy quickly. Your tooth is filled with soft tissue called pulp that contains blood vessels and nerves. These vital structures help sustain your teeth and communicate sensation to your nervous system.
Why is the apical foramen important?
Your apical foramen presents challenges during a root canal procedure because your dental professional will most often rely on X-rays. This imaging is essential to your treatment but is far from perfect as it provides a two-dimensional view. The better information your dental professional has, the better they can remove infected tissue and abscesses.
Why is it important to know the location of the apical foramen?
Your dental professional can assess the location of the apical foramen to help ensure successful endodontic treatment . However, it takes finesse to locate the apical foramen because it is small and varies in the exact location ...
What to do if your tooth gets infected?
If your tooth does get infected, your dental professional may recommend a root canal treatment to remove the infection and prevent it from worsening.
When would I need Apical Surgery?
Apical surgery is needed when conventional root canal treatment is not enough to get rid of the root canal infection/damaged root tip. This can be caused by resistant bacterial strains that are well embedded in biofilm beyond the root canal system in the surrounding bone/external root surface. Another reason for this procedure would be damage to the root tip area caused by chronic infection or damage caused by operator error when the initial root canal treatment was done. The root canal system is a delicate system and damage can easily occur if correct treatment protocols and skill are not applied.
What is apicoectomy surgery?
What is Apical Surgery (Apicoectomy)? (in less than 2% of cases) to remove infection from the tip of the roots. This is usually caused by embedded bacteria that colonize on the outside of the root or in the surrounding bone. This resistant disease process is usually caused by “biofilm”.
Can apicoectomy be done without surgery?
Apicoectomy is a rare occurrence these days as the vast majority of root canal complications can be treated non-surgically through the tooth with the aid of cutting edge materials and the microscope. It is quite remarkable how we have advanced in this regard. The face of endodontics has forever changed due to the surgical microscope. We do way less surgery than ever before but it is still critical in some cases and avoiding it in these cases limits the long-term success of the root canal procedure.
Can a root canal be done through a tooth?
In about 98% of these cases, the problem can be solved by correctly doing a root canal treatment conventionally through the tooth. Very often, the apical surgery procedure is totally avoided.
Is a surgical procedure tolerated?
As stated before, all procedures are about correct management. Most of the time when correctly handled, this surgical procedure is well tolerated. In my experience, patients do very well intra-operatively as well as post-operatively when good pain management protocols are implemented.
What happens during an apicoectomy?
During the treatment, an incision is made in the gum near the tooth to expose and get rid of any inflamed or infected tissue. Your endodontist will also remove the tip of the tooth’s root.
What is the procedure for a tooth that is giving you problems again?
This time, your dentist suggests a different dental procedure— an apicoectomy.
How are teeth held in place?
Our teeth are held in place by roots that extend into our jawbone. An apicoectomy is aminor surgical procedure that removes the apex, or very tip, of the tooth’s root.
Can you save a tooth with a root canal?
If this is suggested for you, it means your tooth cannot be saved by conventional root canal treatment. Often, the only alternative to an apicoectomy is removing [ML1] the tooth, which could affect adjacent teeth that are healthy. The purpose is to preserve the function of your natural tooth.
Can you continue to do normal activities after endodontic surgery?
Many patients are able to continue to normal activities the next day. You may experience discomfort and swelling as you heal. Make sure to follow postoperative instructions – including diet and brushing advice - given by your endodontist. Call him or her immediately if your pain doesn’t respond to medication or recovery instructions.
Does Delta Dental cover oral surgery?
Access to affordable, routine care can prevent the need for oral surgeries, but coverage depends on your specific plan. Contact Delta Dental if you have questions about your coverage or compare Delta Dental plans now to enroll today.
Is it painful?
An apico ectomy can be more invasive than a typical root canal surgery, meaning the recovery time is usually more painful. Patients will receive local anesthesia during an apicoectomy to help prevent any pain.
What happens after a root canal is removed?
After the root tip is removed, the root canal inside the tooth is cleaned and sealed with a small filling to prevent future infection. Your dentist or endodontist may then take another X-ray to make sure your tooth and jaw look good and that there are no spaces where a new infection could take hold.
Why do people have apicoectomy?
An apicoectomy is a straightforward, minor surgical procedure that’s done on children and adults as a way to save at-risk teeth and prevent potentially serious complications. An apicoectomy is also known as root end surgery. This is because it involves the removal of a tooth’s root tip and surrounding tissue.
How to remove a tooth root?
Here’s a breakdown of the procedure itself: 1 Before any work is done, you’ll be given a local anesthetic to numb the area around the affected tooth. 2 During the procedure, your dentist or endodontist cuts through your gum and pushes the gum tissue aside in order to reach the root. Usually just a few millimeters of the root are removed, as is any infected tissue surrounding the root. 3 After the root tip is removed, the root canal inside the tooth is cleaned and sealed with a small filling to prevent future infection. Your dentist or endodontist may then take another X-ray to make sure your tooth and jaw look good and that there are no spaces where a new infection could take hold. 4 The tissue will then be sutured (stitched), so your gum can heal and grow back in place. Your jawbone will also eventually heal around the filling at the end of the root. You shouldn’t feel much, if any, pain or discomfort during the procedure.
How long does it take for an apicoectomy to be successful?
Apicoectomy success rate. Apicoectomies are considered routine outpatient dental procedures. A 2020 study. found that about 97 percent of cases still experienced excellent results following apical surgery up to 5 years later, and good results in more than 75 percent of cases after 10 to 13 years.
What is the procedure to numb a tooth?
Before any work is done, you’ll be given a local anesthetic to numb the area around the affected tooth. During the procedure, your dentist or endodontist cuts through your gum and pushes the gum tissue aside in order to reach the root.
How long does it take for a gum to heal after an apicoectomy?
You shouldn’t feel much, if any, pain or discomfort during the procedure. An apicoectomy usually takes 30 to 90 minutes.
What Is an Apical Abscess?
A dental abscess is your body's inflammatory reaction to an infection in the tooth's nerve. The abscess itself is a collection of pus arising from a source of infection at the tooth's root, which can break through the tissues and discharge into the mouth.
What to do if you have an abscess?
When you have an abscess, it's important to visit your dentist promptly for diagnosis and treatment. Arriving at your appointment armed with a basic knowledge of what the abscess is can also help.
What is a chronic abscess on an X-ray?
On an X-ray, a chronic abscess will display bone destruction as dark regions in the bone, also known as radiolucencies.
Can a dentist insert a gutta percha point?
As a study in the Journal of International Dental and Medical Research notes, if this is the case, your dentist may insert a gutta percha point — a flexible material — into the draining opening of the abscess.
Can a dental abscess cause a swollen lymph node?
Pus may form with swelling of surrounding tissues. X-rays may appear normal. Often, an acute abscess comes with malaise, fever or swollen lymph nodes. As the Mayo Clinic explains, severe dental abscesses can even lead to sepsis, which is a life-threatening infection in the blood stream.
Can a dentist tap your teeth?
Your dentist will tap your teeth to assess sensitivity, take X-rays and possibly recommend a CT scan for further evaluation, according to the Mayo Clinic. Your history of symptoms will also aid the diagnosis. Sometimes, it can be unclear which tooth is causing the abscess.
Can an infection cause an abscess?
An infection can cause severe problems and spread to other regions of the body, making it a higher risk to your health. Arming yourself with this information can help you keep an eye on your dental health and make appointments with your dentist as necessary if an urgent concern arises, such as an apical abscess.
What is apical surgery?
Apical surgery is considered a standard oral surgical procedure. It is often a last resort to surgically maintain a tooth with a periapical lesion that cannot be managed with conventional endodontic (re-)treatment. The main goal of apical surgery is to prevent bacterial leakage from the root-canal system into the periradicular tissues by placing a tight root-end filling following root-end resection. Clinicians are advised to utilize a surgical microscope to perform apical surgery to benefit from magnification and illumination. In addition, the application of microsurgical techniques in apical surgery, i.e., gentle incision and flap elevation, production of a small osteotomy, and the use of sonic- or ultrasonic driven microtips, will result in less trauma to the patient and faster postsurgical healing. A major step in apical surgery is to identify possible leakage areas at the cut root face and subsequently to ensure adequate root-end filling. Only a tight and persistent apical obturation will allow periapical healing with good long-term prognosis. The present paper describes current indications, techniques and outcome of apical surgery.
How successful is apical surgery?
With regard to the outcome of apical surgery, inconsistent success rates ranging from 44% to 90% were reported prior to the introduction of microsurgical techniques (Hepworth and Friedman, 1997). However, recent studies have shown that the treatment outcome of apical surgery has considerably improved, and the success rates have approached or exceeded 90% (von Arx, 2005a,b). This tendency of consistently high healing rates after apical (micro-)surgery has been substantiated by several clinical studies published in the last 5 years (Lindeboom et al., 2005a,b; Tsesis et al., 2006; von Arx et al., 2007a,b,c; Kim et al., 2008; Saunders, 2008; Taschieri et al., 2008; Christiansen et al., 2009).
How deep should a retrocavity be?
After the careful check of the resection plane, a retrocavity is prepared into the root-end. This retrocavity should have a depth of 3 mm and should follow the original path of the root canal. The cavity should also include an isthmus or accessory canal, if present. While the conventional technique of root-end cavity preparation, i.e., the use of a small round bur or of an inverted cone bur in an angled micro-handpiece, was problematic with regard to direction and depth of the retrocavity, the development of sonic- or ultrasonic driven microtips (retrotips) was a major breakthrough in apical surgery, and has considerably simplified the technique of root-end cavity preparation (von Arx and Walker, 2000). The small and angled configuration of the microtips does not require an acute bevel of the resection plane; hence, fewer dentin tubules are exposed. In addition, the osteotomy (bony window and bony crypt) can be kept to a minimum with microtips, compared to with conventional rotary instruments. This also leads to less trauma for the patient and faster bony healing (von Arx et al., 2007a,b,c). Concern over the possibility of increased frequency of dentinal cracks following root-end cavity preparation by means of ultrasonic or sonic microtips has been refuted in several clinical and cadaver studies (Calzonetti et al., 1998; Morgan and Marshall, 1999; Gray et al., 2000; de Bruyne and de Moor, 2005).
What is the use of a microscope in apical surgery?
The use of a surgical microscope is strongly advocated in apical surgery since it allows inspection of the surgical field at high magnification with excellent and focused illumination, detection of microstructures (additional canals, isthmus) and root integrity (cracks, fractures, perforations), distinction between bone and root, and identification of adjacent important anatomical structures. The incision and flap design should be chosen according to clinical and radiographic parameters, including condition, biotype and width of gingival tissues, presence of a restoration margin, location and extent of the periapical lesion, and patient’s esthetic demands. A small osteotomy is produced to locate the root-end that is resected by about 3 mm. The resection plane should be perpendicular to the long axis of the tooth. At this stage, all pathological tissue should be removed and adequate hemorrhage control be established. The application of 1–2% methylene blue dye aids in the careful inspection of the cut root face. It is important to identify possible areas of leakage such as root-fractures, un-negotiated accessory canals or isthmuses, and gaps between the existing root-canal filling and the root-canal walls. Root-end cavity preparation is performed with sonic- or ultrasonic driven microtips. The use of rotary instruments to prepare a root-end cavity is no longer recommended. The retrocavity should have a depth of 3 mm, follow the original path of the root canal, and also include accessory canals and isthmuses, if present. How to surgically manage dentinal cracks has not been clarified yet, but teeth with vertical root fractures must be extracted. With regard to the root-end filling material, mineral trioxide aggregate (MTA) appears to become the standard. Although it is a comparatively expensive material and the clinician has to become familiar with its handling, MTA has excellent biocompatibility, ideal adherence to the cavity walls, and low solubility. Clinical (comparative) studies have reported excellent success rates for MTA ranging from 90% to 92% (follow-up periods from 1 to 5 years).
What is CBCT in dentistry?
The introduction of cone beam computed tomography (CBCT), also called digital volume tomography (DVT), has had an enormous impact in dentistry, and particularly in surgical fields of dentistry. Whereas conventional computed tomography (CT) provides sliced-image data, CBCT captures a cylindrical volume of data in one acquisition and thus offers distinct advantages over conventional radiography. These advantages include increased accuracy, higher resolution, scan-time reduction, and dose reduction (Cotton et al., 2007). CBCT greatly aids in assessment prior to apical surgery.
What is the use of a surgical microscope?
The utilization of a surgical microscope is today considered a must in endodontics. Teaching the use of magnification is now an accreditation requirement of the American Dental Association (ADA) for endodontic speciality programs (Kim and Kratchman, 2006). Several authors have described the benefits of using a surgical microscope in apical surgery as well (Kim, 1997; Rubinstein and Kim, 1999): inspection of the surgical field at high magnification, smaller osteotomy, identification of microstructures (additional canals, isthmus) and root integrity (cracks, fractures, perforations), distinction between bone and root, identification of adjacent important structures (roots of neighboring teeth, maxillary sinus, nasal cavity, mandibular canal, mental foramen, etc.). The use of a surgical microscope also requires an erect posture, thus reducing occupational and physical stress. In addition, video recordings of surgeries can be used for research, education or case documentation.
What is the best material for root end filling?
However, mineral trioxide aggregate (MTA) appears to have become the gold standard for a root-end filling material. All clinical comparative studies published to date have reported higher success rates for MTA than for the competitor material (Chong et al., 2003; Lindeboom et al., 2005a,b; von Arx et al., 2007a,b,c; Kim et al., 2008), although the differences were not found to be significant (probably due to the number of treated cases). Although MTA is an expensive material and the clinician has to become familiar with its handling, it has major advantages, including excellent biocompatibility (Camilleri and Pitt Ford, 2006), ideal adherence to the cavity walls and low solubility (Poggio et al., 2007), and cementogenesis at the cut root face, with deposition of new cementum onto the exposed dentin and MTA surfaces (von Arx et al., 2003a,b; Baek et al., 2005; Bernabé et al., 2007). The most recently published randomized clinical trial compared MTA to smoothing of the existing orthograde gutta–percha (GP) root filling. Teeth treated with MTA demonstrated a significantly (p < 0.001) better healing (96%) than teeth treated with the smoothening procedure only (52%) (Christiansen et al., 2009). The results emphasize the importance of placing a root-end filling after apical resection.