What is panagglutinin antibody?
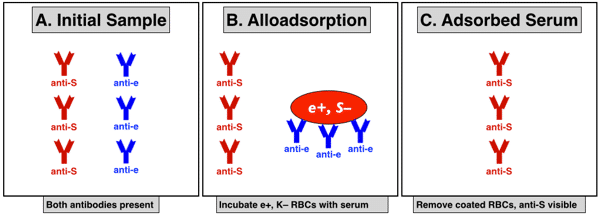
Panagglutinin. An antibody that reacts against all reagent cells in an antibody panel, rather than against one or more specific cells. Panagglutinins are most commonly autoantibodies, but may also be alloantibodies targeted against high-frequency red cell antigens (antigens present on just about everyone else’s RBCs).
What causes panagglutination in agglutinin disease?
Cold agglutinins usually cause panagglutination and cell group shows AB group and serum O group. Because these antigens are usually high-incidence, these patients will typically demonstrate panagglutination when their serum is exposed to most commercially procured screening red blood cells.
What is Polyagglutination?
Polyagglutination Nonspecific agglutination of red cells in the presence of human serum, not related to blood group specificity. This occurs most often as a consequence of infections, when bacterial enzymes actually strip off parts of antigens normally present of the surface of the red cell.
Do cold autoantibodies cause panagglutination?
Discrepancy caused by red cell autoantibodies was observed in 187 cases (14.5%), in that causing panagglutination was observed in 69/187 cases by cold autoantibodies (37%), rest of discrepancies were because of mixed and warm autoantibodies. Cold agglutinins usually cause panagglutination and cell group shows AB group and serum O group.
What is Pan agglutination in blood bank?
An antibody that reacts against all reagent cells in an antibody panel, rather than against one or more specific cells.
What is the 3 3 rule in blood bank?
Rules for what constitutes a proof of association vary from centre to centre, but a commonly accepted approach is the “rule of three”: if three cells that express the antigen in question all react with the patient's plasma, and three cells that don't express the antigen are also all non-reactive, the antibody can be ...
What is Autocontrol in blood bank?
An autocontrol tests the patient's serum with his or her own red cells. Testing an autocontrol routinely with the screen is optional; most blood bankers prefer to perform a DAT only if the screen is positive.
What is Alloantibody in blood bank?
In blood banking, an antibody formed in response to pregnancy, transfusion, or transplantation targeted against a blood group antigen that is not present on the person's red blood cells.
What is enzyme panel?
Enzyme Panels. Proteolytic enzymes, such as ficin and papain enhance certain blood group antibody-antigen reactions, but also reduce or destroy the reactivity of others.
How do you identify antibodies?
Antibody detection and identification are performed by testing patient serum or plasma with reagent red cells. Agglutination or hemolysis indicates sensitization of the reagent red cells by an unexpected antibody in the patient's serum. The reagent red cells come with an antigram or antigen profile sheet.
What are the 3 phases of crossmatching?
Crossmatch TestingMajor crossmatch: This is the most important one. ... Minor crossmatch: This detects antibodies in the donor serum to the recipient's red blood cells. ... Autocontrol: We also perform an auto-control with our crossmatches, i.e. recipient serum with recipient red blood cells.
What is positive autocontrol?
Positive autocontrol is noted when cells taken from the patient and mixed with their own serum react positively. This is usually seen if there is an autoimmune process going on with the patient (antibody on his own cells) or a transfusion reaction (antibodies on donor cells in patient's circulation).
Why is auto control positive?
When a patient has an autoantibody, the direct antiglobulin test and the autocontrol in an antibody panel will be positive. In addition, all cells in the panel will be reactive. If the antibody reactions are stronger at colder temperatures and weaker at warm temperatures, the patient probably has a cold autoantibody.
What is Isohemagglutinins?
Definition. Absent or undetectable level of isohemagglutinin. An isohemagglutinin refers to the naturally occurring antibodies in the ABO blood group system (i.e., anti-A in a group B person, anti-B in a group A person, and anti-A, anti-B, and anti-A,B in a group O person). [ from HPO]
What is the difference between auto and Alloantibodies?
Alloantibody and autoantibody are two types of antibodies generated in our body against antigens. Alloantibody is produced against alloantigens, which are foreign antigens introduced into our body by transfusion or pregnancy, while autoantibody is an antibody that reacts with self-antigens.
What is anti BGA antibody?
Bg Antibodies Anti-Bga is an antibody directed against HLA antigens on red blood cells. Bga represents HLA- B7. There are a few reports of Bg antibodies causing Hemolytic Transfusion Reactions. Anti-Bgb is an antibody directed against HLA antigens on red blood cells.
What is cross matching in blood?
A crossmatch is performed prior to administration of blood or blood products (e.g. packed red blood cells). The purpose of the crossmatch is to detect the presence of antibodies in the recipient against the red blood cells of the donor. These antibodies attach to the red blood cells of the donor after transfusion.
What are the procedures in blood bank?
A certain set of standard tests are done in the lab once blood is donated, including, but not limited to, the following:Typing: ABO group (blood type)Rh typing (positive or negative antigen)Screening for any unexpected red blood cell antibodies that may cause problems in the recipient.More items...
What is the difference between blood bank and blood banking?
A blood bank is a place where blood is collected and stored before it is used for transfusions. Blood banking takes place in the lab. This is to make sure that donated blood and blood products are safe before they are used. Blood banking also determines the blood type.
What is the basic responsibility of blood bank in hospital?
The hospital blood bank is responsible for management of the hospital's blood stock. This includes maintining an inventory for each blood group, ensuring an average age of blood at time of issue, and monitoring the amount of blood that becomes out dated or is not used for other reasons.
adiescast
Try the Coombs crossmatch first. If it is incompatible, definitely check for cold reactive and high frequency antibodies as well as trying a different enhancement medium. If it is compatible, the antibody could be against a preservative in the reagent cells. Was there any problem with the back type?
TimOz
Just a minor technical point. In this case it is very important that the autocontrol is performed in exactly the same way as the screen and ID panel. By that, I ,ean that the patient cells must be washed in exactly the same diluent as the panel cells. If not, you can really end up in a tangle.
Abid
If the patient BG look like O pos or Neg and the Ab screen pos in all phases, I would think that the patient has antibody to high prevalence such as Anti-H in bumpy blood group or Anti-HI, Anti-I, Anti-Vel, Anti-Tja etc….
JohnT
My apologies for being flippant - I was referring to one of the gurus on this site, Malcolm Needs at the National Blood Service in the UK.
LaraT23
I usually ask my techs to run a tube panel if this is happening on gel. If it still reacts, we do a DAT and auto and if those are negative, it depends on the patient's situation. If we have time, we send it our reference lab, if not I try to start full crossmatching to find least incompatible while it is being worked on at the reference lab.
What is autoagglutination in EDTA?
Autoagglutination – agglutination of erythrocytes that is not eliminated by diluting blood in sterile saline is suggestive of immune-mediated haemolytic disease (dilute 1 drop EDTA blood: 4 drops saline).
How to distinguish autoagglutination from rouleaux formation?
Autoagglutination must be distinguished from rouleaux formation by proper washing or dilution of the blood on the slide.
What is the CBC pattern for IMHA?
Diagnosis of IMHA is typically based on identifying moderate to large numbers of spherocytes, autoagglutination, or both in a dog.19 A typical CBC pattern in canine IMHA (mean figures from an author's retrospective study) is: moderate to severe anemia (e.g., PCV 16%), marked reticulocytosis (e.g., 625,000/µl), polychromasia (e.g., 3+ or 4+), normal to slightly increased PP (e.g., 7.2 g/dl), marked leuk ocytosis (e.g., 54,000/ml), significant spherocytosis (e.g., 2+ or more) in most (i.e., 82%) dogs, and autoagglutination and thrombocytopenia (e.g., 29%) in some dogs. The RI is usually greater than 3, suggesting hemolytic anemia. The mean RI in one study of IMHA was 4.8. Moderate to marked spherocytosis (e.g., spherocytes > 50% of RBCs) in dogs is diagnostic for IMHA with rare exceptions, such as viper bite. RBC agglutination, persisting after saline dilution (i.e., autoagglutination), is also diagnostic of IMHA. Thrombocytopenia may be immune mediated or caused by a thromboembolic (disseminated intravascular coagulation [DIC]) problem. Some IMHA cases are nonregenerative if the immune reaction damages erythroid precursor cells in the bone marrow. A positive Coombs test is also good evidence for IMHA.
What are the characteristics of a virulence plasmid?
A number of virulence plasmid-mediated phenotypic characteristics, including colony morphology, autoagglutination (AA), serum resistance, tissue culture detachment, hydrophobicity (HP) and low-calcium response (Lcr), have been applied to the determination of virulence in strains of Y. enterocolitica. These methods require specific reagents and conditions and do not give clear-cut results. In addition, most of these procedures are costly, time-consuming, complex and impractical for routine diagnostic use, particularly in field laboratories. Although the virulence can be effectively demonstrated using laboratory animals, this test is not suitable for routine diagnostic use. Molecular techniques such as DNA colony hybridization, DNA restriction fragment length polymorphisms and polymerase chain reaction (PCR) have also been successfully applied to the detection of virulent strains. However, these techniques are complex and time-consuming. These methods detect only the presence of a specific gene and not the presence of the organism. Although virulence is plasmid-mediated in all strains examined, the plasmids involved differ in molecular weight. Thus, in epidemiological studies it is not sufficient to search for plasmids of a particular molecular weight as an indicator of Y. enterocolitica virulence.
What are the characteristics of a pyv-mediated phenotypic test?
A number of pYV-mediated phenotypic characteristics, including colony morphology, autoagglutination (AA), serum resistance, tissue culture detachment, hydrophobicity (HP), and low-calcium response (Lcr) have been applied to the determination of virulence in strains of YEP+. These methods require specific reagents and conditions and do not give clear-cut results. In addition, most of these procedures are costly, time consuming, complex, and impractical for routine diagnostic use, particularly in field laboratories. Although virulence can be effectively demonstrated using laboratory animals, this test is not suitable for routine diagnostic use. Molecular techniques such as colony hybridization, restriction fragment-length polymorphisms, and the polymerase chain reaction (PCR) have been successfully applied to the detection of virulent strains. These techniques are complex and time consuming, however. These methods detect only the presence of a specific gene and not the presence of the organism. Although virulence is pYV mediated in all strains examined, the pYVs involved differ in molecular weight. Thus, in epidemiological studies, it is not sufficient to search for pYV of a particular molecular weight as an indicator of virulence in YEP+.
What is the physiologic property of equine erythrocytes to aggregate and form rou?
The physiologic property of equine erythrocytes to aggregate and form rouleaux on the peripheral blood smear ( Fig. 44.3) requires special consideration and should be distinguished from pathologic autoagglutination. The latter leads to formation of irregularly shaped erythrocyte clusters of different sizes, whereas rouleaux formation leads to a more orderly association with the erythrocytes lining up in rows. Mixing of the blood with normal saline (in a ratio of 1 part blood to 4 parts saline) will break up rouleaux , but not agglutinated erythrocytes. 20,39,40
When autoagglutination is absent direct or indirect Coombs test can be used?
When autoagglutination is absent direct or indirect Coombs test can be used. The direct test is more sensitive but it is important to realize that false-negatives may be obtained if an incomplete set of reagents is used, if the test is not performed at both 40°C and 37°C, or if severe hemolysis has already resulted in the removal of the majority of antibody-coated RBCs from the circulation.
Passive Antibodies Other Than Anti-D Through RhIG?
RhIG and its many brand names (Rhophylac, WinRho, RhoGAM, etc) is derived from human blood plasma containing the anti-D antibody. Plasma is harvested from healthy Rh negative donors who are intentionally alloimmunized with with the RhD antigen. Those with an active immune response will create Anti-D in 1 to 2 weeks time.
ADAMTS13 has logged into the chat..
Who is ADAMTS13? ADAMTS13 stands for "A disintegrin and metalloproteinase with a thrombospondin type 1 motif, member 13". If you can't remember that, just remember that it's also known as von Willebrand factor-cleaving protease. It's easy to see, though, how you could mistake it for someone's online username or handle.
Duffy The Vampire Slayer?
Duffy The Vampire Slayer? The prevailing thought was that Duffy negative (Fya-Fyb-) phenotypes typically found throughout the African population confer a level of immunity, protection, against Plasmodium vivax (and Plasmodium knowlesi) infection typically spread through Anopheles mosquito encounters.
Platelet Additive Solution (PAS) Platelets and Their Variations
What's the difference between all of the different types of PAS platelet variations? Maybe you're only used to seeing one type, such as PAS-C, but there are other variations out there. What are PAS platelets anyway?Well by actual volume, a whole-blood derived or apheresis platelet collection...
Is Blood a Drug?
Yes! At least as defined by the Food and Drug Administration.
What phase does panagglutinin use?
ok - I got the results of 8/11 cells reacting. The tertiary care place called in a panagglutinin (they use solid phase).
What cells block negative cells from falling through gel?
3. White cells physically blocking the negative cells from falling through the gel
Why are auto control cells negative in gel?
They often give that characteristic “mixed field-ish” looking agglutination typical of IgM antibodies. Some are quite strong (even 4+). The Auto Control in Gel is typically negative because the patient cells are in MTS diluent and not exposed to the same antibiotics that are in the reagent cells. It seems like the 0.8% cells manufactured by Ortho for Gel testing have the offending ingredient and the 3% cells do not. When we see this pattern of all screening and panel cells positive, autocontrol negative we will prepared our own 0.8% dilutions of 3% screening cells to test in Gel and get negative Gel reactions. Of course all of this does not help with solid phase but the mechanism may be similar.
Why does antibody only react with gel?
This antibody only react at gel, maybe because gel is more sensitive than other method, or there is something in the patient's plasma react with the additive in gel.
Do lymphomas throw out antibodies?
I have in the past seen lymphomas throw out atypically presenting "antibodies or antibod-like" reactions. What I had noted over the many years (pre-gel or enhanced IDC) that the more undifferentiated the lymphoma, the more reactions you are likely to encounter (often reacting at 4 deg C).
Is panagglutinin clinically significant?
Unless they have performed thermal amplitude tests, which, of course, they may have done for all I know, I can't see that they can say it is a clinically insignificant panagglutinin. If the antibody is detectable at 30oC or above, then it is clinic ally significant, whatever the specificity.
Does gel pick up HLA antibodies?
Gel is also great at picking up HLA/HTLA antibodies.