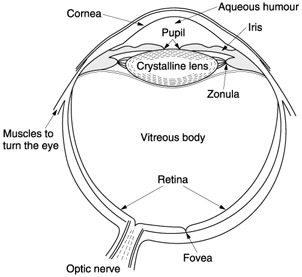
What are granulomatous KP (keratic precipitates)?
This photo shows granulomatous KP (keratic precipitates) plastered on the back surface of the cornea. These opacities are clumped in groups and in this eye, are so large that they can be seen with the naked eye. This photo shows KP, collections of sticky inflammatory cells, that have adherred to the inner surface of the cornea.
Which tests are used to diagnose keratosis pilaris (KP)?
Since the appearance of keratosis pilaris is recognizable, specific laboratory tests are not needed for the diagnosis. Skin biopsy (surgically taking a small piece of skin using local numbing medicine) may be useful in atypical or widespread cases.
Where can I see the KP spots?
As you can see in this video, the KP spots are visible on the back surface of the corneal light-beam, and can also be seen when retroilluminating the iris behind. To download this video, right click on a link below and choose “Save Target As…”
What is the prognosis of keratosis pilaris (KP)?
Keratosis pilaris frequently improves with age in many patients. Many patients note improvement of their symptoms in the summer months and seasonal flares in colder winter months. Keratosis seems to improve in areas of high humidity. More widespread, atypical cases of keratosis pilaris may be cosmetically distressing.
What causes Keratic precipitates?
Formation of keratic precipitates (KP) is a characteristic finding invarious forms of intraocular inflammation, including uveitis and corneal transplantrejection. Generally, KP are created by the clustering of cells with adherenceto the corneal endothelium.
What is KPs Ophthalmology?
1 Keratic precipitates (KPs), are characteristic features of various types of intraocular inflammation. These are cellular aggregates on the corneal endothelium, typically composed of epithelioid cells, lymphocytes and polymorphonuclear cells.
Where are Keratic precipitates found?
Cellular deposits on the corneal endothelium. Acute, fresh KPs tend to be white and round, while old KPs are usually irregular, faded and pigmented.
What causes granulomatous uveitis?
Granulomatous uveitis tends to be chronic and is often associated with systemic conditions and autoimmune reactions. It may also be associated with infectious etiologies such as syphilis, Lyme disease, tuberculosis (TB), and herpetic viral infections.
How are KP formed?
KPs are corneal endothelial deposits that are frequently observed in association with anterior-segment inflammation. [17] These precipitates are formed by the aggregation of polymorphonuclear cells, lymphocytes, and epithelioid cells.
What is the best treatment for uveitis?
Most cases of uveitis can be treated with steroid medicine. A medicine called prednisolone is usually used. Steroids work by disrupting the normal function of the immune system so it no longer releases the chemicals that cause inflammation.
How long does it take for anterior uveitis to resolve?
Attacks of anterior uveitis last for different lengths of time but most settle within six to eight weeks. Your symptoms should disappear within a few days of treatment but you will need to take the treatment for longer whilst the inflammation goes down.
What causes cells in uveitis?
Possible causes of uveitis are infection, injury, or an autoimmune or inflammatory disease. Many times a cause can't be identified. Uveitis can be serious, leading to permanent vision loss. Early diagnosis and treatment are important to prevent complications and preserve your vision.
What is cell and flare in the eye?
“Cell” is the individual inflammatory cells while “flare” is the foggy appearance given by protein that has leaked from inflamed blood vessels. This finding is commonly seen with uveitis, iritis, and after surgery … and actually seeing it can be challenging for the beginning ophthalmology residents.
How is granulomatous uveitis treated?
Topical corticosteroids are the mainstay of therapy and should be used aggressively during the initial phases of therapy. If the patient poorly complies with topical therapy or if the iritis is not responding to topical corticosteroids, a subconjunctival injection of shorter-acting or depot steroids may be used.
Can an optometrist treat uveitis?
How do you treat uveitis? Optometrists will usually prescribe two different eye drops for uveitis. Depending on the severity of the condition, the drops can be used for up to four weeks. The object of the treatment is to reduce pain and inflammation, prevent further tissue damage and restore any loss of vision.
How can I reduce inflammation in my eye?
How to treat a swollen eye at home, quicklyUse a saline solution to rinse your eyes if there's discharge.Use a cool compress over your eyes. ... Remove contact lenses, if you have them.Place chilled black tea bags over your eyes. ... Elevate your head at night to decrease fluid retention.More items...
What are stellate Keratic precipitates?
Keratic precipitates are observed from 80% to 100%. These KP have distinctive features with a characteristic morphology and distribution. They are generally grayish, numerous, translucent, small to medium in size and typically scattered all over the entire corneal endothelium.
What causes superficial punctate keratitis?
Superficial punctate keratitis is an eye disorder caused by death of small groups of cells on the surface of the cornea (the clear layer in front of the iris and pupil). The eyes become red, watery, and sensitive to light, and vision may decrease somewhat.
How common is posterior uveitis?
This condition affects males and females in equal numbers. It can strike at almost any age, but usually begins between the ages of 30 and 40. According to one estimate, posterior uveitis occurs in 18/100,000 people (2020).
What causes Fuchs Heterochromic Iridocyclitis?
No specific cause has been identified although toxocariasis and toxoplasmosis have both been implicated by associated antibody findings. Rubella virus and antibodies against rubella virus have been found in the aqueous humor of young patients with Fuchs' heterochromic iridocyclitis.
Download this video
To download this video, right click on a link below and choose “Save Target As…”
Screencaptures
This photo shows granulomatous KP (keratic precipitates) plastered on the back surface of the cornea. These opacities are clumped in groups and in this eye, are so large that they can be seen with the naked eye.
What is keratosis pilaris?
Keratosis pilaris is a very common skin disorder that affects people of all ages. Keratosis pilaris is a benign condition characterized by numerous small, rough, red, or tan bumps primarily around hair follicles on the upper arms, legs, buttocks, and sometimes cheeks. Keratosis pilaris creates a "goose bumps," "gooseflesh," or "chicken skin" appearance. Keratosis pilaris may be cosmetically displeasing, but it is medically entirely harmless. Keratosis pilaris is common in otherwise healthy people.
What are keratosis pilaris symptoms and signs?
Typically, keratosis pilaris patients present with a scattered, patchy rash composed of very small red or tan bumps. Anywhere from 10 to hundreds of very small slightly rough bumps produce a fine sandpaper-like texture. Some of the bumps may be slightly red or have an accompanying light-red halo indicating inflammation.
What types of doctors treat keratosis pilaris?
Most family physicians and pediatricians are able to diagnose and treat this condition. Occasionally, a dermatologist referral may be necessary.
Does diet have anything to do with keratosis pilaris?
Diet does not affect keratosis pilaris. Vitamin A deficiency may cause symptoms similar to keratosis pilaris, but it's not known to cause keratosis pilaris.
Is keratosis pilaris curable?
There is no available cure, miracle pill, or universally effective treatment for keratosis pilaris. It sometimes clears completely by itself without treatment.
Are there home remedies for keratosis pilaris?
Do take measures to prevent excessive skin dryness, especially in colder winter months.
What is the prognosis of patients with keratosis pilaris?
Keratosis pilaris frequently improves with age in many patients. Many patients note improvement of their symptoms in the summer months and seasonal flares in colder winter months. Keratosis seems to improve in areas of high humidity. More widespread, atypical cases of keratosis pilaris may be cosmetically distressing.
How to diagnose keratosis pilaris?
Your doctor can diagnose keratosis pilaris by looking at your skin. You don't need to be tested for it.
What Is Keratosis Pilaris?
Keratosis pilaris is a common, harmless skin condition that causes small, hard bumps that may make your skin feel like sandpaper. You may have heard it called “chicken skin.”
Is keratosis pilaris worse in the summer?
It's usually worse in the winter months, when there's less moisture in the air, and then may clear up in the summer. It often affects people with certain skin conditions, including eczema (also called atopic dermatitis).
Does keratosis pilaris hurt?
Except for some possible itching, keratosis pilaris doesn't hurt and doesn't get worse.
How does Kaiser Permanente work?
When you’re a Kaiser Permanente member, your whole care team is connected — to you, and to each other — through your electronic health record. Every visit is captured, so your doctor can use your health history to inform your care. If you need to see a specialist, they’ll have important information about your health before they even meet you in person.2 And when you fill a new prescription, your pharmacist can make sure it’s safe to take with your other medications. This enables us to deliver the right care faster — and help members avoid unnecessary visits, serious health conditions, and sleepless nights.
How to get self care advice from Kaiser?
Fill out a short questionnaire about your symptoms online and get personalized self-care advice from a Kaiser Permanente health care professional.
Is Kaiser Permanente a preventative health care provider?
Many common health conditions are preventable — so a proactive approach to prevention is the foundation of how we practice medicine. When you’re a Kaiser Permanente member, your electronic health record triggers automatic reminders for screenings, so we can let you know when it’s time to make an appointment. Your care team sees a complete picture of your health at every visit. And your care gets documented along the way. It’s how we help many members avoid serious health issues, and help others catch problems before they’re serious.
What is an optician?
Opticians are skilled technicians. They do not test vision, prescribe corrective lenses, or diagnose or treat eye diseases. Some states require completion of a 2-year training program or a 3-year apprenticeship for a license. Others have no formal requirements.
What is an ophthalmologist?
Ophthalmologists are medical doctors (MDs) who specialize in eye care. Ophthalmology is a surgical subspecialty. Ophthalmologists are licensed by state medical boards to practice medicine and are usually board-certified in ophthalmology. Ophthalmologists are certified to:
What are the requirements to become an optometrist?
Optometrists (ODs) have at least 3 years of undergraduate science work and may have a 4-year degree. They attend 4 years of optometric college. They are not medical doctors. Optometrists can: 1 Diagnose refractive errors and prescribe corrective lenses. 2 Detect signs of disease and refer you to an ophthalmologist. 3 Administer diagnostic drugs. 4 Diagnose and treat eye diseases and prescribe therapeutic drugs (in most states). 5 Perform some eye surgery (in some states).
Can optometrists diagnose eye disease?
They can carry out any medical or surgical treatment. In a few states, even where they are allowed to administer diagnostic drugs, optometrists are not allowed to diagnose or treat eye disease. They may observe signs of disease and refer you to an ophthalmologist.
Can an optometrist diagnose nearsightedness?
Making the choice. Both ophthalmologists and optometrists can diagnose refr active errors, such as nearsightedness, and prescribe corrective lenses, such as glasses or contact lenses. Ophthalmologists can diagnose all disorders that affect the eye. They can carry out any medical or surgical treatment.
